Intracranial Arteriovenous Fistulae
Etiology
Intracranial arteriovenous fistulae are of two main types: carotid-cavernous fistulae and dural arteriovenous fistulae. Carotid-cavernous fistulae (CCF) are abnormal vascular connections between the internal and/or external carotid artery and the cavernous sinus. Dural arteriovenous fistulae (DAVF) are direct connections between the arterial and venous systems within the dura, which bypass the capillary bed. Dural arterial feeders can be from the internal carotid artery, external carotid artery, or vertebral system; they most commonly connect into one of the dural sinuses.
Classification
CCFs can be classified according to various criteria: pathogenetically (traumatic versus spontaneous fistulae), hemodynamically (high- versus low-flow fistulae) or angiographically (direct versus dural fistulae), but they are most commonly described according to the Barrow classification (Table 15.1).1 Type A CCFs are by far the most common (72%); Type D is the most common low-flow CCF (21%).2 Direct CCFs usually occur secondary to trauma causing carotid laceration or rupture of a cavernous carotid artery aneurysm. Indirect CCFs are acquired lesions, thought to originate from an insult to a dural venous sinus that stimulates an inflammatory response, with subsequent neovascularization, angiogenesis, and the development of pathological shunts at the arteriolar level. Alternatively, the fistula may be the initial event, with turbulent arterialized blood flow in the dural venous sinus inciting a process of thrombosis. Another theory supposes the existence of small dural channels between arteries and a venous sinus that may enlarge, should that sinus thrombose. A third theory suggests that spontaneous low-flow CCFs form after the rupture of a dural artery traversing the cavernous sinus. Indirect dural CCFs most commonly occur in perimenopausal women, implying a hormonal influence. In the largest series of studies on indirect CCFs to date (n = 135), Meyers reports that 73% occurred in women with a mean age of 60 years.3
Table 15.1 Barrow Classification of Carotid-Cavernous Fistulae
Type | Fistulous vessels | Comments |
A | Carotid artery to cavernous sinus (CS) | Direct, high flow, most common |
B | Dural ICA branches to CS: Meningohypophyseal trunk (66%), inferolateral trunk (30%) | Indirect, low flow |
C | ECA branches to CS: internal max (67%), middle mening (59%), accessory mening (31%), ascending pharyn (24%) | Indirect, low flow |
D | Both ICA and ECA branches | Indirect, most common low flow |
DAVFs may be classified according to their pattern of flow (Fig. 15.1). Djindjian first classified DAVF according to angioarchitecture in 1978 (Table 15.2).4 In 1995, Cognard (Table 15.3) further classified both cranial and spinal arteriovenous fistulae with prognostic and treatment implications.5 Borden simplified the classification, emphasizing that the major factor in predicting a clinical course centers on the presence of cortical venous drainage and direction of flow (Table 15.4).6 Unlike drainage into the sinuses, cortical veins are not protected by the dura and cannot withstand arterial pressures. Therefore, DAVFs with cortical drainage are at a higher risk for rupture and hemorrhage.
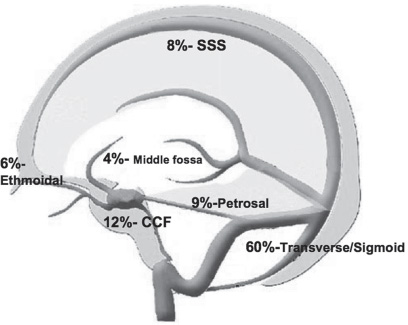
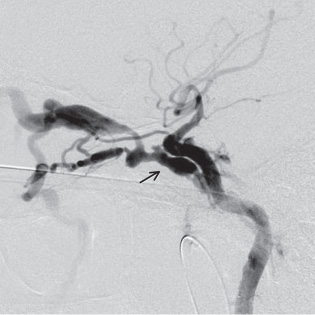
Dural arteriovenous fistulae can occur from direct trauma, sinus occlusion, tumor invasion, vascular collagen diseases, or infections involving the sinus. Inflammatory changes from these conditions can cause angiogenesis, demonstrated by high concentrations of vascular endothelial growth factor (VEGF) found near fistulae. There are also embryological theories, which state that there are primitive direct connections between the arteries and veins that can reopen in the setting of an inflammatory response or a sinus occlusion. Dural fistulae can present anywhere the dura is in proximity to venous drainage (Fig. 15.1), but they are usually classified by several common locations: transverse/sigmoid sinuses (Fig. 15.2), cavernous sinus (Fig. 15.3), superior sagittal sinus (SSS) (Fig. 15.4), anterior fossa (ethmoidal) (Fig. 15.5), petrosal (Fig. 15.6) and sylvian fissure/middle fossa.
Fig. 15.1 This figure shows the relative distribution of intracranial DAVFs. Most are located in the transverse and sigmoid sinuses and carry a low risk of intracranial hemorrhage, whereas DAVFs found in the ethmoidal, middle fossa, and petrosal regions often present with hemorrhage.
Table 15.2 Djindjian DAVF Classification
Type I: Drainage into a venous sinus |
Type II: Drainage into a venous sinus with reflux into cortical veins |
Type III: Drainage into cortical veins |
Type IV: Presence of venous lakes |
Djindjian R, Merland JJ, Theron J. Super-Selective Arteriography of the External Carotid Artery. Springer-Verlag; 1978:606–628
Table 15.3 Cognard DAVF Classification
Type I: Anterograde drainage into a venous sinus |
Type IIa: Retrograde drainage into a venous sinus |
Type IIb: Anterograde drainage into a venous sinus and cortical veins |
Type III: Drainage into cortical veins only |
Type IV: Drainage into cortical veins only with venous ectasias |
Cognard C, Gobin Y, Pierot L, et al. Cerebral dural arteriovenous fistulas: clinical and angiographic correlation with a revised classification of venous drainage. Radiology 1995;194:671–680
Table 15.4 Borden DAVF Classification
Type I: Antegrade flow into a venous sinus |
Type II: Retrograde flow into a venous sinus |
Type III: Retrograde into cortical veins |
Borden JA, Wu JK, Shucart WA. A proposed classification for spinal and cranial dural arteriovenous fistulous malformations and implications for treatment. J Neurosurg 1995;82:166–179
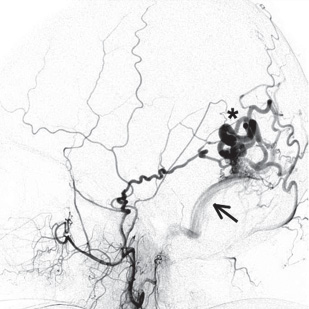
Fig. 15.2 A lateral angiogram of the external carotid artery showing a DAVF fed by the posterior limb of the middle meningeal artery draining into the transverse sinus (arrow) with cortical venous drainage (asterisk).
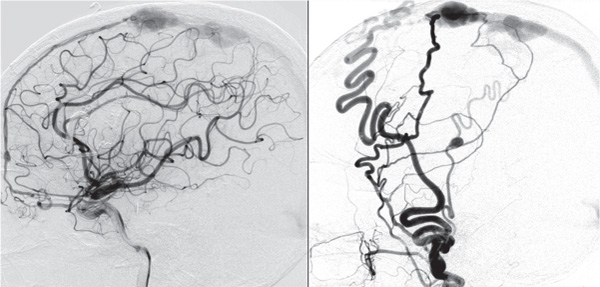
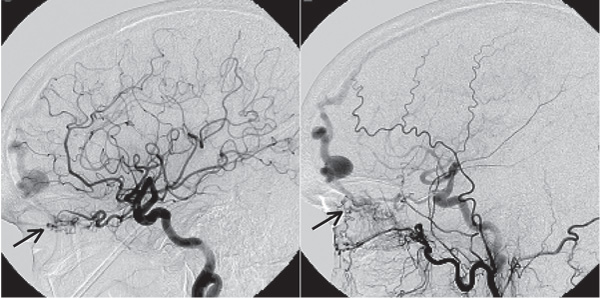
Fig. 15.4 Lateral angiogram of the internal (left) and external carotid artery (right) showing a DAVF fed by the anterior meningeal artery (left) and the superior temporal and middle meningeal arteries (right) draining into the superior sagittal sinus. Note the common fistulous point into a venous varix.
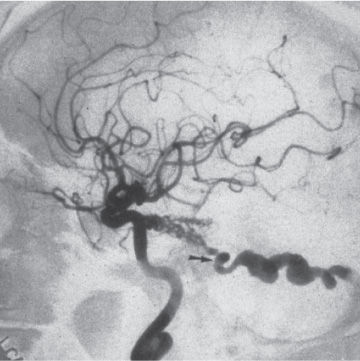
Fig. 15.6 A lateral angiogram showing a petrosal fistula filling from the tentorial artery through the tentorium into the petrosal vein (arrow shows the fistulous point).
Presentation
CCFs commonly present with ophthalmological symptoms, such as proptosis, chemosis, conjunctival injection, diplopia, secondary glaucoma, and loss of vision (Table 15.5). These symptoms are related to the degree of shunting and the route of venous drainage. They occur as a result of venous hypertension, due to high-pressure arterial flow invading a low-pressure venous system. Headache may occur due to engorgement or partial thrombosis of the cavernous sinus, with stretching of the dura, or due to cortical venous drainage, with cerebral venous hypertension. Subarachnoid or intracerebral hemorrhage from rupture of arterialized cortical veins may also occur as the presenting symptom. Although retrograde cerebral venous drainage is more common in direct, high-flow fistulae, Meyers et al. report that 31% of patients with indirect CCFs presented with this symptom,3 a significant risk factor for hemorrhage
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree