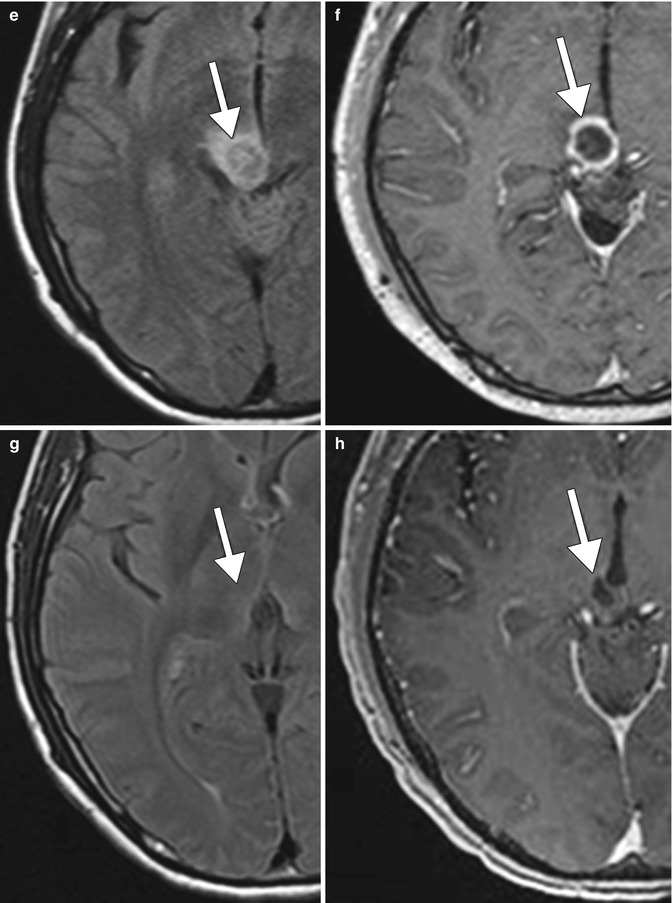
Fig. 17.1
Pseudoprogression. A 32-year-old male with right thalamic glioblastoma treated with surgical debulking followed by temozolamide (TMZ) and radiation (XRT). Serial axial FLAIR (a, c, e, g) and T1 post-contrast (b, d, f, h) MR images show that the right thalamic glioblastoma (arrows) responds to initial treatment then increases in size following TMZ plus XRT with a subsequent decrease in size and enhancement on follow-up
17.4 Differential Diagnosis
The main differential considerations for pseudoprogression are true tumor progression (Fig. 17.2) and radiation necrosis (Fig. 17.3). The timing of the imaging findings and serial imaging can help differentiate pseudoprogression from true tumor progression. Unlike tumor progression, there is stabilization or eventual decrease in tumor enhancement on follow-up imaging with pseudoprogression. Furthermore, pseudoprogression is observed only in the first few months after treatment, much earlier than radiation necrosis. Various enhancement patterns on MRI have been described with radiation necrosis, including advancing wavefront, cut-pepper appearance, soap bubble appearance, and Swiss cheese appearance. However, the findings are somewhat subjective and there can be substantial overlap between treatment changes and true tumor progression. Diffusion-weighted imaging may provide additional insights: true progression tends to display homogeneous or multifocal high signal intensity on DWI, while peripheral high signal or no high signal on DWI is more characteristic of pseudoprogression. With regards to MR perfusion imaging, it has been found that cases with unmethylated MGMT promoter have a significant difference of mean rCBV between pseudoprogression and real progression, while cases with methylated MGMT promoter have no significant difference. On MR spectroscopy, there is a significant increase in the Cho/NAA and Cho/Cre ratios in areas of recurrent tumor compared with areas of treatment-induced necrosis and normal brain tissue. Ultimately, currently available imaging techniques are not 100 % sensitive or specific in diagnosing progression. Furthermore, the frequent coexistence of treatment-induced necrosis and tumor progression can be a confounding factor when interpreting the imaging studies.
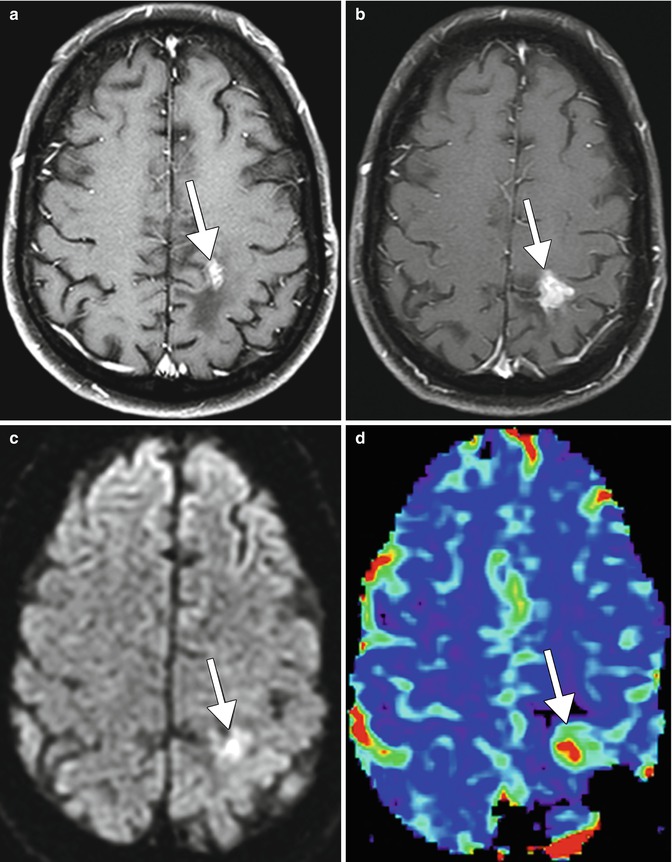





Fig. 17.2
True tumor progression. Axial post-contrast T1-weighted MRI (a) shows an enhancing focus in the left paracentral lobular (arrow). Follow-up post-contrast T1-weighted MRI (b) obtained 6 months later shows interval increase in size of the lesion (arrow). There is corresponding high signal on DWI (c) and elevated perfusion on the rCBV map (d) (arrows)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








