Trauma-Informed Perspective
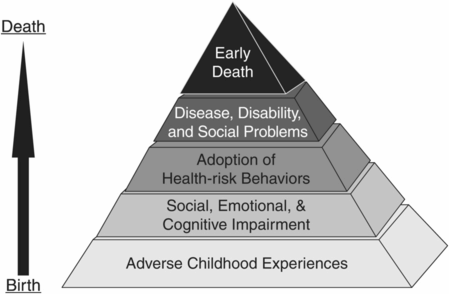
There is growing recognition that trauma is widespread, and that the experience of trauma has far-reaching effects on a person’s physical and mental well-being. The Adverse Childhood Experience (ACE) Study, utilizing a 10-item survey, found a powerful relationship between the number of traumatic incidents individuals had experienced prior to the age of 18 and their developmental challenges and chronic health conditions [4]. The items of the original ACE survey underscore that not only is trauma historical in nature, but it is also largely interpersonal, e.g., physical or sexual abuse at the hands of a family member or disrupted attachments due to parental death, incarceration, or substance abuse.
The TPR approach to treating violence starts with the recognition that the behaviors that lead to inpatient psychiatric care, e.g., violence to self or other, are a person’s best attempt to communicate or mitigate the innumerable effects of the traumas they have experienced (see Figure 28.2). Among people with severe mental illness, the sheer pervasiveness of trauma, estimated to be as high as 90%, is staggering and requires us to assume that trauma is a universal experience among people served on our state psychiatric inpatient units [5]. The implication is that more than 90% of persons served have suffered some form of significant pain, loss, and fear, often at the violent hands of another. Assessing and treating violence as a direct consequence of trauma is but the first step on that journey of recovery.
Assessment
Equally central to TPR is the observation that “violence is a process, not an act” [6]. In order to accurately address violent behavior for a particular individual, a wider lens is needed to assess and understand the context and risk for violence. The public health model of violence defines three levels of violence: organizational/institutional (e.g., stigma, discrimination); structural (e.g., unemployment, involuntary hospitalization); and direct (e.g., trauma) [7] (see Table 28.1). Violence is the synergistic culmination of individuals interacting with each other and the environment, each operating from their cultural affiliations and status within society overall, their relationships and trauma history, and their individual intrapsychic schemas [8]. Inpatient psychiatric units comprise miniature communities within which all three levels of violence (institutional, structural, and direct) are operating and relevant. A narrow focus on direct violence with little regard to the contributions of institutional and structural violence limits the efficacy of any intervention or treatment modality.
| Public health prevention model | Threat assessment prevention model | |
|---|---|---|
| Primary | Institutional | Universal |
| Secondary | Structural | Identifying those at risk |
| Tertiary | Direct | Intervening in an act of violence |
Within the field of violence risk assessment, the concept of threat assessment focuses on preventing violence within a community or institution. Threat assessment, consistent with the public health prevention model of violence, is organized into three levels of prevention: (1) primary (creating a community-wide climate that mitigates institutional violence and supports the commitment to nonviolence, (2) secondary (reducing structural violence by identifying and intervening with people at risk), and (3) tertiary (utilizing violence-specific interventions with people who are persistently violent).
Primary prevention at the culture of care level
The National Association of State Mental Health Program Directors (NASMHPD) has been the leader in emphasizing that the path to reducing violence on inpatient psychiatric units is to transform the authoritarian, controlling culture, which is too common among inpatient units, into a TPR culture [1,5]. NASMHPD clearly places the locus of change within the organizational culture, as the mechanism necessary to reduce violence and associated restraint and seclusion episodes [5]. A TPR culture of care may ameliorate the larger socioeconomic and cultural effects of institutional and structural violence, and thus reduce triggers for direct violence. Organizational expectations, values, and actions can influence the exhibition of challenging, aggressive, or violent behavior or they can encourage its prohibition. When a unit is motivated and committed to making changes, interventions are even more effective at reducing rates of violence. Fortunately, even when unit motivation is low, reduced violence rates are observed as a consequence of changes in the culture of care [3,9].
(1) Leadership commitment to TPR culture of care
In creating a TPR care delivery environment, the very process of culture change must reflect these principles across all organizational levels. Successful systems have engaged organizational leadership, frontline staff, and persons served in the process of direct change [3]. Staff supported in the pursuit of their own growth and development activities can foster this in others [10]. Also, those who are invested in the agency’s mission are more likely to remain consistent with the interventions, modalities, and protocols associated with the overarching vision [5].
(2) Staff training
(a) Given the pervasiveness of trauma, one of the first steps in the promotion of TPR culture of care is staff training. Staff should receive training on the etiology and universality of trauma, trauma’s neurobiological sequelae, and implications for the nature and timing of early intervention and de-escalation strategies [11,12].
(b) Since the therapeutic alliance is integral to recovery, recovery-based communication styles must be taught. Staff who utilize therapeutic approaches of compassion, empathy, and respect reduce violence motivated by fear, anger, and shame [13]. Training in low Expressed Emotion communication style, e.g., avoiding verbal and nonverbal criticism, hostility, or over-intrusive, paternalistic attitudes; using supportive and nonthreatening methods for limit-setting; and emphasizing positive rather than negative communications, has been associated with a reduction in rates of restraint and seclusion [3].
(c) Staff should be trained to respond to an individual who is experiencing distress in order to avert escalation and possible violence. Utilization of noncoercive de-escalation and crisis intervention techniques is associated with reduced violence and fewer episodes of restraint or seclusion [14–17].
(d) Safety, Hope, and Healing (SHH) is a model developed by the Massachusetts Department of Mental Health for training staff that assumes that trauma is pervasive and influences many aspects of human behavior including violence. SHH involves four key components: (1) knowing the individual, (2) knowing the environment, (3) knowing yourself, and (4) knowing society. Importantly, SHH empowers staff to understand their own histories, triggers, and risk factors, as well as those of persons served, as a vehicle for identifying and mitigating potentially dangerous situations. These tools enable staff to better understand, make meaning of, and predict violence, thereby increasing personal and organizational safety and fostering hope for both staff and persons served. This approach supports an individualized formulation and treatment plan for recognizing and responding to the contextual fluctuations in risk for violence, and allows for an accurate contextually based evaluation of historical, intrapsychic, and interpersonal factors at play in any given interaction at any given moment.
(3) Staff supervision and support
Staff members require ongoing training, supervision, and support in order to respond effectively to a person’s level of distress. The intensity of people’s need, despair, fear, shame, loneliness, or rage can be overwhelming, and may lead staff to recoil and distance themselves from their own intolerable feelings, which are often engendered by fear of professional inadequacy or fear for personal safety. Psychosocial interventions for staff include trauma-informed supervision, tertiary trauma and employee assistance services, and self-care and wellness activities that replenish staff and lead to higher work satisfaction. These interventions result in fewer negative encounters, including violence, as the result of staff compassion fatigue, vicarious trauma, and burnout [10].
(4) Modifying environmental factors
Violent incidents are lower on units where staff members have clear job descriptions and role expectations, and when staff are visibly present and actively engaged on the floor rather than sequestered in the nurses’ station. The physical presence of unit and organizational leaders and predictable schedules filled with meaningful activities are associated with lower rates of violence [18].
(5) Systematic review of violent episodes
Systematic attention and review of past violent episodes have been associated with reductions in future violent episodes. Multidisciplinary consultation teams, with an eye toward reducing violence, consult on persons served who repeatedly exhibit challenging or unsafe behaviors, or who have had multiple episodes of seclusion or restraint. Formal debriefing of the involved persons served and staff is especially effective when a peer specialist participates in the debriefing. The use of multidisciplinary feedback teams who review each violent incident for alternatives to restraint and seclusion decreases unwarranted restraint and seclusion episodes [3].
Secondary prevention at the culture of care level
In a TPR culture of care, secondary prevention efforts target the reduction of violence through identifying people at higher risk for violence, intervening to treat factors that increase vulnerability to violence, and monitoring risk status regularly and persistently over time. A comprehensive violence prevention assessment is ongoing and utilizes standardized measures; clinical observation; and collaboration, engagement, and empowerment with the person served [19,20]. Staff monitor both the universal indicators for potential escalation, as well as an individual’s specific contextual triggers and indicators of escalating risk. When done in collaboration with the person served, this model proves to be more effective as individuals learn to accurately assess their own ongoing fluctuations in stress, triggers, and coping resources.
(1) Standardized assessment of universal risk factors
A person is most at risk for violent behavior in the first 3–4 days of admission [9,21]. A standardized violence risk assessment, e.g., the Brøset Violence Checklist, is most effective, given that the person served is new and not well known or understood by staff [22]. Systematic risk assessment upon admission can differentiate people at greatest risk for violent behavior [23]. Systematic and frequent risk monitoring (e.g., twice daily) during the first 3–4 days of a person’s admission is associated with decreased rates of violent episodes [24,25].
The formalization of risk assessment procedures affects the culture of a unit in several intangible ways as well. Regular review of the risk assessments promotes more effective intra- and inter-team communication and treatment planning. Staff knowledge and attention to the universal indicators of violence risk is increased and the direct focus on early intervention supports the use of more effective strategies for de-escalation [9]. In one study, the number of severely aggressive incidents was unaffected; however, staff assessed these incidents as less severe, suggesting that systematic risk assessment increased staff’s confidence in their ability to manage the risk for violence [16].
(2) Individualized formulations of violence risk
Traditional, systematic risk assessment is integral to violence prevention efforts, but must be supplemented with other modalities and types of assessment in order to increase efficacy. With TPR systems of care, violent behavior is conceptualized as a “message,” be it to the self or others. In order to understand the meaning of a person’s violent behavior, a multidisciplinary approach is necessary to uncover the connections between the individual, the situation at hand, the setting, and the target of the violence. Attention to the relevant institutional and structural violence a person is subject to further informs this formulation. It requires a more dynamic focus and “an investigative, skeptical, inquisitive mindset” [6].
(3) Therapeutic alliance
A powerful vehicle for preventing adverse events like violence is knowing the individual based on a nonstigmatizing therapeutic relationship built over time. Through this relationship, staff are aware of the meaningful aspects of an individual’s history and are able to predict potential triggers, recognize early signs of difficulty, and utilize individual-specific interventions to avert escalation. Through this lens, the question becomes how to understand an individual’s current presentation against the backdrop of “what happened to you?” rather than “what’s wrong with you?” and shifts the paradigm even further to asking “what’s strong in you?” [26]
(4) Collaborative monitoring
A person’s risk status is fluid; it is not a static state. At any given moment, an individual’s level of risk is specific to his/her present emotional state, motivational attributions, interpersonal reactivity, internal coping mechanisms, external sources of support, and the level of distress and hopelessness he/she is experiencing. Staff and persons served can utilize knowledge of the individualized formulation of violence risk to collaborate in the monitoring and early intervention process.
Psychosocial Interventions to Address Risk Factors Associated with Violence
Psychosocial interventions that address the underlying risk factors associated with risk for violence and foster a strength-based understanding of trauma are an essential component of secondary prevention of violence.
Treatment delivery in a TPR system of care is based on two core principles [27].
(1) Delivery of treatment reflects systemic awareness of the pervasiveness of trauma, the recognition of the impact of trauma on the individual, and an organizational responsiveness to that knowledge.
(2) Treatment includes an integrated continuum of trauma-specific modalities to address the immediate cognitive, somatic, and emotional distress experienced by the person served and to foster long-term hope and recovery.
Cognitive behavior therapy (CBT)
CBT is the most widely studied modality of psychotherapy in the field of violence prevention, although other forms, e.g., psychodynamic psychotherapy, are also effective [28]. Most CBT approaches emphasize the ability to (a) recognize internal and external triggers; (b) observe and manage one’s cognitive and emotional responses; and (c) resolve interpersonal conflict and negotiate getting one’s needs met. CBT helps the person served to recognize the power of his/her own thoughts, particularly interpersonal/relational triggers, cognitive distortions, and the possibility of alternative interpretations (see Table 28.2). As cognitions shift, people’s associated feelings of inadequacy, inferiority, and hopelessness also shift, and the possibility of recovery increases. CBT components that address the psychological factors that underlie violence, including fear, anger, and shame, empower an individual to resume a self-regulated life course.
| Cognitive skills | Training on general thinking and decision-making skills such as to stop and think before acting, generate alternative solutions, evaluate consequences, and make decisions about appropriate behavior |
| Cognitive restructuring | Activities and exercises aimed at recognizing and modifying cognitive distortions and errors that trigger violence |
| Interpersonal problem solving | Training in problem-solving skills for dealing with interpersonal conflict and peer pressure |
| Social skills | Training in prosocial behaviors, interpreting social cues, taking other persons’ feelings into account |
| Anger control | Training in techniques for identifying triggers and cues that arouse anger and maintaining self-control |
| Relapse prevention | Training on strategies to recognize and cope with high-risk situations and halt the relapse cycle before lapses turn into full relapses |
| Moral reasoning** | Activities designed to improve the ability to reason about right and wrong behavior and raise the level of moral development |
| Victim impact** | Activities aimed at getting people to consider the impact of their behavior on others |
Sensory modulation interventions
More recently, there has been increased recognition that in order for most CBT to work, one must include attention to the body because people who are physiologically aroused have difficulty utilizing cognitive strategies [29]. People with mental illness are frequently less aware of their own physiological and sensory experiences [30]. Identifying sensory triggers and physiological reactivity are essential to any effort to understand the antecedents of a violent episode and to develop person-specific strategies for early intervention and de-escalation. Teaching someone to recognize the changes in their own sensory experience enables them to more fully participate in the recovery process. Sensory modulation techniques allow for the creation of individualized tools to manage one’s own physiological state. It is much easier for a person served to make their way in the world using personalized sensory tools under their conscious control than to rely on the presence of a staff member to do the same. Sensory modulation methods allow for choice and empowerment and decrease the sense of shame associated with being “less than” or “dependent.” Empowering someone to use sensory strategies to self-regulate their level of arousal promotes self-efficacy. Inpatient units have introduced “sensory rooms” that provide a calming space with avenues for soothing and arousing each sense [31].
Interventions based on the presenting emotions
Shame
Symptoms and behaviors that are triggered via a shame-based mechanism respond best to cognitive interventions within a “socio-ecological framework” [5]. Skill-based modalities that target the need for control, mastery, and meaningful purpose foster pride and self-respect. Cognitive restructuring and enhancing therapies, motivational interviewing, stress management, vocational training, community outreach, and access to housing and higher education all counteract the negative messages that persons served have experienced via institutional and structural violence (see Table 28.3).