T2-weighed MRI for: (a) a 83-year-old female, multiple lesions in white matter seen on MRI, (b) a 76-year-old male with recurrent ischemic stroke and lesions with hemorrhagic transformation in left frontal parietal area, (c) a 55-year-old female with chronic ischemic stroke in right middle cerebral artery area
Enrolled subject demographic characteristics
Group | Age, mean ± SD | Male | Female | ||
|---|---|---|---|---|---|
N | % | N | % | ||
SC infarction | 56.8 ± 3.3 | 17 | 63.0 | 10 | 37.0 |
Posttraumatic myelopathy (PTM) | 46.7 ± 2.1 | 15 | 60.0 | 10 | 40.0 |
Radiculopathy (Rad) | 57.0 ± 1.7 | 18 | 56.3 | 14 | 43.7 |
Ischemic stroke (IS) | 56.6 ± 1.5 | 17 | 56.7 | 13 | 43.3 |
Healthy subjects | 50.2 ± 3.6 | 8 | 53.3 | 7 | 46.7 |
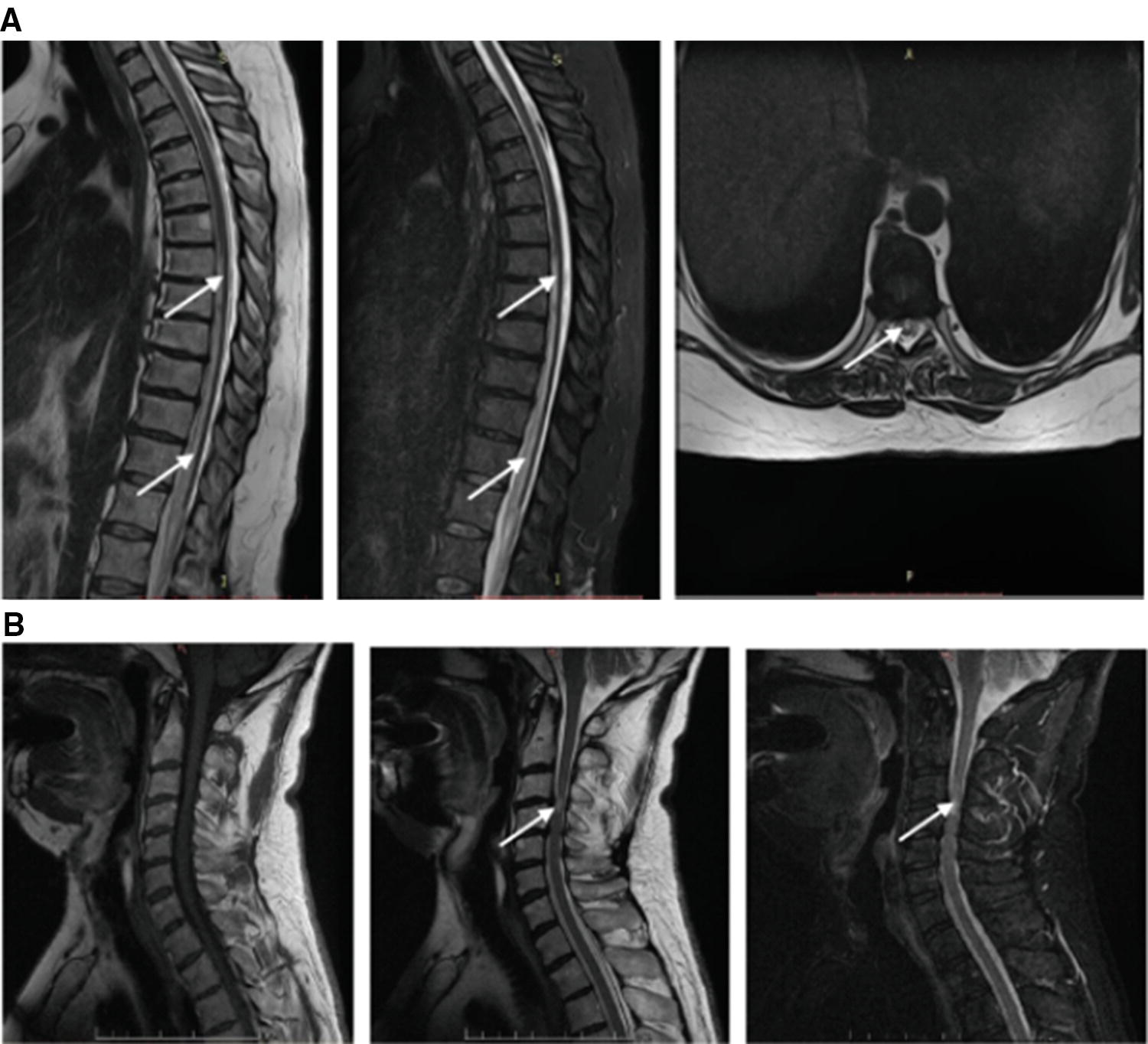
Spinal cord MRI sequences (left-to-right): (a) thoracic spine area: T2 (1, 3) and STIR (2) of a 47-year-old female with spinal stroke in the ASA territory and Factor V Leiden thrombophilia (arrows indicate prolong hyperintensities on level of T7–L1). (b) cervical spine area T1 (1), T2 (2), and STIR (3) of a 56-year-old male patient with ischemic myelopathy due to protrusion on the C3–C4 (arrow indicates hyperintensity of lesion and edema on level C4)
Among the main causes of SC infarction (Ia subgroup), herniated intervertebral discs in 12 (44.4%) cases, arteriovenous malformations in 6 (22.2%) patients, and thrombotic coagulopathies in 3 (11.1%) cases were diagnosed. In 6 (22.2%) patients, the cause of SC infarction could not be established at the time of the study. The isolated lesion of cervical segments in 10 (37%), thoracic segments in 6 (22.2%), and lumbosacral in 2 (7.4%) were defined by MRI. There were observed lesions spread within cervical/thoracic areas (n = 3, 11.1%) and thoracolumbar region (n = 6, 22.2%).
In the PTM subgroup Ib, spinal cord injury was more common in the form of household trauma in 13 (52%) cases, motor vehicle accidents in 7 (28%) cases, acts of violence in 3 (12%) patients, and sport-related injuries in 2 (8%) cases.
Lesion volumes in patients with SC infarction and PTM defined by MRI
Lesion volume, mL | SC infarction (n = 27) | PTM (n = 20a) | ||
|---|---|---|---|---|
N | % | N | % | |
<1.0 | 5 | 18.5 | 2 | 10 |
1–3 | 6 | 22.2 | 4 | 20 |
3–5 | 4 | 14.8 | 6 | 30 |
6–8 | 7 | 25.9 | 6 | 30 |
>8 | 5 | 18.5 | 2 | 10 |
3.2.2 NR2 Antibody Results
Evaluation of NR2 antibodies in serum of patients
Group | N | Gender | NR2 Ab ng/mL | p a | |||
|---|---|---|---|---|---|---|---|
M | F | Median [Q25; Q75] | Average | Maximum | |||
SC infarction | 27 | 17 | 10 | 1.92 [1.60; 2.45] | 2.30 | 8.12 | – |
PTM | 25 | 15 | 10 | 1.51 [1.29; 1.98] | 1.63 | 3.50 | 0.45 |
IS | 30 | 17 | 13 | 1.46 [0.99; 2.42] | 1.96 | 9.37 | 0.18 |
Rad | 32 | 18 | 14 | 1.25 [0.87; 1.59] | 1.29 | 2.58 | 0.0001 |
Healthy subjects | 15 | 8 | 7 | 1.30 [1.01; 1.53] | 1.31 | 2.22 | 0.013 |
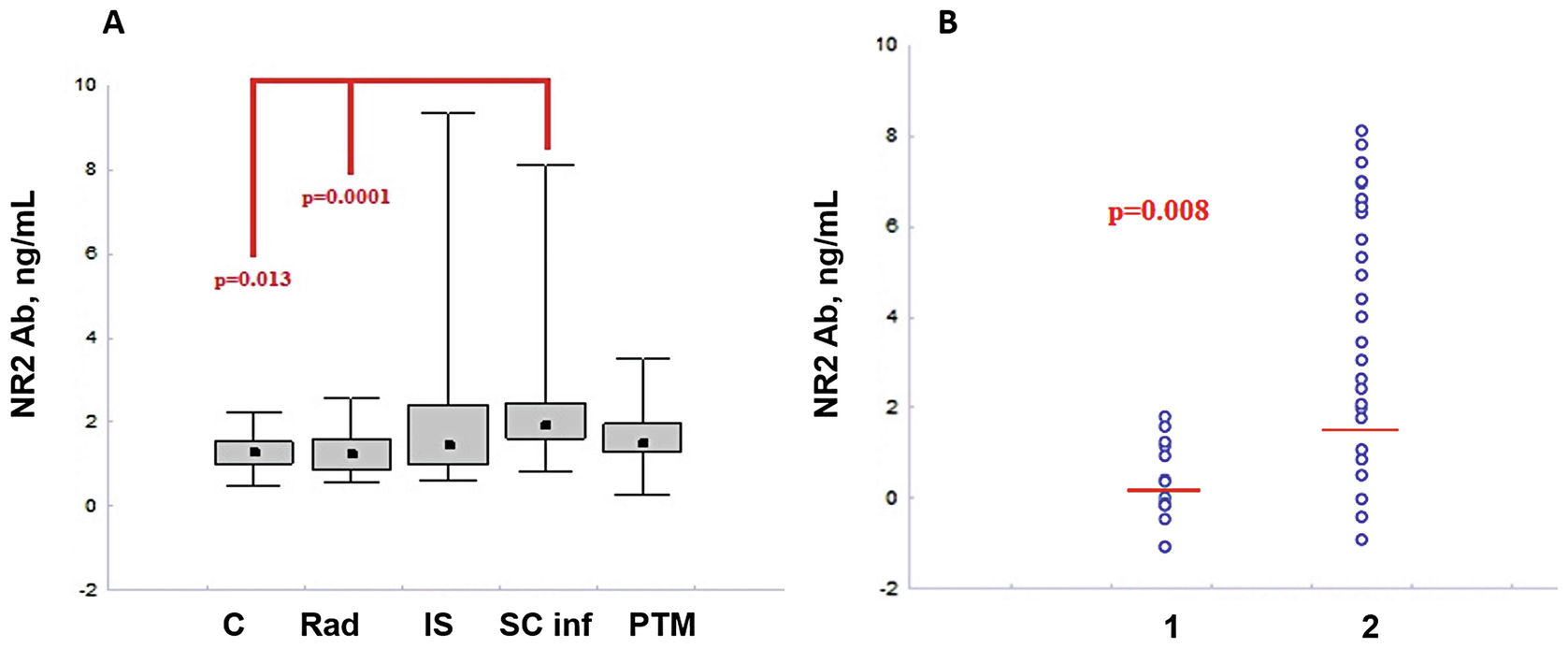
NR2 Ab levels in serum of subject (a) healthy (C), radiculopathy (Rad), IS, SC infarction, and post-traumatic myelopathy (PTM), Kruskal–Wallis and post hoc tests, Mann–Whitney U test, median [25; 75], (b) patients with traumatic myelopathy (1) and SC infarction (2), Mann–Whitney U test

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


