3 Imaging in Endoscopic Paranasal Sinus and Skull Base Surgery: Three-Dimensional Reconstruction
Rainer Guilherme Haetinger
 Introduction
Introduction
The role of high-quality imaging in planning surgery is paramount for a safe surgical approach and successful results. The detailed demonstration of anatomy and of the relationship between lesions and vascular and bony structures is an essential guide for the surgeon. Multislice computed tomography (MSCT) and volumetric computed tomography (VCT) provide a very reliable panorama of the anatomy because of their very thin slices (less than 1 mm) with isotropic pixels and high-speed acquisition (hundreds of images per second), allowing even greater quality in vascular studies. For the purposes of this chapter, these types of computed tomography are included in references to “CT.”
A specific and very useful protocol is computed tomography angiography (CTA or CT-angiography), which is performed with a contrast media injector and later postprocessed with volume rendering (VR) (Fig. 3.1), maximal intensity projection (MIP), and multiplanar reconstruction (MPR) software. This method is the best choice to demonstrate the vascularity of tumors, the relation between vascular structures and the bone, as well as bony integrity.1
On the other hand, high-field magnetic resonance imaging (MRI), with a 1.5- and 3-tesla field, is improving the quality of imaging and the capacity to distinguish tissues and structures, mainly in the brain. Equipment with higher magnetic fields (4 to 9 tesla) is still not generally available for medical use. Magnetic resonance angiography (MRA) is also an excellent and widely used method, and may be performed with or without contrast media (preferably with contrast media) and postprocessed with the same software as used for CTA. In this method the bony structures are not visualized, and there is a very clear view of the vessels, including those inside the canals and the foramina of the skull and spine. Computed tomography cisternography (CT-cisternography) is considered the radiologic “gold standard” to investigate cerebrospinal fluid (CSF) fistulas.
This chapter presents examples, using CT and/or MRI, of lesions that may be suitable for endoscopic surgery.
 Evaluation of the Paranasal Sinuses and Skull Base
Evaluation of the Paranasal Sinuses and Skull Base
The evaluation of the nose, paranasal sinuses, and skull base is done mainly by CT,2 which provides the following essential information:
1. The degree of aeration of paranasal sinuses and integrity of the medial orbital wall and cribriform plate
2. The location of intersinus septa
3. The position of anterior skull base vessels (better demonstrated by CTA)
4. The relationship between the fovea ethmoidalis and the cribriform plate
5. The presence of anatomical variations, such as Onodi cells, basilar expansion of the sphenoid sinus, pneumatization of the anterior clinoid processes, supraorbital ethmoidal cells, dehiscence of the medial wall of the orbit (with protrusion of the orbital fat tissue toward the ethmoidal labyrinth), and dehiscence of the lateral wall of the sphenoid sinus3
6. The presence and extent of bony dehiscences in the skull base near the internal carotid arteries, optic nerves, and cavernous sinuses
For skull base lesions, MRI is indicated to establish the following:
1. Recurrent skull base tumor
2. The intra- or extraaxial origin of tumors
3. The type of tissue located adjacent to dehiscent or destroyed bone
4. The invasion or external compression of the brain
5. The involvement of the internal carotid arteries, cavernous sinuses, vertebrobasilar system, or dural sinuses
6. The anatomical areas of potential major risk for a surgical approach, such as cavernous sinuses, Meckel’s caves, optical nerves, internal carotid arteries, the vertebrobasilar system, and jugular foramina
7. The relationship between the lesion and adjacent cranial nerves
8. The presence of scar tissue and reconstructive grafts
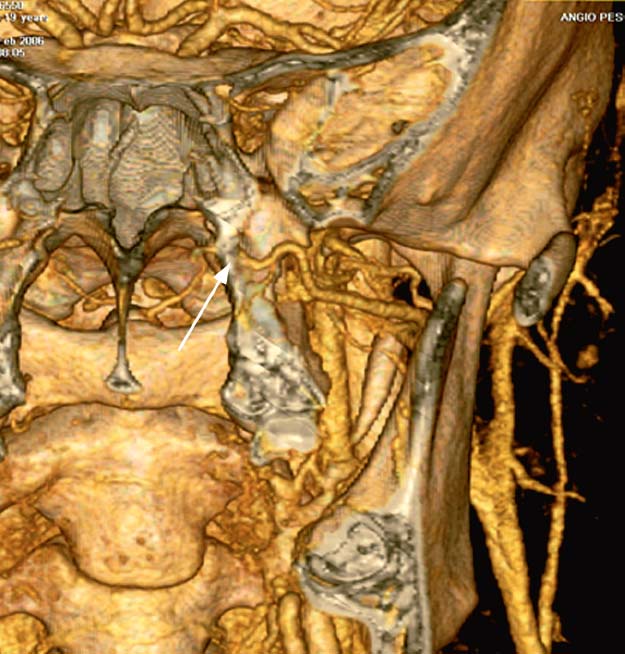
Fig. 3.1 CT-angiography with volume rendering 3D reconstruction (excluding the anterior part of the face). This postprocessed 3D reconstruction nicely shows the region of the pterygopalatine fossa and the left maxillary artery reaching the pterygopalatine foramen (arrow). This protocol maintains the bone, and thus it is easy to identify the pterygoid process, the inferior and superior orbital fissures, and the sphenoid sinuses.
An additional tool to evaluate the intra- and extracranial vessels is MRA, a noninvasive method that is very helpful in patients who have contraindications for iodinated contrast media, such as allergy or renal failure. It must be remembered that in cases of renal failure, the paramagnetic agent should also be avoided. The recent medical literature reports many cases of nephrogenic systemic fibrosis due to the association of renal failure with paramagnetic agents.
Digital subtraction angiography (DSA) is not used in most case, but in high-risk surgeries, mainly with involvement of arteries, it demonstrates thin but important vessels and verifies the functional integrity of the circle of Willis. In some cases it indicates the need for presurgical intravascular embolization of a vascular malformation or a vascular tumor.
 Importance of Anatomy and Anatomical Variations
Importance of Anatomy and Anatomical Variations
Arriving at a correct diagnosis requires identifying the anatomical origin of a lesion; failure to do so may lead to an incorrect differential diagnosis and a high probability of surgical complications. Therefore, radiologists and surgeons must have extensive knowledge of the complex anatomy of the skull base and face. They must be familiar with the axial, coronal, sagittal, and oblique planes. Three-dimensional (3D) reconstructions are helpful, but first the anatomy must be evaluated and the location of lesions determined on 2D reformations, such as MPR. It is also essential to observe the dislocation of vessels and nerves from their original topography, caused by the lesions or by anatomical variations.
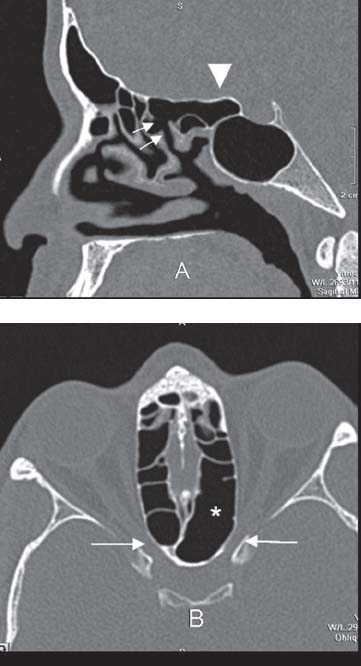
Fig. 3.2 Onodi cell. (A) Multislice CT image on a sagittal multiplanar reformation (MPR) exemplifying a typical Onodi cell, characterized by a posterior ethmoid cell extending backward and above the sphenoid sinus (arrowhead), reaching the anterior wall of the sella turcica, and also clearly demonstrating its drainage to the superior meatus (small arrows). (B) Axial plane view at the level of the optic canals (arrows) demonstrating the contiguity between the left canal and the ipsilateral Onodi cell (*).
There is abundant medical literature on this anatomy. So this chapter will focus on some advanced topics that are relevant to an endonasal approach to the skull base.
Anatomical variations in the posterior ethmoid or in the sphenoid sinus (e.g., Onodi cells, pneumatization of the anterior clinoid processes and pterygoid processes) may increase the risk of damage to optic nerves, internal carotid arteries,4 maxillary and vidian nerves, as well as the anterior structures within the posterior cranial fossa, behind a very thin or dehiscent clivus (basilar expansion of the sphenoidal sinus). Variations of the fovea ethmoidalis may increase the risk of anterior cranial fossa damage during surgery assisted by endoscopy, as classified by Keros in 1962,5 and referred to many times in the specialized literature. The presence of supraorbital ethmoidal cells, agger nasi cells, frontal bulla, and anterior and superior insertions of the uncinate process are also essential to determine and describe in each patient.
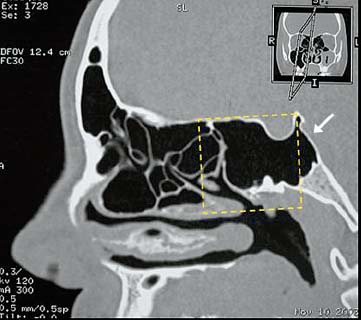
Fig. 3.3 Basilar expansion of the sphenoidal sinus. Multislice CT imaging with sagittal MPR showing the 90-degree angle with the planum sphenoidale at the dorsum sellae (dotted square) and the posterior extension of the sinus with a consequently thin clivus (arrow).
There are originally different types of Onodi cells, as Hungarian professor of Rhinology Adolph Onodi described in his original work.6 The most important type that is currently used is defined as the most posterior ethmoidal cell in contiguity with the optic canal, and it typically expands backward and above or laterally to the sphenoid sinus (Fig. 3.2). This expansion also leads to contact between the posterior ethmoid and the internal carotid artery, which usually is related only to the sphenoid sinus. For a surgical approach into the posterior ethmoidal and sphenoidal region, knowledge of this variation is essential to avoid complications and to plan the best surgical approach. (See also the subsection Meningioma in the section Extraaxial Lesions of the Anterior Cranial Fossa, below, and a specific example in the section Meningioma of the Anterior Cranial Fossa, below.)
The basilar expansion of the sphenoidal sinus result is an extension backward to the dorsum sellae, based on a 90-degree angle with the planum sphenoidale, in association with a thin clivus (Fig. 3.3). This basilar expansion represents a feature of great surgical importance. Complications may occur using the endoscopic approach in endonasal surgery, in which the form of basilar expansion is critical, that is, less than 2 mm thickness of the clivus, with an incidence of 45% in a series of 750 CT examinations and 50 dry skulls reported by Haetinger in 2006.7 There are reports in the literature of fracture, vertigo, posterior headache, vomiting, and empyema in patients with sphenoidal sinus prolongations. Recent reports of vasculitis of the basilar artery with ischemic infarction of the pons secondary to sphenoidal sinusitis, of spontaneous CSF fistula (Fig. 3.4), and of frequent exposure of the internal carotid arteries support the risk factors of a thin clivus due to a basilar expansion of the sphenoidal sinus.8–12 In addition, a thin clivus is a potentially weak region in cases of a skull base fracture, and it is susceptible to traumatic CSF fistula.
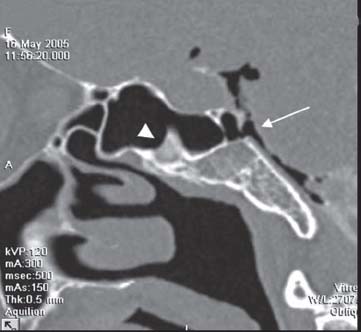
Fig. 3.4 Spontaneous CSF fistula at the clivus due to basilar expansion of the sphenoid sinus. CT-cisternography demonstrates pneumocephalus due to a CSF fistula in a patient with a dehiscent clivus (arrow). There is also CSF with contrast media inside the sphenoid sinus, adjacent to an intrasinusal septum (arrowhead).
 Characteristic Findings in Imaging
Characteristic Findings in Imaging
The most relevant lesions related to the nose, paranasal sinuses, and skull base are listed below, with their most characteristic imaging findings.
Lesions of the Nose and Paranasal Sinuses
Solitary Polyps and Cysts
• CT: well-defined mass, low to intermediate density, rare peripheral enhancement of mucosa, no central contrast enhancement
• MRI: intermediate signal on T1-weighted imaging (T1WI), hypersignal on T2-weighted imaging (T2WI), only slight peripheral enhancement of mucosa, no central contrast enhancement on enhanced T1WI13
Sinonasal Polyposis
• CT: well-defined polypoid masses, low to intermediate density, with irregular peripheral contrast enhancement, without central enhancement; in advanced stages, bone remodeling is a common finding
• MRI: intermediate or mixed signal on T1WI, hypersignal or mixed signal on T2WI (with central low signal in cases of chronic secretions), with peripheral irregular enhancement on enhanced T1WI
Mucocele
• CT: filled sinus with remodeled and thinned bony wall, hyperdense content (high protein content), without contrast media enhancement
• MRI: low signal on T1WI, usually with peripheral hyperintensity of the mucosa and central hypointensity on T2WI, no enhancement on enhanced T1WI; in earlier stages, with predominant high water content, there is diffuse hypersignal on T2WI
Inverted Papilloma
• CT: soft tissue mass in the nasal cavity, usually arising from the lateral wall, extending into the maxillary sinus, or within the maxillary sinus extending into the nasal cavity, with bone remodeling and erosion; there is a variable enhancement pattern, but it is usually heterogeneous
• MRI: intermediate or slight hypersignal on T1WI, heterogeneous hypersignal on T2WI, irregular enhancing mass on enhanced T1WI; cortical bone erosion may be seen, but this aspect is better evaluated by CT
Squamous Cell Carcinoma
Squamous cell carcinoma arises in the nasopharynx from the pharyngeal mucosal space and forms a mass in the posterior and lateral wall. When clinical symptoms begin, the tumor is usually large and there is often invasion of the skull base. Extensions to the prevertebral and parapharyngeal spaces, as well as to the posterior nasal cavity and oropharynx, are also patterns of spread. Metastatic disease to the lymph nodes is very common.
• CT: soft tissue mass producing bone destruction, with irregular enhancement after contrast media injection, usually infiltrating the clivus, pterygoid process, and prevertebral space; sagittal and coronal MPR images are very important for diagnosis
• MRI: isointense on T1WI, slightly hyperintense on T2WI, and diffuse enhancement on enhanced T1WI. It is essential to obtain an enhanced series with fat suppression (fat saturation). Perineural and perivascular spread is best evaluated with these series. Eventual invasion of the cavernous sinus is best evaluated on the coronal plane.
Adenoid Cystic Carcinoma (Cylindroma, Adenocarcinoma)
This carcinoma is an aggressive malignant tumor arising from seromucous glands or surface epithelium. It may originate in a paranasal sinus, at the hard palate, or in the parotid and submandibular salivary glands. Perineural spread is common and very dangerous, mainly through the pterygopalatine fossa, the inferior and superior orbital fissure, and the cavernous sinus.
• CT: irregular and infiltrating mass, with bone remodeling and destruction, with heterogeneous enhancement after iodinated contrast media intravenous injection
• MRI: mixed signal intensity, sometimes with hyperintense hemorrhagic foci on T1WI, irregular hyperintensity on T2WI, and irregular enhancement on enhanced T1WI; it is essential to use fat suppression in the enhanced series
Esthesioneuroblastoma
The origin of this tumor is in the olfactory membrane of the upper nasal cavity, at the cribriform plate.
• CT: mass causing remodeling or destruction of the cribriform plate, usually with inhomogeneous enhancement, sometimes with areas of cystic degeneration or necrosis
• MRI: low or intermediate signal intensity on T1WI, hyperintensity or mixed intensity on T2WI, and inhomogeneous enhancement after infusion of gadolinium contrast
Non-Hodgkin’s Lymphoma
• CT: lobulated soft tissue mass in nasal cavity or paranasal sinus, remodeling or destroying bone, with potential intracranial invasion; there is usually a moderate and diffuse enhancement after iodinated contrast media injection
• MRI: intermediate signal intensity on both T1WI and T2WI, with diffuse enhancement on enhanced T1WI
Extraaxial Lesions of the Anterior Cranial Fossa
Meningioma
• CT: extraaxial well-circumscribed mass, usually hyperdense (75%), sometimes isodense (25%), with homogeneous, intense, and diffuse enhancement after intravenous (IV) contrast media; about 25% have calcifications, and hyperostosis or irregular bone cortex are frequent findings
• MRI: intermediate signal on T1WI, variable signal on T2WI, sometimes with a sunburst pattern, homogeneous and intense enhancement after gadolinium in the majority of cases
• In the anterior cranial fossa, approximately 5 to 10% occur at the olfactory groove and 10 to 20% at the planum sphenoidale.14
• There are also atypical and malignant meningiomas that have areas of necrosis, bone destruction between the intra- and extracranial mass, and marked perifocal edema.
Craniopharyngioma
• CT: frequent tumor calcification; mixed cystic and solid mass with enhancement of the solid component and cyst wall
• MRI: variable from hypo- to hyperintense on T1WI depending on the cystic contents; mixed solid and cystic components with enhancement of the solid component and cyst wall; T2WI and fluid-attenuated inversion recovery (FLAIR) demonstrate heterogeneous signal in the solid components and cyst hyperintensity; calcification has low signal on T2WI
Frontoethmoidal Meningocephalocele (Cephalocele)
• CT: bone deformity with frontal bone displacement superiorly and nasal bones inferiorly, bifid or absent crista galli, absent or incomplete lamina cribrosa and frontal bone; there is a heterogeneous mass in continuity with the brain
• MRI: T1WI and T2WI demonstrate soft tissue mass isointense to gray matter herniated through the bony defect, without abnormal enhancement postgadolinium (but enhancement may be seen in cases of inflammation or infection)
Meningocele
• CT: similar bone deformity to meningocephalocele, but with hypodense content (CSF)
• MRI: hypointense on T1WI and hyperintense on T2WI CSF content, without brain parenchyma
Metastasis
• CT: bone destruction or permeative behavior adjacent to soft tissue, usually enhancing after IV contrast media injection
• MRI: intermediate signal in nonenhanced images, and heterogeneous enhancement postgadolinium; usually hyperintense on T2WI. It should be always considered in the differential diagnosis for solid aggressive lesions.
Aneurysm
• CT: well-delineated round or oval extraaxial lesion, which may be slightly dense in the precontrast phase, with high enhancement of its lumen after contrast media injection; there may be peripheral calcifications or not
• MRI: low (“flow void”) or heterogeneous signal on T1WI and low intensity on T2WI; sometimes the signal intensity is mixed or laminated
Extraaxial Lesions of the Middle Cranial Fossa
Meningioma
• CT: extraaxial well-circumscribed mass, usually hyperdense (75%), sometimes hypodense (25%), with homogeneous, intense, and diffuse enhancement after IV contrast media; about 25% have calcifications, and hyperostosis and irregular bone cortex are frequent findings
• MRI: intermediate signal on T1WI, variable signal on T2WI, sometimes with a sunburst pattern, homogeneous and intense enhancement postgadolinium in the majority of cases; the meningioma “en plaque” is seen as a sessile thickened enhanced dura
• T2* gradient echo (GRE) is very helpful to see calcifications.
• A “dural tail” is a very common finding in this tumor (~80% of cases).
Schwannoma
When a schwannoma affects the mandibular branch from the trigeminal nerve (V3), the solid mass enlarges the foramen ovale, with components below, in the masticatory space, and above, in the middle cranial fossa. Atrophy of the masticator muscles is common.
• CT: isodense to a musculature nodule or mass before IV contrast, and diffuse but moderate enhancement after contrast media injection. Bone remodeling may be seen, especially at the foramen ovale. There may be also little cysts and hemorrhagic components.
• MRI: intermediate or low signal intensity on T1WI, variable intensity on T2WI and different modes of enhancement, from homogeneous to heterogeneous, also depending on the presence of cysts and hemorrhagic foci
Aneurysm
• CT: well-delineated round or oval extraaxial lesion, which may be slightly dense in the precontrast phase, with high enhancement of its lumen after contrast media injection; there may be peripheral calcifications or not
• MRI: patent aneurysm has “flow void” or heterogeneous signal inside; a partially thrombosed aneurysm has commonly a mixed or laminated thrombus, depending on its age, on T1WI. On T2WI the aneurysm appears as hypointense. A patent lumen may enhance on enhanced T1WI.
Metastasis
• CT: bone destruction or permeative behavior adjacent to soft tissue, usually enhancing after IV contrast media injection
• MRI: intermediate signal on nonenhanced images, and heterogeneous enhancement postgadolinium; usually hyperintense on T2WI. It should be always considered in the differential diagnosis for solid aggressive lesions.
Extraaxial Lesions of the Posterior Cranial Fossa
Chordoma
Chordomas are typically localized at the clivus (when intracranial).
• CT: bone erosion and diffuse enhancement; the tumor may also extend into the middle fossa
• MRI: intense hypersignal on T2WI, hyposignal on T1WI, diffuse enhancement on enhanced T1WI
Chondrosarcoma
Chondrosarcomas are typically localized at the petro-occipital fissure, out of the midline.
• CT: bone erosion, irregular shape, and irregular or diffuse enhancement
• MRI: intense hypersignal on T2WI, hyposignal on T1WI, irregular or diffuse enhancement on enhanced T1WI
Meningioma
• CT: extraaxial well-circumscribed mass, usually hyperdense (75%), sometimes hypodense (25%), with homogeneous, intense, and diffuse enhancement after IV contrast media; about 25% have calcifications, and hyperostosis and irregular bone cortex are frequent findings
• MRI: intermediate signal on T1WI, variable signal on T2WI, sometimes with a sunburst pattern, homogeneous and intense enhancement postgadolinium in the majority of cases; the meningioma “en plaque” is seen as a sessile thickened enhanced dura
• A “dural tail” is a very common finding in this tumor (~80% of cases).
• T2* GRE is very helpful to see calcifications.
Metastasis
• CT: bone destruction or permeative behavior adjacent to soft tissue, usually enhancing after IV contrast media injection
• MRI: intermediate signal in nonenhanced images, and heterogeneous enhancement postgadolinium; usually hyperintense on T2WI. It should be always considered in the differential diagnosis for solid aggressive lesions.

Fig. 3.5 Juvenile angiofibroma (recurrence). (A) CT-angiography with maximal intensity projection (MIP) technique on the axial plane, thick slice, demonstrates a high vascular tumor in the nasopharynx and choanal region, as well as the pterygopalatine fossa. The pathologic tor tuous vessels are well seen in the center of the lesion, as well as their relationship with the right maxillary artery. There is also a postsurgical status on this side. (B) MRI T1WI postgadolinium on the coronal plane demonstrates the extension of the tumor, without intracranial involvement. (C) A 3D reconstruction in lateral view with volume rendering technique gives the surgeon a very helpful view of the anatomical relationships.




