Patient
Age
No. of previous surgeries
Size 1st op (cm)
Tu. types
Grade resection last surgery (%)
Radiation therapy after previous surgery(ies)
Size before definitive surgery (cm)
Time between last surgery and definitive surgery (years)
1
23
1
4.0
Solid
40
No
4.5
3
2
27
2
4.0
Cystic
30
No
5.0
2
3
58
1
4.0
Solid
40
No
3.5
5
4
21
1
4.5
Solid
30
No
4.5
1 ½
5
29
3
5.0
Cystic
60
No
5.0
3
6
52
2
4.5
Solid
40
No
4.0
4
7
38
1
4.0
Solid
30
No
4.0
3
8
42
3
4.0
Solid
40
No
4.5
2 ½
9
47
1
4.0
Solid
40
No
4.0
2
10
40
2
4.5
Solid
30
CSR
4.5
2
11
35
2
5.0
Solid
50
No
5.0
4
12
47
2
4.0
Cystic
50
GKS
5.0
3 ½
13
28
2
4.5
Cystic
30
No
4.5
1 ½
14
39
2
4.0
Solid
50
No
4.5
4
15
42
1
3.5
Solid
30
GKS
4.0
2 ½
16
30
1
3.5
Solid
40
No
4.0
3
17
60
1
4.0
Solid
50
No
4.0
4
18
30
1
4.0
Solid
40
No
4.5
3
19
21
2
4.0
Solid
30
No
4.5
2
20
51
1
3.5
Solid
50
No
4.0
5
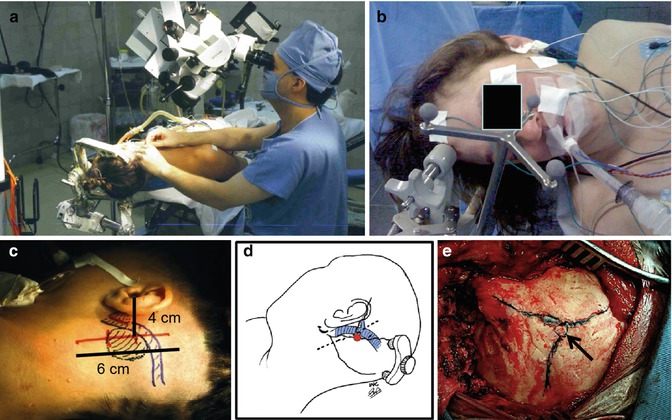
Fig. 25.1
Upper: (a–b) Patient and surgeon position. Lower: Skin incision (c–d) and (e) asterion (arrow)
25.3 Results and Surgical Complications
Surgery was indicated to decompress the brainstem and save patient’s life. The aim of surgery was also to remove completely these large and giant residual/recurrent tumors and cure the patient. Radical removal was possible in all cases (Table 25.2). The surgical procedure was much more difficult than in nonoperated cases. From the beginning of surgery, fibrosis caused by the previous procedure(s) difficult dissection of the dura mater and identification of the sigmoid sinus. Careful dissection was necessary in order to not injure the sigmoid sinus. After dura opening there, no clear arachnoid plane could be found. The cases submitted to radiotherapy presented even more adherences. Dissection and preservation of cranial nerves, vessels, and brainstem was the main task of surgery. Monitoring of facial and caudal cranial nerves helped to preserve these structures. When the IAC had not been opened by the previous surgery, identification and dissection of the facial nerve and removal of the intracanalicular portion of the VS within the IAC was less difficult. Postoperative anatomical preservation of the facial nerve was possible in eight of nine patients with preoperative facial nerve function. Reconstruction of facial nerve through hypoglossal-facial anastomosis was performed 2 or 3 weeks after surgery in seven of the remaining eight cases. House and Brackmann facial palsy grades III–IV were obtained in these patients.
Table 25.2
Patients with large and giant residual/recurrent VSs
Patient | VII CN preopa | Other preop neurol. deficits | VII CN post-opa | Hydrocephalus | Grade of removal | Follow-up | Complications |
|---|---|---|---|---|---|---|---|
1 | II | Ataxia | IV | Yes | Total | 12 years | No |
2 | VI | Ataxia, V CN, dysphasia | VI | Yes | Total | 10 years | CSF leak/meningitis |
3 | I | No | III | No | Total | 9 years | CSF leak |
4 | IV | Ataxia | VI | No | Total | 10 years | No |
5 | VI | Ataxia, VCN, dysphasia | VI | Yes | Total | 9 years | Facial numbness |
6 | VI | Ataxia, V CN | VI | Yes | Total | 10 years | No |
7 | I | No | I | Yes | Total | 8 years | No |
8 | VI | Ataxia | VI | Yes | Total | 6 years | IX, X (transient) |
9 | III | No | IV | No | Total | 5 years | No |
10 | VI | Ataxia, V CN, dysphasia Tracheotomy, gastrostomy | VI | Yes
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|





