34 Skull Base Traumatology • Skull base fractures (SBFs) occur in 3.5 to 24% of head injuries.1 • SBFs can cause death or coma. They may be associated with immediate or delayed complications, such as cerebrospinal fluid (CSF) leakage, possible meningitis, and neurovascular damage (injury of arteries, dural sinuses, and/or cranial nerves).2,3 The causes of SBFs vary depending on the severity of the injury. Although sports and recreation activities account for large numbers of head injuries, these injuries are rarely severe enough to lead to a SBF. The most common mechanisms of head injury are motor vehicle accidents (which account for 40% in both the adults and children), followed by falls, direct trauma by falling/penetrating objects, and assaults.1,4 In the pediatric population, SBFs are caused by falls from heights (32%), falls on the ground (10%), falls related to sports (3%), and episodes of violence (8%)4 (for the pediatric skull base traumatology, see page 876). • Skull base fractures are among the most difficult fractures to evaluate and manage. • They are an epiphenomenon in polytrauma patients, occurring alongside other body trauma with or without neurologic deficits. Pearl In skull base fractures or penetrating injuries, always investigate for other fractures (mid-face, cranial vault, spine), brain injury, neurovascular injury, and neurologic deficits, and assess the general clinical and neurologic status (more than just using the Glasgow Coma Scale [GCS]). • Anatomic location of SBFs: 70% involve the anterior skull base, 5% the middle skull base, 5% the posterior skull base, and 20% the central midline skull base. • Battle’s sign (postauricular ecchymosis) • Raccoon’s eyes or panda’s eyes (periorbital ecchymosis). This is an indicator that is not always associated with SBFs. It occurs in 42% of cases, of which 53% have been found to occur in the petrous bone/middle skull base. Periorbital ecchymosis has been associated with several further findings, such as intracranial hemorrhage, cranial nerve injury, soft tissue injury with or without fracture, and convexity fracture. Surgical intervention is required in 22% of patients with periorbital ecchymosis.5 • CSF rhinorrhea/otorrhea/orbitorrhea or leak from the traumatic wound • Hemotympanum with or without laceration of the external auditory canal • Cranial nerve injuries Computed tomography (CT) is the imaging gold standard for the detection of SBFs, and several classification systems are CT-based. To overcome the limits of low-resolution single slices to detect fractures, high-resolution CT (1-mm slice thickness) is often required with solid and transparent three-dimensional (3D) volume-rendering reconstructions6–9 or curved maximum intensity projection (cMIP) reconstructions to improve fracture detection.9,10 • A step-by-step analysis of the axial and multiplanar reconstructions of the skull base is critical to avoid missing fractures and clinically relevant neurologic findings.11 Frontobasilar fractures require special attention to assess the integrity of the nasofrontal ducts or nasofrontal outflow tracts, and the involvement of the cribriform plate, posterior wall of the frontal sinus, optic canal, sella turcica, and orbit walls and contents. • CT angiography (CTA) or digital subtraction angiography (DSA) should be performed in cases of SBF with possible vascular injury (laceration, thrombosis, dissection, pseudoaneurysm12). • Have a high index of suspicion for vascular, neural, or dural injuries in any patient with SBFs. • The involvement of specific regions of the skull base already suggests the possible neurovascular involvement of the anatomically contiguous structures: • Whenever feasible, magnetic resonance imaging (MRI) is helpful for the detection of traumatic involvement of soft tissues (brain, orbit contents) and dural defects. Classification systems of SBFs should consider radiological, anatomic, and clinical information related to clinical decision making. • Anatomy-based classification systems offer a general framework including the specific complications related to the site of the SBFs. • The involvement of the skull base must also be investigated in facial fractures. For example, Le Fort II and III fractures are associated with an increased risk of blunt injury to the carotid arteries,14 and Le Fort III may have skull base involvement (Table 34.1). • Fractures of the petrous bone can cause facial palsy, deafness, and CSF leakage with otorrhea or paradoxical (oto)rhinorrhea (see Chapter 32). Fractures of the posterior fossa may lacerate the major venous sinuses and affect craniocervical stability.3 Pearl • A classification system should be logically structured, accurate, comprehensive, and systematic, and should provide information regarding the severity of the injury and recommendations regarding therapeutic options.13 Table 34.1 Le Fort Fracture Types
 Causes
Causes
 Typical Signs of Skull Base Fractures
Typical Signs of Skull Base Fractures
 Imaging
Imaging
 Petrous portion of the internal carotid artery (ICA) and facial nerve in petrous bone fractures
Petrous portion of the internal carotid artery (ICA) and facial nerve in petrous bone fractures
 Dissection of the vertebral artery in craniovertebral trauma
Dissection of the vertebral artery in craniovertebral trauma
 Injury of the intracavernous ICA, carotid-cavernous fistula in sellar/parasellar fractures
Injury of the intracavernous ICA, carotid-cavernous fistula in sellar/parasellar fractures
 Laceration of the middle meningeal artery in middle fossa/temporal squama fractures
Laceration of the middle meningeal artery in middle fossa/temporal squama fractures
 Venous dural sinuses injuries in cranial vault/skull base fractures
Venous dural sinuses injuries in cranial vault/skull base fractures
 Classification Systems
Classification Systems
Type and Definition | Fracture Pattern | Signs and Symptoms |
I: horizontal/transverse
| Fracture line above the apices of the upper teeth, crossing the pterygoid plate and the maxilla, then entering into the maxillary sinus | Ecchymosis, swelling, teeth mobility |
II: pyramidal
| Pyramidal pattern involving the medial orbital walls, inferior orbital rim, nasofrontal suture, pterygoid plates | Face deformity with midface mobility, cranial nerve V2 anesthesia/paresthesia |
III: transverse, craniofacial dislocation
| Zygomatic arches, zygomaticofrontal and nasofrontal sutures, pterygoid plates, orbital floors | Separation of the frontozygomatic suture, eyeball deviation, often associated with other injuries in polytrauma |
Clinical- and Radiology-Based Classification Systems of the Skull Base Fractures
In a 48-patient study, high-resolution thin-section CT scan enabled the classification of fractures into four major types15:
• I: cribriform
• II: frontoethmoidal
• III: lateral frontal
• IV: complex (combination of the other three types)
The major finding of this study was that there is a trend of increased infection rate related to (1) prolonged duration of rhinorrhea, (2) large size of fracture displacement, and (3) proximity of the fracture to the midline (to the cribriform plate).
• Cranial and facial injuries in high-velocity injury events can be classified16 as frontal, basal, or combined, as well as central, lateral, or combined. Moreover, fractures can be classified as unilateral or bilateral, as well as pure or impure, depending on the absence (pure) or presence (impure) of midfacial fractures. The most common injuries are the combined frontobasal type (30% of cases), with CSF leak occurring more commonly in impure types of frontobasal fractures.16
• Frontobasal and midface fractures involving the skull base are classified into the following three types, based on the fracture pattern, location, involvement of the midface, and related complications14:
 Type I: isolated linear cranial base fractures
Type I: isolated linear cranial base fractures
 Type II: vertical-linear fracture of the skull vault (frontal bone) in combination with a SBF
Type II: vertical-linear fracture of the skull vault (frontal bone) in combination with a SBF
 Type III: comminuted fracture of the frontolateral skull vault and orbital roof in association with a linear SBF
Type III: comminuted fracture of the frontolateral skull vault and orbital roof in association with a linear SBF
• In this classification system, in which 290 patients were analyzed, type III patients had the highest rate of complications (CSF leaks and infections), followed by type II.17
• Radioanatomic and clinical findings (rhinorrhea, periorbital hematoma, and pneumocephalus) have been analyzed in two studies of the Arbeitsgemeinschaft für Osteosynthesefragen: Association for the Study of Internal Fixation (AO), to develop a hierarchical classification system in which the score stratifies patients’ risk of complications and suggests a treatment approach.18,19 The classification system defined three fracture types (A, B, C), three groups (1, 2, 3), and three subgroups (1.1, 1.2, 1.3) with increasing severity from A1.1 (lowest severity) to C3.3 (highest). The operative cases had significantly higher severity scores than the nonoperative ones. More severe fracture grades were significantly associated with the occurrence of pneumocephalus and rhinorrhea, and with the treatment approach. A correlation among the se verity of the fracture, the number of posttraumatic functional limitations, the need for bone grafting or duraplasty, and facial asymmetry was observed. The proposed classification system enables standardized documentation of midfacial and craniofacial fractures, including those not precisely defined by other schemas, as well as the relationship among the severity of the fracture, the posttraumatic functional limitations, and the need for different therapeutic strategies. The classification, although limited by the fact that it is roughly regional, also has been found to be of reliable utility in arriving at a prognosis, demonstrating that almost 87.5% of patients who died had sustained group 3 fractures involving the skull base.18
• The most recent AO proposed classification system also has a hierarchical system: levels 1 and 2 define the anatomic localizers (region of the head, cranial vault, and skull base involvement), whereas level 3 describes the fracture morphology in an array of modules specific for anatomic regions and subregions.20,21 According to this model, the skull base is divided into two lateral compartments and a central compartment, from the frontal sinuses to the foramen magnum (see Chapter 2, Fig. 2.3b, page 12), and the types of fractures can be classified by means of classifier software.22
• Based on their morphology, fractures are defined as single or multiple, crossing one or more bones, displaced or nondisplaced, depressed or not depressed, and involving or not involving the paranasal sinuses. Radiologically, it is important to correlate the presence of fractures with other findings, such as the presence of pneumocephalus or intracranial mass lesions (epidural, subdural, subarachnoid, intraventricular, or intraparenchymal hematoma, brain contusions, foreign bodies).
 Anterior Skull Base Fractures
Anterior Skull Base Fractures
Craniofacial fractures may involve the anterior skull base, which includes the posterior wall of the frontal sinus, the ethmoid cells, the cribriform-ethmoid junction, and the orbits.
Head injury with frontobasal involvement is generally associated with facial fractures (87% of patients), as well as hematomas (epidural/subdural or subarachnoid) or otobasal fractures (15%).23
Signs typically associated with these fractures are CSF rhinorrhea with (3%) or without (37%) meningitis, hyposmia/anosmia (91%), and raccoon’s eyes (21%).23
Frontal Sinus Involvement
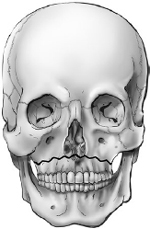
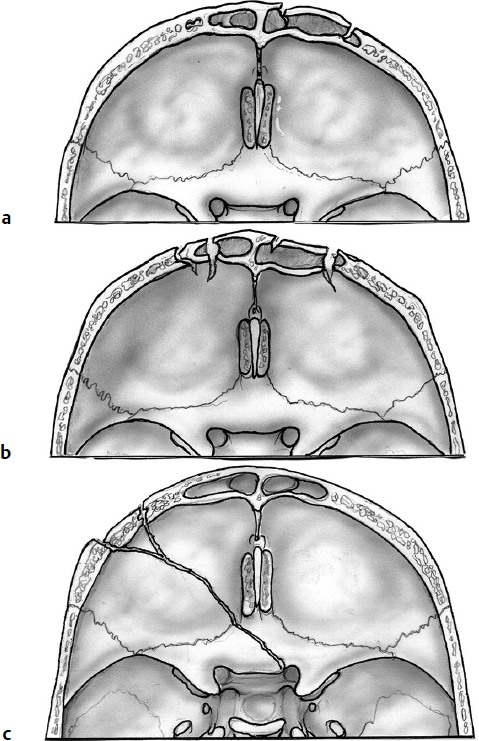
A three-grade classification system exists for frontobasal fractures involving the frontal sinus24 (Fig. 34.1):
• Type A: The anterior wall of the frontal sinus is fractured.
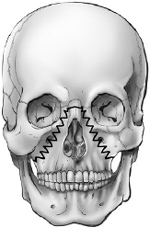
• Type B: Both anterior and posterior walls are fractured.
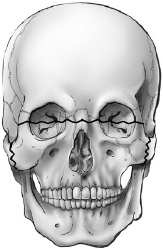
• Type C: The frontobasal fracture does not involve the frontal sinus.
Patients in type B generally present with pneumocephalus, CSF rhinorrhea, and displaced fractures, and they often require surgery. Type A patients generally require surgery only for cosmetic reasons. Type C patients generally do not require surgery for their fracture.24
The complication rate in patients undergoing surgery of the frontal sinus (see below) is up to 10%, and should be considered before proceeding with surgery.25–27 Moreover, the presence of an obstructed outflow tract must be considered as well, because it might be treated by stenting of the duct.28
Fractures of the anterior wall may undergo reconstruction by using bony fragments and titanium mesh.29
Fig. 34.1a–c Frontobasal fractures. (a) Type A: anterior wall of the frontal sinus involvement. (b) Type B: anterior and posterior walls fractured. (c) Type C: frontobasal fracture not involving the frontal sinus.24
Cranialization of the Frontal Sinus
The so-called cranialization of the frontal sinus is a technique used to resect sinus mucosal tissue from the frontal sinus and separate the nasal cavity from the cranial fossa. Although this can almost always be effectively accomplished without resorting to removal of the posterior table of the frontal sinus, the procedure to do so is still in use. In cases with a comminuted fracture of the posterior table, the main reason to remove it is to avoid the development of sequestra.
In general, a coronal scalp incision approach is used for the cranialization procedure (see Chapter 14, Fig. 14.3, page 342).
• Using an extradural dissection, expose the posterior table of the frontal sinus and the anterior skull base. The ethmoidal arteries should be identified as they exit the bone, and they are later coagulated and cut.
• Remove the posterior wall of the sinus by means of rongeurs or drills. A drill should be used to smooth the contour of the remaining bone.
• Strip out the sinus mucosa, and use a fine high-speed drill to remove any remnant of the mucosa. One can entirely exenterate the mucosa or, rarely, invert it, pushing it inferiorly in order to obstruct the outflow tract. The tract can be plugged also with fragments of bone or fascia.
• Cover the frontal sinus and the anterior skull base with the pericranial flap.
• To close the bone flap, use miniscrews, mini-plates, titanium meshes, or cement, depending on the size of the defect. Avoid strangulating the pericranial flap across too tight a gap in the bone or across a too posteriorly placed craniotomy cut.
Surgical Pearl
To make a “watertight” compartmentalization, the pericranial flap has to be intact. If some holes are present, repair it with sutures.
Ocular/Orbital Involvement
Patients with major trauma and facial injuries have a high risk of vision-threatening injury. Patients with orbital fractures, SBFs, eyelid lacerations, or superficial eye injuries should be assessed by an ophthalmologist as part of the early management of their trauma to determine whether an ocular injury is present.30 Documentation of visual acuity and the pupillary responses including searching for a Marcus Gunn pupil are important in all patients with trauma. (See Chapter 10).
• Nondisplaced orbital fractures do not require surgical treatment.31
• Superiorly displaced fractures (isolated blowup) may be associated with neurologic deficits (including brain contusion, CSF leakage, and hematoma), whereas inferiorly displaced fractures (isolated blow-in) result in ophthalmic injury (including proptosis, hematoma, blindness, globe rupture, and ophthalmoparesis).31,32 Only 10% of patients with orbital fracture require surgical repair (orbital roof and dural defect repair).33
• Orbital roof fracture may also be associated with supraorbital rim or frontal sinus involvement.
• Surgical treatment of orbital fractures may require a coronal bifrontal approach, optic nerve decompression, repair of the orbital roof, cranialization of the frontal sinus, open reduction and internal fixation, external orbital frame, or restoration of the internal orbital volume (see Chapters 20 and 27).34
Pearl
Patients who have complete loss of vision at the time of injury should be investigated for optic nerve transection with CT or MRI as appropriate.
 Temporal Bone Fractures
Temporal Bone Fractures
Temporal bone fractures are most commonly caused by motor vehicle accidents, followed by assaults and falls,35 and account for 14 to 22% of all skull fractures. They are more common in men than in women.36,37
• Typical signs and symptoms: sensorineural hearing loss, conductive hearing loss, perilymphatic fistula, cerebrovascular injury, CSF leak (otorrhea), and facial nerve paralysis.38
• High-resolution CT is fundamental for identification of temporal bone fractures.
Radiology Pearl
Recognize normal anatomy and avoid misinterpreting the sutures (tympanomastoid, tympanosquamous, petrosquamosal, petrotympanic sutures) as fractures.39,40 Temporal bone fractures caused by gunshot wounds are frequently complex, and CT scan may be limited by metallic streak artifacts.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree