Complications in the Treatment of Subaxial Cervical Fractures and Dislocations
Rolando Figueroa Roberto
Eric O. Klineberg
Subaxial cervical spine fractures and dislocations are common injuries. Many opportunities may arise for undesirable or unanticipated results during both nonoperative and operative treatment. An understanding of treatment principles, as well as prior reports of complications, should allow the treating surgeon to avoid most adverse events and to respond appropriately when they do occur.
NONOPERATIVE MANAGEMENT
While most fractures and ligamentous injuries can be immediately divided into stable or unstable injury patterns, failure to correctly diagnose and treat unstable ligamentous and osteoligamentous injuries still may occur. The incidence of an incorrect diagnoses or delay in diagnoses has been reported from 5 to 20% of all cervical spine injuries (1, 2 and 3). In one series, a delay in diagnosis occurred with an interval between injury and diagnosis that ranged from 1 to 30 days (3). In cases of missed diagnoses, neurologic complications may occur including isolated nerve root dysfunction, spinal cord compromise, quadriplegia, and death. A review of a malpractice database reported 20 missed cervical spine injuries with progression to quadriplegia and/or death resulting in plaintiff verdicts averaging $2.9 million per case (4). Given the human and economic costs of missed injuries, all appropriate diagnostic modalities should be utilized if any uncertainty remains in the evaluation of a patient with a sufficient mechanism (the obtunded or chemically paralyzed patient). Computed tomography (CT), magnetic resonance imaging (MRI), and static and dynamic radiography may all play a role in characterizing injuries into stable and unstable types to prevent potentially devastating consequences (5,6).
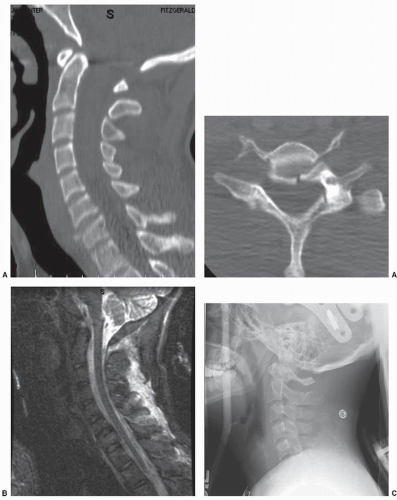
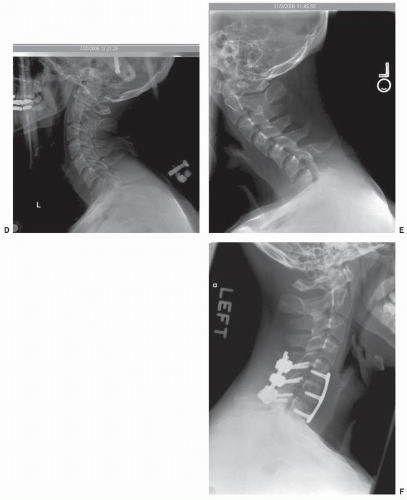
Even with the appropriate injury diagnosis, fracture displacement and progressive deformity has been reported with experienced providers utilizing nonoperative orthotic devices for well-defined injury patterns. For example, Fisher et al. (7) reported on five failures occurring in a series of 24 patients with flexion teardrop injuries treated in halo-thoracic vests. This is a retrospective, nonrandomized series that compared the differences between operative and nonoperative management of flexion teardrop fractures. In this series, halo vest treatment was abandoned in five patients, two patients for acute neurologic deterioration after mobilization, and in an additional three patients due to loss of fracture reduction without neurologic sequelae. Radiographic analysis also favored surgical treatment with improved maintenance of cervical alignment. After 3 months of treatment, the average kyphosis across the injured segment was 11.4 degrees for the orthosis group compared to 3.5 degrees in the operative group treated with corpectomy and plating. If nonoperative management is selected, close radiographic and clinical follow-up is required. Fracture displacement may occur, despite the correct osseous diagnosis, in cases with underestimated ligamentous instability. In addition, early outpatient radiographic surveillance 7 to 14 days after hospital discharge should be obtained to verify maintenance of satisfactory spinal alignment (Fig. 106.1A-F and 106.1). Surgical management should be undertaken if instability is recognized.
NEUROLOGIC COMPLICATIONS
Closed reduction of cervical dislocation and fracture subluxation is generally accomplished with low complication rates at centers following established treatment protocols. However, consensus statements and protocols regarding timing or method of reduction (open or closed) are lacking (8). Several institutions have reported their preferred methods of achieving reduction as well as associated complications experienced with the reduction techniques (9, 10 and 11).
Lee et al. (9) published their experience in the reduction of 210 patients with unilateral and bilateral facet dislocations using manipulative reduction or a rapid traction protocol. In their series, rapid traction with weights (without cervical manipulation) resulted in successful reduction more reliably with a lower overall complication rate when compared to techniques using manual manipulative reduction. In 91 patients treated with manipulative reduction (three-person traction maneuver), six patients were noted to have lower American Spinal Injury Association (ASIA) motor scores after reduction than prior to reduction. In contrast, only 1 of 119 patients reduced using the rapid traction protocol (without manipulation) sustained a minor neurologic decline reflected in a lower overall ASIA motor score.
Grant et al. (10) reported their experience with a rapid traction protocol and its success in achieving reduction of cervical fracture dislocations. Eighty of eighty-two patients were successfully reduced with Gardner-Wells tongs with application of traction weights at 5-minute intervals to an ultimate weight of 80% body weight. Patients were monitored clinically with repeated neurologic exams in these awake, cooperative individuals. Only 1 of 76 patients declined 6 points in ASIA motor score after successful reduction. Interestingly, 22% of patients had some degree of disk herniation, at the level of injury, on postreduction MRI performed within 24 hours of reduction.
Mahale (11) reported a retrospective series of 16 patients referred to their center for rehabilitation who had sustained neurologic injuries after open or closed reduction for cervical dislocation. Twelve patients were initially Frankel grade D or E, with three patients Frankel grade B or C. After reduction, 12 patients declined to Frankel A or B status. New neurologic deficits were diagnosed within 12 hours of surgical treatment in seven patients, and nine patients developed deficits within 12 to 48 hours after reduction. Recovery to Frankel grade D or E status occurred in 14 of 16 patients with one patient remaining Frankel C and one patient with complete paraplegia and eventual death. The delayed neurologic deteriorations were presumed to occur because of increased spinal cord edema. In one patient, vertebral artery injury was documented as a possible cause of further cord infarction. While the reduction of a cervical dislocation carries significant neurologic risks and all efforts to reduce the risks of reduction should be employed, a zero percent risk of neurologic complication may be impossible to achieve. Nonetheless, a stable spine is critical for the prevention of late neurologic injury, and unreduced facet dislocations have been associated with late pain and instability (12).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree