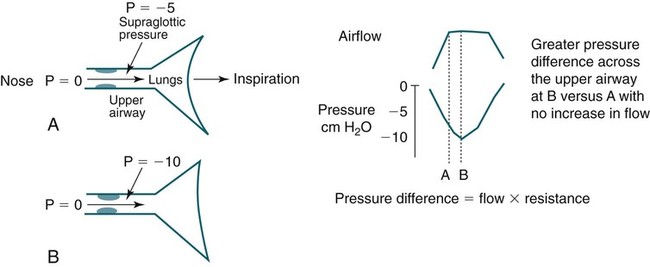
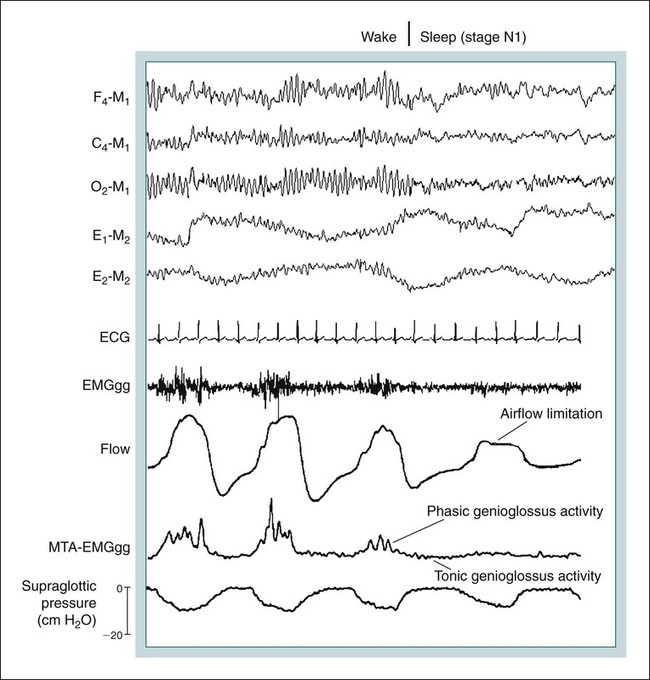
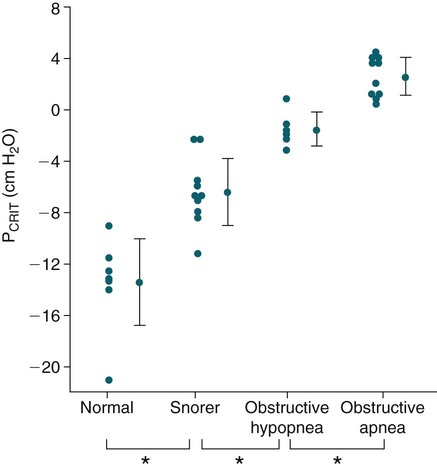
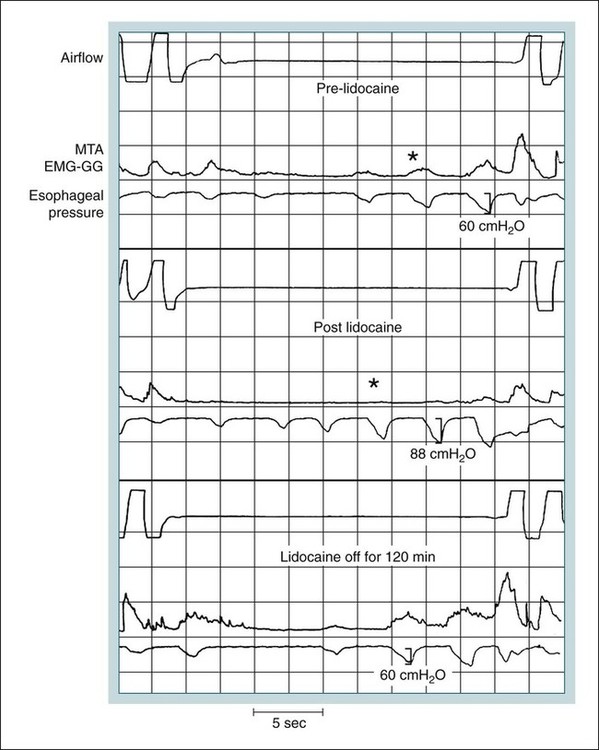
• Patients with OSA have a positive critical pressure during sleep. A positive intraluminal pressure is needed to keep the airway patent. • Patients with OSA have airway occlusion or severe narrowing during sleep because of a variable combination of factors including unfavorable upper airway anatomy, inadequate upper airway muscle compensation, and instability in ventilatory control. Whereas a high arousal threshold may prolong respiratory events, a low arousal threshold may predispose to instability in ventilatory control. Traits Contributing to Obstructive Sleep Apnea From White DP: The pathogenesis of obstructive sleep apnea. Am J Respir Cell Mol Biol 2006;34:1–6. • The reasons for the greater prevalence of OSA in men than in women are incompletely understood. Men have longer upper airways and this may predispose to upper airway collapse. • The activity of phasic upper airway muscles (e.g., genioglossus—tongue protruder) increases with each inspiration. The activity of tonic upper airway muscles is constant (does not vary with respiration). However, the activity level of tonic muscles can vary with sleep state (wake > NREM > REM). The activity of phasic upper airway muscles is controlled by central pattern generators, sleep state (wakefulness stimuli, NREM, REM), and negative-pressure stimulation of upper airway mechanoreceptors. More negative upper airway pressure is associated with increased upper airway inspiratory activity in the genioglossus. • Upper airway muscle activity falls with sleep onset and the decrease is greater in patients with OSA than in normal individuals. During wake, increased upper airway muscle activity in patients with OSA may compensate for unfavorable anatomy. • The arousal stimulus during obstructive apnea and hypopnea appears to be proportional to the magnitude of inspiratory effort (esophageal pressure excursions). Hypercapnia and hypoxemia may cause increasing respiratory effort, but arousal occurs when the level of effort reaches an arousal threshold. • The arousal threshold to respiratory stimuli during NREM sleep is increased in patients with OSA compared with normal individuals (higher inspiratory effort is needed to trigger arousal). • Factors associated with more severe arterial oxygen desaturation include a higher BMI, low awake SaO2 or PaO2, longer respiratory events/shorter period of ventilation between events, and a smaller ERV. Multiple factors determine upper airway patency during sleep (Table 16–1).1–9 Different factors may be more or less important in a given individual. Patients with obstructive sleep apnea (OSA) tend to have small upper airways either secondary to a small bony enclosure or due to increased soft tissue surrounding the airway.10,11 In general, a short and posteriorly placed mandible, a long dependent palate, a large tongue, nasal obstruction, and thick lateral pharyngeal walls, and/or pharyngeal fat all predispose to upper airway collapse during sleep. Most studies have suggested that the shape of the upper airways of OSA patients differs from that of normal individuals and is narrower in the lateral dimension.10–12 A study comparing the passive properties of the upper airway during general anesthesia in normal individuals with those of OSA patients found that the upper airways of OSA patients are narrower and more collapsible.13 TABLE 16–1 Factors Determining Upper Airway Patency Airflow through the pharynx shows various degrees of airflow limitation during sleep. Inspiratory flow limitation is defined by an increase in the pressure drop across the upper airway (more negative supraglottic and intrathoracic pressure) without a corresponding increase in flow rate (Fig. 16–1). This alinearity in the pressure-flow relationship during inspiration is commonly caused by narrowing of a hypotonic upper airway in response to the increasingly negative intraluminal pressure developed during inspiration.14,15 In Figure 16–2, the first three breaths do not show airflow limitation and airflow has a round shape. The fourth breath, which occurs after sleep onset, demonstrates airflow limitation with a constant flow during the time when the inspiratory pressure (supraglottic pressure) as reflected by esophageal pressure is becoming more negative (increased pressure difference across the upper airway). The pharynx is not rigid and pharyngeal resistance is not constant. The nonrigid portions of the pharynx tend to become increasingly narrow with more negative inspiratory pressure. The collapsibility of the upper airway and tendency for closure can be defined by the pharyngeal passive closing pressure (PCRIT).16,17 The PCRIT values for normal people, snorers, patients with obstructive hypopneas, and patients with obstructive apnea are plotted in Figure 16–3.14 As upper airway dysfunction increases (normal → snorers → apnea), the PCRIT is progressively more positive. During sleep, a positive pressure is needed to keep the airway open (PCRIT > 0) in patients with sleep apnea. In normal patients, the airway does not collapse unless a negative mask pressure is applied. The PCRIT is determined by applying various positive or negative mask pressures (Pmask) and determining the inspiratory flow rate. In patients with OSA, flow decreases as mask pressure decreases from a more positive pressure (Fig. 16–4). The mask pressure at which flow is zero is PCRIT. The inverse of the slope is the effective resistance (Δ pressure/Δ flow) and is called the upstream resistance (Rus). The equation relating flow ( The relationship between flow and mask pressure can be modeled using a Starling resistor (Fig. 16–5) using Pus (upstream pressure) = Pmask. This consists of a collapsible segment between rigid tubes.16 As long as the intraluminal pressure within any point of the collapsible segment is less than PCRIT, the relationship in Figure 16–4 will hold. Creating more negative pressure downstream from the collapsible segment will not increase flow. When the intraluminal pressure along the entire collapsible segment is less than the PCRIT, no flow occurs. During wakefulness, upper airway muscle activity maintains an open upper airway even if the airway is anatomically narrow. Some upper airway muscles such as the genioglossus (GG; tongue protruder) and palatoglossus show increased activity with inspiration (phasic activity) (see Fig. 16–2), whereas others such as the tensor velli palatini (a muscle of the palate) show tonic (constant) activity.18–20 Activation of phasic upper airway muscles is triggered slightly before the muscles of the respiratory pump. This allows for a stable upper airway during inspiratory flow. The inspiratory activity of the GG muscle is affected by (1) negative intraluminal pressure via effects on upper airway mechanoreceptors in the laryngeal area, (2) central pattern generators in the brainstem, and (3) influences of sleep state (wakefulness stimulus).1–6 The activity of the phasic upper airway muscles (GG) but not the tonic palatal muscles relates closely to pharyngeal pressure. The activity of tonic upper airway muscles appears to be more sleep state–dependent (wake > non–rapid eye movement [NREM] > rapid eye movement [REM]).18,20 Greater upper airway inspiratory muscle activity occurs with more negative upper airway pressure. Hypoxia and hypercapnia could potentially modulate (increase) upper airway muscle activity via effects on the central pattern generators or indirectly by augmenting ventilatory drive/inspiratory effort, generating more negative upper airway pressure (higher suction pressure). Pillar and coworkers21 administered exogeneous CO2 to normal individuals during NREM sleep and found no significant augmentation of GG activity. The epiglottic negative pressure was not significantly different between baseline and CO2 inhalation. Thus, hypercapnia was not associated with more negative upper airway pressure or an increase in GG activity. This study was performed with subjects in the lateral sleep position. In contrast, during monitoring in the supine position, Lo and colleagues8 did find that exogenous CO2 administration augmented GG activity. The administration of continuous positive airway pressure (CPAP) did not change the slope of the GG response to hypercapnia. However, upper airway pressure was not measured. The etiology of the effect of posture is not clear. With sleep onset, the loss of the wakefulness stimulus on upper airway muscles causes a decrement in their activity. This may be mediated in part by a loss of serotonergic or noradrenergic excitatory modulation of upper airway motor neuron activity.5 At the onset of NREM sleep, the activity of both phasic and tonic upper airway muscles decreases18,19,22,23 and upper airway resistance increases24 (see Fig. 16–2). With stable sleep, the activity of the GG may actually return to waking or higher than wakefulness levels as upper airway pressure becomes increasingly negative25 (Fig. 16–6). If upper airway activity is favorable or upper airway muscle activity has “compensatory effectiveness,” stable ventilation will be maintained. Compensatory effectiveness requires a sufficient increase in upper airway muscle activity (stimulated by hypercapnia and negative upper airway pressure) and that the increase in muscle activity is effective in maintaining upper airway patency.26 Patients with OSA tend to have higher than normal awake basal GG activity.27–29 The higher activity is believed to be compensation for an intrinsically narrow or more collapsible upper airway. Most patients with OSA also have a greater than normal fall in GG activity with sleep onset.29 A reflex activation of the GG muscle to a sudden brief pulse of negative pressure can be demonstrated.30 The response of the GG and palatal muscles to negative pressure is reduced during sleep.30–32 During wake, patients with OSA have a greater response in GG activity to a sudden negative pressure pulse than normal subjects.33 The greater response to negative pressure and higher basal GG activity allow the upper airway to remain open during wakefulness. In contrast, the response of the palatal muscles to negative pressure may be impaired in OSA patients.34 Despite evidence for higher basal upper airway muscle activity during wakefulness, the upper airways of OSA patients are still more collapsible than those of normal persons.35 With sleep onset, the wakeful stimulus to GG activity is no longer present and upper airway muscle activity falls in normal individuals and patients with OSA. However, as noted previously, OSA patients have a greater than normal fall in upper airway muscle activity.29 Owing to unfavorable anatomy, the residual upper airway activity is not sufficient to maintain an open upper airway. In Figures 16–6 and 16–7, a fall in GG activity as the patient returns to sleep is associated with an obstructive apnea. Posture also has important effects on airway patency,36 and some patients with OSA have apnea or hypopnea only in the supine position. During upper airway obstruction, phasic GG activity increases proportionately to esophageal pressure deflections (reflecting increased respiratory drive) (see Figs. 16–6 and 16–7).9,37,38 Stimulation of chemoreceptors by hypoxia and hypercapnia increase inspiratory drive and esophageal pressure deflections increase. At apnea termination, both GG and palatal muscles are preferentially augmented and the upper airway opens.9,37,38 Although it was once assumed that increasing GG activity during obstructive apnea or hypopnea was driven entirely by hypoxia and hypercapnia, a study of the effect of upper airway local anesthesia suggests that mechanoreceptor stimulation (from increasingly negative pressure below the site of obstruction) plays an important role in the augmentation of GG activity.37 In Figure 16–8, the top panels (Pre-lidocaine) show a progressive increase in GG activity during apnea. After topical lidocaine anesthesia of the upper airway, the GG activity is markedly diminished. This implies that mechanoreceptor stimulation from increasingly negative pressure below the site of obstruction results in augmentation of GG activity. Traditionally, a concept of a balance between negative inspiratory pressure tending to collapse the airway and upper airway muscle dilating forces was assumed to determine the state of the airway. However, more recently, the concept of passive collapse at sleep onset (including return to sleep after termination of respiratory events) has gained favor. In fact, at sleep onset, the ventilatory drive decreases and supraglottic pressure may initially decrease (less negative) in some patients (although resistance increases). Upper airway closure has also been documented during central apnea in which there is no inspiration or negative collapsing forces.39 Therefore, suction pressure during obstruction may help keep the airway closed but is not necessary for the onset of airway occlusion. Cyclic variations in ventilatory drive can induce obstructive or central apneas at the nadir in drive.40 Thus, even if ventilatory drive to the respiratory pump muscles decreases, the simultaneous reduction of neural drive to the upper airway muscles can result in airway narrowing or collapse. Upper airway size also has a dependence on lung volume with decreasing airway size as lung volume decreases.41,42 The upper airways of patients with OSA have greater lung volume dependence than normal individuals.41 The lung volume dependence of the upper airway may be mediated via passive distending forces due to a downward tension on upper airway structures during inspiration (“tracheal tug”).43 Another way of thinking of the tracheal tug is a decrease in extramural pressure surrounding the airway. Any fall in end-expiratory volume (functional residual capacity [FRC]) would then reduce upper airway size. FRC is known to decrease during sleep,44 and this would tend to predispose to airway closure. Morrell and coworkers45 demonstrated a progressive fall in end-expiratory retropalatal cross-sectional area as well as end-expiratory lung volume in the breaths leading up to obstructive apnea. Heinzer and colleagues46 found that an increase in lung volume (induced by extrathoracic pressure) resulted in a lower level of CPAP required to prevent airflow limitation.
Pathophysiology of Obstructive Sleep Apnea
ANATOMIC/PHYSIOLOGIC TRAIT
APNEA PREDISPOSITION
Upper airway anatomy
Small pharyngeal airway
Upper airway motor control
Poor muscle response during sleep
Ventilatory control stability
High loop gain
Arousal threshold
Low arousal threshold
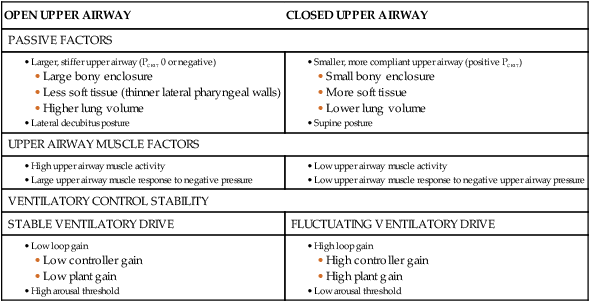
Pathogenesis of Upper Airway Obstruction
OPEN UPPER AIRWAY
CLOSED UPPER AIRWAY
PASSIVE FACTORS
UPPER AIRWAY MUSCLE FACTORS
VENTILATORY CONTROL STABILITY
STABLE VENTILATORY DRIVE
FLUCTUATING VENTILATORY DRIVE
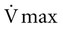 ), mask pressure, and PCRIT
), mask pressure, and PCRIT
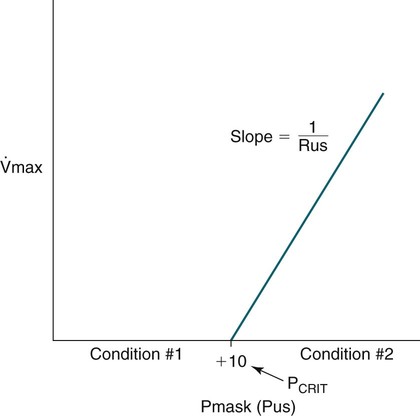
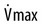 ) and various mask pressures (Pmask) in a sleeping patient. When Pmask falls below PCRIT, no flow is noted (Condition #1). When Pmask exceeds PCRIT (Condition #2), the flow depends on the pressure difference (Pmask – PCRIT) and the slope of the line is the inverse of the upstream resistance (Rus). In the Starling model, the Pmask is considered the upstream pressure (Pus)—see Figure 16–5. From Gold AR, Schwartz AR: The pharyngeal critical pressure. Chest 1996;100:1077–1088.
) and various mask pressures (Pmask) in a sleeping patient. When Pmask falls below PCRIT, no flow is noted (Condition #1). When Pmask exceeds PCRIT (Condition #2), the flow depends on the pressure difference (Pmask – PCRIT) and the slope of the line is the inverse of the upstream resistance (Rus). In the Starling model, the Pmask is considered the upstream pressure (Pus)—see Figure 16–5. From Gold AR, Schwartz AR: The pharyngeal critical pressure. Chest 1996;100:1077–1088.
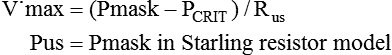 Equation 16–1
Equation 16–1
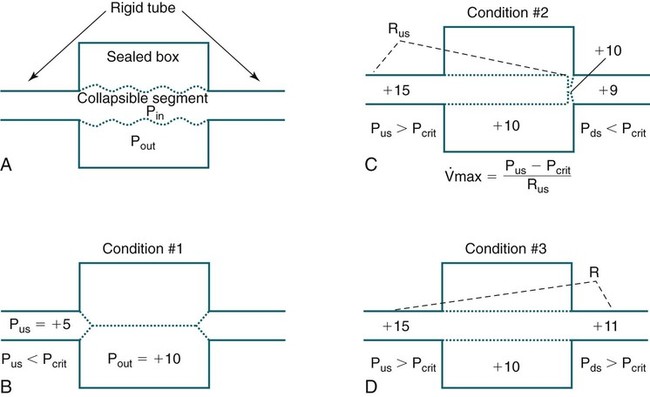
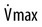 = flow rate. Adapted from Gold AR, Schwartz AR: The pharyngeal critical pressure. Chest 1996;100:1077–1088.
= flow rate. Adapted from Gold AR, Schwartz AR: The pharyngeal critical pressure. Chest 1996;100:1077–1088.
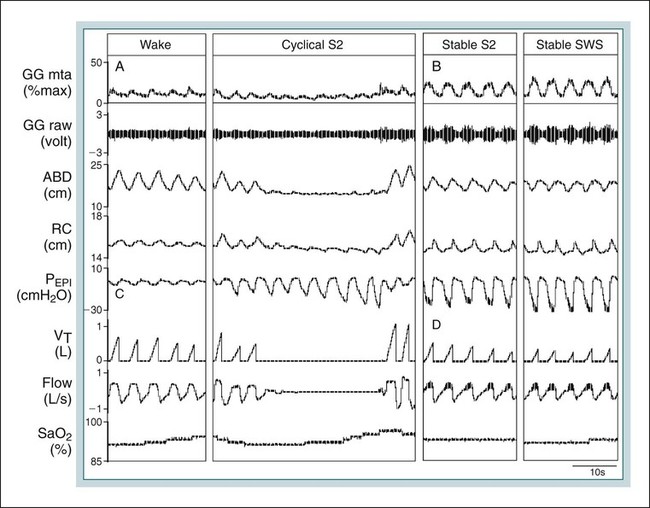
Lung Volume Effects
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







