No history of self-harm.
Index offense: extremely violent murder.
PCL-SV: Psychopathy Checklist-Screening Version [38]. A score of 16/24 or greater indicates psychopathy; HSH: High-security hospital.
Symptom improvement
Of the seven patients, one had a CGI score that displayed “vast improvement” (reduced CGI by 4 points), one showed “major improvement” (reduced CGI by 3 points), and all other patients (N = 5) displayed “significant improvement” (reduced CGI by 2 points). The severity of illness decreased significantly for all patients (see Table 18.2).
| Patient | Duration of clozapine treatment (weeks) | Clozapine dose (mg/day) | Concurrent medication (mg/day) | Clozapine/norclozapine level (ng/mL) | CGI | AD | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Pre | Post | CP | IB | Low mood | Anxiety | Anger | Lability | |||||
| A | 12 | 325 | Quetiapine (200 mg tapering dose) | 350/140 | 6 | 4 | ↑ | ↑↑ | ↔ | ↑ | ↑↑ | ↑ |
| B | 14 | 200 | Mirtazapine (30 mg) | 270/210 | 5 | 3 | ↔ | ↑↑ | ↔ | ↔ | ↑ | ↔ |
| C | 12 | 175 | Chlorpromazine (400 mg) Duloxetine (30 mg) Sodium-valproate (1600 mg) | 160/70 | 5 | 3 | ↑↑ | ↑↑ | ↑↑ | ↑↑ | ↑↑ | ↑ |
| D | 38 | 150 | Chlorpromazine (125 mg) Methadone (30 mg) Tropimarate (200 mg) Trihexyphenidyl (6 mg) | 230/110 | 5 | 3 | ↑ | ↑ | ↑↑ | ↑ | ↑ | ↑↑ |
| E | 65 | 100 | Fluoxetine (40 mg) | 150/60 | 7 | 3 | ↑↑ | ↑↑ | ↑↑ | ↑↑ | ↑↑ | ↑↑ |
| F | 7 | 100 | Amisulpride (600 mg) Diazepam (15 mg) Trihexyphenidyl (20 mg) | N/A | 5 | 3 | ↑ | ↑↑ | ↔ | ↔ | ↑ | ↑ |
| Venlafaxine (300 mg) | ||||||||||||
| G | 67 | 150 | Sertaline (50 mg) Sodium valproate (1200 mg) Pregabalin (300 mg) | 170/80 | 6 | 3 | ↑↑ | ↑↑ | ↑↑ | ↑↑ | ↑ | ↑ |
mg: milligrams; ng/ml: nanograms per milliliter; Pre: before clozapine initiation; Post: after clozapine initiation; CGI: Clinical Global Impression Scale.39 1 = normal, not at all ill, 2 = borderline mentally ill, 3 = mildly ill, 4 = moderately ill, 5 = markedly ill, 6 = severely ill, 7 = among the most extremely ill, 0 = not assessed.
Symptom domains: CP: cognitive perceptual symptoms; IB: impulsive-behavioral dyscontrol; AD: affective dysregulation; ↓ worse; ↔ no change; ↑ some improvement; ↑↑ much improved.
With regard to improvement in specific symptom domains, six of the seven patients showed improvement in the cognitive-perceptual domain. All of the patients showed improvement in impulsive-behavioral dyscontrol. All patients showed improvement in some aspect of affective dysregulation; specifically, four showed improved symptoms of low mood, five in anxiety, all demonstrated improved anger control, and six of the seven improved mood lability.
Clozapine and nor-clozapine serum levels, concurrent medication
Data were available for clozapine and nor-clozapine levels for six of the seven patients. Levels were not available for one patient (Patient F), as he was on clozapine for 7 weeks only, and subsequently it was discontinued. Serum clozapine level results were as follows: 150, 160, 170, 230, 270, and 350 ng/ml. Concurrent psychotropic medication was recorded (see Table 18.2). None of the patients was started on any antipsychotic or other psychotropic medication concurrently after the initiation of clozapine.
PCL-SV and PCL-R scores
All patients scored highly on psychopathy as assessed by the PCL-SV (all scored 19 or above out of 24; mean: 19.6; range: 19–21). One patient had an additional PCL-R assessment and scored 28 out of 40. These tests were administered by a trained psychologist or doctor.
Improvement in aggression and violence
All patients’ risk of violence and aggression to others reduced following treatment with clozapine, as quantified by formal risk assessment changes and staff opinions recorded in the weekly records. In all cases, this risk reduction was associated with clinical improvement in symptoms and positive engagement with OT and psychological therapies. In three of the seven patients, their risk reduced sufficiently to merit a move to a lower dependency ward or transfer to a medium-security unit. None of the patients had to be moved to a higher dependency ward following commencement on clozapine.
Incidents of violence logged in the hospital’s incident reporting system were assessed in the 90 days before clozapine was initiated and in the most recent 90 days on clozapine at the time of the writing of this report. It will be pertinent to mention here that in cases where clozapine was started less than 90 days after admission to the hospital, potential incidents may have been missed, as we did not have access to other hospitals’ or prison service records. Post-clozapine initiation, no incidents were missed for any patient, as all hospital records were available. Incidents were divided into the following subgroups: verbal aggression, aggression toward property, aggression toward others (physical), and self-harm.
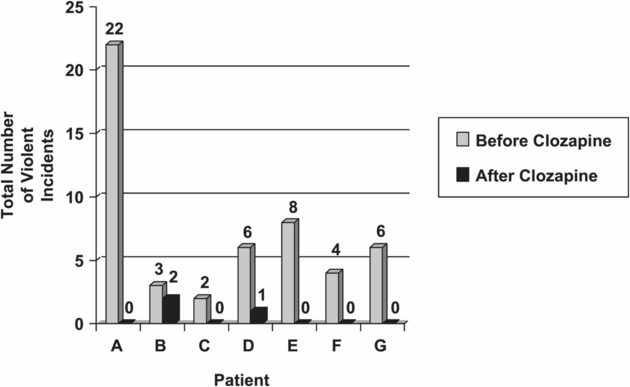
Six of the seven patients showed a reduction in their number of total violent incidents, with four of the six demonstrating a 100% reduction (see Table 18.3 and Figure 18.1). The remaining patient (Patient C: see Case Reports) did not have any recorded incidents before or after clozapine was initiated, but reported a diminished preoccupation with violent fantasies.
| Total number of violent incidents | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Verbal aggression | Aggression against property | Aggression against others | Self-harm | ||||||||
| Patient | Pre | Post | Pre | Post | Pre | Post | Pre | Post | % Reduction in total number of incidents | Risk of violence to others* | Dependency level |
| A | 22 | 0 | – | – | – | – | – | – | 100% | ↓ | ↔ |
| B | 2 | 2 | 1 | 0 | – | – | – | – | 33.3% | ↓ | ↓ |
| C | – | – | – | – | – | – | – | – | – | ↓ | ↔ |
| D | 6 | 1 | – | – | – | – | – | – | 83.3% | ↓ | ↔ |
| E | 6 | 0 | – | – | 1 | 0 | 2 | 0 | 100% | ↓ | ↓ |
| F | 1 | 0 | 3 | 0 | – | – | – | – | 100% | ↓ | ↔ |
| G | 5 | 0 | 1 | 0 | – | – | – | – | 100% | ↓ | ↓ |
Metabolic parameters (see Table 18.4) and side effects
Four patients’ body mass index (BMI) increased and 3 decreased over the treatment time period. The mean BMI was 30.2 before clozapine was initiated; this increased to 31.6 after treatment. The result was positively skewed by Patient G’s significant BMI increase from 31.8 to 37.4. There was a minor increase in fasting blood sugar results (mean 5.0 pre-clozapine and 5.2 post-clozapine). Finally, there was a slight increase in total cholesterol:HDL ratios (mean 5.5:1 pre-clozapine, 5.9:1 post-clozapine).
| Pre-clozapine | Post-clozapine | ||||||
|---|---|---|---|---|---|---|---|
| Patient | BMI | Fasting blood glucose | Total cholesterol:HDL ratio | BMI | Fasting blood glucose | Total cholesterol:HDL ratio | Side effects |
| A | 33.9 | n/a | 3.4:1 | 32.0 | 5.4 | 3.1:1 | Drowsy, tachycardia |
| B | 29.1 | 5.0 | 8.6:1 | 32.2 | 5.7 | 11.9:1 | Hypersalivation, drowsy, slurred speech |
| C | 28.4 | 5.0 | 4.6:1 | 31.8 | 5.0 | n/a | Drowsy, slurred speech, hypersalivation |
| D | 27.1 | 5.7 | 9.6:1 | 24.4 | 5.6 | 4.6:1 | Drowsy |
| E | 27.5 | 4.8 | 4.0:1 | 31.5 | 5.6 | 5.2:1 | Drowsy |
| F | 33.7 | 4.8 | 2.9:1 | 31.7 | 4.1 | 5.3:1 | Various: non-specific, drowsy |
| G | 31.8 | 4.9 | n/a | 37.4 | 4.8 | 5.5:1 | Drowsy, slurred speech, weight gain |
BMI: Body Mass Index, HDL: high density lipid, n/a: information not available.
All patients reported a similar profile of side effects. These included drowsiness, hypersalivation, and slurred speech. One patient (Patient F) discontinued clozapine, despite “feeling better,” due to various side effects and his subsequent noncompliance. None of the patients presented with neutropenia or agranulocytosis after initiation of clozapine.
Patient case reports
Patient A has a history of conduct disorder as a child, and presented in his adolescence with violent thoughts, animal abuse, and incidents of interpersonal violence. His index offence involved a serious assault on one of his parents with a knife, and he was convicted of attempted murder. He came to the hospital with symptoms of self-harm, emotional lability, and numerous acts of violence against fellow patients and staff. He has remained an inpatient for the last 7 years. Since 2011, he has had over 88 incidents of verbal aggression and has physically assaulted or attempted to assault fellow patients and staff on 16 accounts. Two years ago, he responded to clozapine for 8 months, but this was stopped due to poor compliance. Since being re-challenged on clozapine, his incidents of aggression have completely ceased, his seclusion hours have more than halved, he is less irritable, and he engages better with staff and fellow patients.
Patient B has a significant history of violence dating back to his early childhood and has over 60 convictions, including assault, arson, criminal damage, sexual assault, attempted murder, and witness intimidation. His index offence was the murder of a fellow prisoner by strangulation and attempted decapitation. He has had several incidents since moving from prison to hospital services, including barricading a door and making serious threats of violence toward staff. Since starting clozapine, he has appeared calmer, violent incidents have reduced, there has been no self-harm, and he has engaged better with staff and other patients. In light of clinical improvement, there are now plans to move him back to prison and prepare him for release on license after he has finished serving his sentence.
Patient C has multiple convictions for assault, actual bodily harm, and the possession of weapons. His index offence was an extremely violent homicide where the victim was hit over the head 30–40 times with a metal bar. He frequently has violent fantasies about killing others and stabbing people with knives. Despite these intense feelings, he has managed to control his impulses while in the hospital and has had no recent incidents of outward aggression toward staff or patients. After the addition of clozapine to his treatment regime, which already included chlorpromazine, Patient C reported feeling better “mentally.” Since starting clozapine, his internal aggression and tendency for violence has improved, and he has engaged well with dialectical behavioral therapy and occupational therapies.
Patient D has an index offence of robbery and wounding with intent to cause grievous bodily harm. He has a significant history of assault, robbery, animal cruelty, and substance misuse, and he poses a significant risk of violence to others. Before starting clozapine, the patient was stable but could be verbally abusive toward staff at times. He also refused to engage in any OT or psychological therapies. After commencing treatment on clozapine, his episodes of aggression have reduced, he is now engaging better with staff, and he has been removed from the high-risk register.
Patient E has multiple convictions of rape and sexual violence, and he has displayed significant interpersonal violence toward others while in prison and hospital care. He also has a high risk of self-harm and made serious attempts to self-mutilate while in prison. Before starting clozapine, Patient E could be aggressive and had to be reminded about inappropriate behavior toward female staff. After clozapine was started, it was noted by staff that he appeared calmer. At this point, he also began to engage more frequently in OT and psychological treatment with great success. He has displayed few incidences of violence, engages well, and has been moved to a rehabilitation ward. There is a plan to move him to a medium-security unit.
Patient F has numerous violent convictions, including assault, actual bodily harm, and the possession of weapons. While in the hospital, this violence has continued, and he is at high risk of aggression, assault, and fashioning weapons from sharp objects. During his short trial of clozapine, it was noted by staff that he showed improvement and was more settled. The patient stated that he “felt better,” and he continued to engage well with psychological therapies. There were plans for him to be moved to a lower dependency rehabilitation ward. However, clozapine was stopped after only seven weeks due to side effects, including drowsiness, which led to patient noncompliance. In the weeks following discontinuation of clozapine, Patient F did not show any signs of immediate relapse. However, several months later, he had to be moved to a higher dependency ward, as he had begun to destabilize. While writing this report, it was noted that patient F has been restarted on clozapine in the hope he will show a similar response as in his previous trial.
Patient G has various convictions beginning at adolescence. His index offence was robbery with assault, which resulted in grievous bodily harm, and assaults on prison staff on numerous occasions causing serious injuries. Upon admission to the hospital, he had a history of self-harm, failure to comply with medication, and violence toward staff. His aggression toward others seemed to settle after only a few weeks on clozapine, and there was a significant reduction in the frequency of incidents reported. At this time, he has begun engaging well with activities off-ward and was moved to a lower security, rehabilitation ward. He has recently been recommended for transfer to a medium-security unit.
Discussion
We report a case series of seven forensic patients with ASPD and significant histories of violence toward others who were being treated with clozapine in a high-security hospital. Among the robust socio-demographic and clinical predictors for dangerousness in people suffering with mental illnesses, previous history of violence and/or incarceration, aggression at the time of referral, and aggression at the time of hospitalization have been identified [46]. These factors are present in our patients, and hence initiation of clozapine was clinically justified, keeping in perspective the additional facts that clozapine has been shown to be of benefit in certain subtypes of personality disorders [23,27], coupled with reducing aggression in schizophrenia [46].
All of the patients also scored high on psychopathy as determined by PCL-SV and additionally by PCL-R (in one patient). All seven of the patients showed clinical improvement in symptoms with the commencement of clozapine treatment and also a reduction in their risk of violence to others. Specifically, six of the seven patients showed improvement in cognitive-perceptual symptoms, all showed improvement in impulsive-behavioral dyscontrol, four in low mood, five in anxiety, seven in anger, and six in mood lability domains. Overall, clozapine treatment showed exceptional improvement in treating all symptom domains, with maximum benefit in the improvement of the severity of impulsive-behavioral dyscontrol and reducing anger.
Two of the patients who had a presentation of self-harming behavior showed a reduction in this risk. Six of the seven patients displayed a reduction in the total number of violent incidents, with four of the six showing a 100% reduction. The dose of clozapine prescribed was below the therapeutic dose for schizophrenia (350 ng/ml) [47] for five of the six patients whose levels were sampled. All patients showed an improvement in engagement with occupational, vocational, and/or psychological work. Metabolic parameters (where available) were largely unchanged, except for one patient who had a significant increase in BMI from 31.8 to 37.4. Considering this effect, clozapine may have caused minor weight gain in our patient sample. In some cases, there was unexpected improvement in metabolic parameters, which may be due to increased engagement in physical activities such as sports and leisure facilities. Side effects reported by the patients included drowsiness, hypersalivation, and slurred speech, which are all commonly reported side effects. It is relevant to mention here that patients were notified of the potential for these side effects before commencing clozapine. In one patient, various side effects led to the discontinuation of clozapine treatment after only seven weeks. To our knowledge, this is the first report to demonstrate that clozapine treatment may have a beneficial effect on ASPD patients with high psychopathy, especially in reducing the risk of violence to others.
Pharmacodynamic rationale for treatment with clozapine
Clozapine has an extensive range of actions, and has a potent affinity for D1, D2, D4, 5-HT2A, 5-HT2C, 5-HT3, muscarinic, α-adrenergic, and histamine H1 receptors; inverse agonist activity at histamine H2 receptors [48]. The full range of actions induced by clozapine is not yet fully understood [18,19,21,49]. The virtue by which clozapine is particularly efficacious in treatment-resistant schizophrenia, and in reducing violence, may be because of this diverse receptor profile.
Animal studies suggest that dopamine has considerable influence in mediating emotion, stress response, aggression, and impulsivity [50–52]. Additionally several studies have demonstrated the association between abnormal dopamine metabolite (HVA) levels and impulsivity [53,54]. These effects are particularly relevant to borderline and antisocial personality disorders, which are characterized by emotional dysregulation and impulsivity [45]. Dopamine dysfunction has been postulated as an underlying pathology in BPD, and this is supported by evidence that personality disorder symptoms can be treated by neuromodulators that improve dopamine dysfunction, such as the atypical antipsychotic clozapine [55].
Additionally, it has been shown that serotonin (5HT) has a key role in the modulation of aggressive behavior [54–62], and several studies have identified an association between serotonin metabolite (5-HIAA) in human cerebrospinal fluid and antisocial behavior such as violence, homicide, arson, and child abuse [57,58,63]. The extent to which serotoninergic dysfunction influences aggression is dependent on a complex interplay between multiple environmental factors [64].
Through its complex action on both the dopaminergic and serotinergic systems, clozapine induces anti-aggressive properties [28,65], which can be of benefit in the treatment of personality disorders. However, further research is needed to evaluate the pharmacodynamic basis for clozapine’s efficacy in this patient group.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree