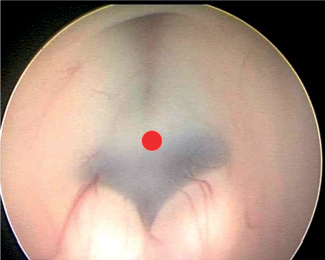
77 What are the goals of shunting? Improve ICP, restore dynamics, minimize future surgeries, and improve cognitive development in the infant Why is the peritoneum chosen for the terminus of shunts in most cases? 1. Easily and repeatedly accessible 2. Good absorptive capacity 3. Solves the need for “catheter-lengthening” in most cases What conditions may cause a problem with regard to the abdominal absorptive capacity? Obesity and previous abdominal surgeries that may have caused adhesions What are other potential sites of distal insertion of the catheter? Atrium, pleura, or gallbladder What is one of the drawbacks of peritoneal insertion? Siphoning What is siphoning? Increased drainage in upright position, sometimes with negative ICP, resulting in headaches, potential shunt obstruction, and other complications Why does this occur? The differential pressure created between the head and abdomen with positional changes Which systems can prevent this event from occurring? Siphon-control valves (e.g., delta, strata, or orbis-sigma valve, etc.) in combination with programmable systems or alone What are these devices collectively also known as? Devices to retard siphoning (DRS) or antisiphon devices (ASDs) What is their functioning principle? When negative pressure occurs, the diaphragm within the valve closes. True or false: A patient with a shunt who presents with clinical signs of raised ICP and small ventricles radiographically may have a shunt failure. True. ICP may be increased regardless of ventricular size. What are the components of a shunt? • A proximal catheter (ventricular) • A valve • A distal catheter • Unitized shunts have these three elements as a single unit Why are unitized shunts not used so frequently? If hemorrhage occurs during proximal catheter placement, immediate obstruction of the valve may occur rendering the shunt nonfunctional. What are the different types of valves on the market? 1. Pressure regulated (low, medium, high) 2. Flow regulated 3. Antisiphon (devices to retard siphoning) 4. On-off (particularly useful for chemotherapy patients) 5. Programmable What is the typical opening valve pressure in “low-pressure” valves? 5 cm H2O What is the typical opening valve pressure in “medium-pressure” valves? 10 cm H2O What is the typical opening valve pressure in “high-pressure” valves? 15 cm H2O Programmable valves are particularly useful in dealing with which specific complication following shunt insertion? Subdural collections (hygromas or hematomas) No What are some of the applications of LP shunts? • Communicating hydrocephalus • Idiopathic normal pressure hydrocephalus • Pseudotumor cerebri treatment • CSF leak/fistula/pseudomeningocele treatment What are some disadvantages of the LP shunts?2 1. Many systems lack a valve, relying only on the tube resistance and distal slits to regulate the diversion of CSF. 2. Measuring pressures may be a problem. 3. In children they has been associated with caudal migration of the brainstem. 4. Overdrainage with subsequent subdural collections may occur. What valves in LP shunts seem to overcome some of these complications? The H-V valves allow access to the shunt and overcome the problem of overdrainage.2 If while performing an LP shunt you encounter resistance with the Tuohy needle, what procedure may be required? Small laminotomy In evaluating a potential shunt complication, what is the most relevant aspect? The clinical history and shunt-related history of the patient and the physical examination. Often the patient (or parents/caregivers) will report a specific pathognomonic set of symptoms that occur when the shunt malfunctions. In addition, what adjuvant tests can (but do not necessarily have to) be performed? • Shunt series: Order skull AP and lateral x-rays, chest x-ray (CXR), and abdominal x-ray (AP and lateral views) • CT head: noncontrasted • CT abdomen: noncontrasted (to rule out the presence of a cyst, if suspected) • Shunt tap: for diagnosis or to alleviate increased pressure • Shunt “pumping”: to either test if it fills with CSF after depressing it or to alleviate increased pressure • Obtaining old records of prior CT scans to compare ventricular size is very useful. True or false: Shunt obstruction typically occurs distally. False. Shunt obstruction typically happens in the proximal catheter. Does it typically happen soon after surgery or long after it? It more commonly occurs in the early setting. How do you test a shunt intraoperatively? • You disconnect it from the valve intraoperatively and watch to see if there is good spontaneous flow. • You can also attach a manometer filled with fluid to the distal catheter to see if the fluid will drain distally (to the peritoneum) and down to what pressure. • Finally, you can try to aspirate proximally with a very low pressure syringe such as a 1-cc syringe) to see if you obtain proximal CSF from the ventricle (if no spontaneous flow is seen immediately upon disconnection). If you need to replace/remove a proximal shunt catheter and it seems “stuck,” what can you do? Do not pull on the catheter. Gently introduce a Bugbee wire and use the monopolar tip on the wire to proximally coagulate any attachments to the catheter (such as choroid plexus). This allows lysis from catheter tip adhesions. If the catheter is still producing significant resistance when attempting to be pulled, then it should be left in place, cut short (flush with the cranium), and a new catheter should be placed through a different entry point. When does valve obstruction typically happen? Soon after surgery How do you test valve obstruction? It is tested by performing a standard shunt tap with the use of a manometer, but it is important to know the valve characteristics to interpret if the valve is draining at its anticipated pressure/speed. What is another important early postoperative complication? Infection What is the overall risk of shunt infection? The risk varies based on the series reviewed, and is approximately 10% overall.3 What is the risk of reinfection following treatment of a first bout of shunt infection? 20% in the first few months4 1. Double glove use 2. Don’t touch the catheter when inserting it in the abdomen (use bayonetted forceps) 3. Don’t let CSF leak (good closure!)5 4. Do it quickly! (longer intraoperative times are associated with higher infection rates) What is the typical treatment of an infected shunt?6 • Externalize or remove shunt (latter requires EVD). • Treat infection (broad spectrum followed by targeted Rx). • Once cultures are negative for 3 days, reinsert shunt. What is the most common offending organism?6 Coag-negative staphylococcus: Staphylococcus epidermidis What is “shunt nephrosis”? A slow protracted infection leading to nephritis from immunocomplex deposition in the glomerular membrane When does shunt disconnection usually occur? Soon after surgery. Do not confuse with shunt fracture, which is a late phenomenon than may occur months to years after surgery. What other complications typically occurs late? • Slit Ventricle syndrome (SVS) • Pseudocyst formation True or false: SVS is a complication due only to overdrainage. False; it is also a problem of lack of cerebral compliance. How do patients with SVS present? With signs of increased ICP (headaches, nausea, vomiting) mixed with posture symptoms (worse when upright) and sometimes acute neurological deterioration What are the options available to treat SVS? • Attempt headache management medically if the patient’s clinical status allows. • Change the valve to a higher setting. • Add a DRS or change it to a flow-regulated valve. What is a common complication of “on-off” valve systems? Inadvertent “off” positioning by the patient during sleep or otherwise, impeding functioning of the valve. This is the reason why these valves should be implanted high in the frontoparietal area. What physiological requirement is necessary when considering endoscopic third ventriculostomy (ETV)? Intact absorption of CSF How can that be tested? By performing an infusion test. However, this is not necessary in all cases. Fig. 77.1 Anatomical point for third ventriculostomy between infundibular recess and mamillary bodies (red dot). Note the infundibular recess anteriorly, and the mammillary bodies posterior to the insertion point.
Treatment
77.1 Basics
77.2 Shunt Complications
77.3 Endoscopy
Treatment
Only gold members can continue reading. Log In or Register to continue

Full access? Get Clinical Tree






