49 Open and MIS Lumbar Microdiscectomy
I. Key Points
– Conservative therapy is the initial and primary treatment modality for radiculopathy caused by a herniated nucleus pulposus (HNP) in the lumbar spine.
– Lumbar microdiscectomy is a safe and effective procedure when the indication is appropriate.
– Cauda equina and conus syndromes caused by HNP in the lumbar spine constitute neurosurgical emergencies and require immediate evaluation.
II. Indications
– Symptomatic HNP
• Radiculopathy (after 6 to 8 weeks of failed conservative therapy)
• Cauda equina syndrome
• Conus syndrome
– Not for isolated axial low back pain
– No instability on preoperative dynamic plain radiographs
III. Technique
Open
– The patient is placed in the prone position.
• Use of a Wilson frame may widen the interlaminar space and assist in access.
– Fluoroscopy is used for localization.
– A 2 to 3 cm midline incision is made with a number 10 scalpel.
– A subperiosteal dissection of tissue from spinous process and lamina on the ipsilateral side is performed.
• Supraspinous and interspinous ligaments should be preserved.
– The medial facet joint is the lateral limit of the dissection.
– A retractor (e.g., Williams or Taylor) is placed.
– The inferior lamina of the superior level and superior lamina of the inferior level are identified and confirmed with fluoroscopy.
– Using a high-speed drill, a laminotomy (usually) is performed by drilling the inferior part of the superior level.
• For inferior fragment migration, some of the superior lamina from the inferior level may need to be removed.
– Ligamentous flavum is removed with curette and Kerrison punch.
– The operative microscope is brought in.
– The nerve sleeve and dura are gently retracted medially (Fig. 49.1).
– The posterior longitudinal ligament (PLL) and annulus fibrosus are incised with a number 11 blade, medial to lateral (always incise away from dura).
– Disc material is removed with a pituitary rongeur.
• The surgeon must have an understanding of where the anterior longitudinal ligament (ALL) is to prevent inadvertent penetration into the retroperitoneal vessels with the pituitary rongeur.
– The disc space is irrigated and loose disc tissue is removed.
– An instrument (e.g., Woodson or dental dissector) is passed beneath the dura to ensure there is no residual fragment.
– A nerve hook is used to probe under the PLL superior and inferior to the disc space to check for residual.
– The fascia is closed with 0 or 2-0 absorbable suture.
– The subcutaneous layer is closed with inverted, interrupted 3-0 absorbable suture.
– The skin is closed with running suture, staples, or skin adhesive.
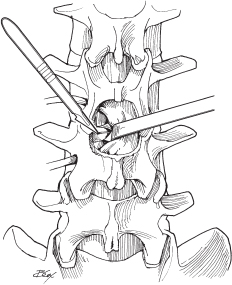
Fig. 49.1 Dorsal view of laminotomy defect showing thecal sac, traversing nerve root (retracted medially), and herniated disc.
Minimally Invasive Technique
– After correct positioning and localization, a 12 to 16 mm incision is made 10 mm lateral to the midline on the appropriate side.
– The thoracodorsal fascia is incised with blade or cautery, and serial dilators are positioned with the use of fluoroscopy.
– The final dilator and working tube should be docked over the interlaminar space with visualization of the inferior lamina of the superior level.
– The operative microscope is brought in.
– Soft tissue is dissected and drilling is performed until ligamentum flavum is reached.
• If drilling is done too laterally, the pedicle or facet joint is at risk; confirm location with fluoroscopy if needed.
– The ligament is removed and discectomy is performed as in the open approach.
– If a wider decompression is needed, the working tube may be repositioned to allow access to more lamina, and even the contralateral foramen.
IV. Complications
– Cerebrospinal fluid (CSF) leak (5 to 8%)1
• Attempt primary repair using nonabsorbable suture (typically challenging).
• Alternatively, cover with Gelfoam (Pfizer, New York) and/or fibrin glue.
– Nerve root injury (1%)
– Wound infection (1%)
– Vascular injury (<1%)
• Suspected injury to the iliac vessels anteriorly (e.g., bright red blood from disc space or sudden, unexplained drop in blood pressure) requires immediate wound closure, repositioning of patient to supine, and immediate vascular surgery consult.
V. Postoperative Care
– Mobilize early; no need for bracing.
– Discharge to home when patient meets discharge criteria (typically, ambulating, tolerating a diet, voiding, and receiving adequate pain control from oral medications—usually same day or on post-op day 1).
VI. Outcomes
– There is an 85% chance of a good (minimal symptoms) or excellent (asymptomatic) outcome.2
– First recurrence is usually treated with repeat microdiscectomy. Further recurrence may necessitate fusion.
– Multiple randomized trials have been plagued by crossovers between cohorts, and the most definitive statement that can be made is that decisions for surgery versus conservative treatment based on symptoms, duration, and patient preference results in similar good outcomes in both treatment groups.3
VII. Surgical Pearls
– Ensure the HNP is the pain/symptom generator based on exam and imaging.
– Minimal disruption of medial facet (don’t confuse the facet for the lamina during the initial approach)
– Overly aggressive drilling of facet may lead to instability.
– Ensure you are not in a nerve root axilla when performing discectomy.
– Preoperative dynamic films may be necessary to rule out instability
– May need hemilaminectomy or complete laminectomy if treating large central disc (e.g., for cauda equina or conus syndrome).
Common Clinical Questions
1. What is the best way to avoid drilling into the facet joint or pedicle during MIS discectomy?
2. When evaluating for recurrent lumbar herniated disc, what radiologic examination is most appropriate?
3. When evaluating a recurrent lumbar herniated disc, what radiologic exam is helpful in ruling out instability?
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







