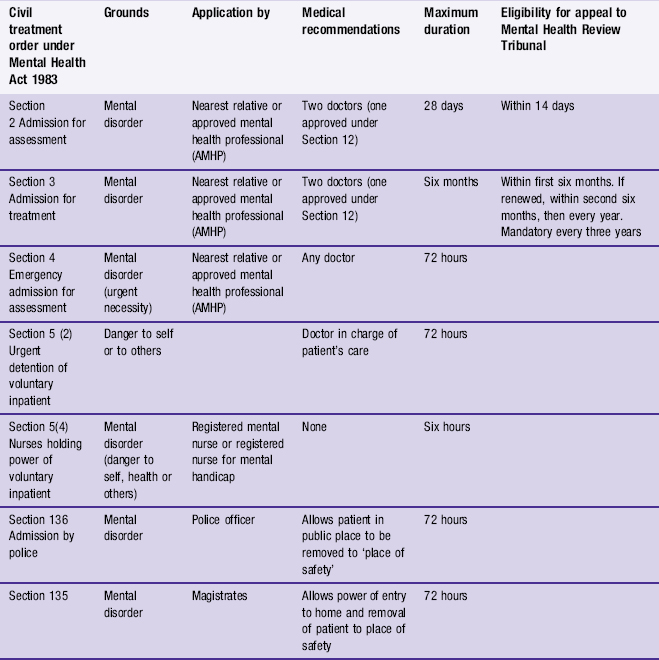
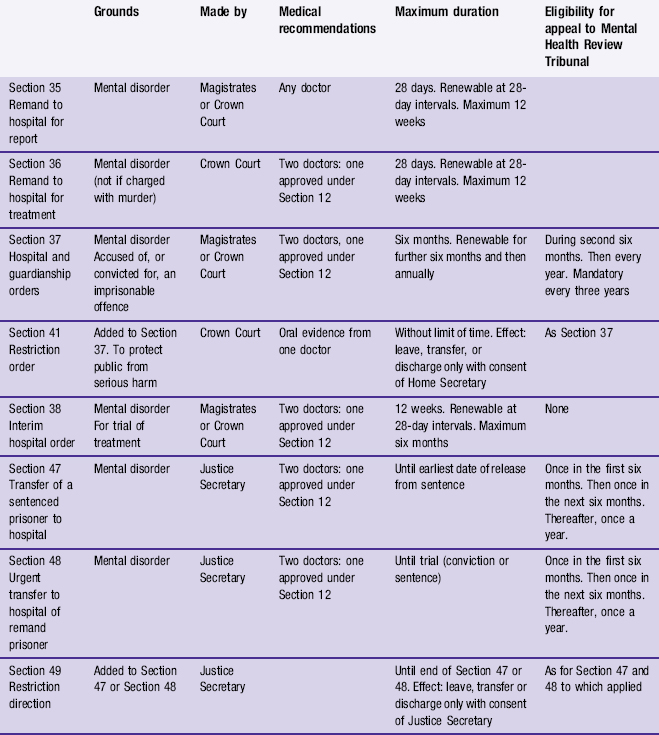
22 Mental health legislation
Definition of mental disorder
Mental Health Review Tribunals (MHRT)
• Independent bodies consisting of doctor, lawyer and lay person whose responsibility is to consider the justification for continued detention under the 1983 Mental Health Act.
• Patients are allowed legal aid to assist in representation, e.g. private psychiatric reports can be commissioned.
• Can order discharge or delayed discharge, and recommend (not order) transfer to another hospital or leave of absence.
• Can also order discharge or conditional discharge (i.e. with conditions such as place of residence) or deferred conditional discharge of a Section 41 restricted patient.
Care Quality Commission (Previously Mental Health Act Commission)
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree