13 Nerve Transfers for Shoulder Reanimation A 20-year-old male involved in a single-vehicle rollover accident suffered severe head injury, for which he spent 7 days in the intensive care unit. His left arm weakness was first discovered nearly 4 weeks postinjury as his cognitive function started to recover. Physical examination at 1 month showed wasting of his supraspinatus and infraspinatus as well as the deltoid muscles. The left biceps muscle bulk was reduced as compared with the right one. Motor examination showed complete absence of function in shoulder abduction, external rotation, and elbow flexion. Arm supination was only possible to 30 degrees. A nerve conduction study was consistent with upper trunk axonal loss but showed preservation of a single infraspinatus motor unit potential (MUP). Paraspinal and rhomboid muscles were intact clinically and electrically. A chest x-ray did not show an elevated diaphragm. Magnetic resonance imaging (MRI) of the cervical spine and brachial plexus showed some signal change consistent with edema in the supraclavicular area but no obvious intraforaminal nerve root injury or pseudomeningoceles. The plan was for conservative management, physiotherapy, and repeat electro-myography (EMG) and clinical assessment after 3 months. At his 4-month postinjury visit, the patient had partially recovered his biceps muscle function, had regained elbow flexion, and also noted that the numbness of his lateral forearm had decreased. However, he showed no recovery of his shoulder function. His examination showed a somewhat pronated hand with Erb posture, improved supination to just beyond 90 degrees, and elbow flexion grade 3/5 achieved with the biceps muscle. Brachioradialis lacked muscle contraction. Shoulder abduction was 0/5 and external rotation also remained absent. Repeated nerve conduction study showed a recovering lateral antebrachial cutaneous nerve response. Nascent MUPs were now present in the brachioradialis, one MUP was still observed in the infraspinatus muscle, but fibrillations were abundant in the deltoid and supraspinatus muscles, with absence of MUPs. The clinical situation suggested a recovering C6 spinal nerve root injury and persistent shoulder weakness most likely compatible with suprascapular and axillary nerve dysfunction, likely from a proximal C5 injury. The patient was offered exploration and possible graft repair and/or accessory to suprascapular nerve transfer and triceps branch transfer to the axillary nerve. Proximal C5 spinal nerve injury with severe shoulder abduction weakness due to suprascapular and axillary nerve dysfunction. In caliber, the fifth spinal nerve (C5) is the smallest of all of the brachial plexus spinal nerve roots. In the intervertebral foramen, it gives off the dorsal scapular nerve that supplies the rhomboids. Within the foramen or shortly after its exit, it gives off a small branch contributing to the long thoracic nerve, usually a branch from the posterior aspect of the spinal nerve. Small arteries and veins usually accompany the spinal nerve in the foramen. As it exits the foramen, C5 is related to the lateral border of the anterior scalene muscle anteriorly and middle scalene posteriorly. Extraforaminally it gives a branch contributing to the phrenic nerve. The C6 joins C5 and forms the upper trunk. The nerve to the subclavius comes off the inferior aspect of the upper trunk before it trifurcates into the suprascapular nerve and the anterior and posterior divisions. The C5 contributes primarily to the suprascapular nerve and (via the posterior division of the upper trunk) to the posterior cord and ultimately the axillary nerve. The accessory nerve can be found distally on the inner surface of the trapezius muscle following partial division of its insertion into the lateral aspect of the clavicle. After it gives off the first motor branch, an adequate 2 to 3 cm can be dissected and mobilized to be transferred to the suprascapular nerve directly with no tension. In the posterior quadrilateral space, as the axillary nerve emerges from the inferior border of the teres minor, it gives the anterior division that supplies the anterior and medial deltoid fibers and the posterior division that supplies the posterior deltoid, teres minor muscle, and also provides the upper lateral cutaneous nerve of the arm. The nerve to the long head of the triceps in the triangular space is quite close to the axillary nerve in the quadrilateral space. The distance between both nerves averages between 2.5 and 5 cm, which, after mobilizing each nerve, allows direct nerve transfer without tension and usually without utilizing an interposition graft. The upper trunk is most prone to injury because it is the most superior and superficial of the trunks of the brachial plexus and is also the shortest. Thus any force strong enough to distract the arm and the neck in opposite directions can cause variable degrees of damage to the C5/C6 nerve roots or the upper trunk. Traumatic Erb palsy (C5 and C6, occasionally C7 spinal nerve root involvement) has a characteristic posture that is known as waiter’s tip. The paralyzed muscles include the supraspinatus and infraspinatus, subclavius, biceps, brachialis, coracobrachialis, deltoid, teres minor, brachioradialis, and supinator. The limb will hang adducted by the patient’s side due to action of the unopposed adductors (pectoralis major, teres major, and latissimus dorsi), medially rotated by the unopposed subscapularis and teres major. The elbow lacks flexion, and the arm is pronated due to the loss of biceps and supinator action. If C7 is also involved, elbow extension may be weak, and variably the wrist extensor will be deficient and the wrist will assume a flexed position. The sensation in the lateral side of the forearm is lost due to loss of function of the lateral antebrachial cutaneous nerve. This typical posture is seen in early and severe cases; however, variable clinical pictures can be seen depending on the severity and the degree of recovery. The presence of associated clavicle or shoulder trauma may make the clinical assessment more difficult. Shoulder abduction for the first 20 to 30 degrees is performed by the action of the supraspinatus muscle, innervated by the suprascapular nerve. Supraspinatus muscle palsy can result from injuries of the C5 nerve root, the upper trunk of the brachial plexus, and the suprascapular nerve. Deltoid weakness following trauma is usually due to injury to the C5 spinal nerve root, the upper trunk of the brachial plexus, or isolated injury to the axillary nerve. Nerve root injury can result from apraxia, traction (neuroma in continuity), and avulsion injury. Axillary nerve injury is usually of a traction nature. This patient’s dysfunction could have occurred from isolated and separate axillary and suprascapular nerve injuries. Alternatively, an isolated C5 injury (avulsion or traction) may have been responsible. However, a unifying diagnosis would be a single traction lesion involving the C5 and C6 spinal nerves into the upper trunk. A greater involvement of the trunk component contributing to the suprascapular nerve and the posterior division of the upper trunk, which contributes mainly to axillary nerve outflow, with lesser involvement of the anterior division (outflow to the musculocutaneous nerve), would exactly fit the pattern of the clinical course witnessed. A thorough and detailed clinical assessment remains the cornerstone in the diagnosis of brachial plexus and peripheral nerve injury. Both EMG and nerve conduction studies are helpful to confirm the diagnosis and help elucidate the possibility for preganglionic injury. Nerve root avulsion can be diagnosed preoperatively when sensory nerve action potentials (SNAPs) are recorded from an insensate dermatome. Nerve root avulsions and pseudomeningoceles can also be imaged by MRI or computed tomographic (CT) myelography directly. Intraoperatively, the differentiation between pre- and postganglionic injury is confirmed by nerve action potential (NAP) studies. Absent muscle contractions and intact, large amplitude, and fast-conducting NAPs are indicative of preganglionic injury. A smaller, slower-conducting response indicates regeneration. In case of absent NAPs, the injury can be either postganglionic or both pre- and postganglionic. Conservative management is usually the first option in the treatment of closed brachial plexus injury because variable degrees of recoveries are common. Shoulder dislocation/ fractures, if present, need to be addressed and repaired to optimize recovery. Physiotherapy is essential during the period of spontaneous recovery to maintain the muscle bulk. Absence of functional recovery at 4 months is usually an indication for surgical exploration. Axillary nerve is known to take a relatively longer time for recovery than other nerves, given its extensive branching into anterior and posterior divisions and both branches dividing further into smaller ones. This carries the possibility of regenerating axons to follow different routes and minimize the axons that reach the anterior division, which supplies the anterior and medial deltoid muscle. For this reason some advocate awaiting policy up to 6 months for isolated axillary nerve injuries. As a practical approach, we recommend booking for surgery at 4 months if no recovery has occurred, with the planned surgical date around 5 to 6 months from injury. The patient was explored 5 months after initial injury. The entire left upper extremity from the neck to the elbow was prepped and draped so that this would allow access to the supraclavicular region as well as both anterior and posterior aspects of the shoulder girdle. Supraclavicular exposure of the brachial plexus was performed by making a transverse incision one fingerbreadth above the clavicle (Fig. 13–1). The upper trunk components were dissected and both anterior and posterior divisions were separated. The suprascapular nerve was also identified. The C5 and C6 spinal nerve and the proximal upper trunk did not look or feel normal; this raised the suspicion of some degree of injury in continuity. It was observed that the proximal C5 spinal nerve also had an abnormal consistency right back to the foramen. More distally, the branching to the anterior, posterior, and suprascapular nerves appeared normal. Intraoperative stimulation of the anterior division demonstrated contraction of the pectoralis major muscle. Stimulation of the anterior division, even with large amounts of current, did not reveal any biceps contraction, which raised the possibility of biceps muscle reinnervation largely from C7 outflow. No response was elicited from the posterior division of the upper trunk or the suprascapular nerve, even with the use of up to 10 mA of stimulating current. It was therefore decided to repair the nerve injuries. An option would have been intraplexal graft repairs from very proximal C5 and C6 spinal nerves to the suprascapular nerve and anterior and posterior divisions of the upper trunk (a strategy reported in chapter 2 of this text). However, we elected instead to transfer the accessory nerve to the suprascapular nerve and the triceps branch to the axillary nerve. The spinal accessory nerve was located after partial (1 to 2 cm) division of the trapezius of its insertion into the lateral superior aspect of the clavicle. After identifying the nerve visually, aided by intraoperative stimulation, a proximal motor branch was dissected off, and the nerve was followed distally deep to the clavicle, and 3 cm of the nerve was isolated. Stimulation of the nerve caused vigorous contraction of the trapezius muscle. The accessory nerve was cut distally, well past its initial motor branch. The suprascapular nerve was cut proximally, just after its origin from the upper trunk. The nerve appeared normal at this level grossly and under the operating microscope with well preserved fascicles. The accessory nerve was then coapted (and was tension free) to the suprascapular nerve using 9–0 nylon monofilament suture under the operating microscope.
 Case Presentation
Case Presentation
 Diagnosis
Diagnosis
 Anatomy
Anatomy
 Characteristic Clinical Presentation
Characteristic Clinical Presentation
 Differential Diagnosis
Differential Diagnosis
 Diagnostic Tests
Diagnostic Tests
 Management Options
Management Options
 Surgical Treatment
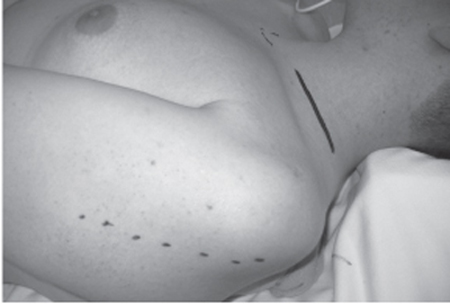
Surgical Treatment
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


