Chapter 61 Epidemiology of Sleep Disorders
Abstract
Every day one third or more of the population suffers from some sleep disturbance and/or from abnormal daytime sleepiness. At least 10% of the population suffers from a sleep disorder that is clinically significant and of public health importance. Insomnia is the most common sleep disorder, followed by sleep-disordered breathing and restless legs syndrome. Sleep disorders are interrelated with medical and psychiatric disorders, such as arterial hypertension, cardiovascular and cerebrovascular diseases, morbid obesity, diabetes, metabolic syndrome, and depression. Many gender, socioeconomic, and also ethnic differences exist; and more epidemiologic and genetic epidemiologic studies are needed to understand reasons for these differences. In the 1980s, the large epidemiologic studies on sleep disorders were based on the 1979 sleep disorders classification. In 1990,1 a new International Classification of Sleep Disorders (ICSD) was published. Its revised version from 20052 is now commonly used in sleep medicine. For statistical purposes the International Classification of Diseases, 10th revision (ICD-10) published by the World Health Organization, is commonly used especially in Europe and Asian countries. The Diagnostic and Statistical Manual of Mental Disorders, fourth edition (DSM-IV), published by the American Psychiatric Association, also includes criteria for diagnosing sleep disorders. The DSM-IV criteria have been commonly used especially in studies of insomnia. From the public health and clinical viewpoints, the most important problems related to sleep–wake disorders are insomnia, sleep deprivation, sleep-related breathing disorders, restless legs syndrome, excessive daytime sleepiness, and parasomnias.
Although sleep disorders are very common, rigorous epidemiologic studies in this field are fairly recent, in part because the discipline of sleep medicine is recent. In this chapter we present epidemiologic data important in the practice of sleep medicine. There are several excellent books of epidemiologic methods that are recommended.3–6
Sleep Duration
Sleep duration is highly individual in all age groups, and it is clearly dependent on age. In the United States the relationship between age and the average sleep time is U-shaped, with a minimum 7.9 hours at age 45 to 54 years and a maximum (9.0 hours) at age 75 years or older.7 In addition to sleep disorders (e.g., insomniacs among short sleepers and hypersomniacs among long sleepers), there are also healthy subjects in the extreme groups: a few percent of the populations are so-called natural short sleepers or natural long sleepers (ICSD-2).2,8
Sleep duration can be considered as a lifestyle factor that is modulated by several background factors and by genotype. In a Finnish general-population study the most important and statistically independent determinants of short and long sleep duration were gender, physical tiredness, sleep problems, marital status, main occupation, and physical activity, but these accounted for only 16% of the variance in sleep duration.9 In the United States the largest reciprocal relationship to sleep was found for work time, followed by travel time, and only shorter than average (<7.5 hours) sleepers spent more time socializing, relaxing, and engaging in leisure activities, whereas both short (<5.5 hours) and long (≥ 8.5 hours) sleepers watched more television than average sleepers.7 The same study showed also significant differences in sleep length between weekdays and weekend (longest on Sunday [9.6 hours] and shortest on Friday [8.0 hours]). The effect of genetic aspects has been assessed in large twin cohorts. In the Finnish cohort, representative of the general population, a significant hereditary effect was found on sleep length (overall heritability estimate h2 = 0.44) and sleep quality (h2 = 0.44).10 Similarly, in an Australian cohort, genetic influences accounted for at least 33% of the variance in sleep quality and sleep disturbance.11
There seem to be differences between populations and countries in the mean duration of sleep and trends in them. Among students from 24 countries, sleep was shortest in Japan (6.2 hours in men and 6.1 hours in women), and longest in Bulgaria (7.8 and 8.0 hours, respectively).12 In the United States the self-reported modal of sleep duration has been estimated to be about 8 hours in the 1960s,13 but more recent Gallup surveys have yielded estimates of about 7 hours or even less (National Sleep Foundation, 2005). However, based on reanalysis of all population-based surveys with information on sleep duration (>440,000 persons) in Finland from 1972 to 2005 the mean sleep duration was shortened only 18.3 minutes to about 7.3 hours.9 The same study showed that sleep was shortest and sleep complaints were most frequent among middle-aged employees.
It is possible that changes in society (e.g., “24/7”) and working life (e.g., increase in irregular working hours and stress) have an effect on sleep and contribute to insufficient sleep, leading to fatigue and sleepiness during awake times.14 In Sweden, 12% of adults had persistent and considerable chronic sleep loss. In subjects without sleeping difficulties, the most common cause of insufficient sleep was too little time for sleep.15 In Finland, the prevalence of insufficient sleep, defined as a difference of at least 1 hour between the reported need for sleep and obtained sleep length, was 20.4% (16.2% in men; 23.9% in women). Almost half of those with insufficient sleep continued to have it 9 years later. One third of the liability to chronic insufficient sleep was attributed to genetic influences.16
Sleep duration is associated with different health outcomes. The first report was by Hammond in 1964, in which there was a U-shaped curve between sleep length and risk of mortality, being lowest in those sleeping 7 hours.13 In the early 1980s a U-shaped curve was also found between sleep length and coronary heart disease.17 Later, more than 20 studies have been published on this topic, and the association between sleep length and mortality/morbidity has been confirmed in many of them.18 The increases in risk have mostly been around 12%. There are also two studies with more than one assessment of sleep behavior,19,20 which may be of importance because in the other studies sleep length and sleep quality changed in one third during 6 years.20 The cause(s) and mechanism(s) of the association are poorly understood. Association with short sleep and sleep deprivation may be linked to dysfunction of the restorative function of sleep. Long sleep may be a consequence of a dysfunction/morbidity (e.g., increased levels of cytokines).21,22 Further long-term cohort studies enable better inferences about causal relationships. It is also important to study natural short and natural long sleepers who have had the same sleeping habits since an early age.
Sleep length has also other interesting and important, yet complex associations. In a recent meta-analysis of short sleep and obesity (45 studies with more than 630,000 participants) there was a significantly increased risk both in children (pooled odds ratio [OR] = 1.89) and in adults (OR = 1.55) but the difficulty of causal inference was noted.23 On the other hand, in a clinical review, Marshall and coworkers considered the evidence in adults to be insufficient.24 The association between sleep length and type 2 diabetes has been found in several studies, indicating a 35% to 100% increase in risk for short sleepers25–27 and a 50% to 200% increase for long sleepers.26,27 There is some evidence about an association between sleep length and hypertension: in short sleepers, risks increased from 66%28 to 110%29; and in long sleepers, 19% to 30%28 increases have been reported. However, in some studies no significant association has been observed in elderly persons30 or after adjustment for known risk factors.31 In women, short and long sleep is associated with a 40% increase of risk of coronary heart disease.31,32
Insomnia and Use of Hypnotic Agents
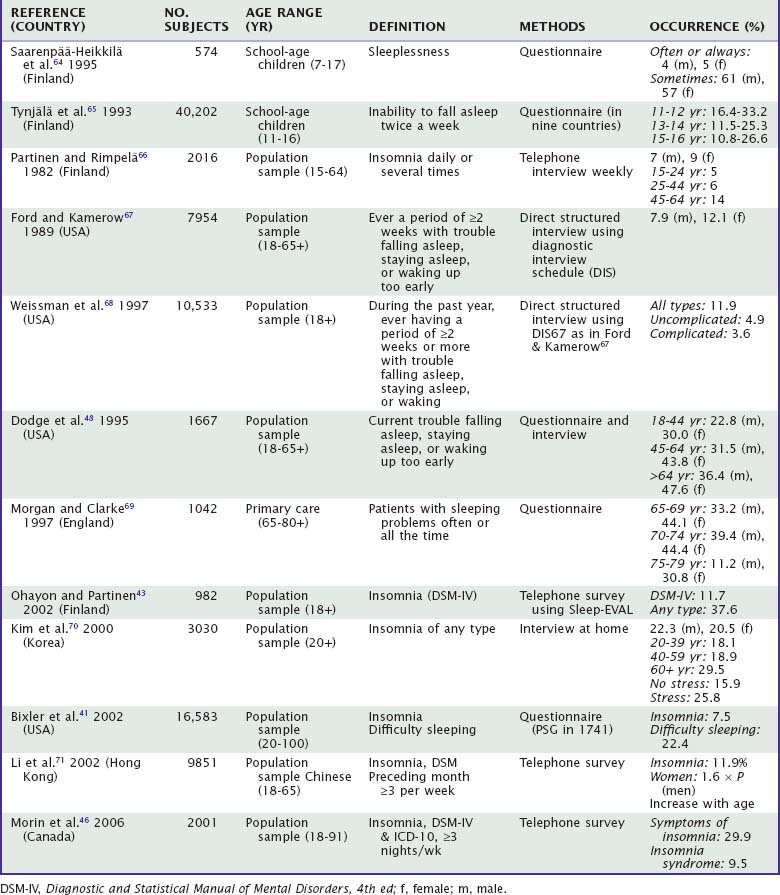
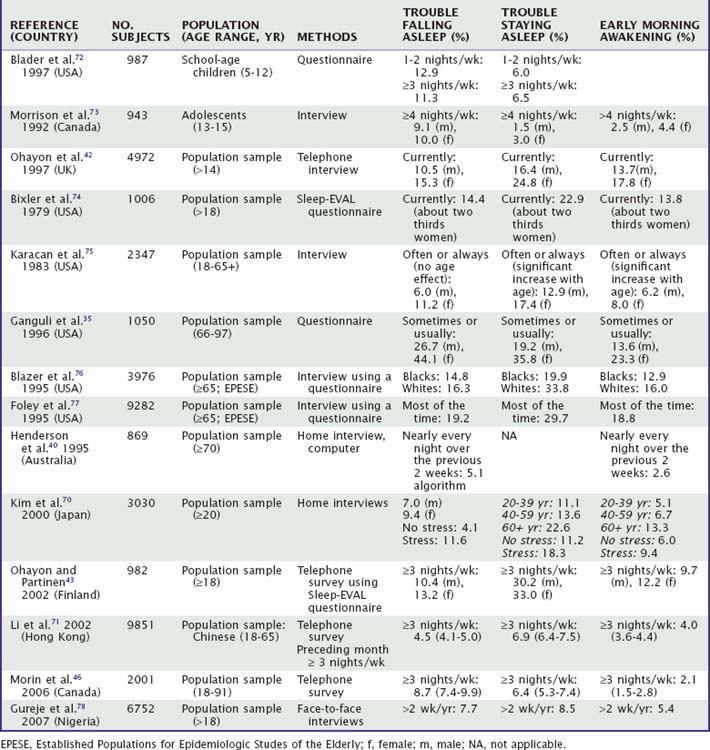
Insomnia is the most common sleep–wake-related complaint, and sleeping pills are among the most commonly prescribed drugs in clinical practice, especially at the primary health care level.32a Based on a large number of published epidemiologic studies we can generalize that the prevalence of symptoms of insomnia is about 30% among adults (Tables 61-1 and 61-2), and the prevalence of specific insomnia disorders varies between 5% and 10%.33,34 Symptoms of insomnia often persist, and earlier occurrence of insomnia increases the probability of insomnia in later life.35,36 There is some evidence that the occurrence of insomnia has increased during the past 30 years.9 Insomnia can be a symptom of an underlying problem with dozens of causes, or it can be a primary disease. Different questionnaires usually contain items about trouble falling asleep, trouble staying asleep, nocturnal awakenings, early morning awakening, and the use of hypnotic agents. The number of urinary voids per night seems to be a good question. People remember easily how many times they wake because of the need to void. Waking up twice to void may not be bothersome. On the contrary, waking up twice or more without the need to void may reflect depression, brain hyperactivity, or some other underlying problem, and frequent (more than two times per night) nocturnal voiding may be a symptom of sleep apnea.37–39
The heterogeneity of the definitions and methods used is striking, but some clear trends can be seen. First, insomnia increases with age. About one third of subjects older than 65 years old have more or less continuous insomnia, although at very old age the levels may be lower. In Australia, insomnia was persistent in 16.2% of the community-dwelling population and 12.2% of the institutional residents. Altogether, 14.5% of the elderly subjects living in the community were using hypnotics regularly while the corresponding percentage was 39.7% among the institutional residents.40 In a large U.S. population–based study,41 the prevalence of insomnia was 7.5% and that of difficulty sleeping was an additional 22.4%. In children and adolescents, the prevalence of frequent insomnia is quite variable; in several studies, it is higher than 10%. In middle-aged populations, the frequency of long-standing insomnia seems to be around 10%. Trouble falling asleep seems to be the most common manifestation in younger age groups, whereas trouble staying asleep is the most frequent form of insomnia in middle-aged and elderly people.9,41–46
Third, seasonal differences, probably due to light exposure, can occur and the results are consistent in Nordic countries. In northern Norway, 41.7% of the women and 29.9% of the men had occasional insomnia.47 As a whole, complaints of insomnia were more common during the dark period of year than during other times of the year. In the Tromsø study, occurrence of insomnia during the midnight sun period (summer insomnia) decreased with age whereas the other seasonal types of insomnia increased with age.47
Fourth, comorbidity is very common. The association of psychiatric disorders, especially depression, with insomnia is well known. Primary insomnia and insomnia related to mental disorders are the two most common insomnia diagnoses listed in the fourth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV).42 Insomnia is a frequent complaint among patients with different respiratory symptoms. In the study of Dodge and coworkers, the prevalence of insomnia was 31.8% to 52.4% among adults with cough, dyspnea, or wheezing; among adults without respiratory symptoms, the prevalence was 25.8% to 26.2%.48 In a World Health Organization collaborative study, 25,916 primary health care attendees were evaluated (Üstün B, Worldwide Project on Sleep and Health; see www-websciences.org). Sleep problems were present in 27% of the patients. Of the patients with insomnia, 51% had a well-defined mental disorder according to the 10th edition of the Internal Classification of Diseases (ICD-10) that mainly included depression or anxiety, alcohol abuse, or both. Use of alcohol and over-the-counter medications to control insomnia is common. Also, somatic and psychological complaints as well as psychological stress are associated with a higher prevalence of insomnia.33,49–51
Fifth, social and occupational factors are important contributors to insomnia. Being unemployed or not married is associated with a higher prevalence of insomnia.14,52,53 In a questionnaire survey of 6268 adults in 40 different occupations, 18.9% of bus drivers complained of having some or very much difficulty falling asleep. Among male executives and male physicians, the respective percentages were 3.7% and 4.9%. Disturbed nocturnal sleep was complained of the most often by male laborers (28.1% waking up at least three times a night) and female housekeepers (26.6%). Disturbed nocturnal sleep was rare among male physicians (1.6%), male executives (7.4%), female head nurses (8.9%), and female social workers (9.4%).54 Symptoms of work-related stress and mental exhaustion are associated with insomnia.46,55–57
Use of Hypnotics
In a nationally representative probability sample survey of noninstitutionalized adults, 3161 people 18 to 79 years old were surveyed.58 Insomnia afflicted 35% of all adults during the course of 1 year. During the year before the survey, 2.6% of adults had used a medically prescribed hypnotic agent; 0.3% of all adults and 11% of all users of hypnotic agents reported using the medication regularly for 1 year or longer. When anxiolytic and antidepressant agents were excluded, 4.3% of adults had used a medically prescribed hypnotic for sleep and 3.1% had used an over-the-counter sleeping pill. In a reanalysis of several studies published in Finland between 1972-2005 (251,083 subjects) the prevalence figures concerning the use of sleeping medicine at least once a week among adult population did not show any clear trend of increase; the figures varied between 4% and 6% from 1982 to 2002.9
In Sweden, 10,216 members of the Swedish Pensioners’ Association were surveyed.59 Hypnotic agents were used by 13.5% of the men and 22.3% of the women. Of the men aged younger than 70 years, 7.9% were receiving such treatment; of those 70 to 80 years old, 14.4% were using hypnotic agents; and of those 80 years old or older, 21.8% were taking hypnotic agents (P < .0001). The corresponding frequencies among women were 15.0%, 23.0%, and 34.9%, respectively (P < .0001). Hypnotic agents are used by many institutionalized elderly subjects even without insomnia. This raises an ethical question because the chronic use of hypnotic agents is associated with excessive mortality rates.60 In a excellent meta-analytic study of risks and benefits of hypnotics among elderly persons the number needed to treat for improved sleep quality was 13 and the number needed to harm for any adverse event was 6.61
An excellent way of tracking the use of hypnotic medication of the population is to count unit defined daily doses (DDD) from the sales statistics. When one knows the assumed average dose per day for each drug, sales per year, and population of the country, one can calculate DDD per 1000 inhabitants per day. In Finland, for all hypnotic agents, the rate in 1994 was 38 DDD/1000 inhabitants/day. In 2002 the rate had increased to 53.4 DDD/1000 inhabitants/day. Since that time the use of hypnotics has remained about the same. In 2007 the rate was 53.8 DDD/1000 inhabitants/day.62 Benzodiazepines are available in all Scandinavian countries, and in 2001 the consumption of benzodiazepines (in DDD/1000 inhabitants/day) was 14.9 in Denmark, 21.5 in Finland, 20.8 in Iceland, 13.1 in Norway, and 11.7 in Sweden.63 Respectively, the consumption of cyclopyrrolones was 17.7 in Denmark, 29.5 in Finland, 34.5 in Iceland, 20.9 in Norway, and 24.3 in Sweden.63
Circadian Rhythms and Their Disorders
Morningness/eveningness or “chronotype” is dependent on genetic, environmental, and age-related factors. Using the Munich ChronoType Questionnaire in more than 55,000 persons, it has been found that the most frequent (about 15%) type has midsleep on free days at 4:14 AM and about 35% earlier and 50% later.79 (Midsleep is the halfway point between sleep onset and sleep end.) Women reach their maximum in lateness at around 19.5 years and men at 21 years, and this sex difference disappears around the age of 50; and people older than 60 years of age, on average, become even earlier chronotypes than they were as children.79 In a Finnish population, morning type increased from 16% among 25- to 29-year olds to about 50% among those 65 years and older.80 Respectively, evening type was observed in 11% to 12% among 25- to 29-year olds and the minimum (6%-7%) was found among 55- to 59-year olds. The estimate for overall genetic effect was 49.7%.80
Studies on the prevalences of circadian rhythm sleep disorders are scarce. Delayed sleep phase syndrome has been found in 0.17% among Norwegians aged 18 to 67 years81 and in 0.13% among Japanese aged 15 to 54 years,82 and the number of cases seems to have increased in the past few decades,83 being about 1.66% in Japanese university students.84 In Europeans aged 15 to 18 years a circadian rhythm disorder was found in fewer than 0.5%.85 One study has suggested that the prevalence of shift-work sleep disorder is about 10%.86
Excessive Sleepiness and Hypersomnia
The feeling of not being alert is common, occurring both as a physiologic everyday phenomenon and as a symptom of sleep disorders.1,2 In spoken language, this feeling is probably most often called sleepiness but the actual meaning varies. By definition, sleepiness implies an increased risk of falling asleep,2 but the complaint of sleepiness is sometimes used to describe physical tiredness, fatigue, and loss of mental alertness without an increase in sleep behavior—conditions often associated with a decreased ability to fall asleep, contrary to true sleepiness. Abnormal sleepiness is often called excessive daytime sleepiness (EDS), but also this condition is difficult to be defined, because falling easily asleep or inability to stay awake may be normal and a desired everyday phenomenon (e.g., in the evening when going to bed). EDS has also been labeled as a disease or a disorder, although it is a symptom of a sleep disorder or of another disease.
Our own studies exemplify these problems.87 Among those reporting daytime sleepiness every or almost every day, 19.5% of women and 42.3% of men were frequent snorers (snoring on at least 3 nights per week), 25% had scores suggesting moderate to severe depression, 25% had insomnia at least every other day, 10% were regular hypnotic or tranquilizer users, and 10% reported insufficient sleep. Thus, a “tired” or “sleepy” (in the patient’s words) person may have insomnia and not EDS or hypersomnia. In practice, it must be remembered that descriptions of the symptoms are related to the person’s feelings, emotions, level of education, and cultural background. Sleep researchers usually talk about sleepiness when referring to poor vigilance, lack of alertness, and tendency to fall asleep, but traffic researchers often use the terms, fatigue or drowsiness.88 Sleeping alleviates sleepiness at least temporarily whereas resting without sleep does not. Fatigue, on the contrary, may be alleviated by having a pause, resting, physical exercise, and management of stress. Chronic fatigue is usually multifactorial in etiology, and it is generally not relieved by usual restorative techniques.88 Fatigue (57%), tiredness (61%), and lack of energy (62%) may be more frequent complaints than sleepiness (47%) in patients with sleep apnea.89 Also in primary care, complaints of chronic fatigue may be more common (20%-25%) than complaints of excessive sleepiness (5%-15%).90,91
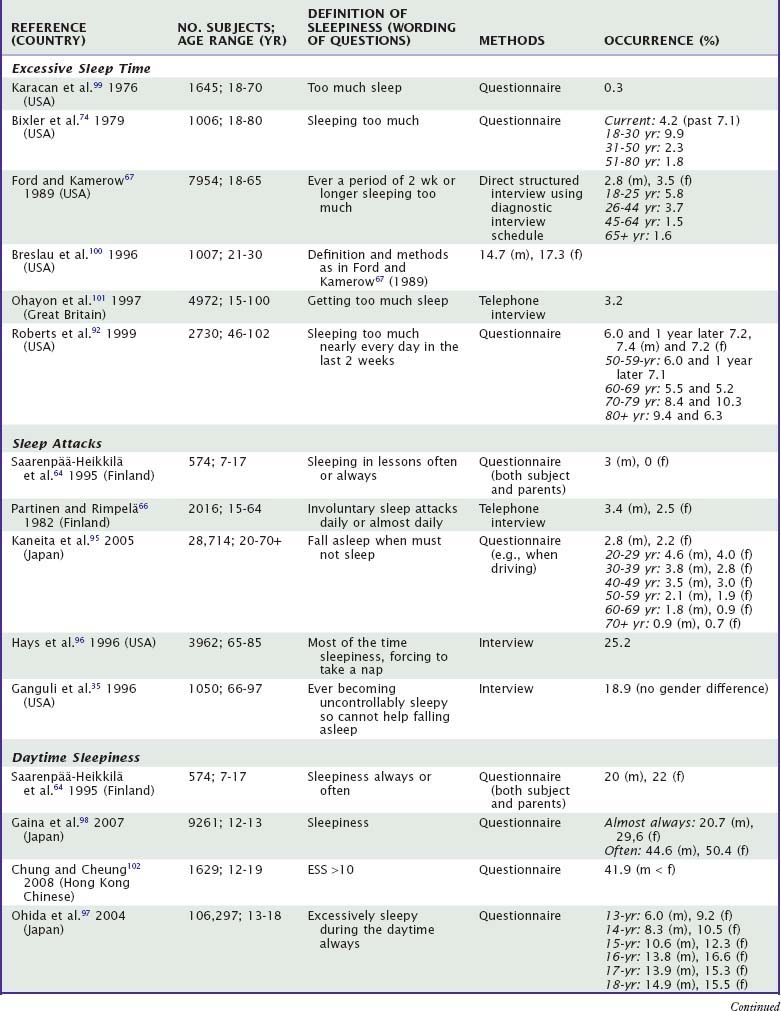
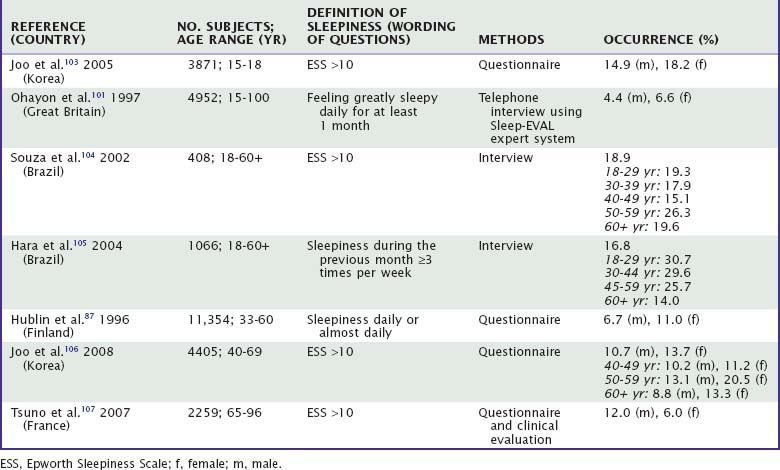
Table 61-3 provides a summary of studies on daytime sleepiness.35,64,66,67,74,87,92,95–107 Depending on the wording, there is approximately a 100-fold difference in occurrence, ranging from 0.3% to more than 30%, and in most of the studies the range is from 5% to 15%. The prevalences of excessive sleep time or hypersomnia-like states are mostly around 5% in adults (no studies on children), with no clear gender difference. The prevalence may be age dependent, although the results are conflicting (decreases67,74 or increases92,93). In the classic study by Ford and Kamerow,67 64% of hypersomniacs had a psychiatric disorder in two interviews with a 1-year interval, most commonly an anxiety disorder or major depression. Similar findings are reported from many European countries.94 Studies with two assessments of excessive sleep have shown stability of the symptom in less than one third.92 Sleep attacks (involuntary sleep episodes during awake periods) also mostly seem to occur in a few percent of the population in all age-groups, with no clear difference between the sexes and with conflicting results as to age-dependence (decreases95 or increases35,96 with age). Frequent or excessive (subjective) daytime sleepiness occurs in 10% to 15%. It occurs more often in school-aged children (with large differences between studies in the same country97,98) or young adults than in middle-aged or older adults. In most studies, sleepiness is more prevalent among women than among men.
Narcolepsy and Narcolepsy-Like Symptoms
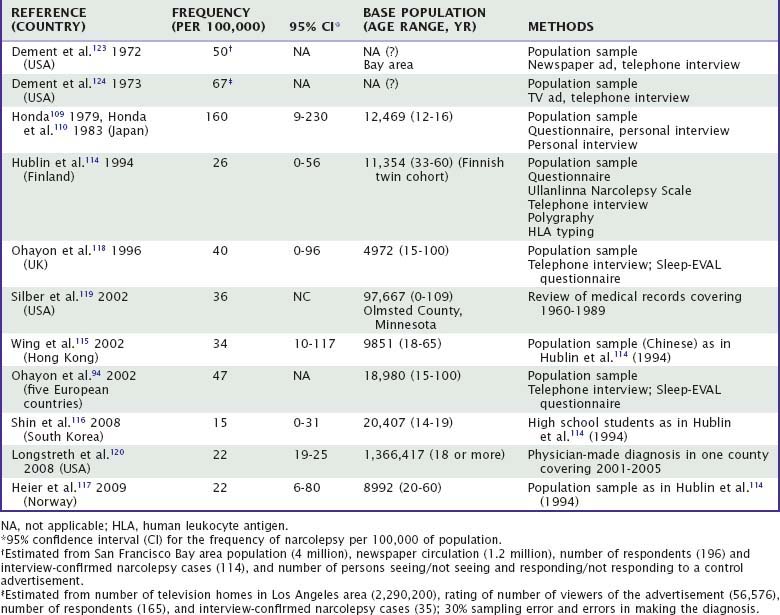
There are about 30 studies published on the prevalence on narcolepsy (most of them on narcolepsy-cataplexy) with considerable differences in the figures. Highest prevalences (up to 30%) are based on questionnaire data without follow-up testing, and the next highest (0.2%-0.8%) on studies with self-reported diagnosis.108 In most studies with more intensive screening or clinical evaluation of suspected narcoleptics the prevalence of narcolepsy-cataplexy falls between 0.025% and 0.05%, or 25 to 50 per 100,000 population, and the 95% confidence intervals (CIs) for the frequencies overlap in the majority of them (Table 61-4). There are some exceptions. The highest figures are from Japan109,110 based on interviews of symptomatic school-aged children selected by questionnaire, giving “a suspect of narcolepsy” in 160 per 100,000 and a surprisingly high prevalence (7.6%) of “interview-confirmed cataplectic attacks,” which suggests criteria different from other studies. The lowest frequency (0.23 per 100,000) is found among Israeli Jews,111 but this was based on an extrapolation of sleep clinic samples to the entire population. However, narcolepsy is likely hugely underdiagnosed.111a
The prevalence of narcolepsy-cataplexy seems to be consistent despite considerable differences methods, ethnic groups, and population frequencies of DQB1*0602, and so on between the studies.112 For example, there are three studies using a simple screening method called the Ullanlinna Narcolepsy Scale (UNS) developed and validated for population studies.113 It consists of 11 items assessing cataplexy-like symptoms and the tendency to fall asleep. Using the UNS, telephone interviews, and polygraphic confirmation of the diagnosis, the prevalence of narcolepsy with clinically significant cataplexy has been found to be of same order among adult Finns (26 per 100,000),114 adult Chinese in Hong Kong (34 per 100,000),115 Korean adolescents (15 per 100,000),116 and adult Norwegians (22 per 100,000).117 Similar prevalences have been obtained in Europeans using telephone interviews (Sleep-EVAL questionnaire) without any other examinations (40 or 47 per 100,000)94,118 and in the United States using a review of medical records (36 per 100,000)119 and physician-made diagnoses (22 per 100,000).120
There are only a couple of studies on narcolepsy without cataplexy, giving a prevalence of 20 per 100,000 in adults in the United States119 and 34 per 100,000 in Korean adolescents,116 which may be gross underestimations.112 However, it can be difficult to assess the true prevalence because diagnostic Multiple Sleep Latency Test criteria may be 100 times more prevalent in a population than narcolepsy.121 One study gives an incidence rate of 1.37 (0.74 for narcolepsy with cataplexy) per 100,000 persons per year. Some studies suggest that narcolepsy may be slightly more common in men.108 Analytic epidemiologic studies have found associations between narcolepsy and body mass index (BMI), immune responses, and stressful life events, but these may rather reflect consequences than cause of disease.108
Although typical cataplexy is pathognomonic of narcolepsy, mild forms are difficult to separate from similar physiologic phenomena. As mentioned, reports of EDS in the population are common. In Finland, 29.3% of the people reported (at least once during his or her lifetime) feelings of limb weakness associated with emotions.114 If this is considered as evidence of cataplexy and combined with the occurrence of daytime sleep episodes at least 3 days per week, 6.5% of the population would have fulfilled the minimal diagnostic criteria for narcolepsy of the International Classification of Sleep Disorders.114,122 Therefore, using only questionnaires in population studies may increase the risk of too high prevalence rates.
Snoring, Sleep-Disordered Breathing, and Sleep Apnea Syndrome
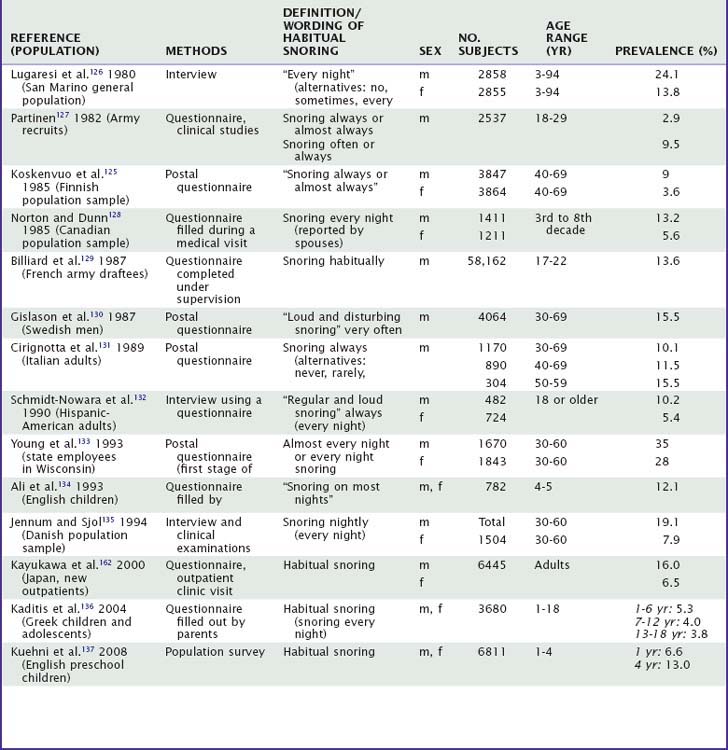
Habitual snoring is defined as snoring almost every night or every night or as snoring at least 5 nights per week. It is almost always present in patients with obstructive sleep apnea syndrome (OSAS). In the first large-scale epidemiologic study on snoring, about 24% of San Marino men and 14% of San Marino women were reported to habitually snore (Table 61-5125–137). In Finland, 9% of adult men and 3.6% of adult women snore always or almost always when asleep.125
A Syndrome or a Disease?
According to various cross-sectional studies, the lowest rates for the prevalence of OSAS among adult men are 1% to 4%. There is an age relationship, so the prevalence of OSAS among men 40 to 59 years old may be greater than 4% or 8%.133 OSAS is less common is younger and older age groups. After menopause, up to the age of 65, OSAS is almost as common among women as among men.
Obstructive sleep apneas are part of the complex of heavy snorer’s disease as defined by Lugaresi and colleagues.138 Heavy snoring (i.e., partial upper airway obstruction), even without apneas, is associated with higher pulmonary arterial pressure, daytime sleepiness, arterial hypertension, and insulin resistance.139–143 Heavy snoring is also associated with case-fatality and short-term mortality after a first acute myocardial infarction.144
Visceral central body obesity, measured by waist circumference, is strongly related to SBD.145 Among morbidly obese patients the proper diagnosis may be morbid obesity with obstructive sleep apnea.146 Another example is acromegaly with symptomatic sleep apnea. This is analogous to a patient with a brain tumor who has symptomatic epilepsy. The primary diagnosis is brain tumor (e.g., glioma), and epilepsy is a secondary symptom caused by the brain tumor.
The severity of sleep apnea must be properly quantified, not only by indices (e.g., apnea index [AI], apnea-hypopnea index [AHI], or respiratory disturbance index [RDI]) but also by the number of oxygen desaturations, presence of cardiovascular effects, and degree of daytime sleepiness. Snoring and sleep apnea are more common in the supine sleeping position than in the lateral positions. It is therefore necessary to give indices separately for supine and lateral sleeping positions. In clinical studies, sequential apnea indices should always be compared relative to sleeping position. The diagnostic criteria should also be adjusted for age. Bixler and associates147 studied 20- to 100-year-old men. The criteria for OSAS were an AHI of at least 10 in the sleep laboratory and fulfillment of clinical criteria, including the presence of daytime symptoms. OSAS was found in 3.3% of the sample, with its maximum among 45- to 64-year-old men. Although the prevalence of sleep apnea increases with age the clinical impact of apnea seems to decrease among elderly people.148–150
Prevalence of Sleep Apnea
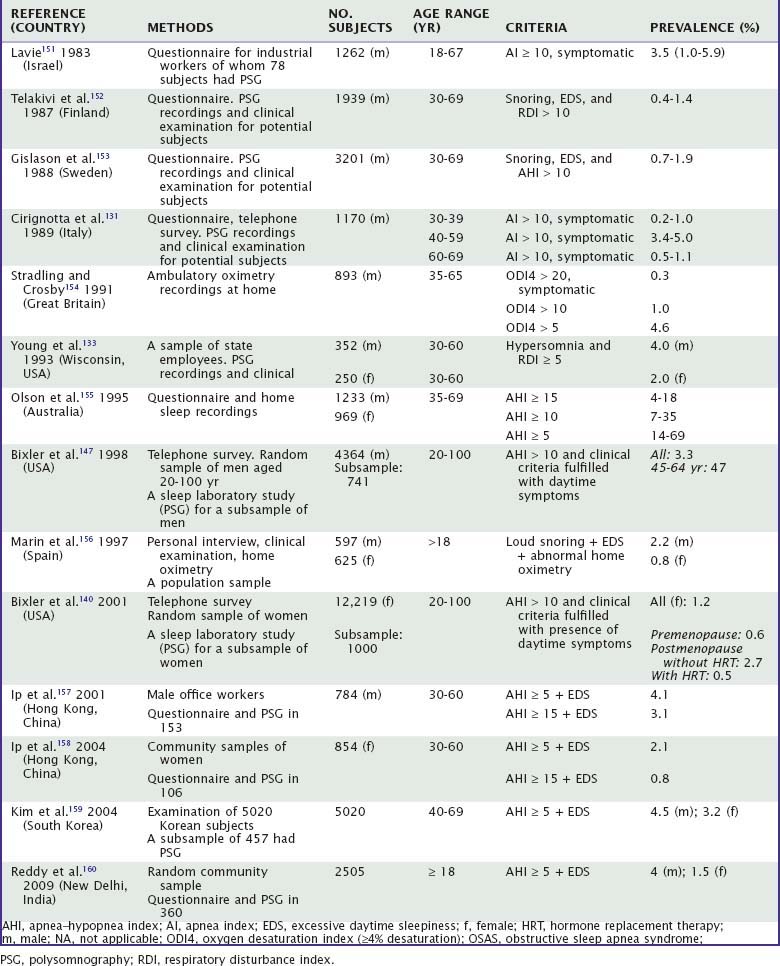
The first large epidemiologic polysomnographic study was conducted in Madison, Wisconsin.133 The authors estimated that 2% of women and 4% of men in the middle-aged work force met the minimal diagnostic criteria for the sleep apnea syndrome, defined as an AHI of 5 and daytime hypersomnolence.133 Up to 9% of women and 24% of men had an AHI of 5 without daytime somnolence. On examination of the subgroup of patients between the ages of 50 and 60, 4% of women and 9.1% of men were found to have an AHI exceeding 15.133 In a large U.S. population–based study,140,147 clinically defined sleep apnea (AHI ≥ 10 and daytime symptoms) occurred in 3.9% of men and 1.2% of women. The peak prevalence, 4.7% (95% CI, 3.1% to 7.1%), was found among men aged 45 to 64 years. Among the 20- to 44-year olds and those older than 65 years, the prevalence rate was 1.7%. Among women, the average prevalence was 1.2.140,147
In women, the prevalence of SDB increases after menopause; hormone replacement therapy is associated with lower occurrence of SDB.140,161 In the study by Bixler and coworkers.140 the prevalence of clinically defined sleep apnea among premenopausal women was 0.6%. Among postmenopausal women on hormone replacement therapy the prevalence was about the same (0.5%).140
Role of Obesity as a Risk Factor for Snoring and Sleep Apnea
Obesity is the most important risk factor for snoring and sleep apnea. The association is found without exceptions, which does not, naturally, mean that lean people could not have OSAS. Neck size162 and especially waist circumference145,163 are related to severity of sleep apnea and may be better indicators than BMI.
Other Risk Factors for Snoring and Sleep Apnea
Alcohol increases upper airway resistance and tends to induce obstructive sleep apnea in healthy people and especially among chronic snorers. In Great Britain, one drink per day increased the odds of mild or worse SDB by 25% (OR = 1.25; 95% CI, 1.07-1.46) among men. Among women, minimal to moderate alcohol consumption was not significantly associated with increased risk of SDB.164 Other risk factors include large adenoids or tonsils, rhinitis, and other abnormalities in the upper airways, such as those found in different syndromes of dysmorphia and in the mentally disabled. Also, smoking,165 acromegaly,166,167 and amyloidosis168 are known risk factors for SDB. Organic solvent use was associated with increased prevalence of SDB in Sweden169 but not in Germany.170
Snoring and Sleep Apnea in Children
Habitual snoring and sleep apnea during childhood (see Tables 61-5 and 61-6125–137,140,147,151–160) may be associated with significant harmful effects on health. Childhood obesity and adenotonsillar hypertrophy are among the most common associated factors.171 In an Italian study, 118 (7.3%) of 1615 children 6 to 13 years of age were often snorers.172 Children with rhinitis were more than twice as likely to be habitual snorers than others. A positive correlation between parental smoking and snoring in children exists. In Singapore, 6% of children snore habitually.173 In Iceland,174 the minimal prevalence of obstructive sleep apnea among children 6 months to 6 years old was 3.2%. In another study, significant sleep and breathing disorders occurred in 0.7% of 4- to 5-year olds.134 The prevalence of SBD among adolescents aged 12 to 16 years was similar to that reported for younger children. In Greece, a survey of 3680 people aged 1 to 18 years revealed a prevalence of habitual (every night) snoring of 5.3%, 4%, and 3.8% among 1- to 6-, 7- to 12-, and 13- to 18-year-old subjects, respectively.136 Sleepiness at school was more common in habitual snorers than in nonhabitual snorers (4.6 vs. 2%, P = .03). Based on 70 random polysomnographic recordings among the 307 snorers without adenoidectomy and/or tonsillectomy the estimated prevalence of OSAS was 4.3%. In a population survey of 6811 children aged 1 to 4 years in the United Kingdom (from parent’s reports) the prevalence of habitual snoring was 7.9%, and 0.9% of children were reported to have habitual snoring and sleep disturbance. Habitual snoring increased with age from 6.6% in 1-year olds to 13.0% in 4-year olds. Habitual snoring was associated with parent’s smoking, road traffic, single parenthood, white but not South Asian children, and socioeconomic deprivation.137 Atopy and respiratory infections were strongly associated with snoring, but BMI was not,137 which shows that the association between childhood obesity and SBD is not simple.175
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree