Fig. 4.1
Venn diagram of Engel’s biopsychosocial model of health
Considerable interest has been generated around understanding the role psychological factors may play in influencing disease trajectories, including susceptibility, progression, and adjustment. In addition to influencing health-related quality of life (Adams et al., 2004; Olson, Trevino, Islam, & Denner, 2010; Thomten, Soares, & Sundin, 2011), as well as disease progression and relapse (Leserman et al., 1999; Pembroke, Rasul, Hart, Davey Smith, & Stansfeld, 2006; Porcelli, Zaka, Centonze, & Sisto, 1994), psychological factors have been related to early mortality in some chronic conditions (Rasul, Stansfeld, Smith, Shlomo, & Gallacher, 2007; Watson, Homewood, Haviland, & Bliss, 2005). Psychological factors are also now beginning to be considered in concert with traditional risk factors such as obesity, poor nutrition, and smoking for the development of some chronic diseases (Clarke & Currie, 2009).
Importantly, there is an increasing body of evidence to suggest that psychological disorders and arthritis are intimately intertwined (Murphy, Sacks, Brady, Hootman, & Chapman, 2012; Shih, Hootman, Strine, Chapman, & Brady, 2006; Soderlin, Hakala, & Nieminen, 2000). Depression is the most commonly examined psychological construct in arthritis research. While anxiety has been examined to a lesser extent, depression and anxiety co-occur in some individuals (Axford et al., 2010). Models of depression and anxiety (e.g., The Tripartite Model) suggest that conceptually these constructs contain shared and specific components (Clark & Watson, 1991). Explicitly, it suggests that anxiety and depression overlap through a general, nonspecific factor related to negative affectivity, or more generally, psychological distress. Therefore, depression, and, by extension, anxiety have been found to result in deleterious health-related effects for individuals with arthritis. In particular, depression and anxiety are known to complicate disease management, thereby increasing health care utilization, costs (McLaughlin, Khandker, Kruzikas, & Tummala, 2006), and risk of early mortality (Ang, Choi, Kroenke, & Wolfe, 2005).
The Psychological Burden of Arthritis
The existence of a chronic illness is a strong risk factor for poor psychological health (Moussavi et al., 2007; Sareen, Cox, Clara, & Asmundson, 2005). Although the adaptation to chronic disease is highly individualistic, the debilitating pain and limitations associated with arthritis have been found to have a significant impact on psychological functioning. The following section describes the prevalence of depression and anxiety (including its more general derivative, psychological distress) in arthritis, changes in psychological functioning over the disease course, and the factors that contribute to poor psychological functioning in arthritis.
Prevalence
Depression
Analyses from a state-based telephone survey of noninstitutionalized US adults found that 13.4 % of individuals aged 45 and over with self-reported arthritis experienced more than 14 mentally unhealthy days in the past month (Strine et al., 2004). Other studies have demonstrated that individuals with arthritis have around a 2–3-fold increase in the odds of reporting depressive and anxiety symptoms when compared with the general population (Murphy et al., 2012; Shih et al., 2006). Dunlop, Lyons, Manheim, Song, and Chang (2004), using data from a population-based cohort of men and women aged 54–65 (n = 7825), have suggested that as much as 18 % of experienced major depression may be attributed to having arthritis. However, these figures are dependent upon the populations studied and the measures utilized.
Specifically, in RA, prevalence of depression ranges from 13 to 20 % when focused on psychiatric assessment or clinical diagnosis (Dickens, McGowan, Clark-Carter, & Creed, 2002; Hyrich et al., 2006) and exceeds 50 % when based on self-report screening tools (El-Miedany & El-Rasheed, 2002). Particularly, a study of 238 Norwegian patients with clinically diagnosed early RA (≤4 years duration) found that 20 % had scores on the Arthritis Impact Measurement Scale (AIMS), indicating possible psychiatric disturbance (Smedstad, Moum, Vaglum, & Kvien, 1996). While less examined than that of RA, depression in OA has also been reported at elevated levels when compared to the general population. A 10-year study of 6153 consecutive RA outpatients found that 20 % fulfilled criteria for ‘probable’ depression, while 16.8 % of individuals with OA of the knee or hip, and 14.3 % with OA of the hand, were found to experience ‘probable’ mental distress (Hawley & Wolfe, 1993). However, slightly higher depression figures for men and women with OA (according to American College of Rheumatology criteria) were reported in a German primary care sample (19.4 %) (Rosemann, Laux, & Szecsenyi, 2007). Likewise, in a recent small clinical study (n = 86), Marks found in men and women (≥60 years) with radiographic and clinical evidence of mild to moderate knee OA that approximately 28 % of the sample were classified as having ‘possible depression’ based on The Center for Epidemiological Studies-Depression (CES-D), while 21 % had nonclinically validated moderate to severe depression.
Anxiety
While anxiety has been less frequently studied in isolation from depression, current research suggests that between 21 and 70 % of individuals with arthritis experience heightened levels of anxiety (El-Miedany & El-Rasheed, 2002; Murphy, Creed, & Jayson, 1988). In particular, Lok, Mok, Cheng, and Cheung (2010), in their examination of rheumatology outpatients with median disease duration of 4 years, found the point prevalence of anxiety disorders (based on the Diagnostic and Statistical Manual of Mental Disorders Fourth Edition criteria) to be 13.0 %, with generalized anxiety disorder the most common.
The Relative Burden of Depression and Anxiety
Although considerable overlap between depression and anxiety has been noted in arthritis populations (Murphy et al., 2012), conjecture exists regarding the relative burden of depression compared to anxiety. While Isik, Koca, Ozturk, and Mermi (2007) reported a significantly higher prevalence of depression compared to anxiety in their small study (n = 82) of consecutive RA patients (41.5 % with depression alone vs. 13.4 % with anxiety alone), Harris, Loxton, Sibbritt, and Byles (2012) argued that anxiety may be a primary and somewhat overlooked concern. In a representative sample of older Australian women, the diagnosis of an anxiety/nervous disorder was the only significant psychosocial factor associated with arthritis following the adjustment for demographic characteristics and health-related quality of life. This finding is supported by previous case–control and clinic-based research (El-Miedany & El-Rasheed, 2002; Hawley & Wolfe, 1988; Odegard, Finset, Mowinckel, Kvien, & Uhlig, 2007; Soderlin et al., 2000), in conjunction with the recent population-based study conducted by Murphy et al. (2012). While one-third of respondents with arthritis reported experiencing either anxiety or depression, the authors noted that anxiety was twice as common as depression (31 % vs. 18 %) and depression was contingent upon the presence of anxiety (84 %). Moreover, El-Miedany and El Rasheed (2002) noted in their Egyptian outpatient study (n = 80) that 63.4 % of women with arthritis experienced depression, while an even greater proportion reported anxiety (66.2 %).
Taken together, these findings suggest that affective disturbance may have important implications over the disease course. It is important to note, however, that findings from a prospective study involving individuals with RA suggest that the prevalence or severity of depression is not dissimilar to individuals with other chronic diseases (Hawley & Wolfe, 1993) and, as such, may be related to reduced quality of life and not a function of the disease per se (Courvoisier et al., 2012; Hawley & Wolfe, 1993).
Psychological Functioning Over Time
Despite the increased reporting of psychological problems in individuals with arthritis, longitudinal studies have found that the process of psychological adjustment is complex with considerable variability in findings. Some studies have found a reduction in emotional distress over time (Crotty et al., 1994; Evers, Kraaimaat, Geenen, Jacobs, & Bijlsma, 2002; Persson, Larsson, Nived, & Eberhardt, 2005), while others have found that mental health remains relatively stable over the disease course (Smedstad, Vaglum, Moum, & Kvien, 1997; Uhlig et al., 2000). A longitudinal analysis of data from 158 Swedish primary care patients found that a latent effect may be associated with psychological adaptation in those newly diagnosed with RA. Improvements were not identified until the three-year follow-up (Persson et al., 2005). Meanwhile, in a 3-year prospective study of Hungarian and Austrian RA outpatients aged 40–75 years (n = 118), it was found that compared to population norms, mild depressive symptoms were noted early in the RA disease process (Palkonyai et al., 2007). It has also been suggested that anxiety may present earlier, with the onset of depression occurring later (Wittchen, Kessler, Pfister, & Lieb, 2000).
However, findings from qualitative research suggest that arthritis involves a spectrum of emotions ranging from frustration and annoyance to fear, anger, resentment, misery, and helplessness (Baird, 2000; Lutze & Archenholtz, 2007; Melanson & Downe-Wamboldt, 2003). In one US study of older women (n = 18) with OA (aged 65–92 years), arthritis was described as an ever-present and unwelcomed entity which dominated their attention. This feeling was likened to ‘wearing a heavy garment’ (Baird, 2000). Norton, Sacker, Young, and Done (2011), using data from a large prospective cohort study of men and women with early RA, identified a nonlinear change in distress over a 10-year period. Using latent growth mixture modeling techniques, the authors were able to demonstrate that while psychological distress remained relatively stable across the disease course (following an increase at the time of diagnosis), heterogeneity in psychological response was identified when individual trajectories were examined. While the majority experienced low levels of distress that remained relatively stable over time (68 %), 12 % demonstrated consistently high levels of distress. Meanwhile, a small proportion showed a decrease in psychological distress (9 %) with a further 11 % reporting increasing distress (see Fig. 4.2).
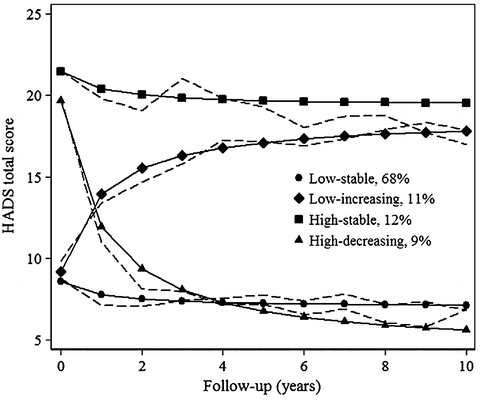

Fig. 4.2
Psychological distress trajectories of the 4-class growth mixture model. Solid lines are model-implied trajectories for each class and dashed lines are sample means weighted by class probabilities. Reprinted from Journal of Psychosomatic Research, 71(5), Norton S, Sacker A, Young A, Done J, Distinct psychological distress trajectories in rheumatoid arthritis: findings from an inception cohort, p. 293. Copyright (2011) with permission from Elsevier
Predictors of Psychological Functioning in Arthritis
Given the variation in long-term psychological functioning identified above, it is important for health professionals to identify factors that differentiate between patients who do and do not successfully adjust psychologically to arthritis. At the extreme end of the spectrum, the coexistence of psychological disorders and chronic pain conditions (particularly RA) has been associated with increased risk of suicidal ideation and suicide completion (Timonen et al., 2003; Treharne, Lyons, & Kitas, 2000). Research has demonstrated that depression and anxiety in individuals with arthritis can result from a complex interaction between physical, clinical, and psychosocial factors (Covic, Tyson, Spencer, & Howe, 2006). Key factors are described below.
Physical and Clinical Predictors
A number of studies have demonstrated an association between physical and clinical indicators of arthritis with reduced psychological functioning. Much of this research, however, has focused on depression or psychological distress as the outcome and has relied on data from RA subpopulations. Considerable conjecture exists regarding the relative importance of these factors.
Functional Impairment and Disability
Despite its slow development, arthritis is progressive in nature and eventually leads to joint destruction, significant loss of function, and reduced health-related quality of life in many patients (Hill et al., 2007; Peters, Sanders, Dieppe, & Donovan, 2005; van Dijk, Dekker, Veenhof, & van den Ende, 2006; Zochling, Stucki, Grill, & Braun, 2007). Findings from the Centers for Disease Control and Prevention (2005) in the USA have indicated that one in three individuals with arthritis report activity limitations as a result of their condition. Findings confined to OA populations have revealed that 80 % of people experience limitations in movement, with 25 % unable to perform major daily activities (WHO Scientific Group, 2003). Further, approximately 10 % of people aged over 60 are disabled as a result of the disease (Buckwalter et al., 2004), with increased levels associated with concomitant disease (Marks & Allegrante, 2002). Similar findings have been reported with respect to RA. Severe functional decline has been noted in 10 % of individuals within 2 years, and up to half of persons with RA are work- disabled within 10 years of diagnosis (Sokka, Kautiainen, Mottonen, & Hannonen, 1999; Wolfe & Hawley, 1998).
In a cross-sectional clinical study of 111 adults with RA, Covic, Adamson, and Hough (2000) found that physical disability was predictive of depression (as measured by the AIMS) and was mediated by psychosocial factors including passive coping and helplessness. Likewise, Margaretten et al. (2009) identified a significant relationship between physical disability and increased depressive symptomatology in their socioeconomic and ethnically diverse RA cohort (n = 174). Specifically, univariate analyses revealed no significant demographic differences between patients reporting depression (measured by the Patient Health Questionnaire 9) and those that did not. Of the clinical features, only physical functioning (measured by the Health Assessment Questionnaire; p < 0.001), disease activity (measured by RA-specific Disease Activity Score in 28 [DAS28] joints; p = 0.04), along with lower use of disease-modifying antirheumatic drugs (p = 0.03) were significant predictors. When these variables were entered into the multivariate model, however, only physical functioning remained significant (p < 0.001). In this multivariate model, a reduction in depressive symptoms was noted for individuals of Asian or Pacific Islander origin (p = 0.02). This finding is supported by another rheumatological outpatient study (El-Miedany & El-Rasheed, 2002). While it was found that functional disability was the only clinical predictor of depression, the authors were able to demonstrate disparate clinical profiles for depression and anxiety. Anxiety was associated with joint tenderness and stiffness, short disease duration, as well as rheumatoid factor and nodules. This finding however, contrasts with that of Ho, Fu, Chua, Cheak, and Mak (2011) who found that among consecutive patients at a University-based hospital (n = 100), while rheumatoid factor and biological indicators of disease activity were significant in univariate analyses, the effect disappeared in the multivariate model. In this study, rheumatoid factor was associated with depressive symptoms only.
On the other hand, a two-year longitudinal study of individuals (n = 227) with early stage RA (i.e., ≤4 years duration) examined predictors of change in depression and anxiety symptoms at both 1 and 2 years (Smedstad et al., 1997). With depression (measured using the AIMS) as the outcome, it was found in multivariate analyses that 1- and 2-year change in depression scores was predicted by level of disability. Serologic indicators of disease activity such as erythrocyte sedimentation rate (ESR) , along with joint tenderness and pain levels, failed to predict the relationship. Importantly, previous depression scores also predicted depression. When cross-lagged analyses were conducted in an attempt to determine causality between the variables of interest, the only significant finding was related to depression at 1 year. High levels of disability at baseline predicted depression at time one. This effect, however, was not sustained at 2-year follow-up. In contrast, no disease-related factors were found to predict 1- and 2-year change in anxiety scores. Previous anxiety levels were the only predictor of future anxiety.
Moreover, in a nationally representative sample of US noninstitutionalized civilians, Godha, Shi, and Mavronicolas (2010) found a strong relationship between RA functional limitation severity and depression. In particular, after controlling for the confounding effects of age, physical activity, and comorbidities, patients belonging to Class II (i.e., able to perform usual self-care and vocational activities, but limited in avocational activities such as recreational activities and/or leisure; and activities related to work, school, and homemaking) were almost four times more likely to have a high tendency toward depression compared to Class I (i.e., completely able to perform usual activities of daily living such as self-care, vocational, and avocational). Meanwhile the odds of depression increased substantially (OR = 5.92) for those in Class III (i.e., able to perform self-care, but limited in vocational and avocational activities) compared to Class I. It is important to note that older age and level of physical activity were associated with a reduction in depression.
Pain and Disease Activity
While clinical expression and progression of arthritis are highly variable, particularly for RA, with the disease course marked by periods of exacerbations and remissions (Australian Institute of Health and Welfare, 2005), pain and joint stiffness have been identified as key indicators of arthritis. Pain, in particular, is often a common reason individuals seek medical attention (Gureje, Von Korff, Simon, & Gater, 1998).
In a longitudinal examination of clinically important predictors of self-reported depressive symptoms (evaluated using the mental health component score of the Medical Outcomes Study Short Form-36 [SF-36]) in 29,524 adults aged 18 and over with rheumatic disease, Wolfe and Michaud (2009) found that 9-year incidence of depression was in the vicinity of 40 %. When RA was specifically examined, those with depression were found to be characteristically different from those without depression on a range of sociodemographic, psychological, and disease-related indicators. Using Random Forest analyses, however, the authors identified factors associated with disease severity, that is, symptom intensity (measured as a combination of the fatigue component of the Visual Analog Scale [VAS] and Regional Pain Scale [i.e., painful nonarticular joint count]), pain and global severity (measured by the VAS), and fatigue, as well as disease comorbidity to classify patients with depressive symptoms. Despite this, when recursive partitioning was applied to the data, only symptom intensity was necessary to identify participants with depressive symptoms. In addition, the cumulative impact of this indicator of disease severity was found to contribute to mortality over the study period.
Further, in a longitudinal study of 15,282 patients with RA, pain was found to account for 44 % of the variance associated with psychological functioning (as measured by the mental health component of the SF-36) (Courvoisier et al., 2012). More specifically, multivariate analyses found that pain explained 60 % of the variance associated with the stable part of psychological functioning over the study period. In this analysis, disease activity and functional disability also contributed to psychological functioning. When the variable part of psychological functioning was assessed, only pain remained as the significant explanatory variable, explaining 5 % of the variance. Moreover, in the Norton study (described in the section above) (Norton et al., 2011), the four psychological trajectories over the 3-year study period were found to be related to self-reported disease severity. Those that had high levels of depression, either high stable or high decreasing, were found to have higher levels of disease severity at baseline compared to those with low-stable or low-increasing depression. Importantly, key serological markers of inflammation, ESR and C-reactive protein (CRP) failed to predict psychological functioning over time. Interestingly, disease severity indicators were also the difference between those with high levels of depression that remained stable over the course of the study compared to those that saw improvements in mental health.
Fatigue
The experience of fatigue is also common to both RA and OA. Although the prevalence has varied according to the measurement used and level of active disease present, it has been suggested that up to 93 % of individuals with OA or RA experience fatigue (Belza, 1995; Wolfe, Hawley, & Wilson, 1996). When clinically significant levels of fatigue have been investigated however, this figure approaches 50 % (Wolfe et al., 1996). Moreover, haematological manifestations have been found to be prominent in arthritis, particularly in RA subpopulations. The prevalence of mild anemia in RA has ranged from 33 to 60 % (Wilson, Yu, Goodnough, & Nissenson, 2004). Wolfe and Michaud (2006) found that mild anemia (as defined by the World Health Organization) was present in 31.5 % of participants with RA, with lifetime prevalence being in the vicinity of 50 %. Using discriminant analysis, Covic et al. (2006) identified 12 specific predictors that were able to correctly classify the majority of participants (80 %) in their rheumatological sample (n = 134) based on depression status. Fatigue was found to be the strongest clinical predictor of depression (loading = 0.57), followed by pain (loading = 0.55) and physical disability (loading = 0.44). Despite this, psychological factors, particularly tension and self-esteem, were the strongest overall predictors of the relationship (loadings = 0.73). Likewise, in a large convenience community sample (n = 200) of older adults with RA (mean age 66.7 years), Franklin and Harrell (2013) examined the unique effect of pain and fatigue on depression. In this study, functional impairment accounted for a significant amount of the variance associated with depressive symptoms (β = 0.47; 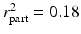 ). Importantly, pain did not contribute to the relationship between RA and depression following control for demographics and functional impairment. After controlling for demographics, functional impairment, and pain, fatigue was found to contribute 10 % unique variance to the RA–depression relationship.
). Importantly, pain did not contribute to the relationship between RA and depression following control for demographics and functional impairment. After controlling for demographics, functional impairment, and pain, fatigue was found to contribute 10 % unique variance to the RA–depression relationship.
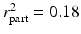 ). Importantly, pain did not contribute to the relationship between RA and depression following control for demographics and functional impairment. After controlling for demographics, functional impairment, and pain, fatigue was found to contribute 10 % unique variance to the RA–depression relationship.
). Importantly, pain did not contribute to the relationship between RA and depression following control for demographics and functional impairment. After controlling for demographics, functional impairment, and pain, fatigue was found to contribute 10 % unique variance to the RA–depression relationship. Psychosocial Predictors
While the findings suggest that long-term disability, joint damage, and pain (to some extent) as opposed to RA disease activity (e.g., swollen joints, ESR, CRP) may contribute substantially to depression in arthritis, these findings are not conclusive. Psychosocial factors are increasingly being suggested as mediators or moderators of the relationship between arthritis and psychological functioning. Although the list of psychosocial factors implicated in psychological adaptation to arthritis is extensive, the following provides an overview of the role some of the key factors play.
Sociodemographics
Depending upon the variables included in the analyses, sociodemographic variables have been inconsistently linked to poor psychological adjustment to arthritis. In particular, various studies have suggested that age (particularly at diagnosis) (Patten, Williams, & Wang, 2006; Ramjeet, Koutantji, Barrett, & Scott, 2005), gender (Marks, 2013; Ramjeet et al., 2005; Theis, Helmick, & Hootman, 2007), education (Mella, Bertolo, & Dalgalarrondo, 2010), and marital status (Katz & Yelin, 1993; Strine et al., 2004) are important indicators. For instance, Strine et al. (2004), in their examination of Behavioral Risk Factor Surveillance System data, found that frequent mental distress in arthritis was associated with female gender, lower education (noncompletion of high school), marital status (previously married), younger age, ethnicity (Hispanic), and employment status. It is important to note, however, that disease-related and psychological factors were not controlled for in this study. Mella et al. (2010), on the other hand, found education to be the only demographic predictor of depressive symptoms, alongside levels of disease activity and functional impairment. In their longitudinal analysis of Swedish primary care patients (n = 158) however, Persson et al. (2005) noted that higher risk of distress was associated with younger age, female gender, and a number of psychosocial factors, including lower social support and higher distress at baseline.
Psychological Vulnerability
Psychological vulnerability has been found to impact future levels of psychological distress. Importantly, previous levels of depression or anxiety have been found to be key predictors of short-term psychological functioning in arthritis (Smedstad et al., 1997). In a small study (n = 22) of individuals with early RA, Sharpe and colleague found that initial levels of depression consistently predicted between 37 and 58 % of the variance attributed to psychological functioning over time. In this study, coping strategies were found to predict psychological functioning in the early stages of the disease, accounting for 9 % and 5 % of the variance at times two and three, respectively. Interestingly, while disability predicted psychological functioning at all follow-up time points (i.e., 2–6), joint function improved despite decreases in mood.
Additionally, in a 2-year longitudinal study of RA, Sinclair and Wallston (2010) identified that the construct psychological vulnerability (measured by Psychological Vulnerability Scale) added 9.3 % unique variance to concurrent depressive symptoms, beyond that of personal control factors such as helplessness and functional impairment. Meanwhile, lower psychological vulnerability contributed 5.6 % unique variance to depressive symptoms 1 year later. In this analysis, age and disease comorbidity failed to predict changes in depressive symptoms (measured by the CES-D). The authors argued that this suggests that these factors do not confound the relationship between psychological vulnerability and psychological distress in arthritis.
Further, while stress and its role in arthritis will be discussed in detail in Chap. 5, it is an important predictor of long-term psychological functioning in arthritis populations. In a study of Irish women (n = 59) with established RA (mean age = 60 years) attending an outpatient clinic, it was found that perceived stress was associated with affective disturbance at 1-year follow-up (Curtis, Groarke, Coughlan, & Gsel, 2004). Correlational and hierarchical regression analyses revealed that psychological stress was the best predictor of depression and was a better predictor than disease severity on measures of positive and negative emotionality. Treharne, Lyons, Booth, and Kitas (2007) provided additional support for the significant impact of perceived stress on mental health outcomes in arthritis. In their longitudinal study involving 134 U.K. outpatients with RA, the authors found that perceived stress had the strongest relationship with psychological well-being at baseline and perceived stress had an impact on anxiety levels at 6 month follow-up.
Coping Efforts
Coping efforts have been suggested as key factors in developing a sense of control and mastery over chronic illness (Dager, Kjeken, Fjerstad, & Hauge, 2012; Shaul, 1995). Studies focused on RA subpopulations have consistently demonstrated that coping strategies employed by an individual in response to arthritis-related symptoms such as pain have a significant impact on psychological and physical health outcomes (Brown, Nicassio, & Wallston, 1989; Covic, Adamson, Spencer, & Howe, 2003; Covic et al., 2006). The majority of this research has generally concentrated on assessing the way individuals manage chronic pain according to the dichotomous problem-focused and emotion-focused approaches (or variants thereof, e.g., active vs. passive coping) proposed by Lazarus and Folkman (1987). Particularly, Curtis, Groarke, Coughlan, and Gsel (2005) found that although perceived stress was associated with affective disturbance and was the best predictor of depression in 59 Irish RA outpatients, the use of avoidant coping efforts (i.e., efforts to distract from, or avoid the stressor) contributed to the prediction of negative affect. These findings were supported in a 12-month follow-up study of this cohort of women (Curtis et al., 2004). Similarly, passive coping with pain has also been found to increase depression at 6-month follow-up. This finding, however, was specific to those with RA experiencing greater pain (Brown et al., 1989).
Previously, emotion or passive-based approaches to coping have generally been regarded as maladaptive. Snow-Turek, Norris, and Tan (1996) indicated that passive, maladaptive coping approaches have qualities that outweigh the benefits of active coping. These approaches have been previously associated with increased arthritis pain, disability, and depression in comparison to individuals who employ problem-based (or active) coping strategies (Brown, Wallston, & Nicassio, 1989; Covic et al., 2000, 2003; Evers, Kraaimaat, Geenen, Jacobs, & Bijlsma, 2003; van Lankveld, Naring, van’t Pad Bosch, & van de Putte, 2000). However, a Canadian longitudinal qualitative study involving three time points (Melanson & Downe-Wamboldt, 2003) found that older men and women with RA (n = 39) used a variety of strategies (i.e., confrontive, palliative, supportant, fatalistic, self-reliant, evasive, optimistic, and emotive) in order to adjust. Meanwhile, Gignac, Cott, and Badley (2000), using content analysis, noted that Canadian community-dwelling older adults with OA (n = 286) employed 13 distinct behavioral efforts in order to adapt to their condition. These coping efforts concerning ‘selection’ (i.e., performing activities less often), ‘optimization’ (i.e., augmenting or enriching reserves to enable continued functioning), ‘compensation’ (i.e., substituting activities), and ‘receiving help’ were integral to perceptions of dependence (or independence) and facilitated psychological adjustment. Another study utilizing a narrative biographic approach, found that Austrian RA outpatients (n = 10) described their experience as positive, with the disease seen as a challenge and facilitator of personal growth (Stamm et al., 2008).
Importantly, a recent systematic review examining the longitudinal association between coping and psychological adjustment in RA found limited evidence that passive or disengaging coping strategies such as helplessness, avoidance, and wishful thinking were prospectively associated with increased psychological distress (Vriezekolk, van Lankveld, Geenen, & van den Ende, 2011). It was also noted that there was no evidence for active or engagement-style coping (e.g., problem-solving, emotional regulation, distraction, and cognitive restructuring) playing a role in the improvement of psychological distress long-term. Therefore, coping strategies may play more of a role in understanding psychological functioning in the early stages of disease only.
Others (e.g., Gronning, Lomundal, Koksvik, & Steinsbekk, 2011) have suggested that adjusting to a chronic illness is a dynamic process, influenced not only by the disease but by the individual’s life circumstances and personal resources. This finding is supported by a recent qualitative study of older Australian women with OA (Harris, Byles, Sibbritt, & Loxton, 2015). In this study it was found that psychological adjustment over time was similar to that of RA and was attributed primarily to cognitive and attitudinal factors such as stoicism, making downward comparisons, and cognitive reappraisal. This was a dynamic “day-to-day” process involving a constant struggle between grieving physical losses and increasing dependence amidst symptom management. Therefore, adopting a balanced or flexible coping approach may be the key to long-term psychological adjustment to chronic diseases such as arthritis (Masuda et al., 2011).
Social Support
Social support has been found to have direct and moderating effects (through the stress response) on the relationship between arthritis and psychological functioning (Brown et al., 1989; Dekkers et al., 2001; Evers, Kraaimaat, Geenen, & Bijlsma, 1997). Social support can be defined as the existence or perceived availability of people who care about an individual and whom they can rely on when needed (Ethgen et al., 2004). In a Dutch study of 229 randomly selected RA outpatients, the support of a spouse was found to be a significant predictor of lower depression and anxiety of individuals with RA (Kraaimaat, Van Dam-Baggen, & Bijlsma, 1995). Evers et al. (1997) found that recently diagnosed Dutch RA outpatients (n = 91) who had smaller networks (i.e., quantity of social support) experienced greater psychological maladjustment in their first year after diagnosis compared to those with a larger network. An analysis of data from an international longitudinal cohort study (Demange et al., 2004) found that RA patients (n = 542) who received more social support (i.e., perceived satisfaction with support given) or had a larger social network had better functional and psychological adjustment over time. However, it has been argued that the perceived availability and quality of the support received may be more important than the size of an individual’s network (Leskela et al., 2006). Perceived social support, in particular, has been found to be beneficial for both physical and psychological outcomes in arthritis (Demange et al., 2004; Ethgen et al., 2004; Ferreira & Sherman, 2007; Sherman, 2003). Ferreira and Sherman (2007) and Sherman (2003) found that perceived social support was associated with reduced depressive symptoms in older adults with OA.
Personality
Personality-based characteristics have been found to influence the way in which individuals appraise a given situation and the selection of coping strategies (either adaptive or maladaptive) (Folkman & Greer, 2000). A longitudinal study of Dutch outpatients with early RA (n = 78) found that neuroticism (i.e., the tendency to be relatively more tense and emotionally unstable) at diagnosis was the most consistent and effective predictor of increased psychological distress (depression and anxiety) at both 3- and 5-year follow-up (Evers et al., 2002). Further, Scheier and Carver (1987) and Scheier, Weintraub, and Carver (1986) have posited that an optimistic life approach may play a protective role in chronic disease, facilitating the choice of disease-related coping strategies and engagement in health behaviors. Optimism has been positively associated with psychological well-being (both cross-sectionally and prospectively) (Brenner, Melamed, & Panush, 1994; Fournier, de Ridder, & Bensing, 2002; Long & Sangster, 1993) and health-related quality of life (Allison, Guichard, & Gilain, 2000; Carver et al., 1994; Scheier et al., 1989) and inversely with symptom expression (Achat, Kawachi, Spiro, DeMolles, & Sparrow, 2000; Ferreira & Sherman, 2007; Scheier & Carver, 1985). Additionally, it is suggested that individuals with an optimistic outlook employ problem-based coping in response to situations appraised as controllable, and emotion-based strategies aimed at harm minimization in response to situations appraised as uncontrollable (Scheier et al., 1986). Similarly, a U.K. longitudinal study of 134 RA outpatients (predominantly women) identified pessimism as a predictor of increased anxiety at baseline and increased depression, anxiety, and decreased life satisfaction at 6-month follow-up (Treharne et al., 2007). Individuals who reported greater levels of optimism reported better adjustment in terms of anxiety at baseline and depression at 1-year follow-up.
The Contribution of Psychological Disorders to the Physical Burden of Arthritis
Management of arthritis has heavily focused on symptom relief, including the reduction of pain and inflammation (Branch, Lipsky, Nieman, & Lipsky, 1999). However, disease-related factors have been found to only modestly predict future arthritis disability (van der Heide, Jacobs, Haanen, & Bijlsma, 1995; Wolfe & Cathey, 1991). With significant variability associated with arthritis disability, it has been suggested that factors extraneous to the disease may play a key role in the burden of disease. Depression, when present in its clinical form, has been attributed to mortality in RA patients (Ang et al., 2005). However, with substantial discordance between objective disease indicators (including radiographic evidence and joint inspection) and the severity of symptomatology (Jones & Doherty, 1995; Kean, Kean, & Buchanan, 2004), a large focus has been on reduced health-related quality-of-life indicators. The link between psychological distress and pain has been suggested to be bidirectional (Kroenke et al., 2011). The following section describes the influence of psychological disorders (depression and anxiety) on physical functioning, pain, and other clinical indicators of arthritis.
Physical Functioning and Disability
With the exception of a few studies, research examining the impact of psychological disorders on physical functioning and disability has largely come from cross-sectional studies (see previous section). In particular, Strine et al. (2004), examining predictors of arthritis in the Behavioral Risk Factor Surveillance System cohort, found that frequent mental distress had a significant impact on physical health. Although a cross-sectional study, the authors noted that after controlling for important sociodemographic characteristics (age, ethnicity, gender, employment status, marital status, and educational attainment), those with frequent mental distress (i.e., reported ≥14 mental health days as not good) were found to have increased associations with reporting their general health as either fair or poor (adjusted OR = 3.1), had 14 or more physically unhealthy days in the past month (adjusted OR = 4.1), as well as increased inability to perform daily activities (adjusted OR = 2.2), and the need to use support aids (adjusted OR = 1.8).
In an earlier RA-focused study (n = 80), Murphy et al. (1988) found that psychiatric illness (depression and anxiety) was only associated with two of the assessed indicators of disease outcomes, grip strength, and functional grade. Psychiatric illness was also not related to disease duration. Using the SF-36 physical summary score as the outcome, Kojima et al. (2009) found that while psychological distress was associated with physical functioning in bivariate analyses, this association disappeared at a multivariate level with only current symptom and physical status predictive of SF-36 physical quality of life.
Similar findings have been obtained in OA. Using a publicly and privately funded prospective cohort study of adults aged 45–79 designed to examine onset and progression of knee OA, Riddle, Kong, and Fitzgerald (2011) found that depressive symptoms were an independent predictor of yearly change (over 2 years) in self-reported disability, walking distance, and chair stand performance in addition to pain. However, while statistical significance was obtained, the authors suggested that the findings were not clinically significant. Examining the prognostic impact of depressive symptoms on future pain and functioning, the authors found that depression was required to be chronic and persist for multiple years in order to produce a meaningful impact on future pain and disability.
On the other hand, another longitudinal study of community-dwelling individuals (n = 257) (Sharma et al., 2003) found that baseline factors associated with poor functional outcome (measured by the Western Ontario and McMaster osteoarthritis index [WOMAC]) at 3 years included higher Body Mass Index, greater knee pain intensity, increased laxity, and reduced aerobic exercise, as well as lower psychosocial functioning in terms of mental health, self-efficacy, and social support. The impact of psychological distress on functional outcomes appears to be latent, with pain intensity the only baseline factor to predict functioning at 18 months. In terms of chair-stand performance, there was no difference between those with poor and those with good WOMAC scores. Self-efficacy was the only psychosocial factor that contributed to both 3-year self-reported functional decline and objective chair-stand performance. Importantly, differences in self-efficacy between those who sustained high functioning over time compared to those that saw a decline or sustained low function were the largest of any predictor. This finding is supported by other longitudinal research (Rejeski, Miller, Foy, Messier, & Rapp, 2001).
Pain and Disease Activity
In chronic pain patients, poor psychological functioning is generally associated with more pain sites, pain intensity duration, and severity and interference (Bair, Robinson, Katon, & Kroenke, 2003; Bair, Wu, Damush, Sutherland, & Kroenke, 2008). In arthritis, most studies have examined the role of pain on psychological outcomes as opposed to the reverse. In an early clinical study of 400 RA patients attending a rheumatological clinic on average for 3 years, Hawley and Wolfe (1988) found that depression and anxiety were associated with number of outpatients visits, while depression (although highly correlated with anxiety) contributed to continued high levels of pain at follow-up. Meanwhile, in a longitudinal analysis of 238 patients with RA (aged 20–70), Odegard et al. (2007) found that anxiety alongside female gender, disease activity (defined as ESR), and physical function (measured by grip strength) independently explained the course of pain over the 10-year study period. While depression and anxiety were found to be interrelated longitudinally, depression (measured by the AIMS or General Health Questionnaire) did not contribute to the final model. These findings were consistent using two different measures of pain (VAS and AIMS).
In another study focused on early inflammatory arthritis, Looper et al. (2011) found that patients with a history of major depression had higher overall disease activity. Importantly, joint symptoms measured by the DAS28 showed significantly higher values according to depression history for both patient and physician assessment of the illness. Objective disease indicators such as tender and swollen joints and CRP levels were not related to depression history. Likewise, pain was not associated with depression history. This contrasts with an earlier study of 188 postmenopausal women with RA and OA (Zautra & Smith, 2001). In this study, Zautra and Smith found that increased pain sensitivity was associated with depressive symptoms. More specifically, weekly pain reports in RA patients were predicted by depressive symptoms, perceived stress, and an interaction between perceived stress and depression. For those with OA, weekly pain was predicted by independent associations of depression and perceived stress, with no interaction noted. The differences in findings between the two studies may have been related to how depression was classified (recurrent as opposed to history) and the population studied.
In a later study examining the effects of depression and anxiety on weekly pain in a mixed RA and OA sample, Smith and Zautra (2008) found that when examined separately, depression and anxiety had similar effects on the reporting of weekly pain, both current and next week (although the effects were nearly twice as large for anxiety). However, when examined in concert, depression was reduced to nonsignificance. This finding was supported by Harris et al. (2012) who examined the relative effects of self-reported diagnosed depression and anxiety in arthritis within a comprehensive model.
The impact of psychological factors on physical outcomes has less often been examined in an OA only population. Kim et al. (2011), in a cross-sectional study of 660 older Koreans with knee OA, found that coexisting depression was associated with knee pain. The strength of this relationship (after adjustment for confounders) was as strong as pathomorphologic damage. Particularly, the presence of depression was associated with a six-fold increase in reporting symptomatic knee OA. However, this influence was only noted in patients with minimal to moderate radiographic severity (measured by the Kellgren–Lawrence grading system). The presence of a depressive disorder was not associated with the risk of symptomatic knee OA in patients with severe OA (Kellgren–Lawrence grade 4). As a result, the authors argued that the findings suggested that depression contributes substantially to the discrepancy between symptoms and radiographic degenerative changes observed in knee OA.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




