FIGURE 48.1 Lippman’s test; moving the biceps tendon back and forth in the bicipital groove reproduces the pain in biceps tendonitis. (From Cipriano, JJ. Photographic Manual of Regional Orthopaedic and Neurological Tests. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2003, with permission.)
Full active ROM should carry the shoulder through flexion, extension, adduction, abduction, and medial and lateral rotation. Note the motion of the scapula and the scapulohumeral rhythm (see Chapter 27). When severe shoulder pathology restricts glenohumeral motion, the patient abducts the arm primarily at the scapulothoracic joint. Excessive scapular motion during arm abduction signifies limited glenohumeral motion. Some or all of abduction may be accomplished by shrugging, and the scapula and humerus move as a unit (reversal of scapulohumeral rhythm). Limitation of active ROM could occur because of mechanical limitation (e.g., frozen shoulder) or because of pain or muscle weakness. Passive greater than active ROM excludes any mechanical limitation. Even when there is marked limitation of active ROM due to pain or a torn rotator cuff, gentle passive ROM may be normal. A convenient way to assess active ROM is the Apley scratch test, in which the patient makes three moves as if to scratch: (a) reaching to the opposite shoulder to touch it from the front, (b) from behind the neck as if to touch the upper vertebral border of the opposite scapula, and (c) from behind the lower back as if to touch the lower tip of the opposite scapula (Figure 48.2A and B). The latter two can be combined by having the patient try to touch the fingertips together in the interscapular space, one hand from above and the other from below. To elicit the drop-arm sign, during passive ROM with the patient sitting, the examiner places the shoulder in 90 degrees of abduction then releases the arm and asks the patient to slowly lower it. This may cause severe pain, or the patient may not be able to lower the arm slowly and it may drop abruptly. A positive drop-arm sign suggests dysfunction of the supraspinatus tendon. In a large series of patients with suspected RCTs the clinical findings most closely associated were included infra-and supraspinatus atrophy, weakness with either elevation or external rotation, painful arc, and impingement sign. Age 65 years and above and night pain also correlated with the presence of RCT.
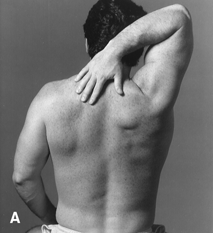
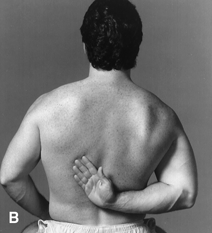
FIGURE 48.2 A,B. The Apley scratch test. Exacerbation of the patient’s pain indicates degenerative tendinopathy of one of the rotator cuff tendons, usually the supraspinatus. (From Cipriano, JJ. Photographic Manual of Regional Orthopaedic and Neurological Tests. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2003, with permission.)
A number of specific maneuvers may be useful to evaluate the shoulder.
Impingement Sign
Two different impingement signs are in common use; both produce pain by trapping the rotator cuff tendons between the humeral head and the acromion during passive movement of the shoulder. In the Neer impingement test, the extended arm is internally rotated and then raised directly overhead with the palm facing laterally (Figure 48.3). In the Hawkins (Hawkins-Kennedy) impingement test, the arm is held in abduction and external rotation, elbow flexed, and then forcefully rotated internally, driving the supraspinatus tendon through the subacromial space (Figure 48.4). In another method, the elbow is flexed and the shoulder internally rotated as if to lay the forearm across the abdomen; the arm is then raised so that the forearm passes in an arc in front of the face and overhead. Internal rotation is a key part of the maneuver in the impingement tests, as it rotates the greater tuberosity anteriorly and narrows the space beneath the acromion. Inflamed and tender tendons are then trapped between the greater tuberosity and the acromion, causing pain during the maneuver. The pain may also lessen when the patient bends forward and lets the arm hang limp, distracting the inflamed tendons from the point of impingement, or if the examiner supports the flexed forearm at the elbow and pulls gently downward. In impingement syndrome, the diseased tendons pass beneath the acromion in the arc between 60 and 120 degrees of abduction. Abduction out to 60 degrees may be painless, but the arc between 60 and 120 degrees is very uncomfortable; beyond 120 degrees, after the swollen and tender supraspinatus tendon has cleared the narrow confines of the subacromial space, motion is again painless. The “painful arc sign” is elicited either by having the examiner elevate the patient’s arm passively to 180 degrees and then having the patient lower the arm actively or by having the patient actively abduct from 0 to 180 degrees. The sign is positive with pain in the 60 to 120 degrees range and not at the extremes. The painful arc sign has high sensitivity as a single finding, making it helpful in ruling out RCTs when absent.

FIGURE 48.3 Elicitation of Neer’s impingement sign. With the arm pronated, elevation entraps the supraspinatus tendon under the coracoacromial arch. (From Cipriano, JJ. Photographic Manual of Regional Orthopaedic and Neurological Tests. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2003, with permission.)

FIGURE 48.4 Elicitation of the Hawkins impingement sign. Rotation forces the rotator cuff tendons beneath the coracoacromial arch. (From Cipriano, JJ. Photographic Manual of Regional Orthopaedic and Neurological Tests. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2003, with permission.)
The action of the supraspinatus can be relatively isolated by having the patient attempt to abduct the arm laterally with the shoulder internally rotated and forearm hyperpronated, as if to move the little finger toward the ceiling. The shoulder should be flexed about 30 degrees forward of the coronal plane of the body to line the humerus up in the plane of the scapula and isolate the supraspinatus. This is the same movement that would be made emptying a can and is sometimes referred to as the empty can test.
In Speed’s test, the elbow is held extended and supinated, and the patient flexes the shoulder (not the elbow) against resistance (Figure 48.5). This movement causes the biceps tendon to move through the bicipital groove and causes anterior shoulder pain in patients with bicipital tendonitis. In Yergason’s test, with the elbow flexed to 90 degrees and the forearm pronated, the patient attempts to simultaneously flex the elbow and supinate the hand against the examiner’s resistance (Figure 48.6). The biceps is an elbow flexor and supinator, and this test uses both motions to cause the biceps to contract and its tendon to move in the bicipital groove, reproducing pain in the anterior shoulder in bicipital tendonitis.
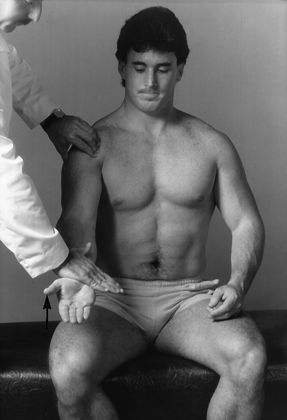
FIGURE 48.5 Elicitation of pain from the anterior shoulder in bicipital tendonitis by flexion of the shoulder against resistance. (From Cipriano, JJ. Photographic Manual of Regional Orthopaedic and Neurological Tests. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2003, with permission.)
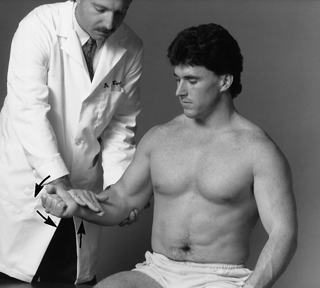
FIGURE 48.6 Elicitation of pain from the anterior shoulder in bicipital tendonitis by flexing and supinating the elbow against resistance, which stresses the biceps tendon in its groove (Yergason’s sign). (From Cipriano, JJ. Photographic Manual of Regional Orthopaedic and Neurological Tests. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2003, with permission.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







