1. Typical history and examination according to International Headache Society criteria
2. Pain has at least four of the following characteristics:
2a. Distribution along one or more divisions of the trigeminal nerve
2b. Sudden, intense, sharp, superficial, stabbing in quality
2c. Intensity severe
2d. Precipitation from trigger areas
2e. Between paroxysms history and examination
3. No neurological deficit
4. Attacks are stereotyped in the individual patient
5. Exclusion of other causes of facial pain by history, examination or special investigations
An imaging study of the brain should be performed early in the course of management. Not only the aforementioned causes of TN but particularly compression of the trigeminal nerve by blood vessels can be demonstrated by magnetic resonance imaging (MRI; Fig. 38.1). The high sensitivity of MRI for the detection of vascular compression is 88.5 % and the low specificity is 50 % [15] elucidates the fact that typical TN is correlated in most cases with vascular compression. In contrast to that fact, neuralgia does not necessary follow from a contact of a vessel to the trigeminal nerve root. There are clearly other causes (e.g. demyelination) underlying the development of neuralgia. In conclusion, decision making to operate upon a patient with typical TN relates to criteria that are summarised in Table 38.2.


Fig. 38.1
A 44-year-old woman suffering from trigeminal neuralgia (TN) of the right third branch for 7 years. Parasagittal magnetic resonance imaging (MRI) along the course of the trigeminal nerve, constructive interference in steady-state (T2 subgroup) protocol with high resolution (0.7 mm). It can be seen an aberrant loop of the superior cerebellar artery (A) is compressing the trigeminal nerve (B) from above (that means that the nerve fibres of the third branch are affected!) within a few millimetres of the entry into the pons (MRI protocol developed and performed by Dr. Papke, Department of Neuroradiology, University of Münster, Germany)
Table 38.2
Indications for neurovascular decompression surgery in patients suffering from trigeminal neuralgia
1. Attacks of facial pain that last a few seconds to less than 2 min |
2. No other pain complaint as a sign of somatisation of chronic pain disease |
3. Exclusion of morphologic abnormalities along the course of the trigeminal nerve by MRI |
4. Vascular compression of the trigeminal nerve (facultative criterion) |
5. Exclusion criterion is not age, but bad ASA classification |
38.5 Treatment
The operation is performed with the patient supine and the head turned to the contralateral side (if preoperative evaluation of the cervical spine by x-ray reveals degenerative lesions or preoperative probe positioning provokes neurological deficits, we select the semisitting position for the procedure). The head is held by a Mayfield three-point head holder. The chin is flexed somewhat forward and the vertex is tilted towards the floor to maximise the working space between the retromastoid space and the shoulder, which is drawn towards the foot and to the floor by tape (care must be taken not to stretch the brachial plexus!). Electrodes necessary for the intraoperative monitoring of auditory evoked potentials and facial stimulation are attached to the patient. Hair is shaved only ipsilaterally in the retromastoid region.
After preparing and draping of the operative area, a skin incision is made behind the hairline along the mastoid crease. Michel clips are applied to the skin edges and the underlying fascial and muscular layers are dissected along the same line. The soft tissue is stripped from the bone and held aside with retractors. The craniectomy is placed high and lateral in the posterior fossa. The superior and lateral edges of the bony opening expose the inferior margin of the transverse sinus and the medial margin of the upper sigmoid sinus. The craniectomy measures 3 cm in craniocaudal and mediolateral length. Mastoid cells that have been opened are sealed with muscle pieces bonded by tissue glue at the end of the operation. Before the dura mater is opened, the patient is given mannitol intravenously.
After the microscope is brought into field, a dura incision is made along the margin of the transverse and sigmoid sinus. If the edge of sinus is incised, a piece of Gelfoam will staunch the bleeding without interfering with venous flow in the sinus. A cottonoid is placed superficially supralaterally over the cerebellum. A first look should now be made in the posterolateral direction as there can be bridging veins in this area, and these are difficult to treat if they are torn. If the cerebellum is “full”, rather than approaching rostrally, one should lift the cerebellum off the occipital plate and the subarachnoid cistern around the nerves IX and X to allow cerebrospinal fluid to escape. As a consequence, the cerebellum will lower by gravity. Now the self-retaining retractor can be slid over the cottonoid towards the petrous bone.
The superior petrosal vein is encountered at or near the anteromedial end of the line of attachment of the tentorium to the petrous ridge. This vein must usually be coagulated to permit adequate visualisation of the trigeminal nerve. Sometimes, just one branch must be taken. The eighth nerve is identified, and the fifth nerve appears deeply anterior and rostral to it.
Now the surgeon looks for vascular compression. The general rule is that rostral compression of the nerve causes lower facial TN, caudal compression causes neuralgia of the first branch, and lateral or medial compression causes second branch neuralgia. Frequently, the superior cerebellar artery loops down anteromedial to the nerve (Fig. 38.2a). The main trunk can be brought up and mobilised away from the nerve (Fig. 38.2b, c). A piece of muscle is inserted between the nerve and the artery and bonded in place with tissue glue (Fig. 38.3). If there is a compression by a small vein, it can be coagulated and divided. Simple coagulation should be avoided because of the danger of recanalisation. Larger veins should be decompressed by means of muscle implants. Sometimes the artery is adherent to the nerve; sharp dissection may then be necessary. Before closure, multiple Valsalva manoeuvres are performed after the retractor has been removed for detecting and servicing lesioned and bleeding veins.
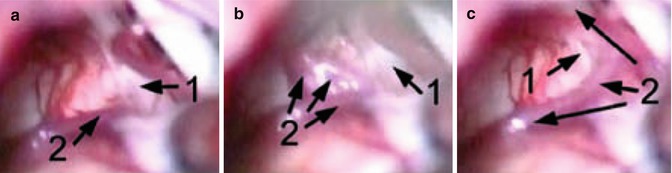
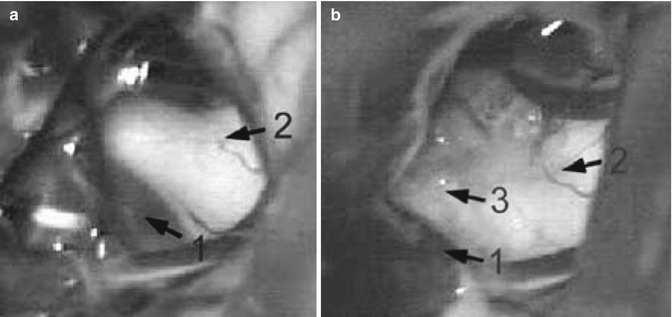

Fig. 38.2
Intraoperative microphotographs showing right trigeminal nerve (1) which is compressed by superior cerebellar artery (2). (a) The caudal loop of the superior cerebellar artery is behind the trigeminal nerve on its anteromedial edge. (b) The main trunk has been brought up from behind the nerve to its cranial border. (c) The artery is mobilised from the nerve and located on its lateral aspect

Fig. 38.3
Intraoperative microphotographs showing the right trigeminal nerve (2), which is compressed by superior cerebellar artery (1). (a) The caudal loop of the superior cerebellar artery is at the superior aspect of the trigeminal nerve. (b) A piece of muscle (3) has been inserted between the artery (1) and the nerve (2)
The cerebellopontine angle is filled with a warm-water irrigation solution. Afterwards, the dura is closed in a watertight fashion with the aid of an operating microscope, which is subsequently removed. Open mastoid cells are closed with muscle pieces bonded by tissue glue. To fill the bony defect, the epidural space is filled with absorbable gelatine sponge. Muscles, fascia and subcutaneous tissue are closed in layers with interrupted sutures. The skin is closed with single stitches according to Donati, using 3-0 nylon sutures.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








