Fig. 52.1
Allergic fungal sinusitis. (a) Sagittal T1-weighted precontrast image. (b) Sagittal CT image with contrast enhancement. (c) Coronal T1-weighted gadolinium-enhanced image. There is expansion of the sphenoid sinus containing heterogeneous-appearing, hyperdense, and partly calcified material
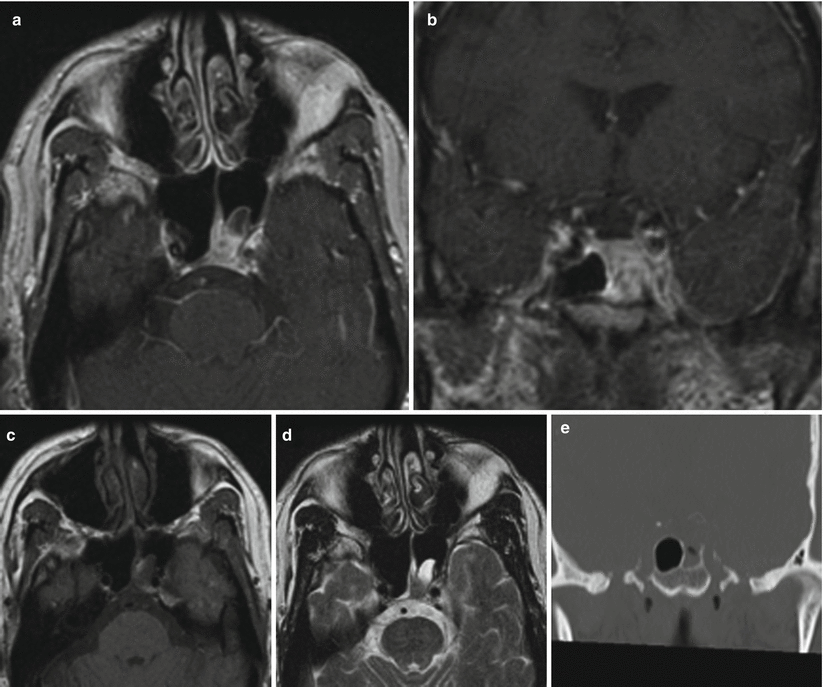
Fig. 52.2
Invasive fungal sinusitis. (a) Axial T1-weighted gadolinium-enhanced image. (b) Coronal T1-weighted gadolinium-enhanced image. (c) Axial T1-weighted precontrast image. (d) Axial T2-weighted image. (e) Coronal CT image in bone window. On (a–c), enhancing tissue is present along the superior medial margin of the left sphenoid sinus. Image (d) reveals erosion through the roof of the left sphenoid
52.3 Histopathology
The most common causes of fungal abscesses are Aspergillus and Candida species.
Mucormycosis is caused by fungi of the order Mucorales, most commonly the Rhizopus species.
Typical staining for diagnosis of fungal disease includes hematoxylin and eosin (H&E), Gomori’s methenamine silver, and periodic acid–Schiff stains.
Histologically, Aspergillus species are characterized by hyaline, uniform, septate, and dichotomously branched hyphae. Purulent, necrotizing inflammation is commonly observed.
Grossly, mucormycosis is characterized by black, necrotic lesions and occasional tumefaction [15].
Histologically, mucormycosis is characterized by broad-based and nonseptate hyphae with irregular branching that may occur at right angles. Vascular invasion and necrosis are common. Pyogenic inflammation and suppurative necrosis are commonly observed.
52.4 Clinical and Surgical Management
Transsphenoidal surgery is the mainstay of treatment for achieving biopsy, cultures, and drainage or resection of sellar region fungal abscesses [20].
In patients with invasive fungal sinusitis and rhinocerebral mucormycosis, early diagnosis and intervention are critical. Management typically consists of aggressive surgical debridement, glucose control, and antifungal therapy.
Following surgical management and diagnosis, long-term antifungal agents are administered. The most common agents include amphotericin B, caspofungin, itraconazole, and voriconazole.
Most patients with fungal pituitary abscesses treated in a timely manner will have a good long-term outcome [5, 20].
On the other hand, outcomes for patients with invasive fungal sinusitis are poor, with an overall survival rate of less than 50 % [6].
Outcomes in patients with invasive rhinocerebral mucormycosis are extremely poor, with a majority of patients dying from the disease.
References
1.
Hao L, Jing C, Bowen C, Min H, Chao Y. Aspergillus sellar abscess: case report and review of the literature. Neurol India. 2008;56:186–8.CrossRefPubMed
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








