PHYSICAL TREATMENTS
Pharmacotherapy (drug treatment)
As mentioned in the preface, it is highly recommended that the reader always refers to the most up-to-date formulary available when prescribing drugs. (In the UK this is the most recent edition of the British National Formulary.)
Antipsychotic drugs (neuroleptics)
Main uses
The treatment of schizophrenia, the acute symptoms of mania, and psychotic symptoms arising from organic disorders and psychoactive substance use.
In the UK, the National Institute of Health and Clinical Excellence (NICE) issued the following guidance (in June 2002) on prescribing atypical antipsychotics for schizophrenia:
• The atypical antipsychotics (amisulpride, olanzapine, quetiapine, risperidone and zotepine) should be considered when choosing first-line treatment of newly diagnosed schizophrenia
• An atypical antipsychotic is considered the treatment option of choice for managing an acute schizophrenic episode when discussion with the individual is not possible
• An atypical antipsychotic should be considered for an individual who is suffering unacceptable side effects from a conventional antipsychotic
• Changing to an atypical antipsychotic is not necessary if a conventional antipsychotic controls symptoms adequately and the individual does not suffer unacceptable side effects
• Clozapine should be introduced if schizophrenia is inadequately controlled despite the sequential use of two or more antipsychotics (one of which should be an atypical antipsychotic) each for at least 6–8 weeks.
(Note that aripiprazole was introduced into the UK market after the above NICE guidelines were published.)
Examples
Typical (conventional or standard) antipsychotics include chlorpromazine, haloperidol, trifluoperazine, fluphenazine, zuclopenthixol and flupentixol. Atypical antipsychotics include amisulpride, aripiprazole, clozapine, olanzapine, quetiapine, risperidone and zotepine.
Mode of action
Typical antipsychotics cause central postsynaptic blockade of dopamine D2 receptors. Atypical antipsychotics have a much greater action than typical antipsychotics on other receptors, such as other dopamine receptors and serotonin (5-HT) receptors.
Administration
Oral, intramuscular and rectal suppositories are available for chlorpromazine. Slow-release depot preparations administered by deep intramuscular injection, usually at intervals of 2–8 weeks, are available (e.g. the typical antipsychotics flupentixol decanoate, fluphenazine decanoate, haloperidol decanoate, pipotiazine palmitate and zuclopenthixol decanoate, and the atypical antipsychotic risperidone).
Main side effects
The antidopaminergic action on the tuberoinfundibular system leads to hyperprolactinaemia, which in turn causes galactorrhoea, gynaecomastia, menstrual disturbances, reduced sperm count and reduced libido.
Peripheral antimuscarinic (anticholinergic) actions lead to dry mouth, blurred vision, urinary retention and constipation.
Central antimuscarinic actions lead to convulsions and pyrexia.
Antiadrenergic actions lead to postural hypotension and failure of ejaculation.
Antihistaminic actions lead to drowsiness.
A serious side effect is the neuroleptic malignant syndrome, a rare but potentially fatal toxic delirious state characterized by hyperthermia, a fluctuating level of consciousness, muscular rigidity and autonomic dysfunction (tachycardia, labile blood pressure, pallor, sweating and urinary incontinence); abnormal investigation results include increased creatinine phosphokinase, increased white blood count (WBC) and abnormal liver function tests. Neuroleptic malignant syndrome requires urgent medical treatment.
Long-term high-dose treatment with chlorpromazine leads to eye and skin changes (e.g. opacities of the lens and cornea) and a purplish pigmentation of the skin, conjunctiva, cornea and retina.
An important side effect of clozapine is neutropenia, and so regular haematological monitoring is required. Some of the atypical antipsychotics (particularly clozapine, olanzapine and zotepine) can cause electrocardiographic (ECG) changes and therefore ECG should be carried out at baseline and at regular intervals after commencing antipsychotic treatment; they should be prescribed with care, if at all, if patients are already taking other drugs that cause prolongation of the QT interval. (The use of one atypical antipsychotic drug, sertindole, has been associated with sudden death; it is now available in the UK on a named-patient basis only.) Caution should also be exercised if considering prescribing atypical antipsychotics for patients with cardiovascular disease or a history of epilepsy, and for those who are elderly.
Weight gain, hyperglycaemia and occasionally type 2 diabetes mellitus may occur as side effects of some of the atypical antipsychotics, particularly clozapine and olanzapine. Patients should therefore be regularly weighed and their blood glucose levels regularly monitored.
Antimuscarinic (anticholinergic) drugs
Main uses
The treatment of parkinsonian symptoms resulting from antipsychotic pharmacotherapy. They should not be prescribed routinely, but only if parkinsonism occurs.
Examples
Benzatropine (previously named benztropine), orphenadrine, procyclidine and trihexyphenidyl (previously named benzhexol).
Mode of action
Antimuscarinic action.
Administration
Procyclidine and benzatropine can be administered orally, intramuscularly and intravenously. Parenteral administration is used in acute dystonic reactions (tongue protrusion, grimacing, opisthotonus, spasmodic torticollis or oculogyric crisis).
Main side effects
Antimuscarinic (see above). They can also worsen tardive dyskinesia and affect memory.
Lithium salts
Main uses
The prophylaxis of bipolar mood disorder and recurrent depression. The treatment of resistant depression, (hypo)mania, aggression and self-mutilation. (Antipsychotics act more rapidly than lithium in the treatment of (hypo)mania.)
Examples
Lithium carbonate and lithium citrate.
Administration
Oral.
Monitoring
Renal function must be checked before starting lithium, as the drug is excreted by the kidneys.
Once on treatment, regular monitoring of plasma levels is required (these should be between 0.4 and 1.0mmol/l, 8–12 hours postdose, for prophylactic purposes) because of its low therapeutic/toxic ratio. Urea, electrolytes and the creatinine level must also be regularly monitored to check renal function. Thyroid function tests should be checked regularly because thyroid function disturbances can result from long-term lithium therapy.
Main side effects
Gastrointestinal side effects, fine tremor, dry mouth, polyuria, polydipsia, weight gain and oedema (Fig. 16.1). Oedema should not be treated with diuretics because thiazide and loop diuretics reduce lithium excretion and so can cause lithium intoxication.
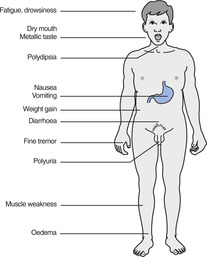 |
| Figure 16.1 (With permission from Puri BK, Laking PJ, Treasaden IH 2002 Textbook of psychiatry. Churchill Livingstone, Edinburgh.) |
Signs of lithium intoxication are shown in Figure 16.2.
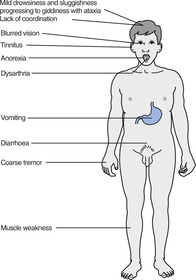 |
| Figure 16.2 (With permission from Puri BK, Laking PJ, Treasaden IH 2002 Textbook of psychiatry. Churchill Livingstone, Edinburgh.) |
Long-term treatment can lead to thyroid function disturbances (goitre, hypothyroidism, hyperthyroidism), memory impairment, nephrotoxicity and cardiovascular changes (T-wave flattening and arrhythmias).
It is useful to give the patient a lithium card describing the side effects, how to take the lithium, the need for regular blood monitoring and the need to keep up an adequate fluid intake and avoid dietary changes that may cause changes in the sodium intake.
Carbamazepine
Main uses
Instead of, or in combination with, lithium in cases of bipolar affective (mood) disorder resistant to lithium, resistant mania and resistant depression. Also used in epilepsy and trigeminal neuralgia.
Administration
Oral.
Monitoring
The full blood count and liver function tests should be checked before starting the drug. Once started, regular monitoring of the plasma carbamazepine level allows the optimum dosage to be determined. The full blood count should be checked regularly because carbamazepine may depress the WBC. Regular monitoring of liver function tests is also advisable as carbamazepine may cause hepatic damage; this is particularly important in those with a history of liver disease.
Similarly, baseline and regular monitoring of renal function, including full urinalysis, are advisable because of the association of carbamazepine with renal dysfunction.
If possible, baseline and regular ocular examinations (including slit-lamp investigations, funduscopy and tonometry) are also advisable, because of the possibility of ocular side effects (such as punctuate cortical lens opacities and conjunctivitis).
It is recommended that patients and their carers be told how to recognize clinical features of blood, hepatic or skin disorders. They should be informed of the need to seek immediate medical attention if fever, sore throat, rash, mouth ulcers, bruising or bleeding develop.
Tricyclic antidepressants
Main uses
The treatment of depressive illness, obsessive–compulsive disorder, generalized anxiety disorder, panic disorder and phobic disorders. In children they are used in low doses to treat nocturnal enuresis.
Examples
Imipramine (less sedating), amitriptyline (more sedating), clomipramine and lofepramine (less toxic).
Mode of action
Their use in treating enuresis is a result of their antimuscarinic action leading to urinary retention.
Administration
Usually orally. Preparations for intramuscular and intravenous administration are also available for some tricyclic antidepressants.
Main side effects
Peripheral and central antimuscarinic side effects (e.g. dry mouth, blurred vision, constipation, urinary retention, sedation and nausea).
Cardiovascular side effects include ECG changes (T-wave flattening, prolongation of QT interval and ST depression), postural hypotension and arrhythmias.
Other side effects are shown in Figure 16.3.
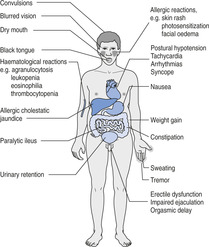 |
| Figure 16.3 (With permission from Puri BK, Laking PJ, Treasaden IH 2002 Textbook of psychiatry. Churchill Livingstone, Edinburgh.) |
In overdose tricyclic antidepressants are toxic, causing cardiac conduction defects, arrhythmias, convulsions, respiratory failure, coma and death.
Selective serotonin reuptake inhibitors (SSRIs)








