FIGURE 7.1 Motor areas of the frontal lobe in monkeys (A) and homologous areas in the human (B). In humans, the border between areas 6 and 4 on the lateral surface is located in the anterior bank of the central sulcus (FEF, frontal eye field; M1, primary motor cortex; PMd, dorsal premotor cortex; PMv, ventral premotor cortex; RCZa, anterior rostral cingulate zone; RCZp, posterior rostral cingulate zone; SMA, supplementary motor area). (Reprinted from Picard N, Strick PL. Imaging the premotor areas. Curr Opin Neurobiol 2001;11:663–672, with permission.)
The Prefrontal Area
The portions of the frontal lobe anterior to area 6, area 8, and the motor speech centers are areas referred to as the prefrontal cortex. It includes areas 9 to 12, 32, 45, 47, and others. These areas are connected with the somesthetic, visual, auditory, and other cortical areas by long association bundles and with the thalamus and the hypothalamus by projection fibers. The prefrontal cortex is the main projection site for the dorsomedial nucleus of the thalamus. The prefrontal cortex projects to the basal ganglia and substantia nigra; it receives dopaminergic fibers that are part of the mesocortical projection from the midbrain. The dopaminergic neurons are associated with reward, attention, short-term memory tasks, planning, and drive.
Clinically, the prefrontal region can be divided into the dorsolateral prefrontal cortex (DLPFC), the medial prefrontal cortex (MPC), and the orbitofrontal cortex (OFC). The cellular structure of the prefrontal region is strikingly different from areas 4 and 6 (the motor and premotor areas). The cortex is thin and granular; the pyramidal cells in layer 5 are reduced in both size and number. These brain areas are highly developed in humans, and they have long been considered the seat of higher intellectual functions. Much of the information about the functions of the frontal association areas has come from clinical observation of patients with degeneration, injuries, or tumors of the frontal lobes, and from examination of patients who have had these regions surgically destroyed. Beginning with Phineas Gage, many examples of patients with dramatic changes in personality or behavior after frontal lobe damage have been reported (Figure 7.2; Box 7.1). Mataro et al. reported a modern case similar to Phineas Gage with a 60-year follow-up.
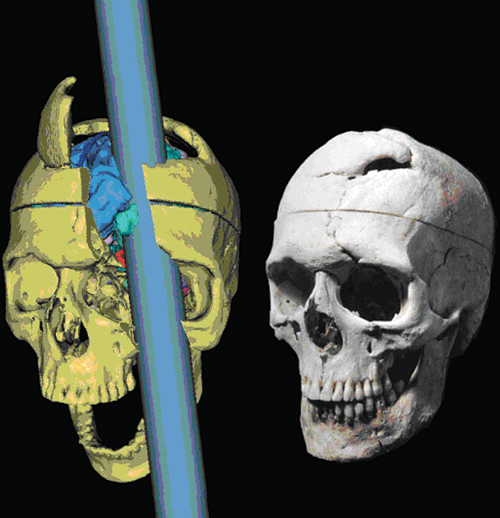
FIGURE 7.2 Phineas Gage, a three-dimensional computer reconstruction of the original skull from a thin-slice computed tomographic image and of the tamping iron. (From Ratiu P, Talos IF. Images in clinical medicine. The tale of Phineas Gage, digitally remastered. N Engl J Med 2004;351:e21, with permission.)
Frontal Lobotomy
In a famous incident in 1848, Mr. Phineas Gage, a 25-year-old railroad worker, sustained severe damage to his frontal lobes when a metal tamping rod was blasted through his head after a freak accident (the “case of the crowbar skull”). The rod entered through the left cheek and exited in the midline near the intersection of the sagittal and coronal sutures. Surprisingly, he survived and has become a celebrated patient in the annals of medicine. Following the accident, there was a dramatic change in his character and personality. He died 13 years later after having traveled extensively and having been, for a period of time, exhibited in a circus. He reportedly became irreverent, profane, impatient, and unable to hold a job. He was “a child in his intellectual capacities, with the general passions of a strong man.” Reports of the case strengthened prevailing ideas about cerebral localization, particularly about the importance of the frontal lobes in personality. Gage’s accidental frontal lobotomy laid some of the groundwork for the surgical procedure of frontal (prefrontal) lobotomy or leukotomy, which was thought to decrease emotional and affective responses and relieve anxiety, apprehension, and “nervous tension.” The operation consisted of cutting the white matter coronally in each frontal lobe, dividing the association fibers that connect the prefrontal areas with other brain regions. This operation became popular in the mid-20th century; it was done extensively over a period of years as a treatment not only for psychosis but also for neurosis and depression. It was even used to control the behavior of criminals and recommended for “difficult” children. A popular procedure was the “ice-pick” lobotomy in which an ice pick was inserted above the eye and pounded through the orbital roof with a mallet, then swept to and fro to sever the connections of the prefrontal region from the rest of the brain. The primary proponent of this technique used a gold-plated ice pick and kept speed records for the procedure. A lobotomy was once done on an eccentric actress who had no mental illness. The abuse of frontal lobotomy was dramatized in the motion picture One Flew Over the Cuckoo’s Nest. The procedure has been abandoned.
There is a paucity of information regarding the functions of the different regions of the prefrontal cortex. The DLPFC is important in the organization of self-ordered tasks. It plays a critical role in the neural network subserving working memory (see Chapter 8). The responsibility for executive function largely resides with the DLPFC and its connections. Frontal lobe executive function is the ability to plan, carry out, and monitor a series of actions intended to accomplish a goal. It is concerned with planning and organizational skills, the ability to benefit from experience, abstraction, motivation, cognitive flexibility, and problem solving. Disturbed executive function is common with frontal lobe lesions. Defects in executive function occur with frontal lobe lesions, but may occur with lesions elsewhere because of the extensive connections of the frontal lobes with all other parts of the brain. The DLPFC is also important in oculomotor control, which is responsible for decision making regarding voluntary eye movements and inhibiting unwanted reflex saccades. It may also play a role in pain perception. There is evidence of DLPFC dysfunction in schizophrenia. The prefrontal region likely plays a role as well in the ability to predict the consequences of actions, emotional expression (affect), “go/no-go” decision making, personality, and the sense of time. Widespread changes in prefrontal activation are associated with calculating and thinking.
The MPC has connections with the several thalamic nuclei, particularly the dorsomedian, and with the superior temporal cortex. There are connections with other portions of the frontal lobe, including the OFC, the DLPFC and the medial motor areas. The MPC is important in auditory and visual associations. The ventrolateral prefrontal cortex is concerned with mnemonic processing of objects. The OFC has important connections with the limbic system, including the amygdala. Disinhibition syndromes, ranging from mildly inappropriate social behavior to full-blown mania, may occur with dysfunction of the OFC, particularly of the right hemisphere. Patients with OFC dysfunction are also prone to display emotional lability, poor judgment and insight, and distractibility.
Frontal association areas may be involved in various degenerative processes, especially those such as frontotemporal dementia, which are likely to affect frontal lobe function. The earliest change is often a loss of memory, especially of recent memory or of retention and immediate recall. This may be followed by impaired judgment, especially in social and ethical situations. Absence of the inhibitions acquired through socialization may lead to inappropriate behavior and carelessness in dress and personal hygiene. Sexual promiscuity may develop. Loss of ability to carry out business affairs and attend to personal finance is common. The ability to perceive abstract relationships is impaired early. The patient may carry out simple well-organized actions, but he may be incapable of dealing with new problems within the scope and range expected for a person of similar age and education. Tasks requiring a deviation from established routine and adaptation to unfamiliar situations are the most difficult. There is loss of attentiveness, and distractibility may be marked. There are problems with comprehension and loss of ability to make associations. Acquisition and synthesis of new material is difficult. The time needed for solving intellectual problems is prolonged, and the patient fatigues rapidly.
Emotional lability may be prominent, with vacillating moods and outbursts of crying, rage, or laughter, despite a previously even temperament. There may be marked irritability. The mood is often euphoric, with an increased sense of well-being. Facetiousness, levity, and senseless joking and punning (witzelsucht) or moria (Gr. “silliness”), or apathy, indifference, emotional blunting, and lack of initiative and spontaneity may be present. Abulia refers to difficulty in initiating and sustaining spontaneous movements and reduction in emotional responsiveness, spontaneous speech, and social interaction. It is characteristic of frontal lobe and basal ganglia lesions. The patient may fail to link immediate impressions with past experience, leading to confusion and disorientation. There is usually progressive deterioration and increasing difficulty with intellectual functions. Extensive bilateral prefrontal lesions may cluminate in akinetic mutism or a state of persistent unresponsiveness (see Chapter 51).
Similar symptoms may occur with frontal lobe neoplasms. Either witzelsucht and euphoria or indifference and apathy are early manifestations, and they may be evident before memory loss and difficulties with judgment become apparent. There are often other signs of intracranial disease, such as weakness, focal or generalized seizures, frontal ataxia, forced grasping, anosmia, or visual field defects. Evidence of increased intracranial pressure usually occurs late. Although severe impairment of function may occur with lesions of the anterior frontal lobes, further localization may not be possible from the examination alone. There is no definite focus for which removal leads to dementia, and massive lesions of the frontal lobe, especially if unilateral, may cause few symptoms, particularly if the lesion is in the nondominant hemisphere.
The severe disability that may result from a frontal lobe lesion is strikingly illustrated by Eslinger and Damasio’s patient “EVR” (Box 7.2). Following frontal lobotomy, patients often developed indifference, lack of insight, euphoria, emotional outbursts, tactlessness, and social ineptitude, but without demonstrable memory or cognitive deficits.
Frontal Lobe Dysfunction
At the age of 35, a previously healthy patient, “EVR,” underwent removal of a large orbitofrontal meningioma. Surgical recovery was uneventful and there was never any evidence of tumor recurrence. Although he seemed superficially normal, with a verbal IQ of 120 and normal neuropsychological testing, the patient’s behavior, judgment, and social interactions were forever impaired. He invested and lost his life’s savings in an ill-advised business venture. He was fired from a succession of jobs because of tardiness and disorganization. His wife divorced him, and, unemployed, he moved back in with his parents. He required 2 hours to prepare for work each morning. He took a job 100 miles from his home but was fired for lack of punctuality. He spent entire days shaving and washing his hair. Minor decisions were scrutinized ad infinitum, including simple purchases and deciding where to eat. He collected outdated and useless items (see also Volle et al.), including dead houseplants, old phone books, 6 broken fans, 5 broken television sets, 3 bags of empty orange juice cans, 15 cigarette lighters, and countless stacks of old newspapers. The New York Times provided a poignant and very personalized description of the personality changes and other effects of frontal lobe dysfunction in When Illness Makes a Spouse a Stranger (D. Grady, May 5, 2012), an article on frontotemporal dementia.
Frontal Motor Areas
The motor areas of the frontal lobe include the primary motor cortex (area 4) as well as the premotor and supplementary motor areas. The motor cortex contains the large motor neurons (Betz cells) that give rise to the corticospinal and corticobulbar tracts. The premotor cortex lies just anterior to the primary cortex, squeezed between the precentral gyrus and the posterior border of the prefrontal area (area 6); it is involved in the planning and execution of movements, particularly sequences of movements (the basis for Luria’s hand sequence or fistedge-palm test, Chapter 8). It receives afferents from other areas of the cortex, including the sensory cortex and elsewhere in the frontal cortex, and projects to the motor cortex and the motor thalamus. Some fibers descend and make up part of the extrapyramidal system.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







