Alcohol and Alcoholism: Introduction
Intemperance in the use of alcohol creates many problems in modern society, the importance of which can be judged by the emphasis it has received in contemporary writings, both literary and scientific. These problems may be divided into three categories: psychologic, medical, and sociologic. The main psychologic issue regards why a person drinks excessively, often with full knowledge that such action will result in physical injury and even death. The medical problem embraces all aspects of alcoholic addiction and habituation as well as the diseases that result from the abuse of alcohol. The sociologic problem encompasses the effects of sustained drinking on the patient’s work, family, and community. Some idea of the enormity of these problems can be gleaned from figures supplied by the secretary of Health and Human Services, which indicate that up to 40 percent of medical and surgical patients have alcohol-related problems and that these patients account for 15 percent of all healthcare costs. Several surveys have suggested a rate of alcohol dependence of 3 to 5.5 percent of adults. A minimum of 3 percent of deaths in the United States are attributable to alcohol-related causes. More striking, but not at all surprising, is the fact that alcohol intoxication is responsible for approximately 45 percent of fatal motor vehicle accidents and 22 percent of boating accidents. It requires little imagination to conceive the havoc wrought by alcohol in terms of suicide, accidents, crime, mental and physical disease, and disruption of family life. Finally, the problems engendered by excessive drinking cannot easily be separated from one another.
The cause of alcoholism as an addiction remains as obscure as it is for other forms of dependence and addiction, although environmental, cultural, and genetic factors are clearly implicated. No single personality type has been shown to predict reliably who will become addicted to alcohol. Similarly, no particular aspect of alcohol metabolism has been found to account for the development of addiction, with the possible exception of aldehyde dehydrogenase (see further on). Some persons drink excessively and become alcoholic in response to a profoundly disturbing personal or family problem, but most do not. Alcoholism may develop in response to a depressive illness, more so in women than in men, but far more often depression is a consequence of drinking. Social and cultural influences are undoubtedly important in the genesis of alcoholism as evidenced, for example, by the remarkably high incidence of alcoholism and drinking problems in the American Indian and Eskimo populations and by the disparity in the prevalence of alcoholism, within a single community, among various ethnic groups. However, no ethnic or racial group and no social or economic class are exempt.
The importance of genetic factors in alcoholism has been amply identified. Goodwin and coworkers studied adopted Danish men whose biologic parents were alcoholic and control subjects whose biologic parents were not alcoholic. All of the subjects had been adopted before the age of 5 weeks and had no knowledge of their biologic parentage. Twenty percent of the offspring of biologic alcoholic parents, but only 5 percent of the control subjects, had become alcoholics by the age of 25 to 29 years. A Swedish adoption study (Bohman) and one in the United States (Cadoret et al) corroborate these findings. Family studies disclose a three- to fourfold increased risk for alcoholism in sons and daughters of alcoholics, and twin studies show a twofold higher concordance rate for alcoholism in monozygotic than in dizygotic pairs. Details of these studies can be found in the comprehensive reviews of the genetics of alcoholism by Grove and Cadoret and by Schuckit. The search goes on for a biologic trait, or marker, that would identify those who are genetically vulnerable to the development of alcoholism, but none has proved to be sufficiently practical or sensitive to identify all such persons (Reich).
Ethyl alcohol, or ethanol, is the active ingredient in beer, wine, whiskey, gin, brandy, and other alcoholic beverages. The stronger spirits contain enanthic ethers, which provide flavor but have no important pharmacologic properties. In some preparations, impurities such as amyl alcohol (fusel oil) and acetaldehyde act like alcohol but are more toxic.
Alcohol is metabolized chiefly by oxidation, less than 10 percent being excreted chemically unchanged in the urine, perspiration, and breath. The energy liberated by the oxidation of alcohol (7 kcal/g) can be utilized as completely as that derived from the metabolism of other carbohydrates. However, calories from alcohol are empty of nutrients such as proteins and vitamins and cannot be used in the repair of damaged tissue. All ingested alcohol, except that metabolized by alcohol dehydrogenase in the stomach wall, is carried by the portal system to the liver. Here several enzyme systems independently oxidize alcohol to acetaldehyde. The most important of these, accounting for 80 to 90 percent of ethanol oxidation in vivo, are alcohol dehydrogenase (ADH) and its isoenzymes. This reaction leads to the formation of acetaldehyde and the reduction of nicotinic acid dehydrogenase (NAD) to nicotinamide adenine dinucleotide (NADH). A second pathway of lesser importance involves catalase, which is located in the peroxisomes and mitochondria; a third uses the “microsomal ethanol oxidizing system” (MEOS), located mainly in the microsomes of the endoplasmic reticulum. The details of the process by which acetaldehyde is metabolized are still not settled. Most likely it is converted by aldehyde dehydrogenase to acetate. Acetaldehyde has a number of unique biochemical effects that are not produced by alcohol alone. Persons who flush easily after ingestion of alcohol (Chinese, Japanese, and other Asians) differ from “nonflushers” with respect to the metabolism of acetaldehyde rather than to the metabolism of alcohol. The flushing reaction has been traced to a deficiency of aldehyde dehydrogenase activity (Harada et al). The low rate of alcoholism among Asians is said to be related to the flushing reaction (which is, in effect, a modified alcohol–disulfiram reaction; see further on), but this can hardly be the case, as North American Indians, a group with a high incidence of alcoholism, show the same reaction.
A scale relating various degrees of functional impairment to blood alcohol levels in nonhabituated persons was constructed many years ago by Miles. At a blood alcohol level of 30 mg/dL, a mild euphoria was detectable, and at 50 mg/dL, mild incoordination. At 100 mg/dL, ataxia was obvious; at 200 mg/dL, there was confusion and a reduced level of mental activity; at 300 mg/dL, the subjects were stuporous; and a level of 400 mg/dL—accompanied by deep anesthesia—was potentially fatal. These figures are valid provided that the alcohol content in the blood rises steadily over a 2-h period.
For all practical purposes, once the absorption of alcohol has ended and equilibrium has been established with the tissues, ethanol is oxidized at a constant rate, independent of its concentration in the blood (about 150 mg alcohol per kilogram of body weight per hour, or about 1 oz of 90-proof whiskey per hour). Actually, slightly more alcohol is metabolized per hour when the initial concentrations are very high, and repeated ingestion of alcohol may facilitate its metabolism, but these increments are of little clinical significance. In contrast, the rate of oxidation of acetaldehyde does depend on its concentration in the tissues. This fact is of importance in connection with the drug disulfiram (Antabuse), which acts by raising the tissue concentration necessary for the metabolism of a certain amount of acetaldehyde per unit of time. The patient taking both disulfiram and alcohol will accumulate an inordinate amount of acetaldehyde, resulting in nausea, vomiting, and hypotension, sometimes so pronounced in degree as to be fatal. Certain other drugs—notably the sulfonylureas, metronidazole, and furazolidone—have effects like those of disulfiram but are less potent.
Alcohol acts directly on neuronal membranes in a manner akin to that of the general anesthetics. These agents, as well as barbiturates and benzodiazepines, are lipid-soluble and are thought to dissolve in the cell membranes (in direct relation to the degree of their lipid solubility). With continued ingestion of alcohol, the neuronal membranes ostensibly “rigidify” and become resistant to the fluidizing effect of alcohol (Chin and Goldstein; Harris et al). It is unlikely, however, that these changes in the physical properties of cell membranes are in themselves sufficient to alter cell function. Probably of equal importance are the effects of alcohol on membrane receptor systems that regulate ion channels, particularly the chloride and calcium channels. One likely site that relates to the acute intoxicating effects of alcohol is a receptor for the inhibitory neurotransmitter gamma-aminobutyric acid (GABA) and its associated chloride-ion channel. Benzodiazepine antagonists appear to block the potentiation by alcohol of GABA-induced chloride flux. Like the GABA-chloride channel, the N-methyl-D-aspartate (NMDA) receptors, which transduce signals carried by glutamate (the major excitatory transmitter in the brain), are sensitive to extremely low concentrations of alcohol. There is also evidence that alcohol selectively potentiates serotonin receptor-ion currents, and the activity of this receptor has been implicated in alcohol- and drug-seeking behavior and addiction.
The effect of chronic administration of alcohol is to increase the number of neuronal calcium channels in the cell membrane. Moreover, calcium channel blockers, given during chronic administration, prevent both the increase in neuronal calcium channels and the development of tolerance to alcohol (Dolin and Little). The significance of these findings has been demonstrated by Little and colleagues, who showed that calcium channel blockers, given to chronically intoxicated animals after withdrawal, prevent withdrawal convulsions.
The molecular mechanisms involved in alcohol intoxication and tolerance are obviously more complex than the foregoing remarks would indicate (see reviews by Charness and by Samson and Harris). There is now a vast literature on this subject, much of it contradictory and a unified concept of the role of neurotransmitters and their receptors and modulators in the production of alcohol intoxication and tolerance has yet to emerge. The part played by internal cellular messengers, which have attracted much attention in the field of addiction, is also currently under investigation.
A scale of blood concentrations such as the one previously described has virtually no value in the chronic alcoholic patient, as it does not take into account the phenomenon of tolerance. It is common knowledge that a habituated person can drink more and show fewer effects than the moderate drinker or abstainer. This phenomenon accounts for the surprisingly large amounts of alcohol that the chronic drinker can consume without showing significant signs of drunkenness. Sober-appearing alcoholics may have blood alcohol levels of 400 to 500 mg/dL. This aspect of tolerance must be considered in judging the significance of a single estimation of the blood alcohol concentration as an index of functional capacity. The mechanisms that underlie tolerance and addiction are just beginning to be understood. There is little evidence that an enhanced rate of alcohol metabolism can adequately account for the degree of tolerance observed in alcoholics. An increase of neuronal adaptation to alcohol is a more likely explanation. Theoretically, the factors that are operative in this adaptation are the increasing resistance of neuronal membranes to the effects of alcohol and an increase in the number of neuronal calcium channels in the cell membrane.
Clinical Effects of Alcohol on the Nervous System
Alcohol functions as a central nervous system (CNS) depressant. Some of the early effects of alcohol, such as garrulousness, aggressiveness, excessive activity, and increased electrical excitability of the cerebral cortex—all of them suggestive of cerebral stimulation—are thought to be caused by the inhibition of certain subcortical structures (possibly the high brainstem reticular formation) that ordinarily modulate cerebrocortical activity. Similarly, the initial hyperactivity of tendon reflexes may represent a transitory escape of spinal motor neurons from higher inhibitory centers. With increasing amounts of alcohol, however, the depressant action involves the cortical as well as other brainstem and spinal neurons. All manner of motor functions—whether the simple maintenance of a standing posture, the control of speech and eye movements, or highly organized and complex motor skills—are adversely affected by alcohol. The movements involved in these acts are not only slower than normal but also more inaccurate and random in character and therefore less well adapted to the accomplishment of specific ends.
Alcohol also impairs the efficiency of mental function by interfering with the speed of perception and the ability to persist in mental processing. The learning process is slowed and rendered less effective. Facility in forming associations, whether of words or of figures, and the ability to focus, sustain attention, and concentrate are reduced. Finally, alcohol impairs the faculties of judgment and discrimination and, all in all, the ability to think and reason clearly.
A number of neurologic disorders are characteri-stically associated with alcoholism. The factor common to all of them, of course, is the abuse of alcohol, but the mechanism by which alcohol produces its effects varies widely from one group of disorders to another and in many cases, the essential problem is one of nutritional deficiency as discussed in the preceding chapter. The classification that follows is based for the most part on known mechanisms.
Alcohol intoxication—drunkenness, coma, paradoxical excitement (“pathologic intoxication”), “blackouts”
Abstinence or withdrawal syndrome—tremulousness, hallucinosis, seizures, delirium tremens
Nutritional diseases of the nervous system accompanying alcoholism (see Chap. 41)
Wernicke-Korsakoff syndrome
Polyneuropathy
Optic neuropathy (“tobacco-alcohol amblyopia”)
Pellagra
Diseases of uncertain pathogenesis associated with alcoholism
Cerebellar degeneration
Marchiafava-Bignami disease
Central pontine myelinolysis
“Alcoholic” myopathy and cardiomyopathy
Alcoholic dementia
Cerebral atrophy
Fetal alcohol syndrome
Neurologic disorders resulting from cirrhosis and portal–systemic shunts (see Chap. 40)
Hepatic stupor and coma
Chronic hepatocerebral degeneration
Traumatic brain lesions acquired during intoxication—subdural hematoma, cerebral contusion
The usual manifestations of alcohol intoxication are so commonplace that they require little elaboration. They consist of varying degrees of exhilaration and excitement, loss of restraint, irregularity of behavior, loquacity and slurred speech, incoordination of movement and gait, irritability, drowsiness, and, in advanced cases, sleepiness, stupor, and coma. There are several complicated types of alcohol intoxication, which are considered below.
As has been indicated, the symptoms of alcoholic intoxication are the result of the depressant action of alcohol on cerebral and spinal neurons. In this respect alcohol acts on nerve cells in a manner akin to the general anesthetics and can cause coma. Unlike the anesthetics, however, the margin between the dose of alcohol that produces surgical anesthesia and that which dangerously depresses respiration is a narrow one, a fact that adds an element of urgency to the diagnosis and treatment of alcoholic coma. One must also be alert to the possibility that other sedative-hypnotic drugs may have potentiated the depressant effects of alcohol. Another treacherous situation is that of traumatic brain injury that is complicated by intoxication, a circumstance that is prone to misinterpretation because of uncertainty as to the main cause of stupor or coma.
Despite what has been said earlier, on rare occasions, alcohol has an exclusively excitatory rather than a sedative effect. This reaction has been referred to in the past as pathologic, or complicated, intoxication and as acute alcoholic paranoid state. Because all forms of intoxication are pathologic, atypical intoxication or idiosyncratic alcohol intoxication are more appropriate designations. Nevertheless, the term pathologic intoxication is still widely used. The boundaries of this syndrome have never been clearly drawn. In the past, variant forms of delirium tremens and epileptic phenomena, as well as psychopathic and criminal behavior, were indiscriminately included. Now the term is generally used to designate an outburst of blind fury with assaultive and destructive behavior. Often the patient is subdued only with difficulty. The attack terminates with deep sleep, which occurs spontaneously or in response to parenteral sedation; on awakening, the patient has no memory of the episode. Lesser degrees are also known wherein the patient, after several drinks, repeatedly commits gross social indiscretions. Allegedly this reaction may follow the ingestion of a small amount of alcohol, but in some of the patients we have observed the amount has often been substantial. Unlike the usual forms of alcohol intoxication and withdrawal, the atypical form has not been produced in experimental subjects, and the diagnosis depends upon the aforementioned arbitrary criteria.
Pathologic intoxication has been ascribed to many factors, but there are no meaningful data to support any of them. However, an analogy may be drawn between pathologic intoxication and the paradoxical reaction that occasionally follows the administration of barbiturates or other sedative drugs. The few patients we have seen, mostly young men of college age or slightly older, have been docile and seemingly well adjusted when not drinking. Usually, they have avoided alcohol after a first episode of this sort, but there have been exceptions.
The main disorders to be distinguished from pathologic intoxication are temporal lobe seizures that occasionally take the form of outbursts of rage and violence and the explosive episodes that characterize the behavior of certain sociopaths. The diagnosis in these cases may be difficult and depends on eliciting the other manifestations of temporal lobe epilepsy or sociopathy. Pathologic intoxication may require the use of restraints and the parenteral administration of diazepam (5 to 10 mg) or haloperidol (2 to 5 mg), repeated once after 30 to 40 min if necessary.
In the language of the alcoholic, the term blackout refers to an interval of time, during a period of severe intoxication, for which the patient later has no memory—even though the state of consciousness, as observed by others, was not grossly altered during that interval. However, a systematic assessment of mental function during the amnesic period has usually not been made. A few observations indicate that it is short-term (retentive) memory rather than immediate or long-term memory that is impaired; this feature and the subsequent amnesia for the episode are vaguely reminiscent of the disorder known as transient global amnesia (see Chap. 21) but without the incessant repetitive questioning and competence in nonmemory mental activities that characterize the latter.
Blackouts may occur at any time in the course of alcoholism, even during the first drinking experience, and they certainly have happened in persons who never became alcoholic. The salient facts are that there is a degree of intoxication that interferes with the registration of events and the formation of memories during the period of intoxication and that the amount of alcohol consumed in moderate social drinking will rarely produce this effect.
Coma caused by alcohol intoxication represents a medical emergency. The main objective of treatment is to prevent respiratory depression and its complications as described in Chap. 17. One would like to lower the blood alcohol level as rapidly as possible. The previously favored administration of fructose or of insulin and glucose for this purpose is now known to be of little value. Analeptic drugs such as amphetamine and various mixtures of caffeine and picrotoxin are antagonistic to alcohol only insofar as they are overall nervous system excitants but they do not hasten the oxidation of alcohol and are not clinically useful. The use of hemodialysis should be considered in comatose patients with extremely high blood alcohol concentrations (>500 mg/dL), particularly if accompanied by acidosis, and in those who have concurrently ingested methanol or ethylene glycol or some other dialyzable drug.
Poisoning with alcohols other than ethyl alcohol is a rare but catastrophic occurrence. Amyl alcohol (fusel oil) and isopropyl alcohol are used as industrial solvents and in the manufacture of varnishes, lacquers, and pharmaceuticals; in addition, isopropyl alcohol is readily available as a rubbing alcohol. Intoxication may follow the ingestion of these alcohols or inhalation of their vapors. The effects of both are much like those of ethyl alcohol, but much more toxic. They also have in common the generation of acidosis, usually with an anion gap and if a sample of serums obtained soon after the ingestion, an osmolar gap that represents the molecules of the circulating alcohol.
Methyl alcohol (methanol, wood alcohol) is a component of antifreeze and many combustibles and is used in the manufacture of formaldehyde, as an industrial solvent, and as an adulterant of alcoholic beverages, the latter being the most common source of methyl alcohol intoxication. The oxidation of methyl alcohol to formaldehyde and formic acid proceeds relatively slowly; thus, signs of intoxication do not appear for several hours or may be delayed for a day or longer. Many of the toxic effects are like those of ethyl alcohol, but in addition severe methyl alcohol poisoning may produce serious degrees of acidosis (with an anion gap). The characteristic features of this intoxication, however, are damage to retinal ganglion cells—giving rise to scotomata and varying degrees of blindness, dilated unreactive pupils, and retinal edema—and bilateral degeneration of the putamens, readily visible on CT scans. Survivors may be left blind or, less often, with putamenal necrosis and dystonia or Parkinson disease (McLean et al). The most important aspect of treatment is the intravenous administration of large amounts of sodium bicarbonate to reverse acidosis. Hemodialysis and 4-methylpyrazole (see later) may be useful adjuncts because of the slow rate of oxidation of methanol.
Ethylene glycol, an aliphatic alcohol, is a commonly used industrial solvent and the major constituent of antifreeze. In the latter form, it is sometimes consumed by skid-row alcoholics (5,000 cases of poisoning annually in the United States) and in suicide attempts with disastrous results. At first the patient merely appears drunk, but after a period of 4 to 12 h, hyperventilation and severe metabolic acidosis develop, followed by confusion, convulsions, coma, and renal failure and death in rapid succession. Cerebrospinal fluid lymphocytosis is a common but not invariable feature. The metabolic acidosis is a result of the conversion of ethylene glycol by alcohol dehydrogenase into glycolic acid, thus producing an anion gap that reflects the presence of this additional substance in the blood. (The anion gap has been defined in different ways, but the most convenient is the difference between the positive ion Na+ and the sum of negative ions, Cl– plus HCO3– [venous CO2 is used for the latter]; a value greater than 12 is considered a gap.) The cause of the renal toxicity is less clear—probably it is a result of the formation of oxalate from glycolate and the deposition of oxalate crystals in renal tubules. (One of our recent patients had hippurate crystals in the urine, a finding that is more characteristic of toluene ingestions.) These crystals appear in the urine and sometimes in the cerebrospinal fluid (CSF) and aid in diagnosis.
The treatment of ethylene glycol poisoning has, until relatively recently, consisted of hemodialysis and the intravenous infusion of sodium bicarbonate and ethanol, the latter serving as a competitive substrate for alcohol dehydrogenase. However, the use of ethanol in this regimen is problematic. Baud and colleagues, and more recently Brent and colleagues and Jacobsen, have advocated the use of intravenous 4-methylpyrazole (fomepizole), which is a far more effective inhibitor of alcohol dehydrogenase than is alcohol. They recommend this form of treatment for methanol poisoning as well. Information from the American Academy of Toxicology is cited in a review of the use of fomepizole by Brent, which is recommended to the interested reader. Generally, for either methanol of ethylene glycol, a plasma level of the alcohol above 20 mg/dL, or above 10 mg/dL when combined with an osmolal gap over 10 is considered appropriate to institute the drug. In the case of ethylene glycol, oxaluria and acidosis are additional factors that may precipitate treatment. Dialysis remains an essential therapy if cerebral and renal damage is not too advanced.
Some patients who recover from the acute renal and metabolic effects are left with multiple cranial nerve defects, particularly of the seventh and eighth nerves. The latter abnormalities develop 6 to 18 days after the ingestion of ethylene glycol and have been attributed to the deposition of oxalate crystals along the subarachnoid portions of the affected nerves (Spillane et al).
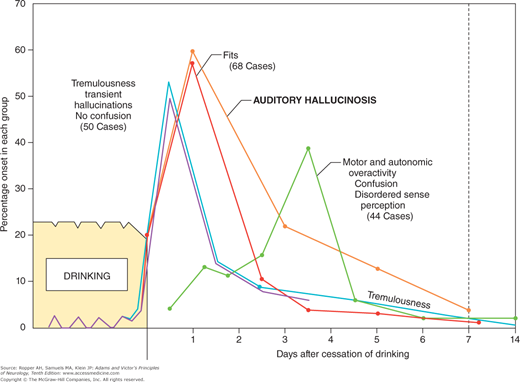
This is the well-known symptom complex of tremulousness, hallucinations, seizures, confusion, and psychomotor and autonomic overactivity. Although a sustained period of chronic inebriation is the most obvious factor in the causation of these symptoms, they become manifest only after a period of relative or absolute abstinence from alcohol—hence the designation abstinence, or withdrawal, syndrome. Figure 42-1 illustrates this concept. Each of the major manifestations of the withdrawal syndrome may occur in more or less pure form and are so described below, but usually they occur in combination. Major withdrawal symptoms are observed mainly in the binge, or periodic, drinker, although the steady drinker is not immune if for some reason he stops drinking, such as during a hospital admission for surgery or a medical illness. The full syndrome, depicted further on, is called delirium tremens.
Figure 42-1.
Relation of acute neurologic disturbances to cessation of drinking. The shaded drinking period is greatly foreshortened and not intended to be quantitative. The periodic notching in the baseline represents the tremulousness, nausea, and so on that occur following a night’s sleep. The time relations of the various groups of symptoms to withdrawal are explained in the text. (Adapted from Victor M, Adams RD: The effect of alcohol on the nervous system. Res Publ Assoc Res Nerv Ment Dis 32:526, 1953, by permission.)
The most common single manifestation of the abstinence syndrome is tremulousness, often referred to as “the shakes” or “the jitters,” combined with general irritability and gastrointestinal symptoms, particularly nausea and vomiting. These symptoms first appear after several days of drinking, usually in the morning after a night’s abstinence. The patient “quiets his nerves” with a few drinks and is then able to drink for the rest of the day without undue distress. The symptoms return on successive mornings with increasing severity. The symptoms then become augmented, reaching their peak intensity 24 to 36 h after the complete cessation of drinking. Generalized tremor
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree