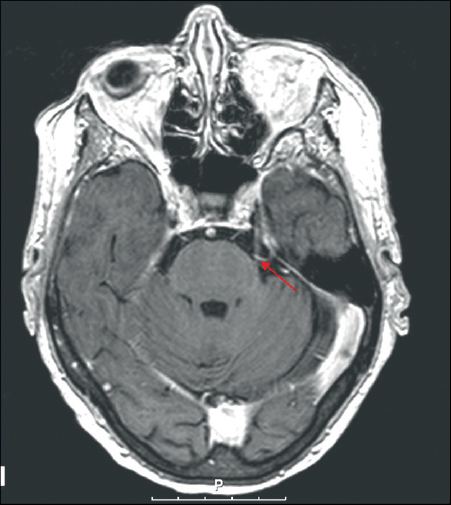
62 When was neuromodulation first used in the treatment of pain? 15 A.D.—before the FDA! Scribonius, the physician to the Roman emperor Tiberius, observed that the pain from gout was reduced in one of the emperor’s freed slaves after the person stepped on and was shocked by an electric torpedo fish! Thereafter, Scribonius recommended this as a treatment for gout.1 Upon what modern theory is neuromodulatory pain therapy based? The gate theory of pain, proposed by Melzack and Wall in 1965. What are the major implanted and noninvasive technologies being used to accomplish neuromodulation? Chronic implanted technologies: 1. Electrical neuromodulation/stimulation (deep brain stimulation [DBS], vagus nerve stimulation [VNS], spinal cord stimulation [SCS], peripheral nerve stimulation [PNS]) 2. Chemical neuromodulation/pharmacotherapy (intrathecal drug pumps, e.g., baclofen, morphine, etc.); acute noninvasive technologies 3. Transcranial magnetic stimulation (TMS) Nociceptive pain, neuropathic pain, and central pain. 1. Nociceptive pain results from noxious stimulation of intact tissues as well as from tissue damage and inflammation. This pain arises from conditions that continually or intermittently activate tissue nociceptors, usually through trauma or an inflammatory process, often autoimmune, which result in peripheral sensitization. 2. Neuropathic pain is generated by a neural structure that does not transduce noxious stimulation and is therefore a result of aberrant signals. It is caused by damage to the peripheral pain pathways arising from conditions including diabetic neuropathy, trauma, nerve crush injury, and amputation. 3. Central pain results from damage to a central nervous system structure governing pain signal transmission, perception, or modulation. This is due to conditions such as thalamic stroke, tumor, multiple sclerosis, or trauma including spinal cord injury or brain surgery. What fiber types conduct nociceptive pain impulses? Aδ-fibers and C-fibers. What are the diameters and conduction speeds of these fiber types? Aδ-fibers: 1 to 6 mm diameter, 5 to 30 m/s (relatively slow), myelinated C-fibers: <1.5 mm diameter, 0.5 to 2 m/s (slowest), unmyelinated What are the pain types and qualities of the pain signals mediated by these fiber types? Aδ-fibers: “first pain,” prickly sensation. C-fibers: “second pain,” slow onset, poorly localized, burning pain What neuronal structure has been implicated in the pathophysiology of chronic cluster headaches (CCHs)? Posterior hypothalamus What is a minimally invasive treatment for CCH? Sphenopalatine ganglion blockade with local anesthetics. How effective is this minimally invasive treatment for CCH? CCHs are alleviated in approximately 30 to 60% of patients treated with sphenopalatine ganglion blockade.2 What is a slightly more invasive treatment for CCH? Greater occipital nerve (GON) stimulation. (This has shown promise in studies as a potential therapy. This modality is presently not FDA-approved for this indication.) For CCH refractory to medications and these two minimally invasive surgical techniques, what is an alternate therapy? Deep brain stimulation (DBS) of the posterior hypothalamus (pHyp). (This has shown promise in a research study as a potential therapy.3 This modality is presently not FDA-approved for this indication.) What are the vertical and lateral coordinates of this target? Coordinates: 2 mm lateral to the midline, and 3 mm posterior and 5 mm inferior to the midcommissural point4 When localizing the pHyp target, what features are seen with microelectrode recording at the pHyp? Average firing rates of approximately 24 spikes per second When localizing the pHyp target, what features may be seen with macroelectrode stimulation at the pHyp? 1. Ocular deviation toward the stimulated side (at 3–4 V, 60 Hz), followed by 2. Ipsilateral CN III motor responses (at 4–5 V, 60 Hz), followed by 3. Sensation of fear and panic (at 5–6 V, 60 Hz) Side effects to avoid: vegetative effects and cardiovascular effects What are representative effective parameters for chronic stimulation of pHyp for CCH? 185 Hz, 60- to 90-μs pulse width, and amplitude between 1 and 3 V, in unipolar configuration with case positive5,6 What is the effectiveness of pHyp DBS for CHH? At 24 months follow-up in one study, effectiveness was characterized by 71% of postoperative days being pain-free, with significantly reduced intensity and duration of pain episodes. The mean time to reach stable pain benefit was 42 days.7 What are the major side effects and complications? Transient reversible diplopia, intraparenchymal and intraventricular hemorrhage6 What is critical for the success of this procedure? Patient selection, specifically proper and precise diagnosis of CCH, as this is not effective for other types of headaches or facial pain syndromes What is occipital neuralgia? The International Headache Society (IHS) defines occipital neuralgia as paroxysmal shooting or stabbing pain in the dermatomes of the nervus occipitalis major or nervus occipitalis minor. What are the causes of occipital neuralgia? 1. Vascular a. Irritation of C2 nerve roots by aberrant branch of posterior inferior cerebellar artery (PICA) b. Dural arteriovenous fistula (DAVF) in cervical region c. Bleeding from bulbocervical cavernoma d. Cervical intramedullary cavernous hemangioma e. Giant cell arteritis f. Fenestrated or aberrant vertebral artery impinging on C2 roots 2. Neurogenic a. Schwannoma of occipital nerve b. C2 myelitis c. Multiple sclerosis 3. Muscular/tendinous 4. Osteogenic a. Arthrosis or sclerosis of C1/C2 b. Cervical osteochondroma c. Osteolytic lesion of the cranium d. Excessive callous formation following C1/C2 fracture8 What is the differential diagnosis of occipital neuralgia? Need to rule out: 1. Tumors 2. Infection 3. Congenital anomalies (Chiari malformation) Distinguish from other headache syndromes: 1. Migraine headache 2. Cluster headache 3. Tension headache 4. Hemicrania continua8 What have been the mainstays of treatment for intractable occipital headache? Conservative management: 1. Reduction of muscle tension and improvement of posture 2. Pharmacological: a. Tricyclic antidepressants b. Antiepileptic medications: i. Carbamazepine ii. Gabapentin iii. Pregabalin Interventional management: 1. Nerve block injection with local anesthetic and steroid along the course of the nerve, usually at the point where it penetrates the trapezius aponeurosis, a common site of constriction 2. Pulsed radiofrequency treatment of the occipital nerve may be performed if lasting relief is not obtained by the nerve block. 3. Subcutaneous occipital nerve stimulation (if the two previous therapies are ineffective)8 How effective are these interventional procedures, and what are their limitations? They are very effective; however, the development of delayed deafferentation pain commonly occurs in the distribution of the affected nerve. What neuromodulatory therapy may be used to treat occipital neuralgia? Occipital nerve stimulation How effective is this modality? Occipital nerve stimulation has been show to provide good outcome in 50%9 to 75% of patients.10 When and by whom was trigeminal neuralgia first described? Nicolaus Andre coined the term tic douloureux in 1756 and is credited as being the first person to describe the symptoms of trigeminal neuralgia. What are the symptoms of trigeminal neuralgia? Idiopathic typical trigeminal neuralgia has been defined by five cardinal features. A. Pain 1. Pain that is paroxysmal 2. Pain that is provocable 3. Pain that is unilateral 4. Pain that is confined to the trigeminal territory B. Sensation 5. Intact light touch or pinprick sensation Idiopathic atypical trigeminal neuralgia is less clearly defined and encompasses departures from the classic symptoms such as presence of prolonged periods of unprovoked milder pain superimposed on paroxysmal pain episodes. What important conditions are in the differential diagnosis (DDx) of trigeminal neuralgia? 1. Dental pathology (which is often the initial misdiagnosis prior to diagnosis of trigeminal neuralgia) 2. Sinus disease 3. Temporomandibular joint (TMJ) disease (pain is not paroxysmal, may be increased with eating but has no trigger point) 4. Cluster headaches (occur in protracted clusters, accompanied by ipsilateral nasal congestion and lacrimation, and an ipsilateral Horner’s syndrome) 5. Atypical facial pain (longer duration, lasting minutes to hours instead of the few seconds characteristic of trigeminal neuralgia) 6. Demyelinating lesions of the brainstem, including multiple sclerosis (MS) (10% of MS patients have facial pain as their initial presentation) 7. Vascular ischemia affecting the descending root of CN V What is symptomatic trigeminal neuralgia? Symptomatic trigeminal neuralgia is the same as secondary trigeminal neuralgia, which comprises the forms of trigeminal neuralgia attributable to a known or demonstrable pathology. How is symptomatic trigeminal neuralgia classified? Symptomatic trigeminal neuralgia (TN) is classified in the same manner as idiopathic TN, as follows: A. Typical symptomatic trigeminal neuralgia: same clinical features as in typical idiopathic TN B. Atypical symptomatic trigeminal neuralgia: clinical features deviating from typical idiopathic TN What are other major facial pain syndromes? 1. Postherpetic zoster neuralgia 2. Postsurgical deafferentation pain conditions: a. Anesthesia dolorosa b. Nervus intermedius neuralgia c. Vagoglossopharyngeal neuralgia 3. Primary headaches a. Migraine (with or without aura) b. Tension-type headaches c. Cluster headache and trigeminal autonomic cephalgia d. Other primary headaches 4. Secondary headaches a. Attributed to head or neck trauma b. Attributed to cranial or cervical vascular disorders c. Attributed to nonvascular intracranial disorder d. Attributed to a substance or its withdrawal e. Attributed to infection f. Attributed to psychiatric disorder 4. Other entities or categories recognized in DDx of craniofacial pain a. Trigeminal neuralgia b. Neuropathic pain disorder c. TMJ disorder d. Ophthalmologic disorders e. Ear, nose, and throat conditions f. Sinus disorders g. Oral cavity and salivary gland disorders h. Craniocervical disease i. Neoplasia j. Psychogenic What is atypical facial pain? Atypical facial pain is an ill-defined category of facial pain, with little or no resemblance to trigeminal neuralgia. What are the more common characteristics of atypical facial pain? Pain is often bilateral, constant (not paroxysmal), and not provoked by external stimuli. Pain qualities are often described as “gripping,” “drawing,” “pulling,” “boring,” and “bursting.” What are the two subtypes of secondary (or symptomatic) trigeminal neuralgia? Secondary (or symptomatic) trigeminal neuralgia is divided into intrinsic and extrinsic forms: 1. Intrinsic secondary trigeminal neuralgia: TN in which a causative lesion is present within the central nervous system 2. Extrinsic secondary trigeminal neuralgia: TN in which a causative lesion is present outside the central nervous system List example cases of intrinsic secondary trigeminal neuralgia. Multiple sclerosis, pontine abscess, syringobulbia, infarct, hydrocephalus, pontine cyst List example cases of extrinsic secondary trigeminal neuralgia. Vascular lesions, skull deformities, normal vessel causing root compression, basilar impression (platybasia), Paget’s disease, aneurysm, persistent primitive trigeminal artery, Chiari type I malformation, infections What side is more common? Right True or false: trigeminal neuralgia is more common in men than women. False. It’s more common in women (1.74:1 age-adjusted).6 Which branch is most commonly affected? V2 + V3 (32%) How frequent is TN in patients with MS? 1% of patients with MS develop TN. For which reflexes does the trigeminal nerve provide afferent signal conduction? • Corneal reflex (V1 afferents to CN VII efferents) • Sternutatory reflex (sneezing) What sensory (and motor) modalities are subserved by trigeminal fibers? • Sensation: soft touch, thermal, and pain sensation in the face • Motor: muscles of mastication Trigeminal nerve → gasserian ganglion (middle cranial fossa) → entry via trigeminal nerve entry zone into mid-pons: 1. Light touch fibers then ascend to terminate in the chief sensory nucleus of CN V. 2. Pain and temperature fibers descend to terminate in the nucleus of the spinal tract of CN V. What remaining modality (other than sensory and motor, detailed above) is sensed and where does it terminate? Fibers transmitting jaw proprioception terminate in the mesencephalic nucleus. What age predilection, if any, exists for trigeminal neuralgia? Most cases occur in adults over age 35, with occasional occurrences in children. How is trigeminal neuralgia diagnosed? Trigeminal neuralgia is usually diagnosed based on a history of extremely severe triggered facial pain in the absence of numbness or other objective findings. Paroxysms of pain recur in a distribution of one or more branches of the trigeminal nerve. What are the neurological findings in trigeminal neuralgia? Neurological exam is usually normal. Some patients may have concurrent hemifacial spasm. Patients whose pain attacks are triggered by eating may appear thin or cachectic. What is the quality of the pain in trigeminal neuralgia? Trigeminal neuralgia pain is typically lancinating, episodic, intermittent pain and is usually triggered by stimuli. What is the quality of the pain in atypical trigeminal neuralgia? Atypical trigeminal neuralgia pain is often steady instead of episodic, throbbing, and persisting for hours. It is characterized as dull, aching, crushing, or burning. What is the drug of choice in the medical treatment of trigeminal neuralgia? Tegretol (carbamazepine) 800 mg/day to 1200 mg/day in four divided doses; doses should be titrated to effect and may require serum levels above those required for seizure control. What are the effects of overdosage with this medical therapy? Drowsiness, dizziness, ataxia, unsteady gait, and nausea What side effects may occur with this therapy? Hepatotoxicity may also occur, but this is reversible upon discontinuation. Aplastic anemia is a rare but serious complication. Patients require periodic liver function tests (LFTs) and blood count (CBC). What alternate medical therapies are available? Phenytoin (Dilantin), baclofen (Kemstro and Lioresal), gabapentin (Neurontin), amitriptyline (Elavil), pregabalin (Lyrica) What is the trigeminal root entry zone (REZ)? The trigeminal REZ is the junctional zone where axons from the gasserian ganglion transition from being myelinated by Schwann cells (of mesodermal origin) to being myelinated by oligodendrogliocytes (of neuroectodermal origin) prior to entering the brainstem. This is a well-defined segment of the trigeminal sensory root located 2 to 3 mm external to the pial surface of the pons. What is the historical name for the trigeminal REZ? Obersteiner-Redlich zone In what other condition is the REZ (from another nerve) affected? Tabes dorsalis, a spirochetal infection, in which over 90% of cases a lancinating brief stabbing pain is associated with pathological findings of thinning and grayness of the posterior roots. What is the most common vascular structure associated with trigeminal neuralgia? Superior cerebellar artery (SCA) Fig. 62.1 MRI axial T1 image with contrast at the level of the midpons showing an aberrant loop of the superior cerebellar artery (red arrow) impinging on the root of the trigeminal nerve. The patient presented with clinical symptoms of trigeminal neuralgia.
Pain
62.1 Introduction
62.2 Headaches
62.3 Occipital Headaches
62.4 Trigeminal Neuralgia
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






