Stroke and Cerebrovascular Disorders
Sean I. Savitz
▪ INTRODUCTION
Stroke results from occlusion or disruption of a blood vessel feeding the brain and has been popularly and incorrectly referred to as a cerebrovascular accident (CVA). Stroke is no more a CVA than a heart attack is a myocardial accident. Strokes present suddenly, in many cases without warning. The effects of stroke are often devastating, and for many patients stroke irrevocably changes their life. It is the leading cause of adult disability, the second cause of death worldwide, and, for certain types, a treatable condition within 3 hours of symptom onset.
▪ EPIDEMIOLOGY
No one is spared from potentially having a stroke, which can occur in any age group. The incidence of stroke is higher in the older population because of accumulating and predisposing vascular risk factors over time, including hypertension, diabetes, and hypercholesterolemia. Young patients are at risk for stroke if they have cardiac abnormalities (e.g., patent foramen ovale), experience arterial dissection from trauma, or are hypercoagulable from genetic or medical disorders.
▪ RISK FACTORS
The nonmodifiable risk factor for stroke is age. Modifiable risk factors are hypertension, diabetes, smoking, obesity, and increased cholesterol level.
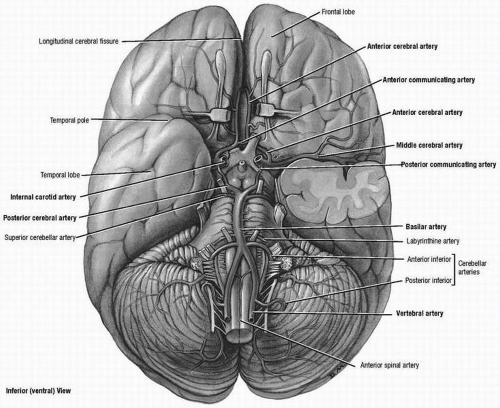
The brain is supplied by anterior and posterior circulations. The vessels for both circulations join at the circle of Willis at the base of the brain. The anterior circulation is fed by the internal carotid arteries (ICAs), which give rise to the middle cerebral artery (MCA) and the anterior cerebral artery (ACA). The posterior circulation is composed of the vertebral arteries joining to form the basilar artery, which gives rise to the posterior cerebral arteries (PCAs) (Fig. 20.1).
There are two major types of stroke—ischemic stroke and intracerebral hemorrhage. The former accounts for 80% of all strokes and the latter for 20%. Each condition is described in detail in the following sections.
▪ CEREBRAL ISCHEMIA
Ischemic stroke is classically defined as damage to the brain because of substrate (glucose) and oxygen deprivation. It is caused by either an occlusion of a large or small vessel feeding the brain or decreased cerebral arterial perfusion. The mechanism or cause of ischemic stroke can be described in four categories—embolic, atherothrombotic, small vessel, and hypoperfusion.
Embolic Stroke
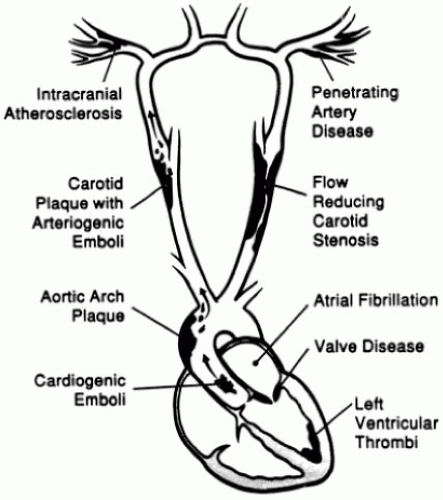
Vessel occlusions are most often due to emboli that have either formed on top of an atherosclerotic plaque or originated and traveled to a cerebral vessel from a proximal site such as the heart. Emboli stick and dock along the endothelial surface and thereby block cerebral blood flow. Figure 20.2 shows the most common origins for emboli in the cerebral circulation.
Atherothrombotic Stroke
Atherosclerosis builds along the vessel wall throughout life in the extracranial and intracranial circulation. In Western society, plaque accumulates in the extracranial carotid and vertebral arteries. Platelet-rich thrombi can form within the plaque and obstruct blood flow.
Small Vessel (Branch Artery or Penetrating Artery Disease) or Lacunar Stroke
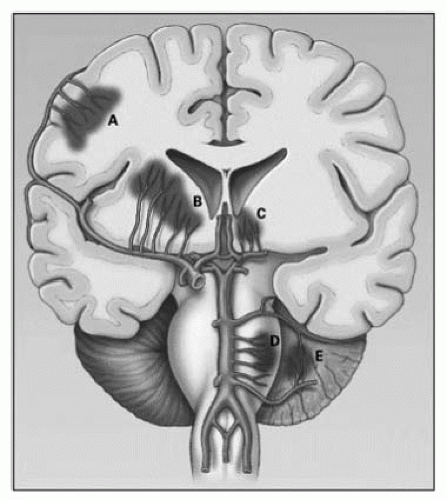
The penetrating arteries that branch off the large cerebral vessels (Fig. 20.3) can degenerate over time, leading to distal narrowing. This may be due to chronic hypertension or atherosclerotic plaques in large parent arteries that block the orifices of the small branches. Arterial occlusion leads to small infarcts called lacunae, which is from the French term for “small lakes.”
Hypoperfusion
Low cerebral perfusion can cause global ischemia of the entire brain or focal ischemia within a tight artery feeding a specific part of the brain. Most common causes include hypotension and systemic hemorrhage.
Pathophysiology
Under ischemic conditions, neurons can no longer generate adenosine triphosphate (ATP), which leads to cell membrane failure and rises in extracellular glutamate. A complex array of interconnected signaling pathways is unleashed, termed the ischemic cascade, which ultimately leads to degeneration of brain cells. The ischemic cascade includes glutamate excitotoxicity,
intracellular calcium overload, oxidative stress, apoptosis, and the inflammatory response, all of which in combination result in widespread neuronal, glial, and endothelial cell death. The entire neurovascular unit breaks down, and cerebral edema (both cytotoxic and vasogenic) soon ensues, contributing to the damage.
intracellular calcium overload, oxidative stress, apoptosis, and the inflammatory response, all of which in combination result in widespread neuronal, glial, and endothelial cell death. The entire neurovascular unit breaks down, and cerebral edema (both cytotoxic and vasogenic) soon ensues, contributing to the damage.
Clinical Stroke Syndromes
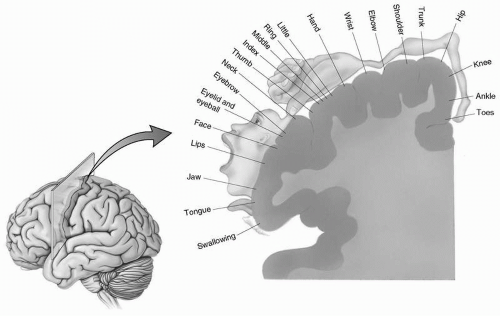
Strokes cause various deficits depending on where they occur in the brain (Fig. 20.4). Classic stroke syndromes resulting from occlusion of specific blood vessels are described in the following section.
Internal Carotid Artery
One of the most localizing signs for internal carotid artery (ICA) occlusions is transient monocular visual loss (amaurosis fugax) caused by ischemia of the retinal artery, which derives from the ophthalmic artery, a major branch of the ICA. ICA occlusions also can cause ischemia in the ipsilateral cerebral hemisphere that often mimic ischemia within the MCA territory but can also cause complete infarction of the anterior circulation, a devastating stroke that leaves the patient paralyzed on the contralateral side with hemianopsia and aphasia (if left hemisphere) or neglect (if right hemisphere).
Middle Cerebral Artery
Occlusion in the MCA typically can cause a mix of signs depending on whether the superior or inferior division of MCA or both is affected.
Signs that occur in the superior division are weakness of the face and arm and sparing of the leg, along with hemisensory loss, Broca’s aphasia (if left hemisphere), and neglect (if right hemisphere).
Signs in the inferior division are contralateral visual field deficit, Wernicke’s aphasia (if left hemisphere), and visuospatial impairments (if right hemisphere).
Anterior Cerebral Artery
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree