Figure 75-1 The report sheet that was completed by investigators.
Participating physicians had been asked before and at the study not to discuss the approaches and criteria they planned on using or were using to diagnose DSPN.
CHOICE OF PATIENTS
Twenty-four patients were recruited from the Rochester Diabetic Neuropathy Study (RDNS), a cross-sectional and longitudinal study of patients with DM, living in Olmsted County, MN mainly of northern European extraction.9 In an attempt to recruit a representative sample of patients with and without varying severities of DSPN, we calculated the normal deviate scores of E 5 NC nds at the last evaluation of all active participants in the RDNS and arranged values from lowest to highest. We then recruited for this study the first five volunteers with the lowest scores (presumably without DSPN), the five with the highest scores (presumably with severe DSPN), the first seven volunteers below the 92.5th percentile, and the first seven above the 97.5th percentile. The intent was to obtain a bell-sloped frequency distribution with approximately one half of patients not having DSPN and one half having DSPN—the approximate distribution of DSPN by nerve conduction criteria in the RDNS. The actual distribution of values, from NC obtained at the time of the study, were presumably somewhat different from the earlier values obtained in the RDNS. The 12 investigators were not told how patients had been selected.
MASKING OF PATIENTS
To test for reproducibility of the clinical examinations, it was necessary that the patients’ identity be hidden from examiners at least for one of the examining days. To do this, for the first clinical examination, all patients were dressed in surgical clothes and wore caps, masks, and dark glasses (Fig. 75-2). Also on this occasion, their voices were distorted by a special microphone and electronic chip to distort the voice heard through earphones by examiners. Patients were asked not to respond to an examiner’s questions unless he or she wore earphones. The patient’s age and gender were provided on a lapel tag. On the second day, patients wore street clothes, were placed in different cubicles, again by random selection, and appearance and voices were not disguised. We also asked physicians to note on the form whether they had recognized any patient from the preceding day’s examination. Patients had been instructed not to provide any identifying information and not to volunteer information which would allow recognition of who they were. Finally, at second evaluation, physicians were asked if they recognized the patient. If they did, was it from voice, physical appearance, examination, or symptoms?
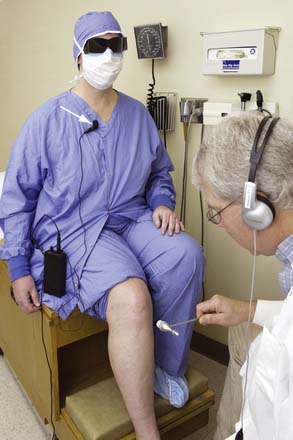
Figure 75-2 This photograph of a participant in the study illustrates the approach used at first examination to obscure recognition of subjects. Surgical clothing, a mask, and dark glasses were worn by all patients at first examination. The voice of the patient picked up by a microphone (arrow) was altered electronically and heard through earphones by the examiner. The subject is told not to speak unless the physician wears the earphones. At second examination, the patient wears street clothes and the voice is not altered.
(Used with permission from Muscle and Nerve, in press)
GOLD STANDARD CLINICAL AND CLINICAL NEUROPHYSIOLOGIC TESTS
An international panel of experts (a few also participating in clinical examination of patients) had been canvassed earlier to establish the percentage of expert opinions evaluating a given patient in study which would be accepted as unequivocal evidence of DSPN, that is, 5%, 25%, 50%, 75%, or 95%. The panel chose 75% (Ex Neur Dx ≥ 75%). Using this criterion, it was anticipated that a variable number of patients would be normal or abnormal at both examinations, but others would be diagnosed with and without DSPN on the two occasions. To break the tie, a second rule was needed. For this purpose, the number of physicians who had diagnosed DSPN on days 1 and 2 were summed, and if this number was 18 or greater (i.e., ≥ 75%), the patient was declared as having DSPN.
Within 2 weeks of the clinical examinations (before or after) patients had two separate evaluations of NCs, QSTs, HRdb, and QSART of the foot (and also of the leg in the case of QSART) by standard approaches described later. For all four clinical neurophysiologic tests, different personnel and instruments were used.
Five attributes of NC (peroneal motor amplitude, velocity and distal latency, tibial motor distal latency, and sural nerve amplitude) were assessed so as to be able to estimate E 5 NC nds.10 Each attribute for a given patient was expressed as a normal deviate from percentiles corrected for applicable variables and was expressed with all abnormalities shown in the upper tail of the normal distribution. Because conduction velocity and latency cannot be estimated when amplitude is 0 (a real value), the summed value of nds is divided by the number of measurable attributes and this value is multiplied by 5 to extrapolate results to five attributes.
For 3 QST nds, vibration and cooling threshold expressed as nds from percentiles corrected for applicable variability and an intermediate pain intensity threshold value (HP 5) were summed, divided by the number of measurable values, and multiplied by 3. The percentile value of this composite score was calculated from values obtained in the RDNS healthy subject cohort.11,12
The HRdb and QSART values of patients also were expressed as normal deviates from percentiles corrected for applicable variables.13,14
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








