Maria Quintieri and Sebastiano Serra
General Considerations
The recuperation of conscious activity is the main therapeutic goal and prevailing task in the treatment of patients in the vegetative state. A variety of approaches, ranging from intravenous amphetamine administration to the electrical stimulation of thalamic structures, have been followed in recent decades. Intense and prolonged sensory stimulation has been used as well, but this method is still a matter of debate (see p. 81). The recuperation of conscious mental activity requires individualized planning and relies on an empirical approach, based mostly on the inventiveness and goodwill of therapists and family members.
The physician needs to follow a scientific approach in order to devise a therapeutic plan that takes into account all the functional systems regulating vigilance and consciousness (p. 11). The theory of coherence suggests that a certain degree of simultaneous stimulation of the four functional systems regulating consciousness is required. It has been noted, for instance, that isolated auditory-tactile sensory stimulation can provoke a state of alarm, accompanied by a diffuse vegetative response. Similarly, a persistent supraliminal stimulation can provoke a state of hypervigilance, which can interfere with perception and the processing of each stimulus. With this in mind, we will put forth some general rules (derived from our practical experience, but also justified in theory) that are based on the knowledge of the neurological mechanisms described. These so-called “rules of thumb” [1] have been summarized as follows:
• First rule: before eliciting any type of performance, it is mandatory to obtain relaxation – so never work under alarm conditions.
• Second rule: assist in the recuperation of circadian rhythms.
• Third rule: passively induce ipsilateral and contralateral motor systems prior to any sensory stimulation, by passively turning the head toward the source of the stimulus.
• Fourth rule: stimulation must at first be simple – a caress on the face or hand. Never repeat a stimulus if a response is not obtained from the first stimulus.
Although based primarily on experience and common sense rather than on scientific evidence, these rules may suggest the choice of proper actions.
There is no particular technique or method for helping the patient to resume conscious activities during the vegetative state, but we would contend that the “method” by which therapeutic procedures are conducted can determine the efficacy of the treatment. In addition, it should be borne in mind that “the patient is locked in the only state of being that is possible to him or her at the moment, and is unable to use the forms of expression we would otherwise expect in different conditions; we must come forward to meet this new structure of existence and let it express itself, possibly also by helping its expression wherever we can” [2]. The observation of a sign, and above all its interpretation, should be shared by the whole team of attending nurses, therapists, technicians, and physicians, in a collective rather than individual effort to achieve objectivity and reliability. Beyond the individual techniques and methods, it is also necessary to establish unequivocal guidelines for use in analyzing each action.
Each single procedure and its modalities of application will be described as derived from the general strategy developed by Zylberman and Vichi [3].
Observation of the General State
Experience is a major source of know-how in the treatment of patients in the vegetative state. It should be noted once again that these patients have no way of interacting with the attending staff and are unaware of the therapeutic approach to be taken. This is a physician’s responsibility, and a consensus from the family members should be obtained according to ethical requirements and local regulations.
The clinical picture is extremely complicated and includes pathologies due to cranial trauma, as well as acute complications [4,5] involving in varying combinations the osteoarticular, respiratory, gastrointestinal, genitourinary, and hemopoietic systems. Also, pathologies and symptoms otherwise not observed in other diseases sometimes have to be dealt with in the vegetative state, which is thus a distinct condition in its own right. Clinical observation and maintenance of the general state are the cardinal aspects of any action to be taken. To make this approach feasible and to some extent standardized, predefined procedures need to be established, and any progress should be detailed in the patient’s records, which must be easy to consult and made available to all members of the staff. Predetermined procedures also make it possible to proceed with a global treatment schedule, which should be common to all patients in the first phase, and thereafter to follow a more detailed and personalized plan based on evaluation by the staff over several days of observation. In this initial phase, continuous monitoring of vital signs (also intended to avoid a wide range of life-threatening complications) and the drawing up of a complete clinical chart form the basis of treatment for patients whose conditions have a similar origin and tend to proceed in a predictable manner, although they may rapidly become different from patient to patient at a later time.
Survey of Vital Parameters
• The vital parameters to be monitored are blood pressure, heart rate, temperature, respiratory rate, and peripheral oxygen saturation.
• The vital functions to be monitored are diuresis, hydration, stool, and sweating.
• Monitoring procedures should be carried out by nursing staff and therapists during treatment in order to evaluate potential changes in vital parameters.
• Monitoring should be continuous throughout the duration of intensive care.
• Data should be recorded on the progress sheets and patient charts by both the nursing staff and therapists. Data that deserve further consideration are forwarded to the department physician.
Pharmacological Therapy and Drug Administration Modes
Particular attention must be paid to the use of pharmacological therapies, which should be reduced to a minimum to comply with essential needs only. Parenteral drug administration using central venous access should be switched to peripheral venous administration as soon as practicable, with a preference for the minimal possible number of administrations per day (possibly once daily). Intramuscular administration should be avoided whenever possible in order to minimize the risks of local infection, which often goes undetected, but may provoke abscesses or fever. The ultimate goal is enteral pharmacological administration via a nasogastric tube or percutaneous gastrostomy. Powders are preferable, while effervescent or oily formulations are not advisable. Subcutaneous administration is reserved for prolonged treatment (e. g. low molecular weight heparin) and should be on a single daily administration. It is only in this way that patients can be treated without the encumbrance of tubes.
Procedure: before Drug Administration
• The patient must be identified.
• An administration schedule for the drug or drugs must be established and detailed in the patient’s charts as required, to ensure compliance by both nursing staff and physicians.
• The modalities for drug administration must be established: parenteral, enteral, aerosol, sublingual, etc.
• Communication with the patient should be established in any way possible in order to inform him or her about what is being undertaken and to avoid any feeling of being threatened.
• Administration.
• Recording of drug administration on the patient’s chart or progress sheets.
The access routes must be monitored and maintained. Enteral nasogastric tubes and percutaneous gastrostomies must be rinsed with 20 mL water before and after drug administration. Parenteral infusions must be checked for drip speed and type of solution. A permanent cannula should be positioned whenever long-term administration or repeated administration are required (e. g., in the case of patients receiving heparin). Central venous catheters are to be replaced every 7 days. Once removed, catheters must be sent in for bacterial culture. Peripheral catheters must be replaced periodically and rotated. When possible, enteral access is preferred to other administration routes.
Treatment Program
Once a treatment plan has been established, the following must be carried out:
• Neurological examination
• Evaluation by an appropriate scale of the degree of communicative functions
• Evaluation by each member of the team
• Elaboration of a treatment plan
• Periodic staff meetings, with evaluations of each patient by each staff member
All staff members should be actively involved in the treatment. It is advisable that the treatment plan be carried out at scheduled times, as this allows reevaluation, monitoring, updating, and adaptation of the treatment plan to the patient’s clinical progress. All colleagues should be provided with the patients’ documentation.
Hygiene
The patients’ hygiene is the responsibility of the nursing staff, and hygiene procedures need to be carried out accurately and according to schedule, after the patient has been informed about what is to be done using a suitable communication mode (if any). The patient is bathed on a fitted stretcher in the room if his or her vital signs are unstable, or otherwise in the bathroom and always at a warm ambient temperature. Soaps and shampoos that do not produce excessive foam should be used with hot water. In cases when communication is possible and there is partial autonomy, the nurse should ask the patient if he/she requires help. In fact, the nurse’s gesture may possibly induce a response or voluntary movements in answer to a simple command. The presence of a gastrostomy or fever and the absence of consciousness are not impediments to this practice. Hot water, tactile stimulation, and repetition of a type of situation the patient might recognize from his or her own life all represent ways of resuming contact with the environment and favor communication. In addition, these procedures allow passive mobilization of all joints, changes in posture, and initial mobilization from the hospital bed. The patient is washed and dried; the use of hydrating and emollient substances allows olfactory and tactile stimulation, besides helping prevent decubitus ulcers and thromboembolic risks. Medications for decubitus ulcer are then reapplied to the skin around the tracheostomy and gastrostomy. In the morning, nurses shave patients, cut their hair, and clean their nails. Next, they dress the patients – again allowing passive mobilization and movements (such as putting on a T-shirt, socks, etc.) that are familiar to the patient and therefore of particular significance. Underwear with elastic or buttons should not be worn in the initial phase, as it produces localized skin pressure and can be an obstacle in emergency situations. Everyday hygiene (oral hygiene using a toothbrush, combing the hair, make-up) is performed at some centers by the therapist, with the patient seated in front of a mirror (Fig. 7.1). In the early phase, the patient passively follows the therapist’s movements, until recuperation occurs at a level involving greater complete autonomy in everyday activities for self-care.
Procedure
The staff is responsible for skin hygiene and for performing procedures which also stimulates the patient’s tactile perception and favors microcirculation through passive mobilization.

Fig. 7.1 Oral hygiene performed by the patient with the help of a mirror and assistance from the therapist
Preliminary procedures. Washing is part of the daily schedule and includes bathing or showering. The bathroom must be properly prepared, with optimal water and air temperature, and whatever may be needed for any individual patient (shampoos, sponges, sponge pieces, gauze to renew medications, diapers for incontinence, clothes, perfumes, emollient creams, etc.)
Shower. The patient is moved from his or her room to the bathroom by means of a lifting device. He or she is then undressed and medication tubes are removed. Care is taken to protect the tracheostomy cannula. The patient is washed by immersion or shower, with proper control of the position in space of each body segment. The nurse sprinkles the whole body surface with soap and asks the patient to follow the massage and washing movements of each body part. Particular care must be shown on surfaces with increased contact with organic liquids (urine, feces, vomit, bronchial secretions, sweat) or surrounding decubital sores. The nurse then rinses the whole body surface in the same manner as described above and dries it gently with a cotton towel. Emollients and hydrating creams are applied, and oral, ulcer, and decubital medications are renewed. Nails are cleaned and hair dried. The patient is dressed, and the entire procedure is documented, as are signs of relief during the shower. The presence of skin damage and anything of potential relevance needs to be noted in the patient’s chart.
Prevention and treatment of decubitus sores. Patients in the vegetative state are by definition unable to care for their own personal needs, nor are they able to move or show appreciation or discomfort which makes them completely dependent on professional care. There are guidelines for the proper management of sphincters and cutaneous trophism in relation to hygiene procedures. In particular, decubitus sores are frequent, and their formation (and development directly proportional to the progression of the clinical picture and metabolic condition) should be prevented. Extreme attention must be given to the revival and maintenance of blood proteins through correct nutrition and integrated therapy. Patients often present with a tendency toward immunodeficiency (see p. 24). Treatment of decubitus lesions is of primary importance, as is the prevention of new sores. Antidecubitus mattresses are critical for this purpose (latex, hollow silicone fibers, air or water stuffing, computerized systems for differential regulation of pressure on skin and muscles, etc.), and remain the best strategy for prevention and therapy, even compared to topical medications. Before treatment, the patient’s general state, skin hydration, and possible mobilization must be checked. The number of lesions, their positions, and their characteristics (depth, margins, secretion, color, odor) should be recorded. Continuous photographic documentation can be helpful in observing the progression of skin lesions.
General Procedures
• Showering and bed hygiene are to be performed daily by the nursing staff (see above).
• Application of hydrating creams, using gentle massage, will avoid maceration of skin areas where there is a risk of sores developing, for example due to continuous position-related pressure.
• Reduction to the minimum possible of any contact with urine and feces.
• Mobilization through frequent changes of position in bed, avoiding constant pressure on areas where there is a risk of sores developing (occipital bone, shoulder blades, trochanters, sacrum, ischial tuberosity, ankles, and any other areas potentially subjected to decubitus sores).
• Mobilization in a wheelchair, at least once a day.
• Progressive upright positioning in an electric bed, for relatively short periods but several times every day.
• Proper hydration and food intake compatible with the patient’s caloric requirements. A hypercaloric diet is advised (estimated requirement for catabolic patients with decubitus sores up to 60 kcal/kg/day), using commercial products that ensure the daily intake of proteins, carbohydrates, fats, and minerals, following allowances detailed in the chapter on nutrition.
Local Treatments
The following methods cover the possible treatment options:
• Cleanse decubitus sores with saline for lesions in the granulation and reepithelialization phases, or with oxygenated water for necrotic or fibrinous lesions.
• Disinfect with 5 % chlorine oxide electrolyte solution, rinsing infected lesions with saline.
• Apply occlusive medication with hydrocolloids for lesions in early or reepithelialization phases.
• Apply highly absorptive hydroactive medication for deep granulating, exudative, and infected lesions.
• Apply occlusive medication with hydrocolloid gels for necrotic and fibrotic lesions.
Management of Sphincter Activity
Again, the entire team should be involved in the effort to restore the patient’s sphincteral continence. Use of a urinary catheter should be restricted to cases in which it is unavoidable and limited to the initial phase of recovery. The procedure involves removal of the catheter and use of an external collector once autonomous miction is reestablished. Defecation must also be controlled. A certain degree of sphincter control and appropriate aids have innumerable advantages, such as allowing the patient to leave the room during rehabilitation.
Constipation and diarrhea can be controlled by a proper diet and the regular application of enemas, whereas the long-term administration of laxatives has proved less effective. Controlling and regularizing stool avoids the danger of fecalomas, hemorrhoids, and autonomic reactions possibly due to the patient’s discomfort. Loose stool is usually related to nutritional problems and can be prevented (after adequate chemical examination and a search for parasites) by means of a proper food plan focusing on food quality, amount, and speed of administration. In cases of diarrhea, the suspension of enteral feeding for a few hours, fecal cultures and parasite examinations, and the resumption of 250 mL enteral water administration (every 150 min up to a quantity of several liters, if allowed by the clinical heart and blood pressure conditions) are useful.
Procedure. First, the existence of sphincteral incontinence should be noted. Fecal and urine specimens should be collected for physicochemical examination and culture. The progress sheets should document the comprehensive water balance (intake, elimination, routes, infusions, hydration, nutritional volume). In case of permanent catheter the urine produced over 24 h should be assessed for diuresis control; contact between organic liquids (such as urine or feces) and skin should be avoided in order to prevent decubitus sores. The reasons for keeping the catheter in place are documented on progress sheets and patient charts.
The urinary catheter should be removed as soon as possible, and an external urine collector (in males) or diapers (in females) should be favored. The catheter needs to be repositioned in the few patients with urinary retention (globoid bladder) or neurological hypertonic bladder, with or without sphincteral incontinence, as well as in cases of urinary retention due to spastic bladder sphincter (as often seen in urinary infections). In the absence of spontaneous miction with urinary retention (globoid bladder) catheters are used extemporaneously or at fixed times. Catheter use should always be documented in the progress sheets.
If there is constipation, an enema is given within 3 days at the latest, with documentation in the progress sheets. In cases of loose stool or diarrhea, care must be taken to ensure immediate removal of feces and application of hydrating and protective substances in the perineal region.
Evaluation of Nutritional Aspects and Methods
Patients in the vegetative state often present with metabolic imbalances, such as increased metabolic processes, appearance of catabolic processes, alterations in the relationship among the different metabolic pathways, or water-electrolyte imbalances with resulting instability of vital signs [6]. Distinct strategies are required for stable patients, whose caloric requirements are estimated in the range of 40–50 kcal/kg/day, and cachectic patients, whose caloric requirement is 60 kcal/kg/day or more. Fat content is about 28 % of total caloric requirements. It should be noted that oleic acid is the most readily oxygenated among dietary fats and that glutamine is the most important amino acid for enterocytes, which use it as their principal energy substrate. Enterocyte glutamine metabolism constitutes the most important role of the intestine in the metabolism of nitrates, which are excreted as urea. Vitamins and minerals should be administered in excess of the daily requirement under physiological conditions. In patients in post-traumatic vegetative state, the autonomic system is highly stimulated, therefore favoring the occurrence of nonspecific phenomena (such as hyperventilation, hemodynamic changes, fever, hypertonus, and convulsions) that all call for increased metabolic requirements. On the other hand, hypothalamic-hypophysial damage can alter the neuroendocrine response significantly.
Attaining a proper metabolic balance is usually possible within a short time. The patient’s general state should be evaluated, however, also by monitoring the anthropometric (starting weight, periodic weight checks, tricipital plica, hydration conditions, and hydration loss) and laboratory (blood albumin, total proteins, transferrin, hemoglobin, creatinine, nitrate and glucose, creatinine clearance, etc.) indices.
Procedure for Body Weight Monitoring
Patients are weighed every 2 weeks in the morning (fasting), following a detailed procedure:
• Determine the scale net weight.
• Determine the weight of the wheelchair and safety belts.
• Remove the patient’s clothes and incontinence aids (urinary sac and diapers).
• Position the belt.
• Position the patient on the wheelchair using a lifting device.
• Weigh the patient.
• Dress the patient and document the weight data in the progress sheets, possibly also noting the presence of any rigidity or temporarily unmovable orthoses.
Feeding: Routes of Administration
The main routes of administration are through a central venous catheter, a nasogastric tube, or gastric tubes (percutaneous endoscopic gastrostomy, PEG). The route of administration and amount may vary according to the protocols in use in the unit, using either continuous or scheduled feeding protocols consistent with the circadian cycles. Enteral feeding eliminates the risks connected with the protracted presence of central or peripheral venous catheters.
Meals are given on a schedule and if possible in a habitual environment, which can contribute to the resumption of biological rhythms and relationship. Oral feeding should be attempted in all patients showing some awareness of swallowing and should be resumed when bronchial aspiration becomes a minimal risk. Small amounts of pureed and jellied food, preserves, and purees, should be administered first, as swallowing liquids remains a persistent deficit. If there is insufficient swallowing, a nasal tube should be positioned.
Procedure for Enteral Feeding
This procedure can be applied in the absence of contraindications such as regurgitation, vomiting, diarrhea, and if there are organic gastrointestinal problems. If patients are fed parenterally at admission, it is necessary:
• To position a nasogastric feeding tube or a PEG, with the patient leaning 30° backward.
• To suspend parenteral feeding progressively and start enteral feeding gradually, in accordance with the assigned quantities and quality.
It is advisable to shift from parenteral to enteral feeding starting with a maximum amount of 500 mL/day, to be increased on the basis of the assigned diet plan. The advised speed of feeding is 160–250 mL/h; in cases of gastrointestinal intolerance, enteral feeding can be discontinued for a few hours and then restarted at the lowest speed tolerated. After feeding, the tube must be cleaned with 50 mL of water, to be subtracted from the amount of total water allowed.
Treatment in the Gym
Gym treatment plays an important role in the day schedule of any patient in the vegetative state, and should include most of the exercises done during nursing care. However, the gym schedule should be tailored to each patient’s needs, with one therapist attending each patient (Fig. 7.2).

Fig. 7.2 Training the attention of the patient sitting in a wheelchair: first elementary signs of an oriented gaze
Passive Mobilization
At the start of treatment, mobilization can only be passive. Treatment can begin very early, as it does not interfere with any medical procedures and represents an effective method of patient care and prevention of neuro-orthopedic complications, while also helping establish channels for communication between the patient, the therapist, and the outside world.
Objectives
• To maintain movements of the joints
• To prevent contractions
• To prevent trophic cutaneous disturbances
• To stimulate proprioception
• To promote awareness, relationships and exchanges between the patient and the therapist
Passive mobilization of the joints should be carried out bilaterally several times every day, each time for at least 20 min. This needs to be done slowly, with the therapist talking to the patient and explaining to him or her which part of body is going to be moved.
Positioning
It is mandatory for the patient to be in an appropriate position, as this is believed to prevent the appearance of muscle tonic disturbances and spasticity and to avoid secondary complications. Changes from supination to pronation and from side to side are warranted. Positions can be maintained with the help of different types of orthosis made of foam rubber with thermoplastic elements, the position of which should be chosen to allow the least number of restrictions possible. Dynamic positioning is very useful – for example, when the limb is positioned on spring supports that allow sub-continuous, intermittent small movements of the joints.

Fig. 7.3 Exercise: rolling
Rolling
Rolling constitutes the most important physiokinetic therapeutic approach in the treatment of patients in the vegetative state, and is mostly indicated when spontaneous motion is absent. Mechanisms regulating rolling along the longitudinal axis have been described and depend on the activity of the interstitial nuclei of Cajal in the mesencephalon, which are very active during wakefulness. This is the first motor system that reaches full myelination, as early as in the sixth month of pregnancy, and it is responsible for fetal intrauterine movements. The axial and belt musculature is innervated bilaterally. The kinetic chain responsible for the movement sequences for rolling is therefore the oldest and the one that first appears in motor development. Passively, both superior and inferior belt transverse axis rolling is seen.
The patient starts from a supine position with trunk and head in axis, with the therapist adducting an upper limb (with the elbow being semi-flexed) while holding the shoulder and gently starting the rolling movement. It is important that the patient complete the kinetic sequence with movements of the automatic motor sequence. The same results are elicited with forced adduction of the thigh while the knees are bent (Fig. 7.3). Rolling exercises are useful for eliciting postural reactions, such as tonic and labyrinth reflexes of the neck or straightening reflexes. The therapist must simultaneously stimulate auditory and visual afferents in order to promote communication, stimulate attention, and call out functions relative to the body scheme.
Respiratory Treatment
The patient in the vegetative state frequently suffers respiratory problems. A series of pathological conditions develop that can induce secondary respiratory disturbances: immobility in bed (often in a fixed position with hardly any mobility of the ribcage, occasionally also due to rib fractures), bronchial stagnation, and susceptibility to infection, should all be considered. The resultant incapacity of the respiratory function, with greater production of secretions and alterations in the rhythm and depth of breathing, often accompanies serious alterations in gaseous exchange, hypo-oxygenation, and sometimes pneumonia due to stasis. Treatment strategies to diminish secretion stasis include techniques based on clapping, vibrations, and shaking when the patient presents with an insufficient cough reflex but there are no rib fractures – as many times a day as deemed necessary for sufficient drainage. Postural drainage is another technique used when the patient is properly stabilized. Staff must periodically change the patient’s position. Gradual verticalization of the patient should be attempted whenever the clinical conditions allow, with the aid of electric beds (see below) and then wheelchairs. The expansion of the rib cage should be improved as soon as possible by periodic mobilization of the upper limbs and by means of respiratory exercises that are able to lower the ribs and favor passive and (consciousness permitting) active expiration. A patented device that can be suitably attached to the tracheostomy cannula has been developed and is routinely used in some highly specialized centers. The device, based on a fitted diaphragm with changeable and progressively decreasing diameter, allows air inspiration only after a progressive increase in the inspiration strength and thoracic expansion. In this way, the patients who have gradually lost elasticity of the respiratory muscles over a period of months gradually recuperate by breathing against resistance and under controlled conditions, with monitoring of the number and depth of breaths, the PCO2, and gas analysis.
All patients who have undergone tracheostomy should be treated with humidification and aerosol therapy several times every day, and the condition of the large bronchi should be checked by bronchoscopy. In general, patients in the vegetative state are also monitored using a pulse dosimeter, and action is taken to maintain the peripheral oxygen saturation (measured from the finger or ear) at values of 95– 100%, with periodic check-ups with gas analysis.
Verticalization
It is important in the treatment plan for patients in the vegetative state and, if properly carried out, combines simplicity of exercise with a valuable treatment, while at the same time allowing the application of the treatment approach suggested by the “rules of thumb” (Fig. 7.4). Early positioning of the patient in an erect position, while still in the vegetative state, involves a series of considerations and serves multiple objectives.
Considerations
The upright position is the best condition for space exploration. The patient is helped to recover and readapt to seeing, grasping, and recovering the body orientation in space by means of which humans relate to the external world. In a vertical position, the four anatomical systems sustaining the state of consciousness are simultaneously involved and, in particular, are “synchronized” with the ipsilateral and contralateral primitive motor systems. The position also helps reestablish or recover the reflexes for straightening the head and trunk.
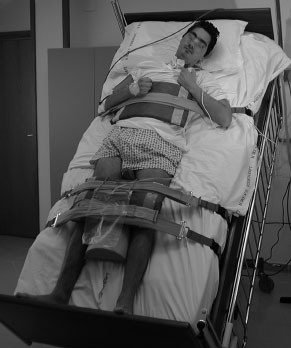
Fig. 7.4 Exercise: verticalization to help the patient explore the surrounding space
Objectives
• Verticalization helps prevent complications due to prolonged immobilization, such as deep vein thrombosis, and favors frequent changes of the patient’s position and body parts that suffer prolonged pressure from supports, stimulation from vessel receptors, reduction of smell stimuli, etc.
• It stimulates the mechanisms that regulate vegetative functions in a controlled way.
• Contraindications to verticalization include:
– Serious orthopedic problems that impede correct positioning
– Unstable vital signs
– Signs of neurovegetative alarm
– Endocranial hypertension

Fig. 7.5 In this position, the patient’s head is rotated toward the therapist, and monomodal stimulation can be started
Procedure
The following equipment is necessary: electric beds (for passive verticalization in the hospital room), static plan, standing device, dynamic standing device (for active verticalization in the therapy room). Accessories (such as elastic socks, belts and straps to hold the patient, foam rubber aids and sand-filled bags for positioning) should be prepared. The vital signs need to be monitored continuously during verticalization.
Methods for Verticalization
• First position the patient in a supine position with the body properly in axis.
• Position wedges beneath the trochanters to avoid lateral rotation of the lower limbs and to improve supination of the feet.
• Place a foam or rubber pillow in the popliteal cavity to prevent hyperextension of the knees.
• Position the feet at 90° onto the lower board of the verticalization bed.
• Apply a strap around the thorax to prevent anteroflexion of the trunk and at the knee level to avoid flexion of the legs.
• Check that the positioning does not produce compression of vessels or nerves.
Following this type of arrangement, the patient can attain complete verticalization (up to 90 °) progressively within 4–5 days. Verticalization treatments should be 30 min long at the beginning, progressively increasing up to 1 h (whenever possible), and should be performed several times every day at approximately the same time. The therapist (who must also prevent the patient’s head from falling onto the chest) stands on one side of the patient, calming the patient by explaining the treatment or using tactile stimulation, and monitors the vital signs. Once the patient is relaxed, his or her head is turned over to one side, and a monomodal stimulation is performed (Fig. 7.5). The treatment can be performed simultaneously in several patients, providing a “mirror” effect that is therapeutic in itself. In the absence of other patients with indications for this treatment, a mirror placed in front of the patient during the treatment serves the same purpose and is as effective.
After a verticalization treatment, the horizontal position should be reached gradually (within about 10 min). If neurovegetative alarm reactions occur, horizontalization should be started over again after normalization from the last tolerated angle. The therapist must report in the progress sheets the duration of treatment, degree of verticalization reached, and all the observed changes in vital parameters or mimicry, as well as all responses obtained during the treatment.
Hydrotherapy
Hydrotherapy has been widely used for several years in the rehabilitation of deficits due to various neurological disorders. In patients in the vegetative state, hydrotherapy is the method of choice for obtaining muscular relaxation and a natural psychophysical condition of well-being. It is easily accepted by patients and therapists and represents a simple way of gradually increasing communication without excessive costs or requirements for complex equipment. In addition, hydrotherapy has trophic effects that go beyond reestablishing neurovegetative balance, and produces slight peripheral vasodilatation (with increased peripheral distribution of oxygen and nutrition) that is compensated for by the peripheral blood pressure with a resulting increase in venous return. It should also be noted that floating and hydrostatic effects promote stimulation of motor responses otherwise unobtainable (Fig. 7.6).
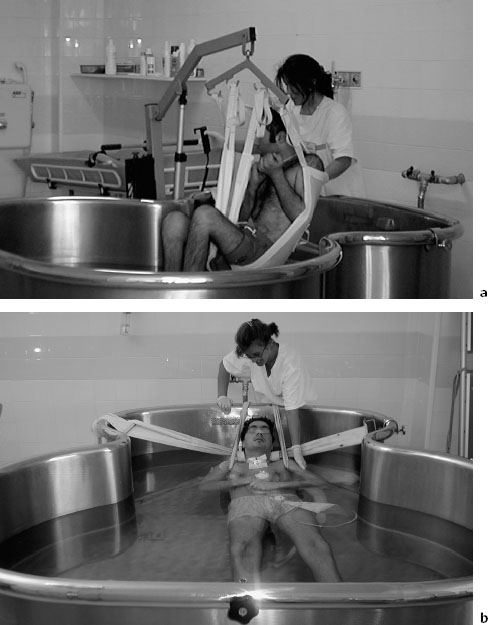
Fig. 7.6a, b Relaxation suitable for facilitating simple responses is best obtained by exercising the patient in the swimming pool at 32 °C
Equipment Needed
• A pool or (in case of space limitation) a butterfly tub, with water at body temperature and with no variations in the external microclimate
• Electrical lifting device, complete with pouch
• Tub cleaning, with local disinfection with liquid products and ambient disinfection with UVA for 12 h
• Attending staff in charge and possibly assisted and helped by family members
Absolute contraindications to hydrotherapy are hyperthermia and serious hypertension or hypotension. Localized infective lesions and psychomotor agitation are relative contraindications, which should be evaluated in each case.
Treatment Methods
The total duration should be about 1 h, with an optimal frequency of three sessions or more every week. For the first 15 min of treatment, the therapist should encourage relaxation in the patient and improvement spastic hypertonia; then passive mobilization and inhibitory maneuvers are performed for about 20 min. Every movement performed is first explained to the patient while touching the part of his or her body that is to be mobilized. This has a calming effect and is favorable for the patient, who has to obey simple commands aimed at obtaining motor responses and maximal limb movements. Orders are given in expectation of a response. In general, the first effects obtained are a change in the patient’s facial expression, together with a reduction in the pathological body posture.
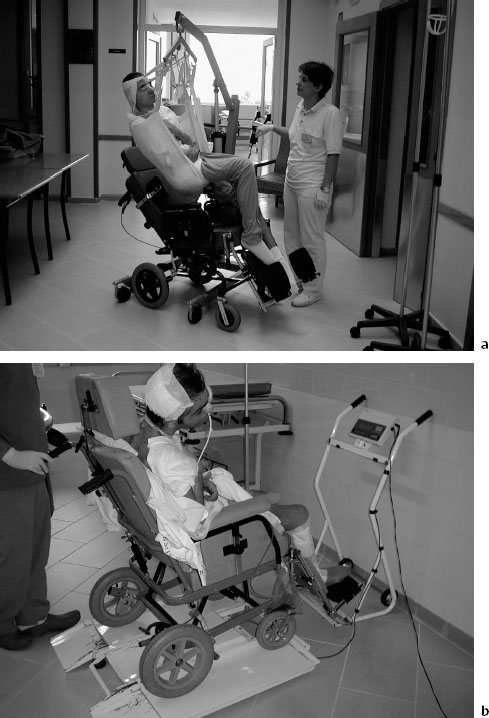
Fig. 7.7a, b The therapeutic effects of positioning the patient in a wheelchair are detailed in the text
Positioning the Patient on the Wheelchair
Positioning the patient on the wheelchair is basically a continuation of the rehabilitation treatment. There may be substantial differences between patients and they may require different types of assistance. Patients with cerebral lesions often require continuous monitoring of vital signs over long periods of time, which keeps the patients linked to monitor devices even in the wheelchair.
Why put a patient in the vegetative state in a wheelchair? The main purposes are to achieve improvement in or encourage the appearance of attentive functions, to stabilize and gradually achieve control over trunk posture and movements, to start the ipsilateral and contralateral primitive motor systems functioning, to reorganize the system regulating pressure and the vestibular system, to establish new proprioceptive inputs and conjugated gaze in the vertical position, to reduce the risk of decubital sores, to achieve better drainage of bronchial secretions and improve lung capacity, to allow a different body response to gravity, to improve sphincter functions (defecation, miction), and to reduce regurgitation due to esophageal sphincter insufficiency. The expectations (sometimes excessive) of the patient’s family, who are able to see improvements as a pathway leading to a possible recovery (Fig. 7.7), are also satisfied. It should also be noted in this regard that adequate positioning of the patient on the wheelchair (with proper pressure on the seat, wedges and containing or corrective bands) is a fundamental step in achieving improved balance for posture and movement [7,8].
Clinical conditions, joint impairment, and the existence of cutaneous lesions should be taken into proper account so as to give the patient the correct position in the wheelchair. The use of buckles and belts should always be discouraged, unless warranted by a state of psychomotor agitation and the need to limit the patient’s movements in or from the chair. The trunk is the main source of stability of the body and is therefore fundamental for correct movements of the head and limbs [5]. Inadequate alignment of the vertebral column affects the trunk and creates compensatory curves, which may erroneously be corrected at the cost of other sections of the column and with other resultant deviations. optimal distribution of the weight over a wider base is also important, and extensive or excessive pressure against the ischial tuberosity and sacral bone should be avoided. Once the trunk is realigned with the pelvis, the base of support changes, with a resultant equal distribution of weight between the ischial tuberosities, thighs, and the feet. Combining all the elements and finding the best position for each patient’s numerous requirements also needs imagination and creativity on the part of staff. It should be noted how tolerance and comfort in the wheelchair may become fundamental. Chairs with rigid backs and providing a solid base are preferable to “very comfortable” chairs, which according to reports by several physicians can even favor the development of decubitus sores. Pillows on solid bases can be provided at a later time.
The normal position of the trunk is the erect posture, with a slight anterior pelvic inclination and the weight equally distributed on both ischial tuberosities. Any incorrect positioning of the patient will cause flexion of the trunk and pelvic rotation (most likely backward), resulting either in scoliosis, an accentuated lateral inclination, or flexion of the thigh on the pelvis. Possible adverse effects of inadequate positions are decubitus sores, thoracic restraint with reduced ventilation and respiratory difficulties, decreased visual perception of the environment, proprioceptive and vestibular changes, antalgic posture and tension in the back muscles, and pain in the joints. A common method of preventing the patient from sliding off at the front is to hold the pelvis against the back of chair with a bilaterally adjustable belt on the pelvis or thighs. With regard to lateral trunk and pelvic inclinations, it is preferable to use wedges (three-point system) and supports placed on both parts of trunk to balance the angle. Also useful are support systems for the thighs (Fig. 7.7). On occasions, it may be necessary to produce a disparity using foam or rubber pillows (about 5 cm or thicker) positioned beneath the pelvis on one side, possibly with a softer pillow positioned contralaterally.
The alignment of the head with the trunk should also be taken into account, to avoid abnormal tonic reflexes in the neck. A collar supporting the head can be used, but may cause chin lesions, dysfunctions of the temporomandibular joints, and lesions on the sides of the neck. Wide straps placed between the forehead and a support on the chair are preferred. The latter arrangement is less traumatic but also less efficient, as the belts often tend to slide away, sometimes also covering the patient’s eyes. Using slight angulation of the back of the chair also does not resolve the problem completely. Rigid lateral supports, similar to headrests, are sometimes used, but often cause microlesions or macrolesions on the temples and ears. A great deal of attention needs to been given to the contact between the occipital region and the support, which should be lined with a satin-type material, sheepskin fleece, or a similar material to avoid abrasions and alopecia due to friction. A support at the back of the head also minimizes muscular tension in the neck (Fig. 7.8).
With regard to the pelvis, the best position is flexion at about 90°, with abduction and spontaneous femoral rotation, which in turn influences trunk alignment. Excessive flexion of the upper hip at angles of more than 90° often depends on spasticity of the flexor muscles and warrants careful positioning with the knees higher than the pelvis, as obtained by reclining the back of the seat. A quite frequent problem is excessive femoral abduction and external rotation, with skin irritation and possible lesions due to tights continuously rubbing against the wheelchair metal. This is generally avoided by providing padding along the sides of the thighs. An abducted or externally rotated thigh, with the other one adducted and internally rotated, or a retracted limb and difficulties in the alignment of the limbs are also common observations. In particular instances, it may become necessary to construct appropriate structures to maintain an optimal joint position. Such structures are usually made out of rigid plastic, wood, foam rubber, plaster, etc. Correct positioning of the feet on the footrests should never be neglected, and abnormal positions should be corrected whenever possible.

Fig. 7.8 A wheelchair and implements allow appropriate positioning of the head and trunk, while at the same time reducing muscle tension
The upper limbs pose different problems, depending on whether the paresis is flaccid or spastic. A flaccid limb requires adequate support, which also prevents subluxation of the shoulder, a frequent complication in the vegetative state. This disturbance must be cared for with functional electrical stimulation (FES) in addition to the use of figure of eight-shaped ortheses and dynamic or- theses. In general, patients with spastic upper limbs have little benefit from the use of restrictive devices, which instead are counterproductive and aggravate the already abnormal motor model in some cases. It is preferable to approach the problem on the basis of the limb’s potential range of motion, its functional limitations, and the extent to which these may alter the entire alignment with the trunk [9]. Customized structures can be made using padded arms, which reduce the risk of skin lesions without interfering with correct positioning. It is also important to note in this regard how important it is to train physicians, physiotherapists, and any other health professionals involved with patients in the vegetative state to carry out accurate observation. One must ensure an ability to foresee potential future needs, progressive clinical and functional changes, and one must adapt any corrective treatment from time to time to suit each individual patient.
Treatment of Swallowing Disturbances
The total or partial loss of the physiological ability to swallow and the resulting inability to eat are common among patients in the vegetative state, especially in those presenting with serious medical conditions. Swallowing problems may be critical and may need to be dealt with by experienced professionals. Both the evaluation of swallowing disturbances and their treatment require a small, dedicated team, which should be organized by the attending physician with proper expertise and equipment (possibly also including fibrobronchos-copy and video fluoroscopy; see p. 108). Video fluoroscopy (which can only be carried out in cooperative patients) allows direct viewing and photographic documentation of possible malformations and pathologies in the oropharynx. It provides indications about the tracheostomy cannula and whether it is possible to remove it when the patient has an adequate laryngeal reflex according to the physiotherapist’s and nurse’s observations. The most frequently observed deficits are: lost or inadequate control of tongue movements, reduced esophageal peristalsis, and uncoordinated chewing movements. Primitive motor schemes, including mastication, sucking, lockjaw, and facial spasms are also observed in the first 3–4 months. Many patients already have a nasogastric tube or PEG in place. A reflex swallowing mechanism can often help in the vegetative state, as food placed in the proper position at the back of the pharynx triggers reflex swallowing movements and allows natural feeding. Some risks nevertheless exist, and anamnestic or direct knowledge of possible fractures of facial structures, respiratory disturbances, or food intolerance may be helpful. The position of the head and primary airways is important. The patient should be seated, with the trunk perpendicular to the seat plane, and the observer should continuously check for facial asymmetries (indicative of deficits of the involved musculature), changes in mimicry or respiration, or hypersalivation [10,11]. Forward flexion of the head is frequent in tracheostomized patients. In other cases, the head is forced to one side or hyperextended which makes evaluating the swallowing reflex a complex and sometimes difficult procedure, even when the therapist can manually move the head.
A proper examination must also include an accurate evaluation of head, neck, and trunk control in order to devise a treatment plan; information on whether the patient can be seated in a chair for feeding is important, for instance. The strength and mobility of perioral structures should be examined, and opening and closing of the patient’s mandibles should be evaluated in order to establish whether food can be introduced into the oral cavity. The jaws open as wide as 35 mm in healthy subjects, with a lateral displacement of about 10 mm, but these figures are significantly reduced in patients with the bulldog reflex.
The physiotherapist is often confronted with patients who show signs of serious regression, such as a bulldog reflex, oculo-oral reflex, automatic sucking, mastication, teeth gritting, etc. The persistence of these signs (see p. 32) beyond 200 days after trauma is generally indicative of severe impairment. In patients in the vegetative state who show a bulldog reflex, for example, there is a considerable reduction in the capacity of the mouth to open. All these factors contribute to residual food remaining between the teeth and cheeks, or to an inability to keep food in the oral cavity. The strength of the muscles closing the mouth should also be evaluated (as it impedes hypersalivation). Possible imitations of visual or oral commands must be checked for. We also evaluate intraoral sensitivity to tastes by means of a pad moistened with flavored water and observation of changes in mimicry. Proper evaluation of the teeth and tongue is important too, as is the examination of the soft palate and posterior pharynx (often difficult in patients in the vegetative state). Presence of the cough reflex must also be noted.
The success of any program for the rehabilitation of swallowing depends on several variables and requires above all a proper, attentive observation of the responses to different types of stimulation. A specific position, an abnormal movement, any change in facial expression, and any other sign, can indicate that a stimulus can be perceived by the patient as abnormal, harmful, or bothersome in some way (the response to a stimulus can be delayed). Often, the rehabilitation of swallowing begins with delicate maneuvers, such as caresses on the cheeks with a cloth dipped in cold or tepid water, which are thought to help the patient relax (see the “rules of thumb,” p. 89). Lips, and at times gums, are gently stroked with sterile pads or a tongue depressor. Firm pressure on the masseter muscles can be useful to obtain relaxation and opening of the lips in case a bulldog reflex appears. A tongue depressor or a gauze pad inserted between the teeth will encourage progressive opening of the mouth; this exercise in regulating muscular tone can be associated with pressure on the masseter muscle and needs to be repeated several times every day. Passive mobilization of the tongue in different directions is carried out using a velvet glove.
Evaluation and Treatment of Spasticity
Spasticity is frequent in patients suffering from neurological pathologies, especially those in the vegetative state. It is regarded as a type of hypertonus, an alteration of movement in which hyper-activity of tendon responses results from increased excitability of the normal stretch reflex and muscular tone. The distribution most commonly observed in patients with serious cranial trauma includes plantar flexion of the foot, elbow, wrist, hand and fingers, and flexion of the hip (very frequent) and knees. Hypertonus of the adductors is common and interferes with correct posture in bed or wheelchair. Hyperadduction of the shoulder and internal rotation of the arm impede cleaning and dressing. According to several authors, spasticity is also a major factor contributing to the development of heterotopic ossification (periarticular new bone formation, PNBF).
Treatment of Spasticity
As a general rule, spasticity should be treated after proper and detailed evaluation and based on a treatment plan precisely matching the patient’s requirements [12]. Treatment for spasticity is required in the following conditions:
• When it limits the range of passive mobility of a joint or limb.
• When prolonged forced postures produce or favor decubitus sores, deformities, and notable difficulties in everyday hygiene.
• When it is necessary to prevent complications (pes equinovarus, pes equinovalgus, etc.).
• When small movements (otherwise hidden) used by the patient for communication need to be promoted and enhanced.
Treatment is based on physiotherapeutic, pharmacological, and physical measures.
Physiotherapeutic Measures
Highly competent physicians, nurses, and physiotherapists need to work together. Every stimulus potentially increasing reflex hypertonus and all sources of friction potentially damaging the skin should be avoided by proper positioning. An initial measure to be taken is passive muscle stretching, based on a suggested mechanism increasing central inhibiting processes, at least transiently. In general, the spasticity of a limb depends more on the agonist than on the antagonist muscles. Reinforcement of antagonist muscles may help reduce the tone through reciprocal inhibition. Passive mobilization of a spastic limb is known to produce changes in the neurophysiological responses of the central nervous system [12,13]. A good residual function of the joints is also important for controlling hypertonus. Plaster casts, preventive splints, and the like are not always accepted and tolerated by patients in the vegetative state. These preventive measures should therefore be of limited use or may become harmful in case of neurovegetative reactions, with a return of the initial condition of deformity after they are removed.
A second step in the rehabilitation of spasticity is an attempt to restore a postural realignment opposing gravity. A reflex decrease in spastic muscles can be obtained by applying warm or chilled water or comparable means. Vibration or electrical stimulation are occasionally used to strengthen on inhibit tonus of the agonist or antagonist muscles [14]. The muscle tone also changes in relation to different head, trunk, and body positions in space. In patients in the vegetative state, primitive reflexes (such as straightening reflexes, symmetrical and asymmetrical tonus of the neck, parachute reflex, stumbling, etc.) are often exploited to help treat spasticity. The use of electromyography (EMG) bio-feedback remains limited to awake patients with sufficient cognition and collaboration.
Magnetic pulse stimulation is used although with little effect. All physical treatments alone are absolutely useless for controlling spasticity, with the exception of the good results obtained with hydrotherapy (see above). This method allows maximal relaxation lasting several hours, a period during which the patient in the vegetative state is freed from the prison of spasticity and can often respond to treatment with an initial motor response.
Pharmacological Therapy
The cerebral or spinal origin of spasticity determines the choice of medication based on the sites and mechanism of action. Often, medications need to be administered in combinations and, unfortunately, may interfere with wakefulness and cognitive processes, or may induce side effects. The optimal dosage always depends on weight, metabolism, and the tolerance of individual patients and should be tailored, with titration in case of side effects. Improvement can be appreciated at dosages high enough to guarantee efficacy in the absence of side effects. The most commonly used medications are:
• Baclofen. This is an analog of γ-aminobutyric acid (GABA) that binds to GABAergic receptors, thereby inhibiting monosynaptic and polysynaptic reflexes and the activity of the neuromuscular junction. The therapeutic dose is in the range of 10–75 mg/day. Side effects include sedation and confusion.
• Dantrolene sodium. This compound acts peripherally at the muscular level, where it interferes with calcium release from the sarcoplasmic reticulum. The main side effects are sedation, nausea, and a rise in hepatic enzymes. The therapeutic dose varies from 25 to 400 mg/day.
• Diazepam. This facilitates the effects of GABA at the postsynaptic level. Side effects include sedation, etc. The therapeutic dose varies between 4 and 40 mg/day.
• Clonidine. This has a main central action as the adrenergic agonist of α2-receptors and inhibits spinal reflexes, through mechanisms of action that are still poorly understood. Side effects include lethargy and orthostatic hypotension. It can be administered transdermally at doses between 0.05 and 0.1 mg.
• Tizanidine. This is a noradrenergic α2-agonist, which shares the side effects of clonidine but is in general better tolerated, at doses of 4–36 mg/ day.
Alternative Techniques, Routes of Administration, Neuromuscular Blocking
Several compounds have been used for some years now to obtain partial relief of spasticity.
Anesthetic block. Distinct approaches can result in a temporary, local blocking of conduction, such as 1–2 % lidocaine in water solution, 0.25 % or 0.50 % bupivacaine and mepivacaine. Procaine has proved less reliable, is difficult to obtain as a commercial product, and acts on both afferent and efferent fibers. In general, the nerve trunk to be injected is located by transcutaneous electrical stimulation (for 30 min, four times a day) with square waves at a current intensity of 1 mA. This stimulation provokes a strong muscle contraction, signaling that the stimulating needle is close to the nerve; alternatively, the drug can be injected at the nerve ending of the muscle.
Neurolysis is a similar technique, much less popular today, using phenol and ethyl alcohol [14,15]. Phenol is used at a concentration of 2% or 7%, with effects lasting longer after administration at the 7% concentration. It can also be injected, at doses depending on the size of the muscle and with electromyography monitoring; the result is a transient loss of spastic contraction. It should be noted that phenol toxicity (convulsions, arrhythmias, and cardiocirculatory collapse, as with all anesthetics at high doses) is to be expected after administration of approximately 1 g. It can also be injected at the nerve ending to produce a localized effect. Inflammation often develops at the injection point.
Ethyl alcohol is injected, at a concentration of about 45% in water solution, into distinct muscle areas and acts by causing degeneration of the muscle tissue. This effect last for about 1 year in patients in the vegetative state, due to the lower tissue regeneration compared to phenol.
Botulinum toxin. There is a growing consensus for this method, which has limited risks of a deafferentation syndrome. Botulinum toxin binds at postsynaptic neuromuscular receptors and is up-taken for reuse [16]. Several types of toxin (A, B, C, etc.) have been isolated from Clostridium botulinum, and all cause neuromuscular blocking by interfering with acetylcholine release at the distal nerve ending. Injections are administered under electromyographic control in the muscle body and nerve ending, at doses varying according to the muscle and protocol used. In general, one to four inoculation sessions are carried out. The lethal dose is about 40 U/kg, and doses not exceeding 300–400 IU can therefore be safely used in single sessions. When administered correctly, side effects are absent and the first effects are observed after 24–72 h, with a maximum effect after about 1 month and a duration of 3–4 months [16–18].
Physiotherapy or orthotherapy and occlusive bandages (favoring muscle stretching and larger toxin diffusion) improve efficacy, with repetitive stimulation increasing the toxin action and reducing the time span between inoculation and clinical results. Occlusive bandaging must be repeated after administration of the botulinum toxin and changed at least once per day for at least five or six consecutive days, while repeated stimulation varies in different institutes in the range of two to three times every day for 4–5 days after toxin administration. Antibodies are produced over time; these reduce the effect and have encouraged the isolation of new types in recent years. This method is unfortunately quite expensive, and the purified toxin must be conserved at low temperatures. In addition, the physician also must be competent in electromyography and neurophysiology.
Careful selection of candidate patients for botulinum toxin administration is important. The time window for expected toxin efficacy is in the range of 3–12 months from the appearance of spasticity, and should be relied on especially in cases of spasticity with flexion of the upper limb, elbow, and fingers of the hand. The main muscles to be treated are the biceps, brachioradialis, radial flexors, ulnar of the wrist, superior flexor of the fingers, pronator teres, etc. The adductor pollicis is always treated when holding movements need to be improved.
Orthopedic Surgery
There are important surgical procedures that can help reduce excessive contraction. In general, tendon elongation is sufficient to reduce the muscular tone, as well as possibly balancing forces. It is also used to correct functional deficits resulting from spastic contraction and the resulting abnormal posture. The most common techniques are: tendinoplasty, split anterior tibial tendon (SPLATT), lateral transposition of part of the tendon of the anterior tibialis muscle, tenotomy, arthrodesis, and osteotomy.
Neurosurgical Measures
The neurosurgical approach is complex, unreliable, and requires expert and dedicated personnel. It is therefore unusual in treatment and restricted to cases that are absolutely refractory to other therapies. One relatively common approach that has been in use for several years now is anterior and posterior rhizotomy [5]); the DREZ-otomy (dorsal root entry zone) is no longer used [8]); myelotomy and electrical stimulation of the spinal cord are also used.
A method that has acquired popularity in recent years is intrathecal administration of baclofen using a controlled-release pump implanted under the skin. This method is generally used when others have failed or when spasticity is diffuse [19]. An administration test is first carried out with an intrathecal baclofen reservoir after evaluation using the Aswort Scale. Administration is usually with 0.25 μg baclofen diluted in 1–2 mL saline, to be increased to a maximum of 1.5 μg within 3 days. If an improvement of at least two points on the Aswort Scale is seen within 2 h after administration, the next implantation is done. Unfortunately, baclofen can cause notable and dose-related side effects, including sleepiness, epilepsy, and exceptionally sudden death. One positive side effect, in the form of a remarkable attenuation of neurovegetative reactions, especially sweating, is frequent [20]. Appropriate equipment allows reprogramming of the pump to administer smaller or larger doses as needed. The results are relatively good in patients with spinal spasticity, with a variability of efficacy among patients in the vegetative state that requires further evaluation.
Heterotopic Ossification
A frequent complication among patients in the vegetative state is the abnormal formation of osseous tissue around the joints, that begins around the second month after head injury and blocks joint and musculature in a spastic contraction. The most common sites are the shoulders, elbows, hips, and knees. Contractures in flexion are often associated with the condition, and aggravate osseous neoformation. The etiopathogenesis is unknown (see p. 71), and not all patients are affected. Alkaline phosphatase is often elevated in the affected patients, without any observed relationship with the extent of heterotopic ossification. Radiographic examination demonstrates friable tissue of lower density, which expands around and within the joint space.
At present there are no valid pharmacological or physical treatments for reducing heterotopic ossification once it has developed, and no results are obtained by physical therapies such as ultrasound, radar, etc. Diphosphonates can prevent its formation but not block its growth. Passive manipulation is again an option for delaying ankylosis. Once osseous neoformations have formed and developed excessively within a time span of 12–15 months, surgical resection is indicated (earlier surgery should be avoided due to the risk of additional heterotopic ossification).
Management of Tracheostomy Patients in the Vegetative State
Paolo Scola
Tracheostomy has been used with increasing frequency in recent years, due to its efficacy in providing better ventilation and easier control on the respiratory functions and the development of simpler and safer surgical procedures. It becomes necessary (after a variable period ranging from 3 to 15 days in different institutions) whenever patients cannot correctly perform the distinct phases of spontaneous breathing.
A wide range of tracheostomy cannulas are available. A cannula selected to suit the needs of patients in post-traumatic vegetative state should have the following characteristics:
• It should have no cap, in order to avoid decubitus sores from mucous membrane.
• It should have an interchangeable countercannula.
• It should be made of a flexible and thermosensitive material that can adapt to the patient’s anatomy and reduce the risk of encrusted secretions.
• It should be movable both horizontally and vertically.
• It should have flanges of minimal thickness for patients whose neck is short.
• It should have a diameter allowing easy management of the upper airways and occlusion compatible with phonation later on.
Countercannula Disinfection
The flowchart for disinfection of the countercannula includes substitution three times a day in order to avoid infections and occlusions caused by bronchial secretions. Countercannulas should be soaked in H2O2 for at least 15 min and then washed under running water, cleaned with a special brush, and then soaked in a suitable disinfectant solution for at least 2 h before being dried up with sterilized gauze.
Inhalation
Tracheostomy tubes increase bronchial secretions, partly due to the altered activity of the ciliary and mucous membrane of the trachea and partly because of the absence of the nose’s protective functions such as filtration and humidification. Aspiration of tracheobronchial secretions is a basic maneuver that reduces slackness in the tube and the risk of respiratory infections, while ensuring accessibility to the upper airways. It is also a maneuver that in itself can potentially promote infections, however, and should be performed with adequate aseptic technique. Tracheostomy should be performed rapidly, when the patient’s physical examination reports cough and production of abundant expectoration, and it should be as non-traumatic as possible. These goals are achieved when the aspiration pressure does not exceed 250 mmHg and the duration does not exceed 30 s. After careful introduction, the probe must be rotated to avoid adherence to the mucous membrane and injury to it. Aspiration can start only after the probe has been completely introduced. Correct hydration of patients and adequate humidification of the environment are factors affecting the quantity and fluidity of bronchial secretion; a direct spout and humidifiers are useful for this purpose, and can help keep secretions fluid and facilitate expectoration. Use of aerosol therapy and mucolytic compounds is common; in our experience, mesna for endotracheal instillation has proved a good choice.
Swallowing
Tracheostomy interferes with the swallowing mechanism; rehabilitation is often disturbed by dysphagia induced by the tracheal cannula, which impedes elevation and shifting forward of the larynx. On the other hand, a cannula protects the airways against aspiration pneumonia and allows the removal of any material that has been aspirated accidentally.
Fibrotracheal Bronchoscopy
A periodic examination of the upper airways and trachea (every 6 months) is advisable in patients in the vegetative state, as it allows observation of the larynx plane and the bronchi underneath it and evaluation of the morphology and the patient’s breathing and swallowing.
Complications
Most complications are associated with the cap pressure from the orotracheal tube and cannula. The mucous membrane in the trachea is damaged by pressure greater than 30 mmHg, which causes ischemia. Tracheomalacia or granulation tissue protruding into the tracheal lumen can develop when there is necrosis of the cartilage rings. Stenosis, the most feared complication, can develop after physiological repair mechanisms, and may become clinically evident only when the lumen is reduced to one-third. Tracheoesophageal fistulas require surgical treatment and the positioning of a stent.
Cannula Removal
In patients in the vegetative state, the cannula should be removed as one of the first steps in the rehabilitation treatment plan. For obvious reasons, the cannula should always be removed following a flow-chart based on a specific sequence. The basic criteria for starting the process of removing the cannula are:
• At least 250 mL expired air volume/min measured by spirometry (Wright manometer)
• Values in the physiological range on blood gas analysis
• Values of blood electrolytes (including Mg) within the physiologically normal range
• Fibrotracheal bronchoscopy estimate (tested through stoma and nose) in the physiological range
• Active and efficient swallowing is not necessary at this point
Occlusion modalities:
• Two blood gas analysis recordings need to be performed, at the baseline and at the end of each occlusion process, respectively.
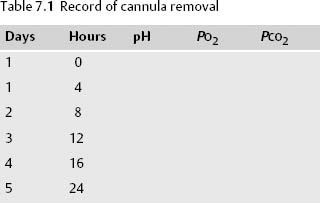
• Occlusion is performed for progressively longer periods of time (e.g., 4, 8, 12, 16, and 24 hours on five consecutive days). Blood gas analysis is carried out at the end of each occlusion procedure and recorded in a special chart (an example is shown in Table 7.1).
• O2 saturation needs to be continuously monitored; if any breathing problem appears during occlusion, blood gas analysis must be performed immediately and occlusion suspended if necessary.
References
7. Letts RM. Principles of seating the disabled. Boca Raton, FL: CRC Press,1991.
10. Lazarus CL. Swallowing disorder after traumatic brain injury. J Head Rehabil 1989; 4: 34, 1989.
< div class='tao-gold-member'>








