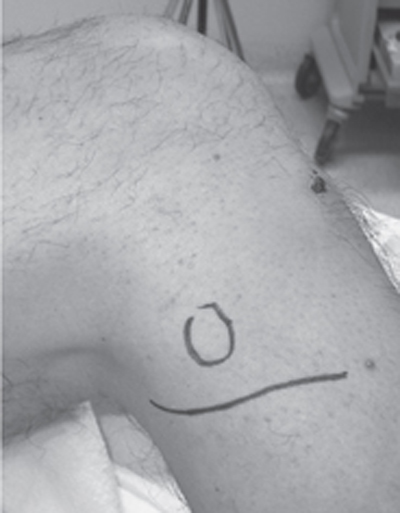
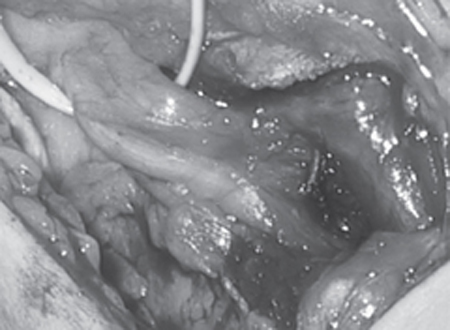
44 Peroneal Nerve Entrapment A 32-year-old, previously healthy woman in her seventh month of pregnancy suffered a fall with a resultant severe left ankle sprain. The sprain was treated with an elastic wrap and activity restrictions. Radiographs revealed no fracture. Over the next several weeks she developed a severe, sharp pain poorly localized to the lateral left ankle, which was distinct from the pain associated with the initial injury. She also noted subjective weakness of ankle dorsiflexion and intermittent paresthesias over the dorsum of her foot and anterolateral leg. Her symptoms persisted for several months following the delivery of her child. Oral medications including acetaminophen, ibuprofen, gabapentin, and amitriptyline were unsuccessful in alleviating her pain complaints. Physical therapy was not helpful. Examination 6 months after injury revealed decreased pinprick sensation and dysesthesia over the dorsum of the left foot and anterolateral left leg. A Tinel sign was elicited with percussion of the peroneal nerve adjacent to the fibula head. Motor strength testing of toe extension and ankle eversion and dorsiflexion was diminished at 4/5. The remainder of the neurological examination was normal. Left peroneal nerve compound motor action potential amplitude was 5.8 mV when stimulated below the fibula head compared with 2.0 mV with stimulation in the popliteal fossa. Peroneal conduction velocity was 43 m/s and 45 m/s below and above the fibula, respectively. Needle examination failed to demonstrate denervation changes in any of the left lower extremity musculature. Surgical decompression was recommended but the patient initially refused surgery. She returned for evaluation 25 months after injury at which time her examination was unchanged. Her pain was worse and pressure in the region of the fibula head exacerbated her pain and sensory complaints. She underwent decompression of the peroneal nerve at the fibula head with a gentle S-shaped incision beginning in the lateral popliteal fossa and extending over the fibula head onto the anterolateral leg (similar to that shown in Fig. 44–1). A fibrous band arising from the peroneus longus muscle was noted to indent the nerve as it entered the anterior compartment. In addition, a small bony protrusion at the fibula neck was identified and removed. The nerve was completely decompressed by incising the overlying fascia and peroneal muscle (as shown from a similar case in Fig. 44–2). The wound was closed in layers and the leg was wrapped in a bulky dressing. No weight-bearing restrictions were imposed. She had no complications related to her surgery. At her 6-month follow-up visit, she had resolution of her pain complaints and complete return of motor and sensory function. Figure 44–1 The surface anatomy and incision to decompress the peroneal nerve at the knee, related to the fibular head (circle) is illustrated. Note that the incision starts just below the popliteal fossa, crosses over the fibular neck, and extends onto the anterolateral leg. (Photo courtesy of Dr. Richard Houlton.) Figure 44–2 The decompressed peroneal nerve is shown after incising the peroneal fascia and some of the overlying superficial peroneal muscle. The proximal nerve (vasoloop) divides into its superficial and deep branches just distal to the (incised) fascia overlying the peroneal muscle. Peroneal nerve entrapment at the knee Dorsal branches of L4, L5, S1, and S2 ventral rami contribute to the formation of the peroneal component of the sciatic nerve that generally exits the greater sciatic foramen of the pelvis along with the tibial component inferior to the piriformis muscle. In a minority of patients, the peroneal component will exit through or superior to the piriformis muscle. The peroneal portion of the sciatic nerve is generally half the size of the tibial nerve. The two travel together in a loose connective tissue sheath under the gluteus maximus muscle in the buttock and into the posterior thigh in a centrally located position. At the apex of the popliteal fossa, at approximately the junction between the middle and distal thirds of the thigh, the peroneal nerve diverts laterally just medial and deep to the tendon of the biceps femoris muscle. It then passes posterior to the head of the fibula and winds around the fibula neck. It passes under the origin of the peroneus longus muscle before dividing into its terminal superficial and deep branches (Fig. 44–2). In the thigh, the peroneal component of the sciatic nerve supplies the short head of the biceps femoris muscle, the long head being supplied by a separate branch from the hamstring division of the sciatic nerve. In the lateral popliteal fossa the peroneal nerve gives off two cutaneous branches, at times from a common origin, the lateral sural cutaneous nerve, which supplies the antero- and posterolateral upper leg, and the sural communicating nerve, which joins its counterpart from the tibial nerve to form the sural nerve proper. Genicular branches accompany the superior and inferior genicular and recurrent tibial arteries to supply the knee joint. The deep peroneal nerve supplies the muscles of the anterior compartment, including the tibialis anterior, extensor digitorum longus, extensor hallucis longus, and peroneus tertius. In the region of the ankle and foot it gives off branches to the ankle joint and extensor digitorum brevis. It ends as a cutaneous nerve supplying skin in the first web space of the foot. The superficial peroneal nerve supplies the peroneus longus and brevis muscles of the lateral compartment before ending as a cutaneous supply to the distal anterolateral leg and dorsum of the foot. Neurological disturbance in the distribution of the peroneal nerve can take many forms. Pain can be poorly localized to the dorsum of the foot, lateral ankle, or distal leg. There may be a deep aching quality with or without dysesthetic burning pain. In some patients, passive ankle inversion and dorsiflexion worsen the pain. Motor deficit is common and involves the peroneal innervated muscles listed in the previous section. Mild weakness of ankle dorsiflexors may lead to a slapping sound during heel strike of the affected foot because the dorsiflexors are unable to maintain ankle posture while the weight is shifted forward onto the leg. Patients frequently trip when the toe catches on the ground during ambulation. The weakness is often more notable when the leg is fatigued, and the patient may exhibit an obvious foot drop. Patients with severe weakness compensate by flexing the hip in an exaggerated fashion and then kicking the affected leg forward in the typical high-stepping gait. Evertor weakness may lead to recurrent ankle sprains. Sensory dysfunction may take the form of paresthesias or numbness. A Tinel phenomenon with percussion of the peroneal nerve at the fibula head is common. Because of its superficial location and anatomical course, focal peroneal nerve dysfunction may result from a direct contusive injury to the nerve at the fibula head, or in association with knee injury or knee surgery. Less obvious is the stretch injury, which may occur with ankle trauma as in this case illustration. Repetitive mild compression in the form of leg crossing has long been implicated as a cause of peroneal neuropathy. External compression injury may also result from poorly fitting casts and braces, during anesthesia or coma, or with prolonged kneeling and squatting. Focal peroneal neuropathy brought on by running has been reported. In these patients, the painful neurological dysfunction has its onset during the run and slowly resolves once the activity is discontinued. Peroneal neuropathy has been associated with rapid weight loss. The exact mechanism for this type of neuropathy has been debated. Explanations include a metabolic deficiency, the ability of a previously obese patient to cross the legs, loss of subcutaneous fat without leg crossing, or some other unknown factor. Metabolic neuropathies such as diabetes mellitus, hypothyroidism, and B12 deficiency may affect the peroneal nerve and should be treated when possible prior to consideration of surgical decompression. Of the masses in this region, ganglion cysts are the most common, although nerve sheath tumors and bony lesions are also found. Finally, in some patients, an exact etiology for the focal peroneal neuropathy cannot be defined. When pain is present without objective neurological dysfunction, ankle derangements such as chronic subtalar synovitis or talar subluxation should be considered. When the pain is brought on by exercise, anterior compartment syndrome may be the cause. Measurement of compartment pressures may be needed in questionable cases. In patients with motor or sensory disturbance, other neurological disorders should be excluded, with sciatica and more specifically L5 radiculopathy being the most common. A history of back pain should be sought, and patients examined for nerve root irritation findings, such as limited straight leg raise. Sciatic nerve compression neuropathy (i.e., piriformis syndrome), or proximal sciatic nerve injury with differential involvement of the peroneal component is also a possible diagnosis. Pain with proximal nerve manipulation would be suggestive of this, and any tibial or hamstring nerve dysfunction would rule against peroneal nerve compression neuropathy at the knee. Focal neuropathy of the deep peroneal nerve at the ankle, referred to as the anterior tarsal tunnel syndrome, or superficial peroneal nerve in the distal lateral leg results in pain and sensory symptoms without clinically significant motor deficit. Finally, painless foot drop may rarely be caused by intracranial processes such as anterior circulation ischemia or tumors. Upper motor neuron findings help to identify these entities. In general, electrodiagnostic tests are the most helpful adjunct in making the diagnosis of focal peroneal neuropathy and excluding other entities. Needle studies that show involvement of paraspinal or tibial-innervated L5 musculature, such as the flexor digitorum longus or tibialis posterior, suggest spinal disorders. Denervation of the short head of the biceps femoris muscle indicates peroneal nerve dysfunction at a more proximal site than the knee region and is extremely valuable for proper localization. Evidence for denervation of peroneal musculature may not be present, especially in milder cases. A decrease in the amplitude of the peroneal compound motor unit potential above as compared with below the fibula head is very helpful as was noted in the present case. Amplitudes can also be compared with the contralateral unaffected peroneal nerve or if necessary to normal control values. Slowing of peroneal nerve conduction velocities at the fibula head may or may not be detected. Imaging studies are not routinely necessary but may be helpful in cases where a mass is suspected. Magnetic resonance imaging studies help delineate ganglia and tumors of the nerve. Bony protuberances can be seen with conventional radiographs or computed tomographic scans. Ultrasound may be helpful in that a large segment of the nerve can be surveyed relatively quickly and inexpensively. Imaging studies of the lumbosacral spine may be necessary to rule out degenerative disk disease. Conservative management is initially appropriate in most cases because many nerve deficits will recover spontaneously. During the waiting period, support of the ankle with an external orthosis, or in milder cases, with well-fitting boots or high-topped sneakers, is appropriate. Pain can be managed with agents such as amitriptyline or gabapentin when tolerated. Physical therapy is also employed to increase strength and teach patients to optimize function with their existing deficit. Strict avoidance of external pressure on the nerve such as with leg crossing or braces is critical. Surgical decompression is recommended in patients who show little or no improvement after 3 to 4 months. The procedure is relatively straightforward, although the superficial location of the nerve at the fibula puts it at risk during the initial incision and dissection. The nerve is identified in the popliteal fossa, and a neurolysis is performed circumferentially to its terminus into the superficial and deep branches. Shortly after its origin, the deep peroneal nerve gives off multiple motor branches, which should be preserved. The genicular branch accompanying the recurrent tibial artery, however, can be sectioned if necessary. In the case of ganglion cysts involving the peroneal nerve, sacrifice of the genicular branch is recommended to decrease the likelihood of cyst recurrence. Neurolysis may be supplemented by a partial osteotomy of the fibular head to remove bony protuberances or simply to shorten the course of the nerve. In patients with severe motor deficit that does not improve following decompression, reconstructive procedures such as tendon transfer of the tibialis posterior muscle can be considered. In general, the majority of patients with focal peroneal neuropathy recover well following surgical decompression, although the recovery is not always complete. This may relate to the varying etiologies for the nerve dysfunction. Most series include patients with nerve injury secondary to knee surgery or traumatic knee injury. In addition, diagnosis may be delayed, prolonging the period of time prior to surgery. In many series, the average time between symptom onset and surgical decompression was 1 to 2 years. The severity of deficit prior to surgery has been variably shown to affect outcome following surgery, with milder deficits showing better recovery. However, even patients with longstanding severe motor deficit can demonstrate good recovery following surgical decompression. Reported complications related to the surgical procedure are relatively infrequent. The superficial location of the peroneal nerve at the fibula head and its surrounding fibrous constraints put it at risk for traumatic injury and entrapment. Focal peroneal neuropathy may be brought on by ankle injury. Excellent results can be obtained with surgical decompression, which should be considered in patients who demonstrate little or no recovery after 3 to 4 months of observation.
 Case Presentation
Case Presentation
 Diagnosis
Diagnosis
 Anatomy
Anatomy
 Characteristic Clinical Presentation
Characteristic Clinical Presentation
 Etiologies
Etiologies
 Differential Diagnosis
Differential Diagnosis
 Diagnostic Tests
Diagnostic Tests
 Management Options
Management Options
 Outcome and Prognosis
Outcome and Prognosis
 Conclusions
Conclusions
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


