30
CHAPTER
![]()
Stimulation Therapy
William B. Gallentine
Despite the addition of numerous new antiepileptic drugs (AEDs) over the past 20 years, a substantial number of patients with epilepsy (approximately 35%) are unable to achieve pharmacologic seizure control. As such, nonpharmacologic options such as epilepsy surgery, ketogenic diet (KD), and neurostimulation are often pursued in these patients. Neurostimulaton refers to the use of electrical stimulation to manipulate neural networks, resulting in a desired therapeutic effect. The FDA has approved two neurostimulators for the treatment of epilepsy: the vagus nerve stimulator (VNS) and a responsive neurostimulation (RNS) known as Neuropace®. The VNS received its initial FDA approval in 1997, and since then, over 50,000 devices have been implanted in both adults and children. The Neuropace device has been approved very recently, and there is much more limited experience with its use. More recently, another type of neurostimulation has been investigated, that is, deep brain stimulation (DBS). This is not yet approved for use by the FDA. The purpose of this chapter is to provide an overview of the various forms of stimulation therapy, with the main focus on VNS, as this is the device being most widely used in clinical practice.
VAGUS NERVE STIMULATION
Overview
The VNS is an electrical device that consists of a generator implanted subcutaneously, usually on the left side of the chest, and an electrode, which is wrapped around the left vagus nerve in the neck. The “pacemaker-like” generator delivers an intermittent electrical stimulus to the vagus nerve which then relays this electrical signal to the brain. The generators, which are programmed to deliver impulses at timed intervals, have undergone several revisions over the years in an effort to upgrade their battery life, size, and diagnostic capabilities. Depending on the settings used for therapy, most VNS batteries will often last 5 to 10 years. However, those patients whose generators are set at low off-times (“rapid cycling”) may get only 1 to 2 years of life from their battery before needing to be replaced.
Implantation
The device is typically placed in the operating room most commonly by a neurosurgeon or an ENT surgeon. Placement is minimally invasive, and is most often considered out-patient surgery, with most patients discharged home the same day. There are two incisions made, one in the left chest, and the other in the left neck. The generator is inserted into a pocket in the chest, while the electrode in the neck is wrapped around the vagus nerve. The two are connected by a lead, which is tunneled under the skin. The procedure is typically performed under general anesthesia and typically is done in less than 1 hour. VNS placement is considered low-risk surgery, with greatest risk surrounding infection, which is thought to occur in less than 2% of cases.
Indications
The FDA has approved VNS in adults and adolescents for the treatment of drug-resistant partial-onset seizures based on its pivotal E03 trial (1). It is approved for adolescents, age 12 years and older, as the pivotal study only included children down to this age. However, multiple prospective and retrospective studies demonstrating both safety and efficacy in much younger children have been subsequently published (2). As such, it is quite common for VNS to be placed in children under the age of 12 (1 year of age being the youngest implanted) (2). Although approved by the FDA only for partial-onset seizures, VNS has also been shown to be effective in generalized epilepsies (Table 30.1).
Patient Identification and Pre-Implant Evaluation
The International League against Epilepsy (ILAE) defines drug-resistant epilepsy as the failure of two appropriately chosen and tolerated AEDs (whether as monotherapies or as combination) to control seizures for an adequate period of time. Once it has become clear that the patient is drug resistant, further evaluation to clarify the potential treatment options for the patient should be considered. This includes MRI (if not done within the past 2 years) and video EEG (vEEG) monitoring for seizure characterization/localization. Findings from these studies are helpful in determining epilepsy surgery candidacy. The importance of vEEG monitoring cannot be stressed enough, not only to localize seizures with the potential for epilepsy surgery, but also to assure that the drug-resistant spells are actually epileptic in nature. Unfortunately, cases have been reported in which EEG monitoring was not performed, and VNS was implanted in patients with psychogenic nonepileptic seizures. In circumstances where vEEG is not an option, ambulatory EEG to confirm that the events are epileptic should be performed at a minimum.
TABLE 30.1 Generalized Epilepsy Syndromes for Which VNS has Been Reported to be Efficacious
Lennox-Gastaut syndrome (both tonic and atonic seizures) Absence epilepsy Dravet syndrome Progressive myoclonic epilepsy Infantile spasms Tuberous sclerosis |
Patients who are not surgical candidates and who routinely have prolonged seizures or frequent emergency department (ED) visits or hospitalizations related to seizures are particularly good VNS candidates. Quite commonly patients will see a decrease in seizure length, resulting in decreased need for hospitalization and rescue medications.
Mechanisms of Action
The definitive mechanism of action for VNS is unknown. Mechanisms likely involve interactions between the locus ceruleus, nucleus solitarius, thalamus, and limbic structures (3). Functional neuroimaging revealed activation of the cortex and thalamus during VNS stimulation. Animal models displayed changes in neurotransmitters, including elevation of norepinephrine, increased GABA, increased serotonin, and decreased aspartate. VNS also has been shown to desynchronize EEG epileptic activity and decrease interictal discharges over time.
Dosing
There are two adjustable modes for the device: the standard maintenance mode and the magnet mode. The standard maintenance mode provides the background settings that run throughout the day at the desired time frequency. The magnet mode provides on-demand stimulation, activated by a swipe of a magnet over the VNS, which may be used in an effort to abort a seizure. The magnet also provides a means for turning off the device. If the magnet is held over the device for more than 65 seconds and held there, the device will turn off until the magnet is removed.
The VNS has several different dosing parameters that can be adjusted, including output current (OC), signal frequency (SF), pulse width (PW), and signal on/off time (Figure 30.1). The OC represents the amount of electrical current delivered in a single pulse of stimulation (mA). OC may range from 0 to 3.5 mA and this is the setting most commonly adjusted in the first few months of VNS titration. Initial OC is usually 0.25 mA, with increases of 0.25 mA every 2 weeks, which is a reasonable time frame to observe for response. A typical goal OC setting is between 1.0 and 2.0 mA. Two adjustments to OC may be done on the same day for those patients who may not be able to come to a clinic every 2 weeks, depending upon patient tolerability. The SF is the number of impulses per second (Hz). The PW is the duration of each individual pulse within the stimulation period. On/off time is the amount of time the generator provides stimulation, and the amount of time between stimulations. The percent on time is referred to as the duty cycle. Changes in the on/off time often take a few months to see the desired effect, so a longer observation period is in order, as opposed to the 2 weeks usually observed when adjusting the OC. Tables 30.2 and 30.3 summarize the typical initial settings and suggestions for VNS dose titrations. There really are no incorrect ways to titrate, as patient tolerability is the most important factor. However, a conservative approach as suggested earlier will allow for the patients settings to be maximized and will likely result in less potential side effects and longer battery life.
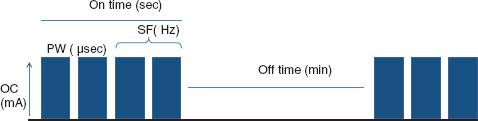
FIGURE 30.1 Adjustable VNS settings.
Abbreviations: µsec, microseconds; Hz, hertz; mA, milliamps; min, minutes; OC, output current; PW, pulse width; sec, seconds; SF, signal frequency.
![]()




