57 Axial Lumbar Interbody Fusion (AxiaLIF)
I. Key Points
– Minimally invasive presacral approach for intervertebral discectomy and fusion
• Originally described for L5-S1 and extended to include L4-L5
• Relies on indirect decompression
• Not intended to be used as a stand-alone, requires supplemental fixation such as transfacet pedicle screws or pedicle screw-rod fixation
II. Indications
– Degenerative disc disease
– Radiculopathy
– Spondylolisthesis (grade I or II)
– Revision
• Pseudarthrosis
• Extension of long fusion to sacrum
III. Contraindications
– Aortic bifurcation below L5-S1 or aberrant midline vessel anterior to S1
– Previous pelvic or retroperitoneal surgery
– Inflammatory bowel disease
– Sacral agenesis
– Severe sacral lordosis
– Spondylolisthesis exceeding grade II
IV. Preoperative Management
– Imaging
• Magnetic resonance imaging (MRI) of the lumbar spine (computed tomography [CT] if MRI is contraindicated) including the tip of the coccyx to evaluate the trajectory, aberrant or anomalous vascular structures, and presacral fat pad
– Bowel prep performed the day before surgery
• GoLYTELY (Braintree Laboratories, Braintree, MA), 4 L
• MiraLax (Merck, Whitehouse Station, NJ), 64 oz
• Mag Citrate (Metagenics, San Clemente, CA)
– Antibiotics
• Make sure to include anaerobic and gram (negative) coverage.
V. Technique1
– Setup: biplanar fluoroscopy and radiolucent bed
– Position: prone with the knees below the level of the hips using Jackson table or OSI table (Mizuho OSI, Union City, CA) with sling for the legs
– A 20 French catheter is inserted into the rectum and 10 ml of air is insufflated to improve visualization of the rectum during fluoroscopy.
– The anus is isolated with an occlusive dressing and the sacrococcygeal region is prepped and draped in the usual sterile fashion.
– A 15 mm skin incision is made 1 cm lateral to the tip of the coccyx and 2 cm caudal to the left or right paracoccygeal notch. Be sure to continue the incision through the underlying fascia (Fig. 57.1).
– Blunt finger dissection is used to develop the presacral space and push the rectum anteriorly.
– A dissecting tool is advanced along the anterior midline of the sacrum using an oscillating movement to sweep the presacral fat away from the floor of the pelvis, and it is then docked at the S1-S2 junction.
– Once the trajectory is confirmed by fluoroscopy, a guide pin is placed into the sacrum (Fig. 57.1).
– A series of dilators are then carefully placed until the working cannula is securely docked into the sacrum.
– The guide pin is then removed and a drill is passed into the sacrum and disc space.
– A series of disc space cutters and wire brushes are used to perform the discectomy.
– Once the discectomy is performed, bone graft material is inserted into the disc space through the cannula. It is important to place the bone graft prior to drilling into the body of L5 so that bone graft material is not packed into that defect.
– An appropriate-size three-dimensional (3D) axial titanium rod is placed through the sacrum into the disc space and into the L5 vertebral body. The axial rod has a differential pitch that creates distraction across the disc space as it is rotated.
– Once satisfactory placement of the axial rod is achieved, the working cannula is removed, and the wound is irrigated and closed in the standard fashion. Dermabond liquid dressing (Ethicon, a Johnson & Johnson company, New York) is placed over the incision as an occlusive dressing.
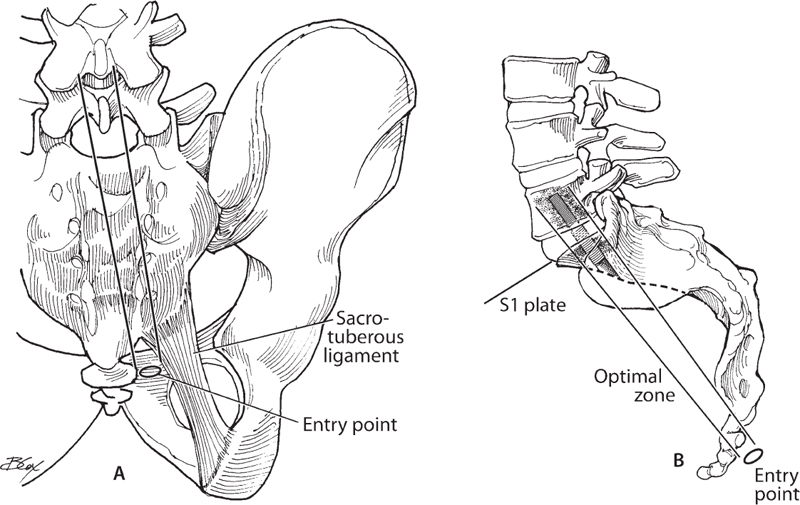
Fig. 57.1 (A,B) Schematic diagram depicting the optimal trajectory and entry point for presacral access to the L5-S1 axial lumbar interbody fusion.
VI. Postoperative Care
– Mobilize patient early with or without brace, according to surgeon preference.
– No procedure-related restrictions
– Discharge to home when patient meets discharge criteria, including tolerating regular diet, ambulating, voiding, and adequate pain control on oral medications.
VII. Potential Complications
– Bowel perforation2
– Vascular injury
• Transverse sacral veins or middle sacral artery
VIII. Outcomes
– Limited outcomes
– Fusion rate, 91%; Oswestry Disability Index (ODI), decrease of 26 points; Visual Analogue Scale (VAS), decrease of 7 points at one-year follow-up3,4
IX. Surgical Pearls
– True anteroposterior (AP) and lateral fluoroscopy images with continuous imaging throughout the procedure to ensure proper trajectory and safe access
Common Clinical Questions
1. True or false: Axial lumbar interbody fusion relies on indirect decompression.
2. True or false: Axial lumbar interbody fusion is safe to perform in patients with a grade III or IV spondylolisthesis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







