Postlaminectomy Cervical Kyphosis
Matthew J. Goldstein
Michael P. Ast
Jeff S. Silber
Greg D. Anderson
Todd J. Albert
BACKGROUND
Cervical lordosis is critical to the normal alignment of the spine. It produces a neutral sagittal vertical axis and minimizes the muscular effort necessary to maintain an upright posture (1). Furthermore, it compensates for the normal thoracic kyphosis and allows the head to be positioned over the trunk. Cervical kyphosis, however, results in a major alteration of biomechanical forces acting on the neck. It results in abnormal biomechanical forces that often lead to mechanical neck pain or progressive neurologic symptoms. As defined by White et al. (2) cervical kyphosis is a forward decompensation of the head in the sagittal plane. Segmental kyphosis is said to be present when there is an angular relationship between two vertebrae with a dorsally directed apex. Patients with preexisting kyphosis, as well as those undergoing excessively wide laminectomy without stabilization, are susceptible to progressive postlaminectomy kyphosis.
Prevention of cervical kyphosis remains paramount and when noted, appropriate treatment should be instituted (3). This chapter focuses on progressive cervical kyphosis following cervical laminectomy.
ANATOMY AND BIOMECHANICS
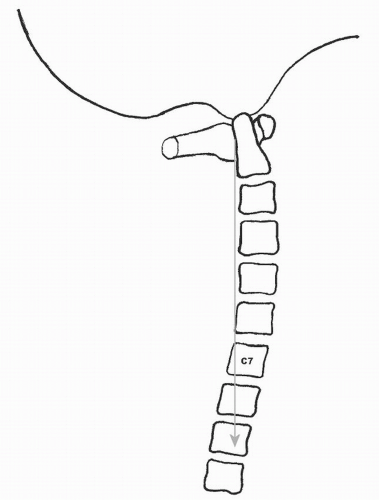
The normal weight-bearing axis of the head (sagittal vertical axis) passes through the middle of the C1 and T1 vertebral bodies and falls behind the vertebral bodies of C2 through C7 (Fig. 101.1) (4). The normal mean sagittal contour of the adult cervical spine is 14.4 degrees of lordosis (5). Biomechanically, the cervical spine comprises an anterior column composed of the vertebral bodies, disks, and associated ligaments and a posterior column composed of the facet joints, laminae, and dorsal ligamentous structures (2,6,7). Under normal conditions, compressive loads are supported by a lordotic cervical spine by distributing 36% of the load through the anterior column and 32% of the load through each side of the posterior column (thus, 64% of the total applied axial load) (8).
Ligament sectioning studies have documented the importance of both the ventral and dorsal osteoligamentous structures in maintaining spinal stability and preventing the development of kyphosis. At least one intact dorsal ligamentous structure and an intact anterior column are required to prevent catastrophic failure of the spinal segment (6,7).
The competence of posterior column structures, in particular the facet joints, is also critical to the maintenance of a lordotic cervical posture. Using finite element analysis, Saito et al. (9) found that loss of one or more dorsal elements (such as the spinous process, ligamentum flavum, or intraspinous ligaments) subjected the facet joints to tensile forces rather than the normal compressive loads. Several investigators have documented decreased stiffness and increased motion of the cervical spine following laminectomy (10,11).
Cusick et al. (12) found that unilateral cervical facetectomy decreased the strength of the vertebral motion segment by 31%, whereas bilateral facetectomy resulted in a 53% decrease in strength during flexion compression loading. Facetectomy produced ventral displacement of the instantaneous axis of rotation in the sagittal plane, further increasing compressive loads on anterior column structures (12). Using a finite-element cervical spine model, Kumaresan et al. (13) demonstrated that removal of more than 50% of the cervical facet joints bilaterally transferred high stresses to the annulus fibrosis during flexion and rotation.
Raynor and Carter (14) studied the effects of both 50% and 70% facetectomies on the ultimate strength of the cervical motion segment. A 50% facetectomy allowed exposure of only 3 to 5 mm of nerve root but did not result in failure at the facet joint, while a 70% facetectomy allowed exposure of 8 to 10 mm of nerve root but resulted in a fracture of the facet joint with shear loading. Zdeblick et al. (15,16) studied the effect of progressive loss of either the facetjoint or the facet capsule in a single-level laminectomy model and found that both flexional and torsional stability were significantly compromised by loss of more than 50% of either structure. Nowinski et al. (17) demonstrated significantly increased motion with resection of as little as 25% of the facetjoint in a multilevel laminectomy model.
Loss of anterior column height can also contribute to the development of cervical kyphosis. The disks constitute 15% of the overall length of the anterior column of the cervical height and are normally slightly trapezoidal in shape with a greater height ventrally than dorsally. Thus,
loss of disk height due to degenerative arthritis or collapse of a vertebral body secondary to a fracture can shorten the anterior column, leading to a kyphotic deformity. This, in turn, can alter the weight-bearing axis and transfer pathologic tensile and shear forces to the posterior column structures.
loss of disk height due to degenerative arthritis or collapse of a vertebral body secondary to a fracture can shorten the anterior column, leading to a kyphotic deformity. This, in turn, can alter the weight-bearing axis and transfer pathologic tensile and shear forces to the posterior column structures.
The contribution of normal muscle function to the development of cervical kyphosis continues to be debated. Perry and Nickel (18) maintained that dorsal cervical muscle paralysis did not necessarily lead to notable instability as long as the bony and ligamentous restraints remained intact. However, Saito et al. (9) demonstrated in an in vitro study that any forward shift in the gravitational center of the head promoted cervical kyphosis. Nolan and Sherk (1) studied the extensor musculature and found that the semispinalis cervicis and capitis were primarily responsible for extension of the spine and head. They emphasized the importance of preserving the attachment of these muscles to the C2 arch whenever possible and demonstrated that approximately 14 kg of force was required to support the head in a horizontal position. Other authors have emphasized the role of muscle denervation or fibrosis secondary to aggressive surgical exposure and retraction that can predispose to the development of a kyphotic deformity (19,20).
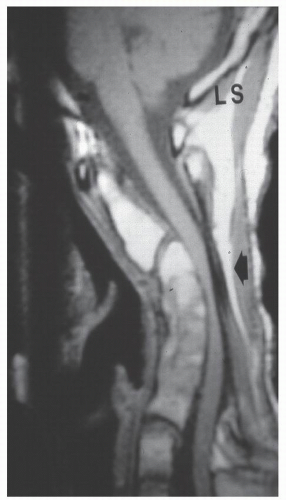
Regardless of the initial pathomechanics, cervical kyphosis initiates a cascade of pathologic forces that can result in the development of a progressive deformity (4). As the head shifts forward, the weight-bearing axis is translated ventrally, causing the anterior column to be loaded with increased compression and the posterior column with increased tension. This translation accelerates the degeneration of the anterior column (21). Dorsal extensor muscles are placed at a mechanical disadvantage and may become less effective at holding the head upright (1). Chronic tensile forces may result in attenuation of the dorsal ligamentous structures and facet capsules. As the deformity progresses, the neural elements are translated forward against the apex of the kyphosis, potentially leading to cord compression and ischemia (Fig. 101.2). This, in turn, can lead to a triad of progressive deformity, neurologic compromise, and further stretching of the dorsal soft tissue restraints, producing a worsening deformity.
As the spinal cord is pulled against the apex of the kyphotic deformity, tensile strain within the spinal cord is generated, resulting in irritation, dysfunction, or cell death of the anterior horn neurons. A finite amount of spinal cord lengthening, such as that which occurs with normal neck flexion, is tolerated. However, in pathologic kyphosis, the dorsal portion of the spinal cord may be lengthened beyond its elastic limit, leading to detrimental effects on the health and survival of cord neurons. Concomitantly, the ventral portion of the spinal cord is compressed against the apex of the kyphosis, bringing it into contact with degenerative osteophytes, ossified posterior longitudinal ligament and prolapsed intervertebral disks. The spinal cord may thus also be subjected to a compressive load across the apex of the kyphosis. The additive effect of these internal stresses results in pathologic changes within the spinal cord, most notably microvasculature and neuronal ischemia, and is partly responsible for the wide spectrum of neurologic manifestations observed in patients with a cervical kyphotic deformity (22,23).
CLINICAL PRESENTATION
The symptoms of cervical kyphosis can vary depending on the nature and severity of the underlying condition. The most common symptoms include neck pain, muscle fatigue, radiculopathy, myelopathy, and if severe, loss of forward gaze.
Patients suffering from postlaminectomy kyphosis often give a history of an initial period with improved myelopathic symptoms following the laminectomy surgery. However, over time, the loss of integrity of the dorsal osteoligamentous column and paraspinal musculature leads to a forward translation of the head. As the head translates in a ventral direction, the patient may experience worsening neck pain, muscle fatigue, neurologic deterioration, and occasionally loss of forward gaze (due to fixed downward head position). In addition to complaints of radicular arm pain, the history and physical may elicit signs and symptoms of recurrent spinal cord dysfunction. Myelopathy can present as subtle clumsiness in the hands, gait unsteadiness, or sphincter dysfunction. Signs of hyperreflexia, pathologic reflexes (such as Hoffmann and Babinski signs), and difficulty with tandem gait may also be observed.
The forward position of the head necessitates constant contraction of the neck extensor muscles in an attempt to balance the weight of the head against gravity, leading to muscle fatigue and neck pain that often worsens as the day progresses. Difficulty with horizontal gaze may be encountered in patients with a severe, fixed cervical kyphotic deformity, especially in patients with ankylosing spondylitis. In order to look forward, these patients must compensate with head and neck hyperextension at another level, typically occurring at the occipitocervical junction or lumbosacral spine.
Myelopathy in the setting of postlaminectomy kyphosis tends to be progressive and should be treated in order to halt spinal cord irritation and neuronal loss. Ebersold et al. (24) reported that, of several factors evaluated, only a prolonged duration of myelopathic symptoms predicted a poor neurologic outcome following surgical decompression for cervical spondylotic myelopathy. Iwasaki et al. (25) used MRI to evaluate cord atrophy at the apex of the cervical kyphosis. They described a ratio between the diameter of the cord at the apex of the kyphosis and the diameter of the cord at the pons-medulla junction. Patients with a ratio of less than 0.3 demonstrated progressive myelopathy. Further study of this measurement is necessary to evaluate its clinical utility.
POSTLAMINECTOMY CERVICAL KYPHOSIS: INCIDENCE AND ETIOLOGY
Due to the heterogeneous nature of patients undergoing laminectomy, the true prevalence of postlaminectomy cervical kyphosis is difficult to ascertain from the scientific literature. However, postlaminectomy cervical kyphosis does not appear to be a relatively rare phenomenon. Factors such as age, preoperative sagittal alignment, underlying diagnosis, aggressiveness of the dorsal surgical decompressive procedure, and the location and number of laminae removed all contribute to the risk of developing postoperative cervical instability.
Iatrogenic instability following multilevel cervical laminectomy often follows a characteristic clinical course. In the early postoperative course, there is often good resolution of radicular or myelopathic symptoms due to successful decompression of the neural elements. As kyphosis develops, the patient may complain of axial neck pain and fatigability of neck musculature. With time, the deformity tends to worsen, leading to recurrence of the original neurologic symptoms, and in some cases, emergence or progression of new neurologic deterioration. In some cases, the patient may return to the use of a cervical collar for comfort or may use manual support of the chin.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree