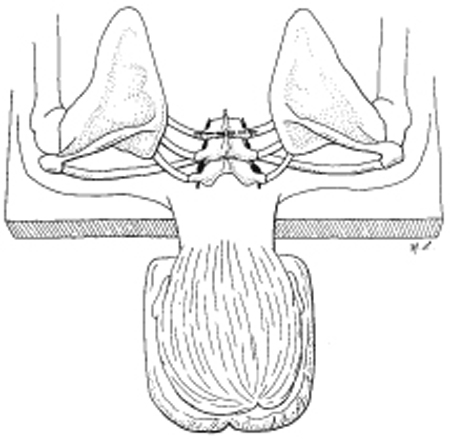
56 Upper Dorsal Sympathectomy for Hyperhidrosis A 24-year-old, right-handed woman who works as a teacher was seen with a main complaint of excessive perspiration in her hands and soles of her feet since puberty. There was no family history of hyperhidrosis. The patient tried medical therapy (anticholinergic drugs), which was not well tolerated because of dry mouth, dilated pupils, and gastrointestinal disturbances. She had not tried any topical anticholinergic agents, antiperspirant creams, or other drugs. Examination revealed excessive perspiration at her hands, axilla, and her feet. Her hands felt cold and clammy but otherwise the neurological exam was completely normal. Essential (idiopathic) hyperhidrosis Essential hyperhidrosis usually begins in the teens after the start of puberty. The excessive sweating is most pronounced in both hands, but axilla and feet may also be involved. This may result in occupational hazards, but the majority of patients seek medical attention because the symptoms are socially unacceptable. Because stressful situations worsen the perspiration, there may be significant interference with work performance. Other than the finding of hyperhidrosis affecting the palms, perhaps the axilla and the soles, the examination is completely normal. Hyperhidrosis can occur as a result of systemic illnesses, including infection, hypoglycemia, thyroid toxicosis, pheochromocytoma, and carcinoid tumors. If an endocrinopathy is suggested, appropriate laboratory blood tests should be ordered. Lymphomas can manifest with perspiration (typically nocturnal), and chronic infection such as brucellosis and tuberculosis may also manifest with episodic hyperhidrosis. Psychiatric disturbance may also result in severe anxiety associated with perspiration but responds to anxiolytic drugs. Rarely, central nervous system (CNS) disorders such as trauma and syringomyelia may result in hyperhidrosis. It is therefore important to rule out systemic diseases and malignancies before making a diagnosis of idiopathic hyperhidrosis. A good history and clinical exam will rule out the majority of the secondary causes. Hyperhidrosis results from overactivity of eccrine sweat glands, which are innervated by cholinergic fibers, which in turn are under the control of the sympathetic nervous system. Mild cases can be treated with topical agents, such as astringents or antiperspirants. Contact dermatitis may limit the effect of these. Systemic medical therapy with anticholinergic drugs (atropine and propantheline bromide) may be effective but is often not well tolerated because of dry mouth and blurred vision. Medical treatment is therefore usually only partially effective and carries limiting side effects. The most effective treatment, which is permanent, is upper thoracic sympathectomy. This denervates the sweat glands of the upper extremity, whereas preservation of the stellate ganglion prevents Horner syndrome as a complication. Several alternative procedures have been described for upper thoracic sympathectomy. These procedures include transthoracic, supraclavicular, dorsal midline approach plus costotransversectomy, percutaneous radiofrequency sympathectomy, and endoscopic trans-thoracic sympathectomy. The author prefers a modification of the dorsal sympathectomy, which has traditionally been done by costotransversectomy via midline incision and retraction of the paravertebral muscles. The modification consists of a costotransversectomy via a transverse skin incision and dissection through the trapezius, rhomboids, and paravertebral muscle fibers. To perform this procedure, the patient is placed in a prone position. A thoracic spine x-ray is performed prior to surgery to identify and mark the second thoracic (T2) spinous process. As in Fig. 56–1, a transverse skin incision is made at the level of the T2 spinous process and extended ˜4 cm to either side of midline if a bilateral sympathectomy is planned and to one side only if a unilateral procedure has been considered. Beginning 2.5 cm lateral to the T2 spinous process, dissection between muscle fibers is carried down to the transverse process of the third thoracic vertebrae and most medial portion of the third rib (Fig. 56–2). The level is confirmed by a second intraoperative x-ray study. The T3 transverse process is then dissected subperiosteally and removed. The same procedure is done for the third rib underlying the transverse process with preservation of the neurovascular bundle as well as the underlying pleura (Fig. 56–3). The pleura is then easily retracted anteriorly to identify the sympathetic chain, and the second and third sympathetic ganglia can be seen in their paravertebral location. These second and third ganglia can be removed after applying a tantalum clip above the second ganglion. The specimen is submitted to pathology for quick section and confirmation of ganglion within the material before initiating closure. The opposite side is then done, using the similar approach. There is no need to suture muscle fibers or fascia at the end of the procedure, and only the skin is closed. Hospital stay postsurgery is usually 1 day, and a chest tube is not required.
 Case Presentation
Case Presentation
 Diagnosis
Diagnosis
 Characteristic Clinical Presentation
Characteristic Clinical Presentation
 Differential Diagnosis
Differential Diagnosis
 Management Options
Management Options
 Surgical Treatment
Surgical Treatment
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


