Viral Infections of the Nervous System, Chronic Meningitis, and Prion Diseases: Introduction
A number of viruses share the unique tendency to primarily affect the human nervous system. Included in this group are the human immunodeficiency viruses (HIV-1 and HIV-2), herpes simplex viruses (HSV-1 and HSV-2), herpes zoster or varicella zoster virus (VZV), Epstein-Barr virus (EBV), cytomegalovirus (CMV), poliovirus, rabies, and several seasonal arthropod-borne viruses (Flaviviruses). Some of these are neurotropic, exhibiting an affinity for certain types of neurons: for example, poliomyelitis viruses and motor neurons, VZV and peripheral sensory neurons, and rabies virus and brainstem neurons. Yet others attack nonneuronal supporting glial cells; JC virus causing progressive multifocal leukoencephalopathy is the prime example. For many of the rest, the affinity is less selective in that all elements of the nervous system are involved. Herpes simplex, for example, may devastate the medial parts of the temporal lobes, destroying neurons, glia cells, myelinated nerve fibers, and blood vessels; and HIV may induce multiple foci of tissue necrosis throughout the cerebrum. These relationships and many others, which are the subject of this chapter, are of wide interest in medicine. In some conditions, the systemic effects of the viral infection are negligible; it is the neurologic disorder that brings them to medical attention.
Viruses gain entrance to the body by one of several ways. Mumps, measles, and VZV enter via the respiratory passages. Polioviruses and other enteroviruses enter by the oral–intestinal route, and HSV enters mainly via the oral or genital mucosal route. Other viruses are acquired by inoculation, as a result of the bites of animals (e.g., rabies), ticks, mites, or mosquitoes (arthropod-borne or arbovirus infections). The fetus may be infected transplacentally by rubella virus, CMV, and HIV. In all these cases, viremia is an intermediate step to seeding the brain or CSF.
Another pathway of infection is along peripheral nerves; centripetal movement of virus is accomplished by the retrograde axoplasmic transport system. HSV, VZV, and rabies virus utilize this peripheral nerve pathway, which explains why the initial symptoms of rabies occur locally, at a segmental level corresponding to the animal bite. It has been shown experimentally that HSV may spread to the CNS by involving olfactory neurons in the nasal mucosa; the central processes of these cells pass through openings in the cribriform plate and synapse with cells in the olfactory bulb (CNS). Another potential pathway is the trigeminal nerve and gasserian ganglion, however, the role of these pathways in human infection is not certain. Of the different routes of infection, the hematogenous one is by far the most important for the majority of viruses.
Additionally, VZV resides in the sensory ganglia and becomes reactivated later in life, causing shingles decades after the primary infection that produces chicken pox. The JC virus also is latent in tissues, possibly the kidney and bone marrow, only to reemerge under conditions of immunosuppression, to infect the brain.
Viruses, once they invade the nervous system, have numerous clinical and pathologic effects. One reason for this diversity is that different cell populations within the CNS vary in their susceptibility to infection with different viruses. To be susceptible to a viral infection, the host cell must have on its cytoplasmic membrane specific receptor sites to which the virus attaches. Thus, some infections are confined to meningeal cells, enteroviruses being the most common, in which case the clinical manifestations are those of aseptic meningitis. Other viruses involve particular classes of neurons of the brain or spinal cord, giving rise to the more serious disorders such as encephalitis and poliomyelitis. The virus or its nucleocapsid must be capable of penetrating the cell, mainly by the process of endocytosis, and of releasing its protective nucleoprotein coating. For viral reproduction to occur, the cell must have the metabolic capacity to transcribe and translate virus-coated proteins, to replicate viral nucleic acid, and, under the direction of the virus’s genome, to assemble virions. Certain agents depend on cell-surface receptors to ingress into the cell; these relationships have potential therapeutic interest as, for example, the use of serotonin receptor for entry of the JC virus into oligodendrocytes.
The pathologic effects of viruses on susceptible cells vary greatly. In acute encephalitis, neurons are invaded directly by virus and the cells undergo lysis. There is a corresponding glial and inflammatory reaction. Neuronophagia (phagocytosis of affected neurons and their degenerative products by microglia) is a mark of this phenomenon. In progressive multifocal leukoencephalopathy (PML), there is a selective lysis of oligodendrocytes, resulting in foci of demyelination. In certain congenital infections, e.g., measles and rubella, the virus persists in nervous tissue for months or years. In still other circumstances, a viral infection may exist in the nervous system for a long period before exciting an inflammatory reaction (e.g., subacute sclerosing panencephalitis, SSPE); in these cases the disease may be so indolent as to simulate a degenerative disease.
Differentiating cells of the fetal brain have particular vulnerabilities, and viral incorporation may give rise to malformations and to hydrocephalus; an example is mumps virus with ependymal destruction and aqueductal stenosis.
In experimental animals cerebral neoplasms can be induced when certain viral genomes are incorporated into the DNA of the host cell. There is suggestive evidence of such a mechanism relating to EBV in B-cell lymphoma of the brain. The prions have yet other means of affecting cells that do not conform to the traditional concepts of infection and are discussed in a later section of this chapter.
Clinical Syndromes
A large number of viruses are able to affect the nervous system. Among the enteroviruses alone, nearly 70 distinct serologic types are associated with CNS disease, and additional types from this family of viruses and others are still being discovered. There is no need, however, to consider them individually, as there are only a limited number of ways in which they express themselves clinically: (1) acute aseptic (“lymphocytic”) meningitis; (2) a less-common recurrent meningitis; (3) acute encephalitis and meningoencephalitis; (4) ganglionitis (herpes zoster); (5) chronic invasion of nervous tissue by retroviruses, i.e., HIV and tropical spastic paraparesis (TSP); (6) acute anterior poliomyelitis; (7) chronic viral infections including the agent causing PML and subacute sclerosing panencephalitis (SSPE) and (8) the prion agents that are discussed later in the chapter.
Acute Aseptic Meningitis
The term aseptic meningitis was first introduced to designate what was thought to be a specific disease—”aseptic” because bacterial cultures were negative. The term is now applied to a symptom complex that is produced by any one of a number of infective agents, the majority of which are viral but a few of which are bacterial (mycoplasma, Q fever, other rickettsial infections). Because aseptic meningitis is rarely fatal, the precise pathologic changes are uncertain but are presumably limited to the meninges. Conceivably, there may be some minor changes in the underlying brain itself, but these are of insufficient severity to cause neurologic symptoms and signs or to show changes on imaging studies.
In outline, the clinical syndrome of aseptic meningitis consists of fever, headache, signs of meningeal irritation, and a predominantly lymphocytic pleocytosis in the spinal fluid with normal glucose. Usually the onset is acute and the temperature is elevated, from 38 to 40°C (100.4 to 104°F). Headache that is more severe than that associated with other febrile states is the most frequent symptom. A variable but usually mild degree of lethargy, irritability, and drowsiness may occur. Photophobia and pain on movement of the eyes are common additional complaints. Stiffness of the neck and spine on forward bending attests to the presence of meningeal irritation (meningismus), but at first it may be so slight as to pass unnoticed. Here the Kernig and Brudzinski signs help little, for they are often absent in the presence of manifest viral meningitis. When there are accompanying neurologic signs, they too tend to be mild or fleeting: paresthesia in an extremity, or wavering Babinski signs.
Systemic symptoms and signs aside from fever are infrequent and depend mainly on the more mundane effects of the invading virus; these include sore throat, nausea and vomiting, vague weakness, pain in the back and neck, conjunctivitis, cough, diarrhea, vomiting, rash, petechia, hepatitis, adenopathy, or splenomegaly. The childhood exanthems associated with meningitis and encephalitis (varicella, rubella, mumps) produce well-known eruptions and other characteristic signs. An erythematous papulomacular, nonpruritic rash, confined to the head and neck or generalized, may also be a prominent feature, particularly in children, of certain echoviruses and Coxsackie viruses. An enanthem (herpangina), taking the form of a vesiculoulcerative eruption of the buccal mucosa, may also occur with these viral infections.
In milder cases, in the first hours or day of the illness, there may be no abnormalities of the spinal fluid, and the patient may erroneously be thought to have migraine or a headache induced by a systemic infectious illness. Microorganisms cannot be demonstrated by conventional smear or culture. As a rule, the glucose content of the CSF is normal; but infrequently, mild depression of the CSF glucose (never below 25 mg/dL) occurs with the meningitis caused by mumps, HSV-2, lymphocytic choriomeningitis, or VZV.
Aseptic meningitis is a common occurrence, with an annual incidence of approximately 20 cases per 100,000 population (Beghi et al; Ponka and Pettersson). Most are caused by viral infections. Of these, the most common are from enterovirus—mainly echovirus and Coxsackie virus. These make up 80 percent of cases in which a specific viral cause can be established. HSV-2 is perhaps next in frequency in adults, followed by varicella, HIV, mumps in children, lymphocytic choriomeningitis (LCM), HSV-1, and adenovirus infections. The next most frequent group comprise EBV (infectious mononucleosis), CMV, leptospira, HSV-1, and the bacterium Mycoplasma pneumoniae (see Chap. 32), and in some parts of the world, tick-borne encephalitis virus and Borrelia, including the Lyme agent (Kupila et al), or during local outbreaks anywhere, arboviruses. Influenza virus, adenoviruses, and numerous sporadic and otherwise innocuous agents are at times isolated from the spinal fluid in cases of aseptic meningitis. The California and West Nile viruses, which are arthropod-borne viruses (“arboviruses” in the family of Flaviviruses) are responsible for a small number of cases; they usually cause an encephalitis or meningoencephalitis in brief regional outbreaks as discussed further on.
It is also recognized that infection with HIV may present as acute, self-limited aseptic meningitis with an infectious mononucleosis-like clinical picture. While HIV has been obtained from the CSF in the acute phase of the illness, seroconversion occurs only later, during convalescence from the meningitis (see further on). HSV-1 has been isolated from the CSF of patients with recurrent bouts of benign aseptic meningitis (so-called Mollaret meningitis), but this finding has not been consistent (Steel et al). As discussed in Chap. 47, it is now believed that this virus also underlies many if not most cases of what has been traditionally considered idiopathic Bell’s palsy.
Two other aspects of the virology of aseptic meningitis should be noted: first, in most published series of cases from virus isolation centers, a specific cause cannot be established in one-third or more of cases of presumed viral origin; second, most agents capable of producing aseptic meningitis also sometimes cause encephalitis.
Clinical distinctions between the many viral causes of aseptic meningitis cannot be made with high reliability, but useful clues can be obtained by attention to certain details of the clinical history and physical examination. Inquiry should be made regarding recent respiratory or gastrointestinal symptoms, immunizations, past history of infectious disease, family outbreaks, insect bites, contact with animals, and areas of recent travel. The presence of a local epidemic, the season during which the illness occurs, and the geographic location, are other helpful data.
Because the common enteroviruses, including polio, grow in the intestinal tract and are spread mainly by the fecal–oral route, family outbreaks are usual and the infections are most common among children. A number of echovirus and Coxsackie virus (particularly group A) infections are associated with exanthemata and may be associated with the grayish vesicular lesions of oral herpangina. Pleurodynia, brachial neuritis, pericarditis, and orchitis are characteristic of some cases of group B Coxsackie virus infections and there are certainly other causes. Pain in the back and neck and in the muscles should suggest poliomyelitis or dengue. Lower motor neuron weakness may also occur with echo, West Nile, and Coxsackie virus infections, but it is usually mild and transient in nature. The peak incidence of enteroviral infections is in August and September.
Mumps meningitis occurs sporadically throughout the year, but the highest incidence is in late winter and spring. Males are affected three times more frequently than females. Other manifestations of mumps infection—parotitis, orchitis, mastitis, oophoritis, and pancreatitis—may be, but most often are not, present. It should be noted that orchitis is not specific for mumps but occurs occasionally with group B Coxsackie virus infections, infectious mononucleosis, and lymphocytic choriomeningitis. A definite past history of mumps aids in excluding the disease as an attack confers lifelong immunity.
The natural host of the LCM virus is the common house mouse, Mus musculus. Humans acquire the infection by contact with infected hamsters or with dust contaminated by mouse excreta. Laboratory workers who handle rodents may be exposed to LCM. The meningitis may be preceded by respiratory symptoms, sometimes with pulmonary infiltrates. The infection is particularly common in late fall and winter, presumably because mice enter dwellings at that time.
Parvovirus causes fifth disease in young children, characterized by high fever and markedly flushed cheeks but not associated with neurologic symptoms beyond irritability and sometimes, febrile seizures. However, when contracted from the child by an adult, various neurologic manifestations such as brachial neuritis can occur. There have also been reports of encephalitis and meningitis with the B-19 strain, particularly in children and sometimes in individuals with altered immunity. By a difficult to understand complication, some patients have had strokes as discussed in the review by Douvoyiannis and colleagues.
HSV and HIV meningitis may be associated with a cauda equina neuritis. In the case of HSV, there is often a preceding genital infection with the virus (see Chap. 46). The presence of sore throat, generalized lymphadenopathy, transient rash, and mild icterus is suggestive of infectious mononucleosis caused by EBV or, at times, CMV infection. Icterus is a prominent manifestation of viral hepatitis and some serotypes of leptospirosis and, at times, of Q fever. Among the bacterial and spirochetal cause of an aseptic meningitis syndrome, leptospirosis, M. pneumoniae, and Lyme borreliosis are notable as discussed in the previous chapter.
Certain forms of encephalitis occur particularly in individual who are immunosuppressed from HIV, chemotherapy for neoplasm, organ transplantation, or hematologic and lymphoid malignancy. The manifestation is usually encephalitis but aseptic meningitis is known to occur. The main causative organisms in this group are HHV-6, CMV, and VZV.
Laboratory findings suggest certain organisms as the cause of aseptic meningitis. Most cases of infectious mononucleosis can be identified by the blood smear and specific serologic tests (heterophil or others). LCM should be suspected if there is an intense lymphocytic pleocytosis. Counts above 1,000 cells/mm3 in the spinal fluid, particularly if the cells are all lymphocytes, are most often due to LCM but may occur occasionally with mumps or echovirus 9. In the last of these agents, neutrophils may predominate in the CSF for a week or longer. Slightly depressed glucose in the spinal fluid is consistent with mumps meningitis and with the viruses mentioned earlier, but it is more often indicative of bacterial or fungal infection.
Liver function tests are abnormal in many patients with EBV infection and leptospiral infections; the hepatitis viruses are not known to produce meningitis. In the majority of patients with M. pneumoniae infections, cold agglutinins appear in the serum toward the end of the first week of the illness.
Panels of serologic tests for the main viruses that cause aseptic meningitis are available; most use complement fixation or enzyme-linked immunosorbent assay (ELISA) techniques; an infection is demonstrated by a fourfold increase in titer from acute to convalescent serum drawn at least 10 days apart, but these, of course, do no more than confirm the diagnosis after the illness has mostly passed. In some instances, elevation of specific IgM antibody directed at an infectious agent is useful. Serologic reactions of CSF for syphilis should be interpreted with caution, because inflammation of many types, including infectious mononucleosis, can produce a false-positive reaction. In the last few years, the polymerase chain reaction (PCR) has been applied to the diagnosis of viral infections of the nervous system, among them being CMV and HSV. The test is most sensitive during the active stage of viral replication, in contrast to serologic tests, which are more accurate later in the course of the infection. There are numerous false-negative and fewer false-positive PCR tests for CMV, but they are nonetheless useful in some circumstances, such as the early diagnosis of fulminant CMV infection in AIDS patients (see later in this chapter). For the most part, neither serologic nor PCR testing is required in clinical practice.
In addition to the aforementioned bacterial infections that can cause meningitis, several other categories of disease may cause a sterile, predominantly lymphocytic or mononuclear reaction in the leptomeninges: (1) foci of bacterial infection lying adjacent to the meninges, such as spinal or cranial epidural abscess (parameningeal infection); (2) partially treated bacterial meningitis; (3) meningeal infections in which the organism is difficult or impossible to isolate—fungal and tuberculous meningitis are at times in this category and parasitic infections are in this group; (4) neoplastic invasion of the leptomeninges (lymphomatous and carcinomatous meningitis); (5) granulomatous, vasculitic, or other inflammatory diseases such as sarcoidosis, Behçet disease, and granulomatous angiitis; and (6) acute or chronic recurrent inflammatory meningitides as a result of chemical irritation, drug-induced allergic reactions, including an aseptic chemical meningitis incited by rupture of a craniopharyngioma or other cystic structure containing proteinaceous fluid. These are described further on under “Chronic Persistent and Recurrent Meningitis.” (7) Rarely, children with scarlet fever or streptococcal pharyngitis develop meningeal signs and slight pleocytosis, the result of a sterile serous inflammation that does not involve invasion of the meninges by organisms. The same occurs in bacterial endocarditis.
An idiosyncratic, presumably immunologic meningitis may result from the use of nonsteroidal antiinflammatory drugs, intravenous immune globulin (due probably to a carrier chemical in the solution), and, rarely, from other drugs, including certain antibiotics. Individuals with systemic lupus erythematosus have an increased risk of aseptic meningitic reactions to antiinflammatory medications.
In respect to the first two categories, parameningeal and partially treated bacterial infections, smoldering paranasal sinusitis or mastoiditis may produce a CSF picture of aseptic meningitis because of epidural or subdural extension into the intracranial compartments; it is infrequent that the entire syndrome of meningitis is present. Uncomplicated sinusitis alone does not cause a meningeal reaction.
Antibiotic therapy given for a systemic or pulmonary infection may suppress a bacterial meningitis to the point where mononuclear cells predominate, glucose is near normal, and organisms cannot be cultured from the CSF although they may still be evident by Gram stain. Careful attention to the history of recent antimicrobial therapy permits recognition of these cases.
Syphilis, cryptococcosis, and tuberculosis are the important members of the third group that cause aseptic meningitis and in which the organism may be difficult to culture, as detailed in Chap. 32. Tuberculous meningitis, in its initial stages, may masquerade as innocent aseptic meningitis and the diagnosis may be delayed. Similarly, the diagnosis of cryptococcosis, other fungal infection, or nocardiosis is occasionally missed because the organisms may be present in such low numbers as to be overlooked in smears, especially in AIDS patients. Brucellosis (Mediterranean fever, Malta fever) is a rare disease that may present as an acute meningitis or meningoencephalitis, with the CSF findings of aseptic meningitis. The diagnosis depends on the detection of high serum antibody titers and Brucella-specific immunoglobulins, using the ELISA or serum agglutination testing.
In the neoplastic group, leukemias and lymphomas are the most common sources of meningeal infiltrations. In children, leukemic “meningitis” with cells (lymphoblasts or myeloblasts) in the CSF numbering in the thousands may occur. In leptomeningeal metastases (carcinomatous meningitis), neoplastic cells extend throughout the leptomeninges and involve cranial and spinal nerve roots, producing a picture of meningoradiculitis with normal or low CSF glucose values. Lymphocytic meningitis that is accompanied by cranial-nerve palsies may prove to be tuberculous if the patient is febrile and the CSF glucose is low (or even without these signs in an endemic area); it is likely to be neoplastic if the patient is afebrile and the CSF glucose is normal or mildly decreased. Concentrated cytologic preparations usually permit identification of the tumor cells. Chapter 31 discusses neoplastic meningitis in detail.
Occlusion of many small cerebral blood vessels by cholesterol emboli may also excite a reaction in meningeal vessels and a pleocytosis that includes eosinophils.
Chronic Persistent and Recurrent Meningitis
Infectious |
Tuberculosis and atypical mycobacterial |
Fungal (cryptococcal, coccidial, histoplasmal, blastomyces, etc.) |
Nocardia |
HIV |
Herpes type 2 (recurrent Mollaret meningitis) |
Lyme disease |
Syphilis |
Brucellosis |
Epidural abscess or hematoma |
Incompletely treated bacterial meningitis |
Granulomatous and vasculitic |
Sarcoidosis |
Wegener granulomatosis |
Behçet disease |
Vasculitis |
IgG-4 pachymeningitis |
Neoplastic |
Carcinomatous |
Lymphomatous |
Leukemic |
Allergic |
Nonsteriodal antiinflammatory drugs |
IVIg |
Antibiotics |
Other medications |
Chemical |
Leakage from epidermoid tumor, dermoid cyst, craniopharyngioma, or teratoma |
Instillation of irritative substances by lumbar puncture, spinal anesthesia, or surgery |
Idiopathic |
Vogt-Kayanagi-Harada disease |
No cause determined in one-third of cases |
Chronic and recurrent meningitides always pose diagnostic problems. Such patients may have a low-grade fever, headache of varying severity, stiff neck, and a predominantly mononuclear pleocytosis, sometimes with slightly raised CSF pressure. There may be limited focal neurologic signs such a slight pronator drift or Babinski sign. A viral or some other type of infective inflammation is always suspected, but a search by culture methods and serology usually yields negative results. Herpesvirus has been demonstrated to be the cause of a few cases, as in the recurrent Mollaret type of meningitis noted later. The process often improves without identification of the cause over a period of months or a year or more; in other cases, the cause is eventually found. Only a few end fatally.
In a group of such patients studied at the Mayo Clinic, 33 of 39 underwent a natural resolution and 2 died; 14 were still symptomatic at the time of the report (Smith and Aksamit). In another series from New Zealand of 83 patients, Anderson and colleagues ultimately found tuberculosis to be the most common identifiable cause, a smaller number being accounted for by neoplastic and cryptococcal meningitis; in fully one-third of the patients, no cause could be established. Charleston and colleagues reported a subgroup of these patients who were responsive to steroids; in only 7 of 17 patients could medication eventually be withdrawn without recurrence; 4 required treatment indefinitely; and the remaining 6 died after many months or years. The outcome and response to steroids in our patients have been much the same. These series excluded chemical or irritative meningitis, which should be considered if there had been spinal surgery or infusion of even apparently innocuous substances into the spinal space.
The special problem of chronic neutrophilic meningitis has been mentioned in the preceding chapter in relation to Nocardia, Aspergillus, Actinomyces, or certain Mycobacterium species; other causes include coccidioidomycosis, histoplasmosis, and blastomycosis, (see Peacock, cited in Chap. 32).
A reasonable approach in patients with chronic meningitis is to repeat the lumbar puncture several times to obtain all cultures including for fungi and cytology of CSF, using markers to detect uniform populations of B and T lymphocytes and tumor cells, biochemical tests that are sensitive to neoplastic meningitis (such as β2-microglobulin, lactate dehydrogenase [LDH]), and PCR amplification of herpesviruses, serologic tests mainly for HIV, syphilis, coccidioidomycosis, Brucella, and Lyme disease. MRI of the brain and spinal cord with gadolinium should also be performed to detect parameningeal collections. If hydrocephalus develops, it should be managed along the lines described in Chap. 30.
A trial of antiviral agents and broad-spectrum antibiotics may be justified, although we have had limited success with them in our last several patients. We resort to a biopsy of the meninges over the frontal convexity or at a site that demonstrates infiltration or marked enhancement if the diagnosis has not been clarified in 6 to 12 months or if febrile meningitis persists for more than several weeks, but examination of this tissue has also proved to be of limited value. In Anderson’s (1995) series, mentioned earlier, biopsy yielded a diagnosis in 5 of 25 patients. Finally, if bacterial infection has been reasonably excluded, corticosteroids are administered for several weeks and then tapered while observing the patient and resampling the CSF.
The CSF formula in a number of other chronic or acutely recurring meningitides corresponds to that of aseptic meningitis. These include (1) the Vogt-Koyanagi-Harada syndrome, which is characterized by combinations of iridocyclitis, depigmentation of a thick swath of hair (poliosis circumscripta) and of the skin, vitiligo, around the eyes, loss of eyelashes, dysacusis, and deafness (the pathologic basis of the syndrome is not known); and (2) Mollaret recurrent meningitis, many instances of which have been associated with HSV-1 (Steel) and others (perhaps most) with HSV-2 infection (Cohen et al). The syndrome is characterized by episodes of acute meningitis with severe headache and sometimes low-grade fever, lasting for about 2 weeks, and recurring over a period of several months or years. In a few patients of ours, in whom no virus could be identified in the CSF, antiviral therapy met with some success, although corticosteroids seemed to reduce the severity of acute episodes. A proportion of these cases follow bouts of genital herpes and individual cases have been reported with EBV, herpes-6 in children, and other viruses. A special syndrome that has been associated with HSV-2 is that of aseptic meningitis and bladder failure and vaginal or vulvar pain after a bout of genital herpes (Elsberg syndrome as reviewed by Ellie and colleagues); (3) In some patients, the recurrent attacks are associated with encephalopathy and headache; this is probably identical to the illness called “pseudomigraine with temporary neurological symptoms” by Gomez-Aranda and described earlier by Bartleson. The entity, also known as HaNDL syndrome (“headache neurologic deficit and lymphocytic pleocytosis”) is allied more closely with the headache syndromes as discussed and cited in Chap. 10. (4) Allergic or hypersensitivity meningitis, in the past occurring in the course of serum sickness and now more commonly of autoimmune diseases such as lupus erythematosus, and in relation to certain medications such as nonsteroidal antiinflammatory drugs and intravenously administered immunoglobulin. (5) Behçet disease, which is an important acute, recurrent inflammatory CNS disease, particularly in individuals of Middle Eastern origin. It is essentially a diffuse inflammatory disease of small blood vessels that has several other characteristic features such as oral and genital ulcers and is more appropriately considered with the vasculitides in Chap. 34.
In summary, the temporal history of the illness, associated clinical findings, and laboratory tests usually provide clues to the diagnosis of nonviral and chronic forms of aseptic meningitis. It is useful to keep in mind the possibility of neoplasia, HIV, tuberculosis, cryptococcosis, sarcoidosis, syphilis, borreliosis, parameningeal collection, and inadequately treated bacterial meningitis—each of which presents an urgent diagnostic problem.
Acute Encephalitis
From the foregoing discussion it is evident that the separation of the clinical syndromes of aseptic meningitis and encephalitis is not always clear. In some patients with aseptic meningitis, mild drowsiness or confusion may be present, suggesting cerebral involvement. Conversely, in some patients with encephalitis, the cerebral symptoms may be mild and meningeal symptoms and CSF abnormalities predominate. The common practice is to assume that viral meningitis causes only fever, headache, stiff neck, and photophobia; if any other CNS symptoms are added, the condition is generally called meningoencephalitis. As has been emphasized, the same spectrum of viruses gives rise to both meningitis and encephalitis. It is our impression that many cases of enteroviral and practically all cases of mumps and LCM encephalopathy are little more than examples of intense meningitis in which the subpial surface of the brain is inflamed. Rarely have they caused demonstrable postmortem cerebral lesions, and surviving patients have no residual neurologic signs. Conversely, several agents, notably the arboviruses, may cause encephalitic lesions with only mild meningeal symptoms.
The core of the encephalitis syndrome consists of an acute febrile illness with evidence of various combinations of seizures, delirium, confusion, stupor or coma; aphasia, hemiparesis with asymmetry of tendon reflexes and Babinski signs, involuntary movements, ataxia, and myoclonic jerks; and nystagmus, ocular palsies, and facial weakness. The meningitic component may be intense, have mild manifestations such as headache, or be entirely inapparent. The spinal fluid invariably shows a cellular reaction and the protein is slightly elevated. Imaging studies of the brain are most often normal but may show diffuse edema or enhancement of the cortex and, in certain infections, subcortical and deep nuclear involvement as well as, in the special case of HSV encephalitis, selective damage of the inferomedial temporal and frontal lobes.
The acute encephalitis syndrome described above may take two forms: the more common direct invasion of brain and meninges (true viral encephalitis) and a postinfectious encephalomyelitis that is presumably based on an autoimmune reaction to the systemic viral infection but in which virus is not present in neural tissue. The distinction between postinfectious encephalomyelitis and infectious encephalitis may be difficult, especially in younger patients who have a proclivity to develop the postinfectious variety with fever. The latter, termed acute disseminated encephalomyelitis (ADEM), occurs after a latency of several days, as the infectious illness is subsiding. It is expressed by a low-grade fever and cerebral symptoms such as confusion, seizures, coma, or ataxia. The spinal fluid shows slight inflammation and elevation of protein—sometimes a more intense reaction, and there are usually characteristic confluent, scattered, bilateral lesions in the white matter in imaging studies, findings that differ from those of viral encephalitis. When there is no coexistent epidemic of encephalitis to suggest the diagnosis, or the preceding systemic illness is absent or obscure, a differentiation between the two may not be possible on clinical grounds alone. The fever is generally higher in the infectious type but even this difference does not always hold in young children with ADEM. The encephalitis that follows certain childhood exanthems (postexanthematous) and vaccinations at any age (postvaccinal) are essentially forms of ADEM.
Because ADEM is predominantly an inflammatory and demyelinative process, we mention it here but discuss its clinical features and imaging more fully in Chap. 36, with the other demyelinating diseases such as multiple sclerosis, with which it shares some features. We also place in special categories further on the now rare Reye syndrome of postinfectious acute encephalopathy with hepatic failure that follows influenza, and other viral infections and postinfectious cerebellitis.
Whereas numerous viral, bacterial, fungal, and parasitic agents are cited as causes of the encephalitis syndrome, only the viral ones are considered here, for they are the most common and it is to these that one usually refers when the term encephalitis is used. The nonviral forms (mycoplasmal, rickettsial, Lyme, etc.) are considered in Chap. 32, under “Encephalitis Caused by Bacterial Infections,” and should be reviewed with this section.
According to the Centers for Disease Control and Prevention, approximately 20,000 cases of acute viral encephalitis are reported annually in the United States. Death occurs in 5 to 20 percent of these patients and residual signs, such as mental deterioration, amnesic defect, personality change, recurrent seizures, and hemiparesis, are seen in approximately another 20 percent. However, these overall figures fail to reflect the widely varying incidence of mortality and residual neurologic abnormalities that follow infections by different viruses. In herpes simplex encephalitis, for example, approximately 50 percent of patients die or are left with some impairment, and in eastern equine encephalitis, the figures are even higher. On the other hand, death and serious neurologic sequelae have been observed in only 5 to 15 percent of those with western equine and West Nile infections and in even fewer patients with Venezuelan, St. Louis, and La Crosse encephalitides.
The types of viral encephalitis that occur with sufficient frequency to be of clinical importance are relatively few. HSV is by far the most common sporadic cause of encephalitis and has no seasonal or geographic predilections. Its age distribution is slightly skewed and biphasic, affecting persons mainly between ages 5 and 30 years and those older than age 50 years. Many other viruses, exemplified by the arboviral encephalitides, have a characteristic geographic and seasonal incidence. The most important of these is the Japanese encephalitis serogroup (Flaviviruses), of which the now common West Nile virus is a member. In recent outbreaks in the United States, the West Nile virus has been more frequent than any of the other arboviruses and has had a wide geographic distribution (Solomon). In the United States, eastern equine encephalitis, as the name implies, is observed mainly in the eastern states and on both the Atlantic and Gulf coasts. Western equine encephalitis is fairly uniformly distributed west of the Mississippi. St. Louis encephalitis, another arthropod-borne late-summer encephalitis, occurs nationwide but especially along the Mississippi River in the South; outbreaks occur in August through October, slightly later than is customary for the other arboviruses. Venezuelan equine encephalitis is common in South and Central America; in the United States it is practically confined to Florida and the southwestern states. California virus encephalitis predominates in the northern Midwest and northeastern states. After West Nile, the La Crosse variety is perhaps the most frequent identifiable arbovirus encephalitis in the United States.
Rabies infections occur worldwide, but in the United States they are seen mostly in the Midwest and along the West Coast. Japanese B encephalitis (the most common encephalitis outside of North America), Russian spring-summer encephalitis, Murray Valley encephalitis (Australian X disease), and several less common viral encephalitides are infrequent in the United States or, as in the case of West Nile fever, have appeared only recently. With the ease and rapidity of travel, many of these will undoubtedly increase in number in North America and parts of Europe where they have not been seen hitherto.
Infectious mononucleosis, which is a primary infection with EBV, is complicated by meningitis, encephalitis, facial palsy, or polyneuritis of the Guillain-Barré type in a small proportion of cases. Each of these neurologic complications can occur in the absence of the characteristic fever, pharyngitis, and lymphadenopathy of infectious mononucleosis. The same is true of M. pneumoniae. In these two diseases there is still uncertainty as to whether they are true infectious encephalitides or postinfectious complications, as discussed in Chap. 32. Evidence from PCR testing of spinal fluid is consistent with a direct infection in some cases. Varicella zoster and CMV are other herpes-type viruses that may cause encephalitis. They are discussed in relation to the particular clinical settings in which they occur. Definite cases of “epidemic encephalitis” (encephalitis lethargica) have not been observed in acute form since 1930, although an occasional surviving patient with a residual parkinsonian syndrome is still seen in neurology clinics. However, various movement disorders, including parkinsonism, are being seen as a residua of encephalitis from the Flaviviruses. The latency from infection to these complications is brief, or may be present from the outset, quite unlike encephalitis lethargica. There may also be a postinfectious-immune variety of this midbrain encephalitis.
More recently, a sometimes overwhelming encephalitis has been recognized as a rare manifestation of influenza infection, particularly the H1N1 strain that has infected mainly children in Southeast Asian countries, but also other serotypes of influenza including mundane influenza viruses that cause yearly outbreaks. The disorder has been called an “encephalopathy” in research publications but convulsions, delirium, and coma suggest that the neurologic aspects are from encephalitis.
The relative frequency of the various viral infections of the nervous system can be appreciated from several studies. An early series from the Walter Reed Army Institute comprising 1,282 patients is particularly noteworthy in that a positive laboratory diagnosis was achieved in more than 60 percent of cases (Buescher et al)—a higher rate than in almost any subsequent study of comparable size. Aside from the poliovirus (some of the data were gathered before 1959) the common infective agents in cases of both aseptic meningitis and encephalitis were group B Coxsackie virus, echovirus, mumps virus, lymphocytic choriomeningitis virus, arboviruses, HSV, and Leptospira, in that order. In a later prospective virologic study of all children examined at the Mayo Clinic during the years 1974 to 1976, a diagnosis of aseptic meningitis, meningoencephalitis, or encephalitis was entertained in 42 cases and an infectious agent was identified in 30 of them (Donat et al). The California virus was isolated in 19 cases and one of the enteroviruses (echovirus types 19, 16, 21, or Coxsackie virus) in 8 cases; mumps, rubeola, HSV, adenovirus 3, and M. pneumoniae were detected in individual cases (several patients had evidence of combined infections). As mentioned, recent outbreaks of West Nile virus, close to 3,000 cases yearly in the United States, make it of more current import than some of the viral infections listed here. The related Japanese encephalitis virus is even more ubiquitous on a worldwide basis, causing 10,000 deaths in Asia each year.
In a more contemporary and impressively large series of viral infections of the nervous system from the United Kingdom involving more than 2,000 patients, viral identification in the CSF was attempted by means of PCR with positive results in only 7 percent, half of which were various enteroviruses (Jeffery et al). The other organisms commonly identified were HSV-1, followed by VZV, EBV, and other herpesviruses. In patients with AIDS, however, the relative frequencies of the organisms that cause meningoencephalitis are quite different and include special clinical presentations; this applies particularly to CMV infection of the nervous system, as discussed further on, under “Opportunistic Infections and Neoplasms of the CNS in AIDS.” Our personal experience has been heavily biased toward HSV encephalitis, seasonal outbreaks of eastern equine or West Nile encephalitis, and AIDS-related cases.
The common arthropod-borne viruses (arboviruses) that cause encephalitis in the United States and their geographic range have been mentioned earlier. Most of the agents are in the category of Flaviviruses. There are alternating cycles of viral infection in mosquitoes and vertebrate hosts; the mosquito becomes infected by taking a blood meal from a viremic host (horse or bird) and injects virus into the host, including humans. The seasonal incidence of these infections is practically limited to the summer and early fall, when mosquitoes are biting. In the equine encephalitides, regional deaths in horses usually precede human epidemics. For St. Louis encephalitis, the urban bird or animal or possibly the human becomes the intermediate host. West Nile outbreaks are preceded by illness in common birds such as crows and jays. St. Louis, California, and La Crosse agents are endemic in the United States because of the cycle of infection in small rodents. Powassan virus from the deer tick has been added to the list of causes of Flavivirus encephalitis in North America as in the report by Tavakoli and coworkers.
The clinical manifestations of the arbovirus infections are almost indistinguishable from one another, although they do vary with the age of the patient. The incubation period after mosquito or tick bite transmission is 5 to 15 days. There may be a brief prodromal fever with arthralgia or rash (e.g., West Nile fever). In infants, there may be only an abrupt onset of fever and convulsions, whereas in older children and adults the onset is usually less abrupt, with complaints of headache, listlessness, nausea or vomiting, drowsiness, and fever for several days before medical attention is sought; convulsions, confusion, stupor, and varying degrees of stiff neck then become prominent. Photophobia, diffuse myalgia, and tremor (of either action or intention type) may be observed. Asymmetry of tendon reflexes, hemiparesis, extensor plantar signs, myoclonus, chorea, and sucking and grasping reflexes may also occur. McJunkin and colleagues described the clinical features of 127 patients with La Crosse infection seen at their medical center over a decade, and their descriptions are representative of other arboviral infections. In addition to the typical features of viral encephalitis they emphasize aspects that occur in a proportion of patients: hyponatremia, raised intracranial pressure with cerebral swelling, and, most notable to us, signal changes in the MRI that simulate herpes encephalitis.
A special syndrome of febrile, flaccid, paralytic poliomyelitis resulting from West Nile virus infection is now also well known. It evolves over several days and in a few cases is accompanied by facial paralysis (Jeha et al). A few cases have had an early extrapyramidal syndrome; any of these features may occur with the other Flaviviruses.
The fever and neurologic signs of arboviral encephalitis subside after 4 to 14 days unless death supervenes or destructive CNS changes have occurred. No antiviral agents are known to be effective; one must rely entirely on supportive measures. On occasion, brain swelling reaches a degree that requires specific therapy, as outlined in “Management of the Acutely Comatose Patient and Management of Raised Intracranial Pressure” in Chap. 17.
Of the arbovirus infections in the United States, eastern equine encephalitis (EEE) is among the most serious, as a large proportion of those infected develop encephalitis; approximately one-third die and a similar number, more often children, are left with disabling abnormalities—mental retardation, emotional disorders, recurrent seizures, blindness, deafness, hemiplegia, extrapyramidal motor abnormalities, and speech disorders. While only a small proportion of those exposed become infected, the poliomyelitis and parkinsonian syndromes of the Flaviviruses may be permanent residua as mentioned earlier (Solomon). On the other extreme, La Crosse encephalitis, which affects mostly children, has an almost uniformly benign outcome. The rate of progression from a nondescript febrile viral syndrome to encephalitis is similarly low in the arbovirus infections and mortality rate varies from 2 to 12 percent in different outbreaks.
The CSF findings are much the same as in aseptic meningitis (lymphocytic pleocytosis, mild protein elevation, normal glucose values). Recovery of virus from blood or CSF is usually not possible and PCR testing is routinely only applied during local epidemics. However, antiviral immunoglobulin (Ig) M antibody is present in the serum and CSF within the first days of symptomatic disease and can be detected and quantified by means of ELISA, making it preferable to other testing for specific diagnosis. Some patients have not developed antibodies by the time of admission to the hospital and the test may have to be repeated in several days. The MRI may be normal or show signal changes and edema in the cortex, basal ganglia, or thalamus (the latter is described particularly in the Japanese B virus group, West Nile, EEE, and rabies).
Perivascular cuffing by lymphocytes and other mononuclear leukocytes and plasma cells, as well as a patchy infiltration of the meninges with similar cells, are the usual histopathologic hallmarks of viral encephalitis. There is widespread degeneration of single nerve cells, with neuronophagia as well as scattered foci of inflammatory necrosis involving both the gray and white matter. The brainstem is relatively spared. In some cases of eastern equine encephalitis, the destructive lesions may be massive, involving the major part of a lobe or hemisphere and are readily displayed by MRI, but in the other arbovirus infections the foci are microscopic in size (Deresiewicz et al). West Nile virus may produce a regional pattern of neuronal damage that affects the anterior horn cells of the spinal cord, a poliomyelitis, as mentioned earlier. Pathologic descriptions of this process have been provided by our colleagues and by others (see Asnis et al).
Of the common viral encephalitides, this is perhaps the gravest and is by far the most common. About 2,000 cases occur yearly in the United States, accounting for approximately 10 percent of all cases of encephalitis. Between 30 and 70 percent are fatal, and the majority of patients who survive are left with serious neurologic abnormalities. HSV encephalitis occurs sporadically throughout the year and in patients of all ages and in all parts of the world. It is almost always caused by HSV-1, which is also the cause of the common herpetic lesions of the oral mucosa; only rarely, however, are the oral and encephalitic lesions concurrent. The type 2 herpesvirus may also cause acute generalized encephalitis, usually in the neonate and in relation to genital herpetic infection in the mother. Type 2 infection in the adult more typically causes an aseptic meningitis and sometimes a polyradiculitis or myelitis, again in association with a recent genital herpes infection. Exceptionally, the localized adult type of encephalitis is caused by the type 2 virus and the diffuse neonatal encephalitis by type 1.
The symptoms, which evolve over several days, are in most cases like those of any other acute encephalitis—namely, fever, headache, seizures, confusion, stupor, and coma. In some patients these manifestations are preceded by symptoms and findings that betray the predilection of this disease for the inferomedial or lateral portions of the frontal and temporal lobes and the insula. The symptoms and findings include olfactory or gustatory hallucinations, anosmia, temporal lobe seizures, personality change, bizarre or psychotic behavior or delirium, aphasia, and hemiparesis. Although several seizures at the onset of illness are not an uncommon presentation, status epilepticus is rare. Disturbed memory function can often be recognized, but usually this becomes evident only later in the convalescent stage as the patient awakens from stupor or coma. Hemorrhagic swelling and herniation of one or both temporal lobes through the tentorial opening may occur, leading to coma during the first few days of the illness, a very poor prognostic sign.
The CSF is typically under increased pressure and almost invariably shows a pleocytosis (range 10 to 200 cells/mm3; infrequently greater than 500 cells/mm3). The cells are mostly lymphocytes, but there may be a significant number of neutrophils early on. In a few cases, 3 to 5 percent in some large series, the spinal fluid was normal in the first days of the illness, only to become abnormal when reexamined. The hemorrhagic nature of brain tissue destruction with this infection may be reflected in the spinal fluid. In fact, in only a minority of cases, red cells, sometimes numbering in the thousands but usually far fewer, and xanthochromia are found. The protein content is increased in most cases. Rarely, the CSF glucose levels may be reduced to slightly less than 40 mg/dL, creating confusion with tuberculous and fungal meningitides. The cerebral imaging appearance, giving highly characteristic features, is discussed later in the section on “Diagnosis.”
The lesions take the form of an intense hemorrhagic necrosis of the inferior and medial temporal lobes and the mediorbital parts of the frontal lobes. The region of necrosis may extend upward along the cingulate gyri and sometimes to the insula or the lateral parts of the temporal lobes or caudally into the midbrain but always contiguous with areas of mediotemporal lobe necrosis. The temporal lobe lesions are usually bilateral but not symmetrical. This distribution of lesions is so characteristic that the diagnosis can be made by gross inspection or by their location and appearance on imaging studies. Cases described in past years as “acute necrotizing encephalitis” and “inclusion body encephalitis” were likely to have been instances of HSV encephalitis. In the acute stages, intranuclear eosinophilic inclusions are found in neurons and glia cells, in addition to the usual microscopic abnormalities of acute encephalitis and hemorrhagic necrosis. Specific intracellular staining with antibody to various portions of the virus is perhaps the most definitive demonstration of the disease.
The characteristic localization of the lesions in this disease has been putatively explained by the virus’ route of entry into the CNS. Two such routes have been suggested (Davis and Johnson). The virus may, for example, be latent in the trigeminal ganglia and, with reactivation, infect the nose and then the olfactory tract. Alternatively, with reactivation in the trigeminal ganglia, the infection may spread along nerve fibers that innervate the leptomeninges of the anterior and middle fossae. The lack of lesions in the olfactory bulbs in as many as 40 percent of fatal cases (Esiri) is a point in favor of the second pathway.
Acute herpes simplex encephalitis must be distinguished from other types of viral encephalitis, from acute hemorrhagic leukoencephalitis, and from paraneoplastic and other forms of limbic encephalitis, tumor, cerebral abscess, cerebral venous thrombosis, and septic embolism (see Chap. 32). When aphasia is the initial manifestation of the illness, it may be mistaken for a stroke. The CSF findings have been mentioned and are typical of a meningoencephalitis. Spinal fluid that contains a large number of red cells may be attributed to a ruptured saccular aneurysm. The electroencephalographic (EEG) changes, consisting of lateralized periodic high-voltage sharp waves in the temporal regions and slow-wave complexes at regular 2 to 3/s intervals, are highly suggestive in the appropriate clinical context, though they are not specific for the disease and their sensitivity has not been established with certainty.
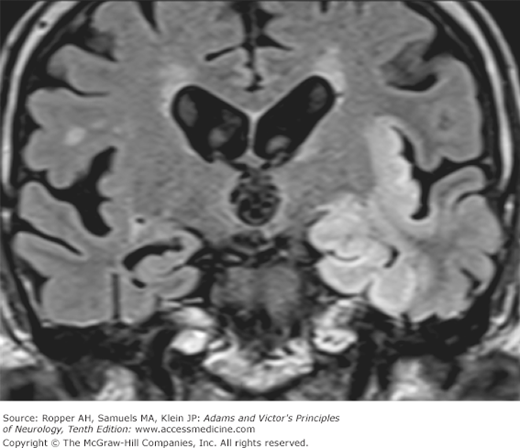
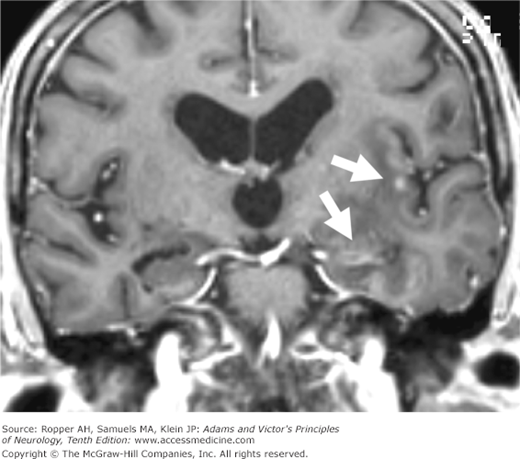
CT shows hypodensity of the affected temporal lobe areas in perhaps two-thirds of cases and MRI shows signal changes in almost all (increased signal in T2-weighted images; Fig. 33-1). T1-weighted images demonstrate areas of low signal intensity with surrounding edema and sometimes with scattered areas of hemorrhage occupying the inferior parts of the frontal and temporal lobes. The lesions almost always enhance to some degree with contrast infusion or with gadolinium, indicating cortical and pial abnormalities of the blood–brain barrier. It should be noted that these destructive lesions, and certainly their degree, are almost unique among the viral encephalitides, being seen only occasionally in other viral infections of the brain.
Figure 33-1.
Herpes simplex encephalitis. Top panel: T2-FLAIR coronal MRI, taken during the acute stage of the illness. There is increased signal in the inferior and medial temporal lobe and the insular cortex of the left hemisphere. Bottom panel: T1-weighted image after gadolinium infusion showing enhancement of the left insular and medical temporal cortices (arrows).
A rising titer of neutralizing antibodies can be demonstrated from the acute to the convalescent stage, but this is not of diagnostic help in the acutely ill patient and may not be significant in patients with recurrent herpes infections of the oral mucosa. Tests for the detection of HSV antigen in the CSF by the application of PCR have been developed and are useful in diagnosis while the virus is replicating in the first few days of the illness (Rowley et al). A refinement in this technique (a nested PCR assay described by Aurelius and coworkers) reportedly has a sensitivity of 95 percent and gives very few false-positive tests in the first 3 weeks of illness. In the experience of Lakeman and colleagues, the test was 98 percent positive in cases proven by cultures of brain biopsy material and gave 6 percent false positives. Antiviral treatment did not appear to affect the results. False-negative tests are most likely to occur in the first 48 h of febrile infection. When the clinical features are consistent with the disease and the PCR test is negative, it is advisable to repeat it in several days, perhaps in another laboratory and to obtain PCR testing for HSV-2 as well.
The only alternative way to establish the diagnosis of acute HSV encephalitis is by fluorescent antibody study and by viral culture of cerebral tissue obtained from brain biopsy. The approach to biopsy as a diagnostic test is now infrequently employed with the availability of the PCR test. We have now found it necessary to perform biopsy in only a very few cases, preferring to treat the patient with antiviral agents based on compatible clinical, radiologic, and CSF findings while awaiting serologic and PCR test results.
Until the late 1970s, there was no specific treatment for HSV encephalitis. A collaborative study sponsored by the National Institutes of Health and also a Swedish trial indicated that the antiviral agent acyclovir significantly reduces both mortality and morbidity from the disease (Whitley et al; Sköldenberg et al). For this reason, it has become general practice to initiate treatment while confirmatory testing is being carried out. Acyclovir is given intravenously in a dosage of 30 mg/kg/d and continued for 10 to 14 days in order to prevent relapse. Acyclovir carries limited risk and can be discontinued if further clinical or laboratory features point to another diagnosis. The main problems that arise from the drug are local irritation of the veins used for infusion, mild elevation of hepatic enzymes, or transient impairment of renal function. Nausea, vomiting, tremor, or an encephalopathy that is difficult to distinguish from the encephalitis itself occurs in a very few patients.
The matter of relapse after treatment with acyclovir has been recognized, particularly in children. Several potential mechanisms have been suggested by Tiége and colleagues, including an immune-mediated inflammatory response, but treatment with too low a dose or for too brief a period is undoubtedly the main cause of the rare relapses that occur in adults. In children, a second course of acyclovir is usually successful.
When a large volume of brain tissue is involved, the hemorrhagic necrosis and surrounding edema act as an enlarging mass that requires separate attention. Coma and pupillary changes should not be attributed to the mass effect unless compression of the upper brainstem is evident on brain imaging, as the infection is capable of spreading to the mesencephalon from the contiguous deep temporal lobe, thereby causing coma by a direct destructive effect. All measures used in the management of brain edema from mass lesions are applicable here, but there are insufficient data by which to judge their effectiveness. The concern that corticosteroids may aggravate the infection has not been borne out by clinical experience, but a detrimental effect cannot be discounted and their value is uncertain. Our experience (reported by Barnett et al) and that of Schwab and colleagues have been that the presence of raised intracranial pressure early in the illness presages a poor outcome. Seizures are usually brought under control by high doses of conventional antiepileptic drugs. The use of these medications prophylactically for seizures has not been resolved.
The outcome of this disease, both mortality and morbidity, is governed to a large extent by the patient’s age and state of consciousness, particularly at the time of institution of acyclovir therapy. If the patient is unconscious (except immediately after a convulsion), the outcome is usually poor. However, if treatment is begun within 4 days of onset of the illness in an awake patient, survival is greater than 90 percent (Whitley, 1990). Evaluation of patients 2 years after treatment showed 38 percent to be normal or nearly normal, whereas 53 percent were dead or severely impaired. The neurologic sequelae are often of the most serious type, consisting of a Korsakoff amnesic defect or a global dementia, seizures, and aphasia as described by Drachman and Adams in the era before treatment became available. If there were seizures during the acute illness, it is advisable to continue antiepileptic medications for a year or more and then judge the risk of discontinuing them on the basis of further seizures, the EEG, and the patient’s exposure to situations that pose a danger, such as driving. With the exception of the rare relapsing cases mentioned earlier, the infection does not recur.
This agent, the cause of roseola (exanthema subitum), has had a controversial role in a number of acute febrile neurologic illnesses, including febrile seizures in infants and young children, subsequent temporal lobe epilepsy, cranial-nerve palsies, and other conditions. However, it is fairly firmly established as the cause of a medial temporal lobe (limbic) encephalitis in adult patients following allogenic hematopoietic stem cell bone marrow transplantation, as summarized by Seeley and colleagues. All of their patients also developed a graft-versus-host reaction. The clinical and imaging features closely resemble the paraneoplastic and anti–voltage-gated potassium channel limbic encephalitis that is discussed in Chap. 31. The prognosis is far better than in herpetic encephalitis. It is mentioned here that mundane adenoviruses can also produce a severe medial temporal lobe encephalitis in bone marrow transplant cases, in one of our patients associated with gray matter damage in the spinal cord.
The other viral agents that appear as causes of encephalitis with some regularity in stem-cell and organ transplant patients include parvovirus, CMV, EBV, adenovirus, HSV, and varicella zoster virus. Quite often, these infections are but one component of multiorgan viral infection. Some of these agents also cause manifestations of infection in peripheral and cranial nerves.
This disease also stands apart from other acute viral infections by virtue of the latent period that follows inoculation with the virus and its stunningly distinctive clinical and pathologic features. Human examples of this disease are rare in the United States; between 1980 and 1997, only 34 instances were known to have occurred and since 1960, there have not been more than 5 or so cases in any 1 year. In some areas (Australia, Hawaii, Great Britain, and the Scandinavian peninsula), no indigenous cases have ever been reported. In contrast, in India there is a high incidence. The importance of this disease derives from the fact that it is almost invariably fatal once the characteristic clinical features appear, making survival of the infected individual dependent on the institution of specific therapeutic measures before the infection becomes clinically evident. Furthermore, each year 20,000 to 30,000 individuals are treated with rabies vaccine, having been bitten by animals that possibly were rabid, and although the incidence of complications with the newer rabies vaccination is much lower than before, a few serious reactions continue to be encountered (see further on and also Chap. 36).
Practically all cases of rabies are the result of transdermal viral inoculation by an animal bite. In developing countries, where rabies is relatively common, the most frequent source is the rabid dog. In Western Europe and the United States, the most common rabid species are raccoons, skunks, foxes, and bats among wild animals and dogs and cats among domestic ones. Because rabid animals commonly bite without provocation, the nature of the attack should be determined. Also, the prevalence of animal rabies virus varies widely in the United States, and local presence of the disease is useful in assessing risk. Rare cases have been caused by inhalation of the virus shed by bats; a history of spelunking suggests this mode of acquiring the infection. In a few cases the source of the infection may not be identifiable. The epidemiology and public health aspects of rabies have been reviewed by Fishbein and Robinson.
The incubation period is usually 20 to 60 days but may be as short as 14 days, especially in cases involving multiple deep bites around the face and neck. Tingling or numbness at the site of the bite, even after the wound has healed, is characteristic. This is thought to reflect an inflammatory response that is incited when the virus reaches the sensory ganglion.
The main neurologic symptoms, following a 2- to 4-day prodromal period of fever, headache, and malaise consist of apprehension, dysarthria, and psychomotor overactivity, followed by dysphagia (hence salivation and “frothing at the mouth”), spasms of throat muscles induced by attempts to swallow water or in rare cases by the mere sight of water (“hydrophobia”), dysarthria, numbness of the face, diplopia, and spasms of facial muscles. These features indicate the involvement of the tegmental medullary nuclei. Generalized seizures, confusional psychosis, and a state of agitation may follow. A less common paralytic form (“dumb” rabies of older writings, in distinction to the above described “rabid” form) as a result of spinal cord infection may accompany or replace the state of excitement. The paralytic form is most likely to follow bat bites or, in the past, the administration of rabies vaccination. Coma gradually follows the acute encephalitic symptoms and, with rare exceptions as noted below, death ensues within 4 to 10 days, or longer in the paralytic form.
The disease is distinguished by the presence of cytoplasmic eosinophilic inclusions, the Negri bodies. They are most prominent in pyramidal cells of the hippocampus and Purkinje cells but have been seen in nerve cells throughout the brain and spinal cord. In addition there is widespread perivascular cuffing and meningeal infiltration with lymphocytes and mononuclear cells and small foci of inflammatory necrosis, such as those seen in other viral infections. The inflammatory reaction is most intense in the brainstem. The focal collections of microglia in this disease are referred to as Babes nodules (named for Victor Babes, a Romanian microbiologist).
Bites and scratches from a potentially rabid animal should be thoroughly washed with soap and water and, after all soap has been removed, cleansed with benzyl ammonium chloride (Zephiran), which has been shown to inactivate the virus. Wounds that have broken the skin also require tetanus prophylaxis.
After a bite by a seemingly healthy animal, surveillance of the animal for a 10-day period is necessary. Should signs of illness appear in the animal, it should be killed and the brain sent, under refrigeration, to a government-designated laboratory for appropriate diagnostic tests. Wild animals, if captured, should be killed and the brain examined in the same way.
If the animal is found by fluorescent antibody or other tests to be rabid, or if the patient was bitten by a wild animal that escaped, postexposure prophylaxis should be given. Human rabies immune globulin (HRIG) is injected in a dose of 20 U/kg of body weight (one-half infiltrated around the wound and one-half intramuscularly). This provides passive immunization for 10 to 20 days, allowing time for active immunization. Duck embryo vaccine (DEV) was previously used for this purpose and greatly reduced the danger of serious allergic encephalomyelitis from about 1 in 1,000 cases (with the formerly used equine vaccine) to 1 in 25,000 cases; it is still used in many parts of the world. The more recently developed rabies vaccine grown on a human diploid cell line (human diploid cell vaccine [HDCV]) has reduced the doses needed to just 5 (from the 23 needed with DEV); these are given as 1-mL injections on the day of exposure and then on days 3, 7, 14, and 28 after the first dose. The HDCV vaccine has increased the rate of antibody response and reduced even further the allergic reactions by practically eliminating foreign protein. A thorough trial of the new antiviral agents in patients already symptomatic has not been undertaken. Persons at risk for rabies, such as animal handlers and laboratory workers, should receive preexposure vaccination with HDCV. A preventative DNA rabies vaccine has been genetically engineered and is being tested for use in animal handlers and others at high risk.
With modern intensive-care techniques, there have been a number of survivors of the encephalitic illness, all of whom had received postexposure immunization. In addition to mechanical respiratory support, several secondary abnormalities must be addressed, including raised intracranial pressure, excessive release of antidiuretic hormone, diabetes insipidus, and extremes of autonomic dysfunction, especially hyper- and hypotension. Willoughby and colleagues were successful in treating a 15-year-old girl who had not received vaccine by using an empirical approach of induced coma with ketamine and midazolam supplemented by ribavirin and amantadine. The goal was to support the patient while her antibody response matured. At least two other cases treated in a similar manner, reported anecdotally, did not survive.
A comment is made here concerning a dramatic syndrome of acute ataxia that occurs in the context of an infectious illness, mainly in children. The syndrome was originally described by Westphal in 1872 following smallpox and typhoid fever in adults, but Batten is credited with drawing attention to the more common ataxic illness that occurs after common childhood infections such as measles, pertussis, and scarlet fever. Currently, acute ataxia of childhood is most often associated with chickenpox (about one-quarter of 73 consecutive cases reported by Connolly et al), but it can occur during or after any of the childhood exanthems, as well as in association with infections caused by enteroviruses (mainly Coxsackie virus), EBV, Mycoplasma, CMV, Q fever, vaccinia, a number of vaccinations, rarely following HSV, and also after nondescript respiratory infections (see Weiss and Guberman). The condition, as mentioned, is far less frequent in adults, but we encounter a case every few years in adolescents and individuals in their twenties; besides a case of varicella that we observed in a 25-year-old, the most common preceding organisms in these individuals have been EBV and Mycoplasma.
This illness, which is essentially a “meningocerebellitis,” appears relatively abruptly, over a day or so, and consists of limb and gait ataxia and often, but not uniformly, dysarthria and nystagmus. Additional signs include increased limb tone, Babinski signs, or confusion. The fever of the original infection may have abated, or it may persist through the early stages of the ataxic illness. As a rule, there is a mild pleocytosis; the CSF protein is elevated or may be normal. The MRI is normal in the majority of cases but some show enhancement with gadolinium of the cerebellar cortical ribbon. Most patients make a slow recovery, but permanent residua are known to follow. Because the benign nature of the illness has precluded extensive pathologic study, there is uncertainty regarding the infectious or postinfectious nature of these ataxic illnesses. Some cases have shown an inflammatory pathology most suggestive of a postinfectious process (see Chap. 36), but the finding of fragments of VZV and Mycoplasma genomes in the spinal fluid by means of DNA amplification techniques favors a primary infectious encephalitis, at least in some instances.
Syndromes of Herpes Zoster
Herpes zoster (“shingles,” “zona”) is a common viral infection of the nervous system occurring at an overall rate of 3 to 5 cases per 1,000 persons per year, with higher rates in the elderly. Shingles is distinctly rare in childhood. It is characterized clinically by radicular pain, a vesicular cutaneous eruption, and, less often, by segmental sensory and delayed motor loss. The pathologic changes consist of an acute inflammatory reaction in isolated spinal or cranial sensory ganglia and lesser degrees of reaction in the posterior and anterior roots, the posterior gray matter of the spinal cord, and the adjacent leptomeninges.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree