58 Facet Screw Fixation/Fusion
I. Key Points
– Pedicle screw fixation historically has been the gold standard for lumbar fusion stabilization. However, criticisms of the pedicle screw construct—including higher complication rates, bulky hardware, increased pain, and excessive wide soft-tissue dissection—have led to a more innovative, minimally invasive fixation technique. Translaminar facet screws have been found to be biomechanically advantageous, significantly increasing the stiffness and stability in compression, extension, flexion, bending, and torsion of spinal motion segments.1,2
– Facet screws were first described by King in 1948 as short screws placed horizontally across the facet joint. Boucher’s modifications in 1959 included an increased screw length directed more vertical into the pedicle. Today’s technique includes Magerl’s 1984 modification, involving a longer screw with an entry point at the base of the contralateral spinous process, increasing its effective fixation strength by expanding the working length at both sides of the facet.3
– This technique involves a minimally invasive approach without significant softtissue dissection. Improved outcomes—including biomechanical stability, decreased complication rates, reduced reoperation rates, lower operative times, minimal blood loss, and improved patient-perceived outcomes—have been demonstrated.4
– The use of image navigation with this posterior stabilization technique has been validated as a safe, feasible, economical and efficient method associated with low screw misplacement rates and excellent operative field viewing.4
II. Indications
– In conjunction with anterior interbody fusion for symptomatic discogenic pain unresponsive to at least 6 months of aggressive nonoperative treatment where posterior elements are present, intact
– Primary circumferential lumbar fusion with less than grade II spondylolisthesis
– Repair of pseudarthrosis after stand-alone anterior lumbar interbody fusion (ALIF)
III. Technique
– The patient is placed in the prone position on a radiolucent Jackson table frame.
– Image navigation rather than fluoroscopy used to localize incision.
– A small posterior midline incision is made at the appropriate level.
– A subperiosteal dissection along the spinous process and lamina to the targeted facet is performed bilaterally. The cephalad juxtalevel facet joint is not exposed. Supraspinous and interspinous ligaments should be preserved.
– The facet joint is the lateral limit of the dissection.
– A retractor is placed, allowing visualization of both the start point and contralateral caudal facet joint.
– A small, 2 cm incision is made lateral to the midline incision to allow a blunt bullet or drill guide to obtain the appropriate trajectory. Dock at the spinolaminar junction and target the contralateral facet/pedicle.
– Create a pilot hole with a starting awl, leaving enough room for the contralateral translaminar facet screw along the width of the spinolaminar junction. Place the first screw at the cephalad, superior aspect of the spinolaminar confluence and the second contralateral screw caudal to it in line with the lamina.
– Using a high-speed drill with a long 2.85 mm bit and image navigation (if available), drill to the contralateral facet/pedicle using tactile progression through the anatomical bony trajectory. Take care not to breach ventrally into the canal, and ideally stay within the lamina. Measure for screw length off the calibrated drill.
– While maintaining the drill guide in fixed position, use power to insert a 4.0 mm screw along the same drilled hole.
– Complete the tightening off power. Avoid overtightening the screw or fracturing the spinous process.
– Repeat the preceding steps for the contralateral translaminar facet screw.
– Obtain final imaging studies (Fig. 58.1).
– Decorticate posterior bony elements/lamina and add bone graft substitute.
– Close the fascia with 0 absorbable suture.
– Close the subcutaneous layer with inverted, interrupted 2-0 absorbable suture.
– Close the skin with running suture or skin adhesive.
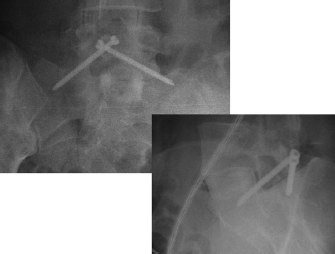
Fig. 58.1 Anteroposterior and lateral views demonstrating facet screw trajectory.
IV. Complications
– Spinous process fracture
– Ventral trajectory breach with either screw or drill
– Nerve root injury
– Wound infection
– Pseudarthrosis
V. Postoperative Care
– Mobilize early without bracing.
– Discharge home when patient meets discharge criteria (typically, ambulating, tolerating a diet, voiding, and adequate pain control on oral medications).
VI. Outcomes
– Reported reoperation rate is 5%, versus 24 to 37.5% for pedicle screw constructs, a statistically significant difference.4
– Operative time and blood loss have been shown to be significantly lower in the translaminar facet screw cohort compared with the pedicle screw population.4
– Patient-recorded outcomes include a significant decrease in postoperative Visual Analogue Scale (VAS) pain scores for both translaminar facet screw and pedicle screw constructs.4
VII. Surgical Pearls
– Obtain adequate visualization of the starting point, trajectory, and contralateral caudal facet joint.
– Plan accordingly for the placement of both screws and the ideal position prior to drilling.
– Establish an appropriate starting point at the confluence of the spinous process and lamina. Do not start high on the spinous process.
– Perform final screw tightening off power and do not overtighten or strip the screw, or fracture posterior bony elements.
Common Clinical Questions
1. Which of the following is a characteristic of the translaminar facet screw?
A. Requires a wide soft-tissue dissection
B. Not a minimally invasive technique
C. Combines an increased working length with greater fixation strength
D. Can be used with bilateral pars defects
2. Translaminar facet screws have been associated with:
A. Longer operative times
B. Lower rates of reoperation compared with pedicle screws
C. Greater operative blood loss
D. Inferior biomechanical properties relative to pedicle screws
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







