14 Other disorders associated with neurological conditions
fatigue, sleep disorders, incontinence and sexual dysfunction
At the end of this chapter, you should be able to:
1. demonstrate an understanding of the prevalence and impact of a range of problems on the lives of people with neurological conditions, i.e. sleep disorders, fatigue, dysphagia, incontinence and sexual dysfunction
2. describe typical alterations in patterns of sleep and fatigue in people with neurological conditions compared to healthy people, and discuss the impact fatigue may have on quality of life
3. explain the physiological processes underlying normal continence function, and discuss which treatments may be available for incontinence in people with neurological conditions
4. explain the physiological processes underlying normal sexual function, and describe some common forms of sexual dysfunction that may result from a neurological condition
5. discuss the potential impact that sexual dysfunction may have on relationships and discuss which treatments may be available for people with a neurological condition.
Sleep and fatigue
Patterns of sleep
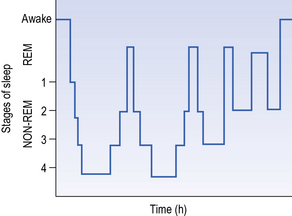
Once we have fallen asleep, if we sleep for long enough, our level of consciousness varies and we alternate between two distinct types of sleep: REM (rapid eye movement) sleep and non-REM sleep (see Fig. 14.1). The two types of sleep pattern are easily distinguishable, one from the other, by their distinct patterns of mental activity, cardiorespiratory patterns, muscle activity and, particularly, electroencephalogram (EEG) activity (see Chapter 1).
Alteration in levels of fatigue and sleep in neurological disorders
Post-stroke fatigue
Fatigue is common after stroke, its prevalence ranging from 16% (Glader et al. 2002) to 70% (Carllson et al. 2003), depending on the definition of fatigue and the population studied.
There is often an increase in the level of fatigue felt by an individual after a stroke, particularly if the level of ischaemia has occurred subcortically, in the brainstem or in the thalamus. In fact, in certain cases, fatigue can be the only major disability and is often accepted as a common part of the disease process. Since, as we stated earlier, the definition of fatigue is so vague, it can be difficult to identify what actually causes it after a stroke. Consequently, it often goes undiagnosed – and thus untreated. In order to mediate this problem, a case definition and interview protocol was developed by Lynch et al. (2007), with one version for inpatients and one for people living in the community. The definition of post-stroke fatigue for inpatients is as follows (p. 543):
Despite the fact that post-stroke fatigue is commonplace, very little is known on the actual extent of the problem or, in fact, what impact it has on the recovery of the individual affected. It does beg the question of how much impact an undetermined level of fatigue could be having on the return to ‘pre-stroke’ levels of activity. There is some evidence that post-stroke fatigue may be slightly more commonplace in females (Glader et al. 2002). However, there are also many studies which find that there is no demographic link with the level of occurrence. There is further contradictory evidence when looking at the severity of the fatigue being experienced. Several studies have linked the severity of fatigue to poor general health, pain, anxiety and depression post stroke. However, other studies report no link between fatigue levels and depression post stroke (Naess et al., 2005, van der Werf et al. 2001). There also appears to be no link between the level of fatigue experienced and either the time since the stroke or the level of disability associated with the stroke (van der Werf et al. 2001).
It therefore appears that, although post-stroke fatigue is a very real issue, there is much we do not know about the factors affecting the occurrence and severity of the fatigue experienced by a patient post stroke. In terms of interventions, a Cochrane systematic review only identified three studies, the results of which were inconclusive (McGeough et al. 2009). Exercise can be effective in reducing fatigue; however a Cochrane systematic review on exercise and fitness training after stroke reported insufficient evidence on this issue (Brazzelli et al. 2011). The unknown aspects of post-stroke fatigue could make the role of the therapist involved in post-stroke rehabilitation particularly difficult. It is clear that a considerable amount of further research is required in this important area.
Fatigue in multiple sclerosis
A definition of multiple sclerosis (MS) fatigue is ‘a subjective lack of physical and/or mental energy that is perceived by the individual or caregiver to interfere with usual and desired activities’ (Multiple Sclerosis Council 1998).
Fatigue in patients suffering from MS is very commonplace; in an audit of people with MS living in Oxfordshire, nearly half of the respondents reported fatigue (Wade and Green 2001). One particular problem mentioned is the fact that fatigue can be experienced at rest and, if occurring following activity, is not helped by rest. Levels of fatigue may also vary within the individual. Another interesting aspect that has been uncovered in some studies is that the level of fatigue experienced appears to be worsened by stress as well as heat (e.g. due to a warm environment or exercise). The exact mechanism behind the occurrence of fatigue in MS patients is not really understood, despite the fact that significant levels of information have been gathered from patients. However, it is thought that fatigue in MS may be associated with depression, cognitive impairment and muscle weakness, as well as disability, and, therefore, a comprehensive biopsychosocial approach to the assessment and management of fatigue should be taken.
Fatigue in Parkinson’s disease
As is the case with both stroke and MS patients, fatigue is also widely observed in Parkinson’s disease (PD), with prevalence ranging from 33 to 58% (Friedman et al. 2007), and about half of patients reporting fatigue as a major symptom (Friedman et al. 2007). Having said that, it is not always clearly defined as a symptom by the patient who may not actually use the word ‘fatigue’ spontaneously. The problems with defining fatigue, mentioned in the context of stroke and MS, also apply to PD and there is currently no consensus on the best tool for assessing fatigue in people with PD (Friedman et al. 2007). Therapists, therefore, need to listen carefully for expressions such as ‘tiredness’, ‘exhaustion’ or ‘lack of energy’ (Brown et al. 2005).
Both depression and cognitive impairment are often linked to fatigue, but this is not necessarily the case in PD patients. Chronic fatigue has been observed in some PD patients, lasting as long as 9 years since diagnosis in some cases, while there is evidence to indicate that fatigue increases with time since diagnosis (Friedman et al. 2007).
Post-stroke sleep disorders
One of the most common forms of SDB is obstructive sleep apnoea (see later). Approximately 65% of stroke survivors will show symptoms associated with SDB, in which the patient usually experiences abnormalities in their respiratory pattern resulting in significant interruptions in their sleep patterns. The knock-on effects of this disrupted sleeping pattern are a marked level of fatigue during the day coupled with a difficulty in focusing their attention on any particular task. One aspect of SDB that has been identified was the fact that those suffering from it exhibited a worrying increase in both blood pressure and clotting factors (Golbin et al., 2008, Robinson et al. 2004). In addition to this, other studies suggest that abnormalities in breathing during sleep may increase the risk of vascular disease. However, it has to be pointed out that there is a lot of debate around this controversial area. A number of clinical studies have been carried out which suggest that habitual snoring actually increases the risk of developing high blood pressure and stroke (Lees et al. 2008, Neau et al. 2002). Interestingly, however, such findings have not been backed up in further work when other risk factors such as age, body mass index (BMI) and smoking were controlled for.
Sleep disorders in Parkinson’s disease
Various studies have shown that somewhere between 60 and 88% of PD patients will show some level of night-time sleep disturbance, coupled with a marked increase in the level of daytime sleepiness (Kales et al. 1971, Larsen 2003, Lees et al. 1988, Tandberg et al. 1998). A number of these patients report a range of marked night-time problems, including broken sleep and regular waking, which do not appear to be helped with use of sleep medications (hypnotics such as Zolpidem®) (Dauvilliers, 2007, Gjerstad et al. 2007, Oerlemans and de Weerd 2002, Tandberg et al. 1998). Any form of sleep fragmentation appears to be more commonplace during the lighter stages I and II, with the patients noting that if they waken they find it exceptionally difficult to fall back asleep.
Sleep apnoea is most commonly found in individuals with a high BMI, a factor not frequently found in PD patients. Despite this, the occurrence of sleep apnoea is much higher than predicted in PD patients. It has been observed in a group of patients with a BMI within the normal range (approximately 19–25 kg/m2) that almost 50% have a significant level of sleep apnoea. Around one-quarter to one-half of PD patients exhibit symptoms of REM sleep behaviour disorder (RBD) where there is an increased level of muscle activity during REM sleep. One key piece of research by Iranzo et al. (2006) showed that RBD may even precede the onset of the clinical symptoms of PD. Further research is required to see if RBD could be an early marker for PD. Another common complaint in about 15% of PD patients is excessive daytime sleepiness (EDS) which results in sleep ‘attacks’ and a danger of, for example, car accidents.
Eating, drinking and swallowing problems
Introduction
Due to the different ways that dysphagia is reported, it is difficult to ascertain the exact incidence and prevalence of the problem. However, some studies have given insight into the extent of people experiencing dysphagia – 64–90% of people in the acute phase of stroke (SIGN 2010); 68% of people with dementia in residential homes (Steele et al. 1997); more than 90% of those with MND; 41% of patients with PD, and 33% of patients with MS (Hartelius and Svensson 1994). While problems eating and drinking can cause poor quality of life it can also cause choking or risk of aspiration (where food or liquid spills into the airway rather than stomach) which in turn can lead to chest infections and pneumonia, malnutrition and dehydration. Patients who are undernourished and dehydrated take longer to recover from illness, and aspiration pneumonia can in some cases lead to death.
Anatomy and physiology of swallowing
In order to understand the difficulties patients with dysphagia are experiencing, it is useful to know the anatomy and physiology of the eating, drinking and swallowing process. There are various anatomical structures that are involved in the swallowing process (see Figs 14.2 and 14.3) and damage to any of the motor or sensory nerves innervating these structures or affecting their coordination can cause an unsafe swallow. There are different stages involved in eating and drinking and problems can arise in any one.
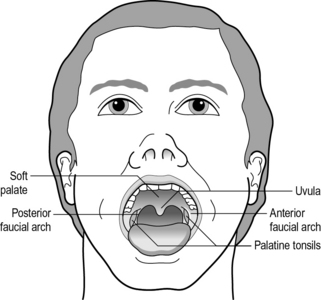
Fig. 14.2 • A frontal view. Anatomical structures involved in the swallowing process.
Adapted from Hardy and Morton Robinson (1999), with permission from Pro-ed, Austin, Texas, USA.
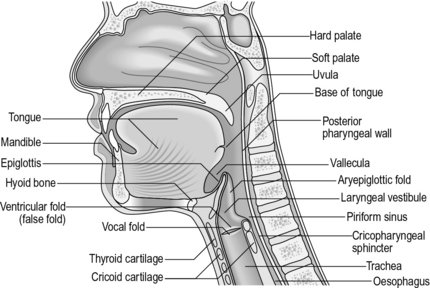
Fig. 14.3 • A sagittal view. Anatomical structures involved in the swallowing process.
Adapted from Hardy and Morton Robinson (1999), with permission from Pro-ed, Austin, Texas, USA.
Oral phases
The first phase prepares the food so that it is in a suitable format for swallowing and involves the various structures in your oral cavity. Have a look inside your mouth using a mirror. You can see many of the structures which include the lips, teeth and tongue, and looking towards the back of your mouth you can see the soft palate (velum), uvula (dangling soft tissue) and faucial arches (see Fig. 14.2). The tongue is an amazing structure which is composed almost entirely of many muscle fibres. It is composed of six regions – the tip, blade, front, centre, back and the base. The first five regions are largely under voluntary cortical control and are involved in the oral phases of the swallow. The sixth region, the base of the tongue, is employed during the pharyngeal phase of the swallow (see below) and is largely under involuntary neural control coordinated in the brainstem. It is also important to note the oral crevices (spaces) between your upper and lower lips and gums and between your cheeks and gums where food can lodge if not cleared by our tongue.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree