Cervical deformity surgery typically involves technically demanding and high-risk procedures with specific surgical goals. These procedures can have substantial impact for improving quality of life; however, many techniques used to correct deformities can increase complication risks. Surgeons treating cervical deformity patients should clearly understand the risks and counsel their patients extensively prior to surgery regarding possible complications. A recent prospective study of cervical deformity patients demonstrated an overall early (within 30 days of surgery) complication rate of 43.6% 1 and another study of patients undergoing three-column osteotomies reported a complication rate of 56.5% within 90 days of surgery. 2 Complications may have transient or lasting effects and may alter functional status and/or quality of life permanently. The incidence of complications may vary based on diagnosis, surgical factors, and confounding patient factors. Some complications may be realized during surgery, while others may not be readily appreciated until postoperatively. Treating complications may range from observation to acute surgical intervention. Surgeons treating cervical deformity should understand the possible adverse events related to cervical surgery in general, the surgical approaches, and the complications specifically associated with deformity surgery. This chapter discusses surgical and neurological complications associated with cervical deformity surgery and presents the supporting literature and suggested management strategies.
18.2 Surgical Complications
Surgical complications during cervical spinal procedures may be directly related to the region and type of surgery, surgical approaches, underlying pathology, or patient factors. Cervical deformity surgery has higher reported complication rates compared to other cervical procedures, based on recent prospective reports. 1,2 Awareness of these potential complications allows surgeons to accurately counsel their patients, identify problems earlier, and implement appropriate treatments as necessary. This section discusses surgical complications associated with the anterior cervical approach, vascular injuries, dural tears and cerebrospinal leaks, wound complications and infections, pseudarthrosis, and instrumentation-associated complications. Surgical complications are summarized in ▶ Table 18.1.
Rates | Risk factors | |
Cervical deformity surgery | 43.6–56.5% | |
Surgical complications | ||
Airway compromise | 0.6–1.6% | Male, older age, operative time, hematoma, 3+ levels |
Esophageal perforation | 0–3.4% | Retractors, instruments, implant erosion |
Dysphagia | 47–50% | Operative time, increased operative levels, C2–C4 segments, rhBMP use, smoking, endocrine disorder |
Vascular injuries | 0.7–1.4% | Anomalous vertebral artery, wide corpectomy, malpositioned hardware, Grade 4 osteotomies, tumor/infection procedures |
Dural tears and CSF leaks | 0–18% | OPLL, revision procedures |
Infection | 0.2–1.6% (anterior) 0.7–4.7% (posterior) | Combined surgical approaches, tobacco use, IV drug abuse, malnutrition, obesity |
Epidural hematoma | 0.09% | |
Pseudarthrosis | 0–54% | Number of levels fused, graft material, surgical technique, tobacco use |
Implant malposition or pullout | 0.085–7% | Surgical level (axial > subaxial), pseudarthrosis, corpectomy |
Neurological complications | ||
Hypoglossal nerve | 0.01% | C1–C3 exposure |
Superior laryngeal nerve | 0–1.25% | C3–C4 exposure |
Sympathetic chain and Horner syndrome | 0.06–1% | Anterior exposure lateral to longus colli |
Recurrent laryngeal nerve palsy | 1.8–2.8% (primary) 14.1 (revision) | Traction, retractors, post-op swelling, cervicothoracic junction surgery, revision procedures |
Spinal cord injury | 0.0–1% | Stenosis/spondylosis, intubation, positioning, instrumentation, technical mistakes, deformity correction |
C5 palsy | 0–12.1% (anterior) 0–30% (posterior) | Pathogenesis not fully understood |
C8 nerve injury | 14% | Three-column osteotomy |
Abbreviations: CSF, cerebrospinal fluid; OPLL, ossification of the posterior longitudinal ligament; rhBMP, recombinant human bone morphogenetic protein. | ||
18.2.1 Anterior Cervical Approach Complications
The anterior cervical spine approach described by Smith and Robinson provides a generally safe and reproducible surgical dissection. 3 Compared to the posterior cervical approach, the anterior approach has unique risks and complications including vascular, neurologic, tracheal, and esophageal injuries. These complications can vary in severity depending on structures involved and extent of injury.
Several nerves are at risk during anterior cervical surgery. Surgical level determines the risk for different nerves. The hypoglossal nerve is at highest risk during anterior exposures from C1 through C3. These injuries are extremely rare with a reported incidence of 0.01%. 4 Palsy of the hypoglossal nerve results in ipsilateral tongue deviation and difficulty swallowing due to impairment of food transport toward the back of the mouth. The superior laryngeal nerve is typically at highest risk at C3–C4 and has a reported injury incidence of 0 to 1.25%. 5 This nerve has two branches: internal (sensory) and external (motor). Injury to the internal branch may result in aspiration difficulties, while injuries to the external branch may result in a monotone voice due to loss of cricothyroid muscle function. The recurrent laryngeal nerve (RLN) is vulnerable at multiple levels and usually injured via a traction-type injury as it sits in the tracheoesophageal groove. Damage to this nerve may result in hoarseness or loss of voice due to partial or complete paralysis of the posterior cricoarytenoid muscle in the larynx. The sympathetic chain is also at risk during the anterior exposure as it lies on the lateral margins of the longus colli. Careful medial to lateral elevation of the longus colli muscles while exposing the vertebral bodies reduces the risk to these structures. Injury to the sympathetic chain can result in a Horner syndrome (ptosis, miosis, and anhydrosis). The incidence of Horner syndrome has been reported to be 0.06 to 1%. 6,7
Airway compromise or respiratory failure is an important and life-threatening complication associated with anterior cervical surgery. Causes of airway compromise can be soft-tissue swelling, hematoma, instrumentation failure, or graft dislodgement. The overall risk for reintubation after anterior cervical surgery is low with a reported rate of 0.5% in a large retrospective database study. 8 They found this rate increased to 1.6% in procedures involving 3+ levels; however, they were unable to specifically stratify cervical deformity procedures. Other factors reported as associated with postoperative airway compromise are male gender, older age, increased number of comorbidities, hematoma, and prolonged operations. 8,9 In patients with acute airway decompensation, etiologies such as hematoma, cerebrospinal fluid (CSF) leak, or plate/graft dislodgement should be considered and may require emergent intervention. Based on a recent prospective report of cervical deformity procedures, respiratory failure occurred in 5.1% of patients. 1 This higher rate may be explained by more levels fused, marked changes in cervical alignment, or longer procedures due to the complexity associated with deformity correction procedures.
Several methods for managing airway edema or postoperative airway protection in higher-risk patients have been described. A randomized controlled trial using perioperative steroids to reduce prevertebral soft-tissue swelling demonstrated decreased airway edema, improved swallowing, and shortened hospital stay. 10 Utilization of steroids both topically and systemically has been described; however, proper dosing, method of application, and duration of use have not been fully studied. Topical retropharyngeal steroids should be used with caution in patients with known chronic corticosteroid use. A case report by Lee et al of two patients suggested this application can lead to increased esophageal perforation risk. 11 For high-risk patients, surgeries with combined approaches, or prolonged procedures, surgeons may also consider continuing postoperative intubation in a monitored intensive care unit for airway protection. Type of surgery and patient factors need to be carefully considered and discussed with patients when planning extensive deformity procedures that may utilize an anterior or combined approach.
Esophageal perforation injuries are rare and have reported rates of 0 to 3.4%. 12,13 Mortality has been reported as 20% if missed within 24 hours and up to 50% if treatment is delayed for more than 24 hours. 14 Perforation injuries may occur during retractor placement, instrumentation, or from dislodged screws, plates, or grafts. Esophageal damage may be noticed at the time of surgery or be discovered in a delayed fashion due to implant/graft erosion over time. Patients present with dysphagia, odynophagia, infection, aspiration, or airway compromise. Diagnosis can be made with endoscopy, contrast-enhanced computed tomography (CT) scans, and/or barium-enhanced esophagrams. Treatment can be complex and may require percutaneous endoscopic gastrostomy tube placement for nutrition, intravenous antibiotics to prevent infection, and possible repair or reconstruction with the assistance of otolaryngology and thoracic surgeons. These can be devastating and potentially life-threatening injuries.
Like esophageal injuries, tracheal injuries are extremely rare during anterior cervical surgery and are usually associated with retractor placement, perforation by a sharp instrument, or erosion by an implant or graft. These injuries can be complex to treat and often require the expertise of a head and neck surgeon. There are no specific reports of tracheal injuries during cervical deformity surgery.
Dysphagia and dysphonia are well-known associated adverse events following anterior cervical surgery and occur far more commonly than esophageal or tracheal perforation injuries. The true incidence of dysphagia has been difficult to define in the literature; however, three prospective studies have reported rates of 48%, 15 50%, 16 and 47% 17 in the early postoperative periods. Patients should be counseled about the risks of dysphagia after anterior surgery. Factors reported to be associated with the occurrence of dysphagia include increased operative time, greater number of surgical levels, angle from C2 to C7, use of self-retaining retractors, elevated endotracheal cuff pressure, ventral instrumentation size and placement, procedures including more proximal cervical exposure (C2–C4), use of recombinant human bone morphogenetic protein-2 (rhBMP-2), staged surgery, presence of an endocrine disorder, and smoking. 15,16,18,19,20,21,22 Although most cases of dysphagia resolve without intervention, resolution can take several months or longer and may impart significant morbidity on patient recovery. Patients with refractory symptoms after 6 to 9 months may require further evaluation and referral to an otolaryngologist. Surgeons should be vigilant in evaluating a patient with new-onset or worsening dysphagia in the late postoperative period and should consider the possibility of implant or graft erosion causing esophageal perforation. Early postoperative dysphagia was reported at 11.5% overall after cervical deformity procedures; however, this rate increased to 24.1% in the subset of patients with combined anterior-posterior procedures. 1
Dysphonia rates have also been difficult to define in the literature. One reason is poor standardization defining the condition. Another reason is there is wide variation in reported incidence between studies that relied on patients to self-report this complication and those that utilized laryngoscopy. The most common cause of dysphonia after anterior cervical surgery is RLN injury or palsy. RLN injury has been associated with traction injury, postoperative soft-tissue swelling, surgery at the cervicothoracic junction, and revision surgery. Incidence of RLN injury has been reported from 1.8 to 2.8% for primary surgeries and up to 14.1% for revision procedures. 23,24,25 Cadaveric studies demonstrated the RLN has a more predictable course on the patient’s left side and historically it was believed that approaching this side may lower injury rates; however, recent studies have shown similar injury rates when approaching from the right or left sides. 23,25 Recent cervical deformity literature has not reported high rates of dysphonia; however, surgeons should be aware of this risk if utilizing an anterior or combined approach for deformity surgery, especially in revision cases.
18.2.2 Vascular Injuries
Vascular injuries can occur during anterior or posterior cervical surgery. Vertebral artery injuries are uncommon during cervical spine surgery with reported rates from 0.07 to 1.4%. 1,26,27,28,29 The vertebral arteries have variable locations based on cervical level; however, they tend to be less commonly encountered during a typical anterior exposure. Anomalous vertebral artery anatomy in the subaxial spine has been reported in up to 20% of the population. 30 Tortuous and/or ectopic arteries may be encountered during ventral or dorsal exposure, corpectomy procedures, or during instrumentation placement. With normal vascular anatomy, factors such as performing a wide corpectomy, Grade 4 osteotomy (complete uncovertebral joint resection to the transverse foramen), 31 or treating tumor and infection-related conditions can increase the risks of vertebral artery injuries as well. Careful evaluation of preoperative MRI or contrast-enhanced CT scans allows surgeons to identify abnormal anatomy and plan appropriately. 32 In a large, multicenter AO Spine database review of 16,582 cervical spine cases, 14 vertebral artery injuries were identified and of these, 50% had anomalous vessel anatomy on preoperative imaging identified during postoperative review. 29
The anatomy of the vertebral arteries is classically described as four segments, V1–V4. V1 runs from the subclavian artery to the C6 transversarium and ventral to the C7 transverse process. V2 describes the segment within the transversarium from C6 to C1. The third segment (V3) extends from the atlas to the foramen magnum, and V4 is intradural from the foramen magnum to the posterior inferior cerebellar artery and joins the contralateral vertebral artery to become the basilar artery. Vascular injuries may occur at any of the four segments. In the subaxial spine, the vertebral arteries take a more predictable pathway than the atlantoaxial regions. Arterial injury rates are low for the subaxial spine for both lateral mass and pedicle screw instrumentation. Abumi et al reported 1 arterial injury among 712 cervical pedicle screws placed (0.6%). 33 Despite the theoretical risk to surrounding structures during subaxial lateral mass instrumentation, there are no specific reports of arterial injury in the modern literature. Nevertheless, undoubtedly this complication does occur at some low rate. In contrast, instrumentation of the atlantoaxial spine has higher reported rates of arterial injury from 4.1 to 8.2%, particularly with transarticular screws. 30 Given that some patients with cervical deformity may require instrumentation of these segments, surgeons should carefully examine preoperative imaging and should consider preoperative CT or magnetic resonance angiography to clearly define the vascular anatomy. If surgeons are planning a three-column osteotomy at C7, preoperative CT with angiography is required to carefully assess the vertebral arteries and their course at the cervicothoracic junction. This is critical for safely performing this procedure at the cervicothoracic junction. Reported vascular injuries during deformity corrective procedures are low, ranging from 0 to 1.3% 1,2,34,35; however, injury to these structures can be catastrophic and life-threatening.
In the event of an injury, tamponade, embolization, surgical repair, and ligation are all considerations for treatment. Direct ligation should be the last treatment option with reported mortality rates of up to 12%. 30 Prompt consultation with a vascular surgeon should be considered if a vertebral artery injury is suspected. If local bleeding control is obtained, immediate postoperative angiography is recommended. Patients should be monitored in intensive care units for changes in neurologic function. Treatment goals should be focused on preventing vertebrobasilar ischemia and cerebrovascular events.
18.2.3 Dural Tears and Cerebrospinal Fluid Leaks
Dural tears or cerebral spinal leaks are uncommon during cervical spine surgery. Reported incidence in anterior cervical surgery is 0 to 8.3%. 36,37 CSF leaks are more common during revision surgery and procedures involving ossification of the posterior longitudinal ligament, with rates reported as high as 32% for the latter. 38 Incidental durotomies may also be encountered during posterior procedures and rates between 0.3 and 13% have been reported, with rates as high as 18% for revision procedures. CSF leaks can cause delayed physical therapy initiation, prolonged hospital stays, increased healthcare costs, wound complications, and need for additional surgeries. Among 78 cervical deformity cases, two (2.6%) dural tears were reported. 1 If encountered, treatments may include direct repair with or without a synthetic sealant adjunct. Proper multilayer wound closure is critical and many authors recommend subfascial drains (with careful monitoring of drain output) or lumbar drains. Pseudomeningocele formation is rare with reported incidence of 0.08%. 39 For refractory symptomatic cases, a peritoneal shunt or revision surgery may be considered. Patients with dural tears are at risk for other complications including delayed wound healing, prolonged recovery, pulmonary complications, meningitis, or even death. 40
18.2.4 Wound Complications and Infections
Surgical-site wound complications and infections are rare occurrences in spinal surgery. Reported rates of deep infection after anterior surgery range from 0.2 to 1.6% and for posterior surgery range from 0.7 to 4.7%. 41 Recent reports have illustrated slightly higher infection rates in patients undergoing cervical deformity surgery with infection rates of 0% for anterior-only, 7.9% for posterior-only, and 6.8% for combined approaches. 1 Of these, 6.4% were deep infections. These rates did not have significant associations with demographic factors; however, other studies have shown alcohol consumption, tobacco use, intravenous drug abuse, malnutrition, and obesity to predispose spinal patients to surgical-site infections. 42,43 These modifiable risk factors should be considered during preoperative optimization. Surgical-site infections can range from superficial to deep and have a wide range of necessary treatments. Patients may require surgical debridement, instrumentation removal or exchange, and possibly complex wound closure or flap reconstruction. Organism-specific antibiosis is often required and long-term suppression may be necessary.
Another wound-related complication that can have devastating effects is symptomatic epidural hematoma. If an epidural hematoma is suspected, early identification and surgical evacuation is key for neurological recovery. A report by Schroeder et al in 2017 demonstrated a 0.09% incidence of symptomatic epidural hematomas among 16,582 cervical spine surgeries. 44 Among patients with known hematomas, those with delayed diagnosis had higher rates of residual neurological deficits and showed no improvement in health-related quality of life metrics at final follow-up. Surgeons should be aware of this complication, make prompt diagnosis, and institute immediate treatment to help achieve optimal neurologic recovery.
18.2.5 Pseudarthrosis
Pseudarthrosis is the failure of bony fusion after a spinal arthrodesis procedure. This is a known complication with surgery of any spinal region. In the cervical spine, pseudarthrosis can occur after anterior or posterior procedures. Nonunions may be asymptomatic; however, they may result in pain, recurrence of radicular or myelopathic symptoms, deformity, graft dislodgement, or instrumentation failure. Development of pseudarthrosis is multifactorial and may be associated with the number of surgical levels, graft type, biomechanical stability, and host factors. Reports over the last three decades have attempted to elucidate the factors associated with pseudarthrosis and guide surgeons toward optimal treatment.
Reported pseudarthrosis rates range from 0 to 11% for single-level surgery, 45,46,47,48 0 to 63% for two levels, 45,48,49,50 and 0 to 54% for three or more levels. 49,51,52,53,54 These studies include other confounding variables such as use of autograft versus allograft, variable use of ventral instrumentation, and variations in endplate preparation. Despite these differences, it is described and accepted that nonunion rates increase as more levels are fused in the anterior cervical spine. For patients undergoing deformity correction surgery, multiple levels may need to be approached and these patients should be counseled regarding the nonunion risks associated with multilevel surgery.
In addition to the number of fusion levels, interbody graft material has been associated with different pseudarthrosis rates. Interbody grafts can be made of autograft, allograft, or synthetic materials such as PEEK, titanium, or carbon fiber. There are conflicting reports regarding potential differences in radiographic pseudarthrosis rates between autograft and allograft materials, especially with multilevel surgery. 48,49,53,55 Additional factors, such as packing material and surgical technique, may help explain these differing results. In addition, similar fusion rates have been reported between structural autograft and synthetic cage materials in anterior cervical procedures. 49,56,57 Standalone interbody devices are also used for cervical fusion; however, the literature related to their efficacy and associated pseudarthrosis rates, especially in multilevel constructs, has yet to be fully reported.
Ventral fixation is also a variable that may impact pseudarthrosis rates. While some reports suggest similar fusion rates with and without anterior plating, a recent meta-analysis suggests that anterior instrumentation improves pseudarthrosis rates, even in single-level surgery. 58 Modern instrumentation includes locking screw technology to increase the fixation rigidity and to help prevent toggling or pullout. Recently, dynamic plate designs have been introduced with the theoretical advantage of maintaining graft and implant load-sharing and possibly increasing fusion rates; however, further studies are needed to determine their clinical impact.
Patient host factors can substantially impact bony fusion rates. The most relevant factor identified in the literature is smoking or tobacco exposure. 59 Other factors such as comorbidities, presence of metabolic bone disorders, or malnutrition should always be considered during preoperative optimization and counseling and may impact surgical outcomes.
Close patient follow-up is necessary to monitor patients for pseudarthrosis. Measuring the interspinous distance on dynamic cervical radiographs is one method for detecting motion after cervical fusion surgery with 2 mm or less of motion being highly associated with solid arthrodesis. 60 Fine-cut CT scanning is the radiographic study of choice for evaluating cervical fusions; however, all radiographic methods have limitations and surgical exploration remains the gold standard for assessing complete arthrodesis. 61
18.2.6 Implant-Associated Complications
Cervical spine deformity surgery usually involves applying instrumentation to the spinal segments. Instrumentation can be inserted into the ventral and/or dorsal spine through various methods. In the anterior spine, ventrally placed plates and screws can be applied to bridge across fusion segments. Alternatively, interbody devices with integrated fixation screws have also been developed. In the posterior cervical spine, wiring techniques, lateral mass screws, pedicle screws, translaminar screws, and transarticular screws have all been utilized. Regardless of technique, implant placement always poses risks during and after surgery.
Screw malposition in the cervical spine can be a detrimental complication. In the anterior spine, improper screw length can lead to iatrogenic spinal cord injury (SCI) and paralysis. This complication was more prevalent when nonlocking bicortical screws were used. With the evolution of locking cancellous screw and plate technology, this complication is now uncommon. Alternatively, depending on plate placement and screw angle, screws may violate adjacent disc spaces, neuroforamina, or vertebral arteries. With posterior fixation, spinal cord, nerve root, facet joint, or arterial injuries can occur, particularly in the atlantoaxial segments. Harms and Melcher reported the incidence of malpositioned screws as 0 to 4% in the atlas and 0 to 7% in the axis. 62 In the subaxial spine, pedicle breaches are less common and insertion techniques using anatomic landmarks 63 or by direct pedicle palpation after laminoforaminotomy 64 have both been shown to be safe and effective.
Screw pullout, breakage, and fixation failure are rare but do occur. A recently published review of 12,903 patients identified 11 cases (0.085%) that required reoperation for malpositioning or screw pullout. 65 In the cervical spine, this may be associated with distal junctional kyphosis and this topic is covered in subsequent chapters. Instrumentation can fatigue and fail in the presence of pseudarthrosis. In addition, several reports have demonstrated high failure rates and graft dislodgement after multilevel anterior corpectomy procedures. 66,67,68,69 Despite reports with low fixation failure rates in cervical deformity cohorts, surgeons should be aware of these risks if corpectomy or osteotomies are necessary for deformity correction. We present a case of hardware failure and screw pullout in ▶ Fig. 18.1.
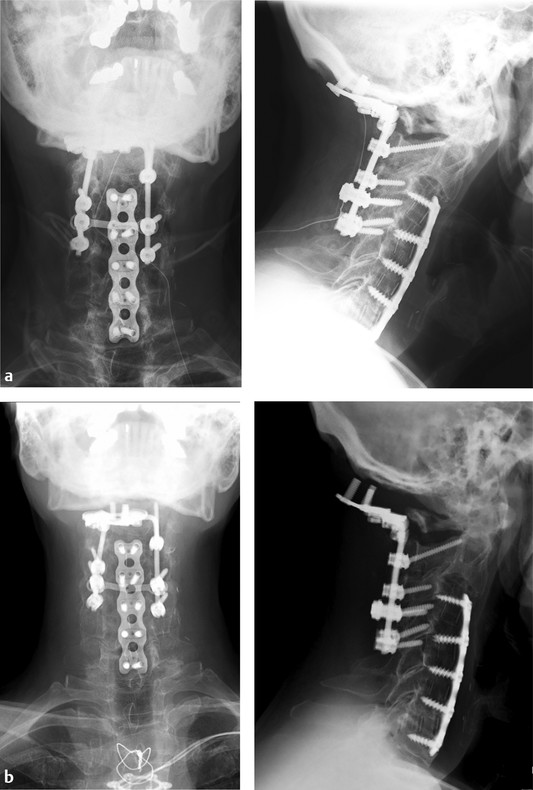
Fig. 18.1 Case example: This 62-year old male had a previous C3–C7 anterior cervical discectomy performed several years prior. He had been recently treated by another surgeon and underwent a posterior procedure occiput to C5 for cervical spondylosis and myelopathy (a). He presented 10 days after surgery with complaints that he could feel that his plate was loose and he had an inability to maintain a horizontal gaze (b). He underwent a revision procedure and was found to have a failed fixation proximally as well as a pseudarthrosis at C6–C7. Revision included occiput to C7 instrumentation, structural allograft augmentation from occiput to C2, along with off-label use of recombinant human bone morphogenetic protein-2 and iliac crest autograft.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


