Fig. 8.1
Conceptual path model for resilience in chronic pain (adapted from Sturgeon & Zautra, 2010)
Although the aforementioned model of resilience in chronic pain can help to organize the multitude of factors that predict positive functioning in chronic pain, some aspects of this model would benefit from further development. For example, paying greater attention to the phenomenological experience of pain, understanding the nature of pain adaptation from the perspective of the sufferer and giving weight to both person-centered and contextual factors in adaptation, may enhance our understanding of chronic pain (Karoly & Ruehlman, 2006; Masi, White, & Pilcher, 2002). Though experimental and observational studies serve an important purpose in identifying and clarifying processes related to positive pain adaptation, the clinical and empirical utility of such models may be limited if they do not meaningfully reflect the experience of pain by the sufferer. This perspective can help to highlight important new areas of inquiry that have remained dormant in existing models. For example, there is a large body of literature that has emphasized the context of pain coping. Though the social context of pain experience has rightfully garnered increased attention in recent years, there is also an expanding body of literature that examines the roles of goal orientation (Ceulemans, Karsdorp, & Vlaeyen, 2013a, 2013b; Coffey, Gallagher, Desmond, & Ryall, 2014) and reward processing in pain (Becker, Gandhi, & Schweinhardt, 2012; Leknes & Tracey, 2008) that may underlie chronic pain processing and adaptation. In many cases, individual goals and the perception of reward involve and interact with interpersonal processes to promote resilience to pain, thereby shaping the experience of the pain sufferer and direct their coping efforts accordingly. Examining contextual goals and reward processing in chronic pain can help to explain many of the subtleties that are inherent in explaining resilient responses to pain from a motivational standpoint, which has remained a relatively understudied area of pain adaptation (Crombez, Eccleston, Van Damme, Vlaeyen, & Karoly, 2012).
Additionally, chronic pain may place a higher demand on an individual’s self-regulatory processes (Solberg Nes, Carlson, Crofford, de Leeuw, & Segerstrom, 2010). The role of self-regulation is key to understanding how individuals with chronic pain are able to override tendencies to avoid pain and to continue to function meaningfully. However, these resources are not boundless, and the process of depletion and recovery of self-regulatory resources may help to explain the trajectories of adaptation inherent within chronic pain. We will pay particular attention to the construct of fatigue, which may reflect a state of depleted self-regulatory resources and may also serve as a significant barrier to functioning in chronic pain.
In sum, this chapter will examine multiple factors that contribute to resilience to pain by identifying specific contributors to sustainability, recovery, and growth. We will also examine the importance of the timeframe of pain adaptation and the very human contexts, both within the person in terms of idiosyncratic goals and motivations and the social relationships that support or interfere with adaptive responses to episodic pain.
Characterizing Sustainability Processes
Defined in terms of chronic pain resilience, sustainability refers to continued positive engagement: the persistence in valued activities in the presence of pain (Sturgeon & Zautra, 2010). Traditionally, studies have examined pain tolerance, which may function as a marker of sustainability. Pain tolerance has been acknowledged as an important factor in resilience in past studies (Karoly & Ruehlman, 2006; Zautra et al., 2005), and there is a logical connection between pain tolerance and sustainability in the face of pain. Individuals who cannot tolerate their pain are, by definition, unlikely to function effectively in its presence. Experimental studies have identified a variety of factors that can modify pain tolerance, including cognitive strategies (Fernandez & Turk, 1989), and a number of variables that predict individual differences in pain tolerance, including gender (Riley, Robinson, Wise, Myers, & Fillingim, 1998), genetic dispositions (Compton, Geschwind, & Alarcon, 2003), emotional temperament (de Wied & Verbaten, 2001), and medication use (Skarke, Darimont, Schmidt, Geisslinger, & Lotsch, 2003). Pain tolerance also shows some utility as a clinical construct, as it has been found to predict treatment response following multidisciplinary interventions for chronic pain (Edwards, Doleys, Lowery, & Fillingim, 2003).
Though useful, pain tolerance has too limited a range to encapsulate resilient responding. Tolerance of induced pain in an experimental setting may not generalize to living with chronic pain (Sturgeon & Zautra, 2013a). Furthermore, indiscriminant persistence when in pain is not inherently adaptive. Put simply, resilience to pain is neither necessary nor likely in cases where the ultimate outcome is of little importance to the pain sufferer; the goals of the individual uniquely identify his or her resilience agenda. Pursuit of valued goals can serve to enhance positive emotions and buffer against negative emotions in the context of dealing with a painful medical condition (Coffey et al., 2014). Similarly, optimism and hope, which reflect an ability to identify one’s goals and to identify the ways to reach these valued goals, are important predictors of positive functioning despite pain (Hood, Pulvers, Carrillo, Merchant, & Thomas, 2012; Wright et al., 2011). Higher levels of optimism have been found to be protective against pain, emotional distress, and catastrophic thinking (Bruce et al., 2014; Hanssen, Peters, Vlaeyen, Meevissen, & Vancleef, 2013) and reduce the deleterious effects of pain on higher-order cognitive functioning (Boselie, Vancleef, Smeets, & Peters, 2014). Indeed, optimism has also been shown to sustain behavioral efforts in a painful task (Solberg Nes, Carlson, Crofford, de Leeuw, & Segerstrom, 2011).
Recently, research has taken steps to clarify the role of goal orientation in sustainability processes using experimental paradigms. The Mood-As-Inputmodel posits that individuals use information gleaned from their emotional states to determine whether to persist or discontinue engagement in an indefinite task (Ceulemans et al., 2013b). Hedonic goals , such as an innate and immediate desire to continue performing a task, can enhance persistence in that task (Ceulemans et al., 2013b), as does the interpretation of a painful task as a challenge (Jackson, Wang, & Fan, 2014) or in terms of achievement (Karsdorp, Ranson, Nijst, & Vlaeyen, 2013). Further, individuals will also persist in a painful task for longer periods if they are acting according to a sense of personal responsibility (Ceulemans et al., 2013a); this finding may suggest that the presence of eudaimonic goals, which are less concrete and oriented towards outcomes that are abstract or occur in the longer term than hedonic goals, may also enhance persistence. Interestingly, negative emotions may also provide an initial impetus for persistence despite pain, as persistence in a painful task was found to be higher for individuals with higher induced levels of negative emotion (Ceulemans et al., 2013a). However, the motivating effects of negative emotion come at a cost to adaptation; more intense negative emotional states in these experiments were also predictive of higher levels of reported pain later in the procedure (Karsdorp & Vlaeyen, 2011). These studies suggest that cognitive interpretation, goal orientation, and emotional states may modify the willingness of an individual to function under painful conditions, and these effects may be relatively independent forces (Ceulemans et al., 2013a). Although these studies provide valuable support for the importance of goals in sustainability, we do not yet know whether these effects can be generalized outside of an experimental setting and whether they persist over time. Similarly, most of the evidence for the Mood-As-Input model has been gleaned from healthy individuals. Though promising, the importance of goal orientation in resilience to chronic pain awaits further study with clinical populations.
Another valuable model of sustainability can be borrowed from a recently proposed model of stress resilience (Smith, Epstein, Ortiz, Christopher, & Tooley, 2013). Smith and colleagues propose a temporal model of resilience, in which individuals undergo a sequential process of confronting a stressful event, identifying a desired outcome, and mobilizing coping efforts. This model of resilience is valuable, both because it incorporates time as an important factor in resilience and also implicates different variables in the promotion of resilience at each stage. The authors posit that mindful awareness and clarity of mood enhance the ability of an individual to initially confront a stressful event, optimism and a purpose in life help to identify a desired future event, and active coping strategies and social support help the individual to mobilize coping efforts. This model of resilience can be reasonably applied to the experience of pain as well: as individuals experience a new pain or a flare in their existing pain, they may be able to employ similar strategies in orienting to pain, identifying a desired goal, and mobilizing coping efforts for pain in a more coherent way. In terms of resilient responses to chronic pain, however, this model may require expansion across a longer span of time, as the experience of stressful experiences of pain may not be discrete events and may not resolve completely. Many individuals with recurrent pain do not experience an end to the experience of their pain and, thus, may not be able to adequately recover from the exposure to the stressful event in the same way as they might from an acute stressor.
A related system underlying sustained functioning in the face of pain is the perception and pursuit of reward. A recent review of the overlap of pain and reward systems in the brain suggests that chronic pain has implications for both the hedonic and motivational aspects of reward processing (Becker et al., 2012). Becker et al. discuss the “Motivation-Decision Model” of pain and reward, which explores the immediate and often unconscious prioritization of competing impulses of pain-related escape and reward pursuit. As an acute pain signal acts as a potent signal to stop or avoid a painful stimulus, the value of a reward stimulus must exceed the impulse to escape a painful stimulus if the organism is to employ a non-avoidant behavioral response. This model provides an intuitive and important concept in explaining the phenomenon of persistence through painful experiences in humans; in order for an individual to persist in a task that is causing him or her pain, the individual must be able to perceive or call to mind an impending or likely reward that is more salient than the experience of pain.
The Motivation-Decision Model also holds value in conceptualizing chronic pain, as it provides a perspective on how patterns of behavior develop in chronic pain as a function of operant learning (Leknes & Tracey, 2010). By understanding how maladaptive behavioral patterns develop in chronic pain, we can better define the meaning of sustainability from the perspective of the pain sufferer. It has been posited that pain relief may function as a salient reward. There is evidence to support this claim; reward and pain relief demonstrate similar patterns of activation in the orbitofrontal cortex and nucleus accumbens (Becker et al., 2012). Considered from an operant learning perspective, pain relief appears to function as a reward through negative reinforcement, or increasing the likelihood of a behavior by removing an aversive or noxious stimulus, while increases in pain serve as a punishment, which introduce a noxious stimulus like pain. This perspective can help to explain the initial development of unhealthy or maladaptive behavioral patterns after the onset of pain, such as behavioral avoidance: if each time an individual engages in physical movement, they also experience an increased level of pain, a natural consequence of this pattern would be an increase in learned avoidant responses. This pattern would be further reinforced by the relief experienced by individuals when they are not performing those activities that cause increases in their pain. Such responses may be adaptive in the case of acute pain, as individuals could be expected to experience activation in their reward processing circuits when they are able to successfully escape danger, thereby reinforcing behavior that will promote safety in the future.
However, the implications of reinforcing avoidant behaviors become more sinister in the case of chronic pain. As the pattern of pain experience becomes chronic, expectancy of increased pain may develop, making more salient those occasions when pain is absent or at a lower level. This pattern may thus reinforce learned responses to pain that are adaptive in the short term (i.e., through avoidance of or relief from pain), but are problematic in the long term; there is ample evidence that behavioral avoidance enhances the risk of longer-term disability in individuals suffering from a chronic musculoskeletal pain condition (Vlaeyen & Linton, 2000).
The difficulty of sustainability in the face of recurrent pain, then, becomes apparent: resilient responses to chronic pain necessitate identification of important goals whose value exceeds the value of short-term relief from pain. As individuals continue to make decisions about whether to persist in or avoid an activity that exacerbates their pain but may yield another reward, the feedback from these decisions, such as temporary relief from pain or achieving their desired goal, will then reinforce the decision that is made. This process of chosen behavior and reinforcement will then inform future decisions about whether to approach or avoid opportunities when they arise. When individuals are faced with an opportunity to pursue a meaningful goal, but also maintain an expectation that goal pursuit will be accompanied by increased pain, their decision to persist or discontinue their pursuit will be contingent on the rewards they received from previous attempts at goal pursuit or avoidance (see Fig. 8.2). From an operant perspective, those individuals who prove to be resilient to their pain are those who pursue opportunities and are sufficiently reinforced by reaching them. As a result, they become willing to tolerate pain in order to reach a greater reward in the future.
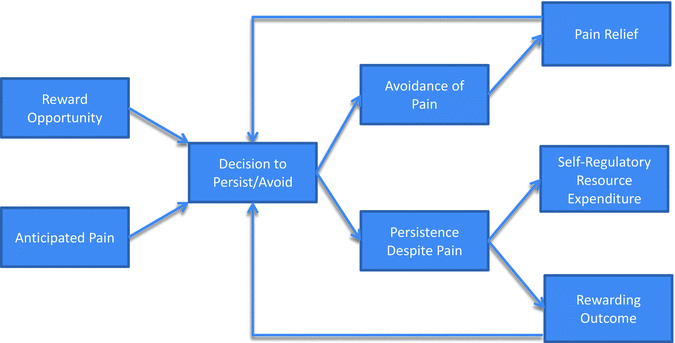

Fig. 8.2
Process of sustainability in chronic pain
Though it is often said that chronic pain is pain that has lost its utility as a biological signal (as it no longer signals continuing damage or dangerous physical changes in the body), it retains some value as a harbinger of future symptoms in the framework of coping with pain in the long term. More specifically, those individuals who disregard their level of pain and attempt to significantly increase their level of activity despite their pain typically demonstrate poorer overall functioning across time (McCracken & Samuel, 2007). Yet, those individuals who attempt to avoid physical activity because of their pain may experience increased pain through deconditioning if they attempt to disregard their pain completely. These patterns of pain coping would suggest that there may be an optimal level of physical activity in which in individual can engage that balances the immediate costs of physical exertion with the long-term benefits of activity (Karsdorp & Vlaeyen, 2011). This concept has been used as a basis for developing behavioral pacing strategies, which are a hallmark intervention of cognitive-behavioral therapy for pain (Keefe, 1996). Curiously, however, even pain-coping styles that center on attempts to pace oneself may predispose an individual to poorer overall functioning (McCracken & Samuel, 2007). Instead, effective sustainability despite pain appears to be dependent on multiple coinciding psychological factors, including a low level of behavioral avoidance, in conjunction with high levels of both physical activity and acceptance of pain (McCracken & Samuel, 2007). In short, the process of sustainability in chronic pain must: (1) engage reward processes oriented towards approach-type or active behaviors; (2) be sensitive enough to immediate, activity-related changes in pain, allowing the individual to persist in these goals across time without the occurrence of significant worsening of pain itself; and (3) maintain a low level of emotional distress related to the experience of pain itself.
Fatigue and Recovery Mechanisms in Chronic Pain
An underappreciated aspect of resilience in chronic pain is the capacity to recover from the deleterious consequences of pain. The costs of sustained functioning despite the presence of significant pain may demand a greater capacity for self-regulatory resources than in healthy individuals, which may manifest in reports of greater fatigue (Solberg Nes et al., 2010). We suggest that fatigue, which is a complex construct comprised of behavioral, cognitive, and emotional components (Nes, Ehlers, Whipple, & Vincent, 2013), should also be understood as a failure of recovery processes in chronic pain. Fatigue has been reported as a significant barrier to functioning and quality of life in osteoarthritis (Murphy, Smith, Clauw, & Alexander, 2008) and rheumatoid arthritis (Pollard, Choy, Gonzalez, Khoshaba, & Scott, 2006), as well as several other chronic pain conditions (Burke, Elliott, & Fleissner, 1999; Feuerstein, Carter, & Papciak, 1987; Kop et al., 2005). Fatigue is also significantly related to anxiety (Roy-Byrne et al., 2002) and shows a reciprocal relationship with depression, such that individuals with complaints of fatigue appear to be at increased risk of developing a future major depressive episode (Addington, Gallo, Ford, & Eaton, 2001), and individuals with depression are more likely to report significant fatigue in the future (Skapinakis, Lewis, & Mavreas, 2004).
Although it is logical to expect fatigue to present a challenge to overall functioning, its role in daily life for an individual with a chronic pain condition is not always appreciated. For example, individuals with chronic pain may be informed by their medical providers about the positive effects of physical exercise for their health, even with recurrent pain. Consequently, many individuals with pain may seek to follow this advice and incorporate greater levels of physical activity into their daily lives and may ultimately experience long-term benefit. Experientially, however, incorporating higher levels of physical activity for an individual with chronic pain may be more difficult than for an individual without chronic pain for several reasons. First, individuals with chronic pain are faced with the task of overcoming a natural impulse to avoid activity and further pain if their symptoms flare up in response to physical activity; this impulse, while frequently adaptive in response to acute pain, may also contribute to longer-term deconditioning and later worsening the experience of pain (Asmundson, Norton, & Norton, 1999). Further, the process of re-introducing physical activity itself into a routine devoid of exercise may initially require significant regulatory effort, as individuals with chronic pain may face increased levels of physical deconditioning if they have fallen into a pattern of behavioral avoidance that frequently accompanies chronic pain conditions (Vlaeyen & Linton, 2000). Additionally, the experience of pain itself may deplete the availability of these self-regulatory resources; individuals with some chronic pain disorders, such as fibromyalgia and temporomandibular joint disorder, demonstrate chronically elevated levels of self-regulatory fatigue, which appear to be partially explained by the intensity of their pain (Solberg Nes et al., 2010). Thus, as a natural consequence of returning to a higher level of physical activity, individuals with chronic pain may experience immediate or prolonged states of regulatory depletion, which may manifest as fatigue (Hagger, Wood, Stiff, & Chatzisarantis, 2010; Segerstrom & Nes, 2007; Solberg Nes et al., 2010; Sturgeon, Yeung, & Zautra, 2014).
As noted previously, some individuals may be prone to maladaptive attempts to excessively increase their levels of physical activity without regard for their level of deconditioning or the severity of their physical symptoms, thereby exacerbating these symptoms (McCracken & Samuel, 2007). In this instance, individuals may appear to be demonstrating some aspects of resilience through sustainability, in that they continue to function despite their pain for a period of time. However, they may be simultaneously demonstrating failures in recovery, as their attempts may prove unsuccessful in the long term because of the unsustainable intensity of activity and disregard for future symptoms, which may make continued functioning progressively more difficult. The role of recovery is particularly important in this case, as resilience cannot continue indefinitely; even the positive effects of optimism on persistence in a painful task can be compromised by those individuals dealing with greater depletion of their self-regulatory resources (Solberg Nes et al., 2011).
Although individuals with chronic pain may be susceptible to greater depletion of their self-regulatory resources, there are several factors that have been implicated in effective recovery from pain. One important factor for recovery is positive emotion. Positive emotion has been implicated in resilience in a multitude of ways. Broadly, positive emotions aid in recovery from cardiovascular disease (Fredrickson & Levenson, 1998), emotional (DeWall et al., 2011; Tugade & Fredrickson, 2004), and cognitive (Boselie et al., 2014) recovery from stress and also appear to have beneficial effects for the immune system (Pressman & Black, 2012). Positive emotional states also appear to enhance cognition, as happier individuals are better able to think broadly and flexibly than they might under conditions of greater emotional distress (Fredrickson, 2001). Similarly, bolstered positive emotional states appear to underlie some of the cognitive benefits of optimism (Boselie et al., 2014). Individuals with chronic pain who are better able to sustain their positive emotions report less intense pain clinically and under experimental conditions (Finan, Quartana, & Smith, 2013) and appear to be less susceptible to catastrophizing about their pain (Hood et al., 2012) and to behavioral avoidance due to fear of their pain (Meulders, Meulders, & Vlaeyen, 2014). Individuals with an induced positive mood are also able to persist for longer periods under painful conditions (Karsdorp et al., 2013). Positive emotional states also appear to be a mechanism of resilience against problematic and habitual opioid medication misuse in individuals with chronic pain (Garland et al., 2014). Importantly for the purposes of resilience, there exists some evidence for the restorative effect of positive emotions for self-regulatory resources. A mutually influential relationship between positive states like enjoyment and levels of fatigue emerges in daily diary models, suggesting that increased levels of enjoyment may predict lower levels of later fatigue (Yeung, Aiken, MacKinnon, & Davis, 2014). Positive emotions thus appear to be a salient recovery factor in chronic pain.
Another key mechanism of recovery in chronic pain is sleep. Sleep quality, like resilience, is a multidimensional construct with effects in the behavioral, cognitive, affective, and physiological domains, and individual differences in sleep processes have been implicated in resilient coping. Sleep also plays a vital role in the development of memories and insight formation (Ellenbogen, 2005) and may be involved in the repair of damaged cells and neurons (Savage & West, 2007). Sleep quality has been associated with a variety of additional benefits, including lower fatigue (Bliwise, 1992) and lower psychological distress (Shaver & Paulsen, 1993). Good-quality sleep has also been implicated in enhanced physical (Haack & Mullington, 2005) and psychological recovery (Hamilton et al., 2008). Conversely, individuals with chronic pain who report more problematic sleep are more likely to experience significant pain (Finan, Goodin, & Smith, 2013), fatigue (Fishbain, Hall, Risser, & Gonzales, 2009), and poorer physical functioning (McCracken & Iverson, 2001). Greater sleep disruption also appears to be associated with greater complaints of both pain intensity and unpleasantness (Morin, Gibson, & Wade, 1998); this relationship may be informative with regard to the ways in which sleep enhances resilient responses to pain, as the ability to modulate attention towards and away from pain appears to be dependent to some degree on the quality of sleep (Affleck, Urrows, Tennen, Higgins, & Abeles, 1996, Edwards et al., 2003). Notably, sleep quality has also been implicated in the maintenance of positive emotional states in chronic pain (Hamilton, Catley, & Karlson, 2007), further strengthening the theoretical connection between both sleep and positive emotions and recovery processes in chronic pain. It is also instructive that cognitive-behavioral treatments focused specifically on sleep or pain demonstrate effects on both domains (Smith & Haythornthwaite, 2004), which indicates that there may be commonalities in the underlying etiologies of both processes.
Social Contributors to Pain Resilience
Although a great deal of research has traditionally been focused on intra-individual processes that contribute to resilient coping, the social world also plays a complex role in adaptation to chronic pain. In general, resilient individuals appear to effectively utilize social resources to recover from stress (Friborg et al., 2006) and can enhance resilience against a stressor by seeking out appropriate social support (Connor & Davidson, 2003). In individuals with chronic pain, a primary source of sustainable positive emotion is through continued positive social interactions (Smith & Zautra, 2008). Similarly, the presence of support from a loved one can buffer against the effects of stress and pain on the HPA axis (Hostinar, Sullivan, & Gunnar, 2014), preserves physical and psychological functioning during times of increased pain (Taylor, Davis, & Zautra, 2013), and predicts decreased pain and central nervous system activity during a pain induction procedure (Montoya, Larbig, Braun, Preissl, & Birbaumer, 2004).
However, individuals with chronic pain may also face unique challenges to their social worlds. Individuals with chronic pain may lose their ability to view their relationships with the appropriate degree of flexibility when experiencing increased pain (Davis, Zautra, & Smith, 2004), may be more likely to become irritable or angry and experience social conflict (Feldman, Downey, & Schaffer-Neitz, 1999), and show a greater tendency to decrease their levels of positive social engagement in the face of significant pain (Sturgeon, Zautra & Arewasikporn, 2014). It has been suggested that some individuals may also adopt a stoic attitude towards their pain, choosing not to seek out appropriate support from their social environment, even if it is available, thereby compromising the beneficial effects of a responsive social network (Moore, Grime, Campbell, & Richardson, 2013). When one’s relationships are damaged, an important source of positive emotion is threatened; in these cases, recovery processes become increasingly important. Recent evidence suggests that a capacity to forgive and to repair damaged social relationships may enhance resilience in chronic pain (Toussaint et al., 2014).
Further, although social relations are fundamental to resilience in pain, a social network that is too large or that enhances dependency rather than rewarding competence may undermine the person’s self-efficacy, leading to poorer long-term pain coping (Franks, Cronan, & Oliver, 2004). Similarly, social goals that are focused on receiving validation from others rather than contributing to the well-being of others may lessen, rather than boost, sustainability (Hamilton, Karoly, & Zautra, 2005). Social resilience in chronic pain thus may be best defined as an ability to maintain engagement in, and appreciation for, valued social relationships, even during painful moments, and to repair meaningful interpersonal relationships when they are damaged. Given the many challenges faced by those dealing with recurrent pain, social support can be an important contributor to successful adaptation, but only within the context of relationships that preserve an individual’s motivation to take an active and meaningful part in shaping one’s life course trajectory.
Growth and New Learning in Response to Chronic Pain
One implicit assumption in our model of resilience is that an individual experiences many opportunities to be resilient to chronic pain that can be measured across time. An individual may find a way to cope effectively with pain immediately, such that it does not meaningfully disrupt his or her immediate emotional, cognitive, or behavioral states. In those cases where pain does lead to poorer functioning, however, individuals may show resilience to pain by effectively bouncing back and returning to their baseline or homeostatic set points. Finally, those individuals who strive and fail, but ultimately bounce back from their pain-related challenges may acquire important new information about how to cope with pain in an effective way, catalyzing long-term growth.
These patterns of pain-coping responses may thus evolve across time; the occurrence of learning, which may spur alternative strategies for coping with pain, expectations about the experience of pain itself, and belief in one’s own ability to cope, is dependent on the coping attempts that have occurred previously. Responses to pain and subsequent coping efforts also have a profound long-term impact; there is evidence that emotional reactivity to stressors can affect health status over a period of time as long as 10 years (Piazza, Charles, Sliwinski, Mogle, & Almeida, 2013). Consequently, it is necessary to expand models of pain resilience to incorporate time as an important contributing factor (Keefe & Wren, 2013); resilience to pain is “learned” through previous painful experiences, and only by acknowledging time as a factor can we understand how the phenomenon of resilience to pain may evolve within individuals as they progress from acute pain to chronic pain, and how they make adjustments to chronic pain itself. Some studies have begun to incorporate time in models of pain resilience by examining trajectories of intensity of specific pain complaints (Collins, Katz, Dervan, & Losina, 2014), which can serve as important characterizations of physical recovery from pain itself, while others have tracked the concomitant changes in pain and mood across time, reflecting psychological recovery from pain (Zhu, Galatzer-Levy, & Bonanno, 2014). We highlight the importance of long-term growth as a valuable temporal indicator of adaptation to chronic pain.
Missing in all models of adjustment, and in some models of resilience, is an appreciation for the capacity of the person with chronic pain to learn, not just to cope successfully, but to further their existing goals and develop new pursuits. Resilient growth in chronic pain occurs through adaptive efforts that are modified according to feedback to the individual and the environment. In early stages of chronic pain, individuals may naturally gravitate to different strategies when they believe their pain to be acute, rather than chronic. However, over time, many individuals discover that these strategies (e.g., behavioral avoidance) are maladaptive and may contribute to longer-standing problems. Further, some individuals may habituate to their pain naturally through the course of their daily lives, as recent findings suggest greater levels of resilience in older individuals with chronic physical ailments than in younger individuals (Terrill et al., 2014). Growth and new learning occurs through experience and, often, through failed attempts to adapt. Indeed, individuals who self-identify as resilient have reported drawing from coping with previous challenges and losses (Gattuso, 2003). Exposure to pain and stress is also important in fostering growth, as it provides an opportunity to learn and respond effectively to pain.
It is well-established that early life exposure to stressors can alter developmental trajectories; there is a robust literature suggesting that exposure to severe traumatic stressors or chronically elevated levels of stress exposure can manifest in poorer overall development and functioning later in life (Rutten et al., 2013). However, an optimal level of stress exposure may exist; put in another way, lack of exposure to stress during earlier developmental stages is unlikely to yield optimal levels of resilience in later developmental stages. A recent study by Seery et al. (2013) has demonstrated this phenomenon. These authors reported that moderate life stress exposure throughout adulthood has been found to predict greater levels of resilience to stress and pain, whereas resilience to these factors was lower in those with no significant life stress or very high levels of life stress. More specifically, individuals who reported moderate levels of life stress during their adult years demonstrated lower levels of situational catastrophizing, pain intensity, and pain unpleasantness to a cold pressor task, were able to tolerate cold pressor pain for longer periods, and also exhibited decreased physiological reactivity to a social stress paradigm in which they were asked to complete a nonverbal intelligence test (Seery, Leo, Lupien, Kondrak, & Almonte, 2013). In short, individuals who faced significant but not overwhelming stress as adults were better able to handle situational challenges like social stress and pain more effectively. Interestingly, individuals with chronic pain have shown decreased levels of emotional stress in response to future stressors after suffering the loss of a spouse, suggesting that resilience may develop even after particularly poignant losses and the ongoing experience of pain (Wade, Hart, Wade, Bajaj, & Price, 2013).
The inoculating effects of stress are also theorized to be present in childhood: early life exposure to periodic, but not necessarily prolonged, challenges like life stressors may contribute to resilience, while severe or prolonged stress exposure may sensitize the hypothalamic-pituitary-adrenal axis and may contribute to longer-term vulnerability to psychiatric disorders (Rutten et al., 2013). This phenomenon has been theorized to fit a quadratic or inverse-U function, such that too much or too little exposure to stress in childhood may contribute to greater vulnerability to poor stress response, while there is an optimal and moderate level of stress exposure (Parker & Maestripieri, 2011). Further, the process of resilient development appears to be modified by epigenetic factors, which may help to explain the large degree of variability of responses among individuals who are exposed to similar levels of challenge during their development (Rutten et al., 2013).
A similar parallel has been drawn to the benefits of a common and frequent physical challenge: physical exercise. Physical exercise presents a notable challenge to physiological adaptation (McEwen, 2003) and has been implicated as a promoting factor in resilience in earlier development (Strohle, 2009) and in resilient responses to stress in adults (Deuster & Silverman, 2013). Further, maintenance of physical exercise earlier in life is predictive of greater behavioral engagement in older age, despite the presence of chronic pain (Moore, Richardson, Sim, Bernard, & Jordan, 2014). However, physical activity in some forms may pose problems to individuals with chronic pain or fatigue, manifesting in increased inflammatory responses (McEwen, 2003). This evidence suggests that the effects of exercise, like stress, are not uniform across individuals in all forms and must be interpreted in the proper context.
Pain acceptance is another salient example of how the timeframe of pain adaptation plays a meaningful role in our understanding of resilience. Pain acceptance is defined as a process by which individuals acknowledge that they have pain, stop maladaptive attempts to prevent or cure their pain, and learn to live meaningful lives despite the presence of their pain (McCracken, 1998). Acceptance of pain may also reflect a greater degree of psychological flexibility, conferring an increased ability to maintain focus on values and goals during times of increased pain and distress, and helping individuals to act or adjust their behavior in ways that are most consistent with their values (Eccleston, Crombez, Aldrich, & Stannard, 2001). Acceptance of pain has proven to be a powerful predictor of better functioning in individuals with chronic pain, as individuals who accept their pain will show lower levels of emotional distress in response to pain and continue to maintain engagement in valued activities despite the presence of pain (McCracken, 2010). More recent studies of pain acceptance have tied this construct more directly to resilience, suggesting that acceptance of pain can buffer against negative consequences of pain on mood and functional impairment (Ramírez-Maestre & Esteve, 2014; Ramirez-Maestre, Esteve, & Lopez-Martinez, 2014) and may be a more salient factor in determining the severity of pain-related disability than negative cognitive factors such as pain catastrophizing (Mun, Okun, & Karoly, 2014).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





