Chapter 106 Pain Management and Palliative Care
Pain Management
Introduction
Pain has been defined as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage” [IASP, 1979]. The stimulus can be thermal (heat or cold), chemical (acid or alkali), or mechanical (torsion, stretch, pinch, or prick). Nociception, or pain perception, is the series of electrochemical events following the tissue damage or injury, excluding any emotional correlates of the noxious sensation. Acute pain occurs in a wide variety of pediatric medical encounters, and chronic pain, in one form or another, affects an estimated 15–20 percent of children [Goodman and McGrath, 1991]. Pain can be effectively relieved in 90 percent of patients; nevertheless, only 20 percent of patients achieve effective relief of chronic pain [Ferrell and Rhiner, 1991]. Many studies now demonstrate that neonates, infants, and children can receive analgesia and anesthesia safely for acute pain [Taddio, 2002; Shah and Ohlsson, 2002; Polaner, 2001; Stevens et al., 2000].
Historical Background
Studies from the 1970s into the 1990s documented under-treatment of pediatric patients compared to adults undergoing uncomfortable diagnostic procedures (e.g., lumbar puncture) and even for major surgical procedures (e.g., amputations, nephrectomies, and atrial septal defect repairs) [Schechter, 1989]. Despite an increased number of studies documenting adverse effects of pain over the past two decades, misinformation about pain and nociception in very young children and neonates has prevailed until very recently. Contrary to prevalent myth, newborn infants have the neurophysiologic basis necessary to experience and remember pain, as well as an intact and functional opiate receptor system [Lee et al., 2005]. Fortunately, pain assessment and treatment of painful symptoms are now standards of care for patients of all ages [Joint Commission on Accreditation of Healthcare Organizations, 2001].
Physiology
The physiology of pain perception has been reviewed previously [Anand and Carr, 1989]. Nociceptors present in mucosal membranes, cornea, subcutaneous tissue, bone and teeth, joints, and muscle detect noxious or potentially noxious thermal and mechanical stimuli, and chemical agents. A noxious stimulus is transduced into electrical sensory nerve activity, and the sensory information is projected to the central nervous system via several types of fibers. A-beta (moderately myelinated, fast-conducting) fibers carry impulses for the perception of pressure/position; A-delta (moderately myelinated, fast-conducting) fibers carry impulses from high-threshold mechanoreceptors and polymodal peripheral sensory neuron, which respond to pressure and temperature; and C-fibers (unmyelinated, slow-conducting) carry impulses from cutaneous and deep, low-threshold mechanoreceptors, chemoreceptors, and thermoreceptors. A-delta fibers carry sharp, spatially distinct pain signals, while C-fibers carry diffuse pain signals. A-beta fibers signal nonpainful touch and pressure that can compete with nociception. The majority of peripheral sensory neurons have cell bodies in the dorsal root ganglion, with some afferent input transmitted through the ventral root. Entering through the dorsal root, these fibers separate into A and C fiber bundles in the medial and lateral divisions of the dorsolateral fasciculus, and form synapses within the laminae of spinal cord gray matter. Neurons within laminae V, VII, and X of the spinal cord relay information to the long ascending tracts to various portions of the brain. The long ascending tracts make monosynaptic or polysynaptic reflex connections with lower motor neurons in the ventral horns and have projections to the locus ceruleus, thalamus, hypothalamus, anterior and posterior cingulate gyrus, amygdala, insular cortex, and somatosensory cortex, forming what has been termed the “pain matrix” [May, 2007]. The components of the nociceptive system mature at different rates [Lee et al., 2005]. Sensory signals can be amplified by neuronal activation in the periphery or the spinal cord by inflammatory mediators (bradykinin, cytokines, catecholamines, and substance P), or they can be attenuated by competitive spinal cord stimulation of A-beta fibers. Afferent impulses can be amplified in the spinal cord by substance P or neurokinin A, or by central processes such as “wind-up” with secondary hyperalgesia, or central sensitization; they can be attenuated by endogenous opioids (endorphins, dynorphins, and enkephalins), and serotonergic, noradrenergic, cholinergic, and gamma-aminobutyric acid (GABA)-ergic compounds via dorsolateral cortex-mediated mechanisms. Opioid receptors present in the cortex, spinal cord, limbic system, midbrain respiratory centers, and the periphery respond to stereospecific endogenous opioids to produce analgesia (mu), as well as side effects such as euphoria/dysphoria, (kappa) respiratory depression, decreased gastrointestinal motility, bradycardia/tachycardia, and dependency. Several anatomical structures contribute to the inhibition of nociceptive afferent input. They include the cortex, thalamus, periaqueductal gray matter, medulla, and dorsolateral funiculus via inhibitory effects of norepinephrine, serotonin, endogenous opioids, GABA, and acetylcholine. Most of the inhibition occurs at the level of the dorsal horn.
Developmental Differences
Fetal stress responses to pain have been documented as early as 18 weeks’ gestation, with peripheral, spinal, and supraspinal capacity for afferent pain transmission by 26 weeks’ gestation [Lee et al., 2005]. At this age, newborns can mount behavioral, autonomic, and metabolic stress responses to tissue injury. Neonates demonstrate characteristic facial expressions, aversive body movements, alterations in cardiac activity, and changes in cry in response to painful stimuli. Nociceptive nerve endings (receptors) are fewer in number in children than in adults; so tissue damage must be more significant before a pain response is elicited. Pain impulses travel over nonmyelinated nerve fibers, potentially delaying behavioral responses to pain. Young infants may perceive pain more intensely than older children or adults since descending inhibitory pathways that modulate and reduce the pain develop later than afferent excitatory pathways [Franck et al., 2000]. Inadequately treated pain in premature infants is associated with adverse short-term effects (e.g., more postoperative complications) [Lee et al., 2005]; the accompanying physiologic changes (increased heart rate, blood pressure, cardiac variability, hypoxemia, changes in autonomic tone, increased venous pressure, increased cerebral blood flow, and increased intracranial pressure) may augment risks of intraventricular hemorrhage or white-matter injury in the immature brain. Inadequately treated repetitive pain in the developing brain may accentuate neuronal apoptosis [Bhutta and Anand, 2002], fosters wind-up (in which unmodified afferent transmission enhances N-methyl-d-aspartate (NMDA) receptors and facilitates hyperalgesia over time) [Taddio et al., 2009], fosters hyper-reactive pain responses to subsequent stimuli [Weisman et al., 1998], promotes allodynia [Anand et al., 2001], causes long-term behavioral changes [Grunau et al., 2009], and influences the future development of pain syndromes [Jones et al., 2009].
Clinical Assessment
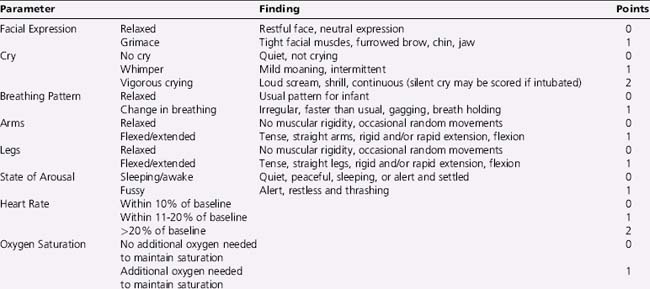
Pain is a subjective and variable experience, with no direct relationship between “pain experience,” physical pathology, and pain intensity [Derbyshire et al., 2004; Danziger and Willer, 2005]. Responses to pain vary widely, depending on gestational age, chronologic age, developmental state, initial behavioral state, prior experience of pain, cognitive state, emotional state, and the ability to respond to and habituate to sensory stimuli. There is no single uniform, standard technique for assessing pain in neonates or children. Biochemical responses to pain, (elevations in cortisol, catecholamines, beta-endorphins, insulin, glucagon, renin-aldosterone, growth hormone, and prolactin) are rarely useful to clinicians. Infants and children demonstrate a variety of nonspecific but consistent behavioral, physiologic, and autonomic responses to pain (Box 106-1) [Anand and Carr, 1989]. These signs have been used by clinicians to recognize pain in nonverbal infants and to quantify severity of the pain experience.
Box 106-1 Responses to Painful Stimuli
Self-report, usually by linear analog scale, is regarded as most reliable, but only for children who have attained the cognitive capacity to use it. Infants and preverbal children cannot self-report pain quality, quantify its severity, nor inform providers as to the efficacy of analgesic treatments. For preverbal patients, pain assessment is best achieved using multidimensional scales, including behavioral, physiologic, and autonomic responses (Box 106-2). Behavioral observational scales are used for pain assessment in neonates, children under the age of 4, or cognitively impaired children. Neonatal scales used include the Neonatal Infant Pain Scale (NIPS), Premature Infant Pain Profile (PIPP), and pain assessment score sheet [Franck et al., 2000]. Toddlers and preschool children who cannot communicate pain quality or intensity effectively can often use structured questioning or standardized semiquantitative pain assessment tools (poker chips in increasing numbers, cartoon drawings of faces, a pain thermometer, and colors or words) to rate pain intensity consistently and reliably. Children of 8 years or older are able to communicate pain intensity and quality effectively using questionnaires or visual analog scales designed for adults. Behavioral assessment tools, such as the FLACC tool, have been used recently to evaluate children with developmental delay at particular risk of undiagnosed or untreated pain, either acute or chronic [McGrath et al., 1999; Voepel-Lewis et al., 2002; Oberlander et al., 1999].
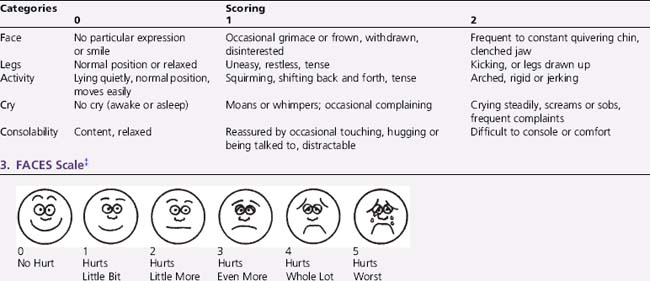
Box 106-2 Examples of Pain Assessment Scales for Differing Developmental Ages
* For preterm and term infants; scored on a 0–10 point system.
† For infants 4 months of age to children 3 years of age. Each of the five categories – (F) Face; (L) Legs; (A) Activity; (C) Cry; (C) Consolability – is scored from 0 to 2, which results in a total score between 1 and 10.
‡ For children 3–11 years of age.
§ For children >7 years of age.
(Example 1, Neonatal Infant Pain Scale (NIPS), modified from Lawrence J, et al: The development of the tool to assess neonatal pain, Neonatal Netw 6:59–66, 1993. Example 2, FLACC Scale, from Merkel SI, et al: The FLACC: A behavioral scale for scoring postoperative pain in young children, Pediatr Nurs 23:293–297, 1997. Example 3, FACES Scale, from Wong DL, et al: Wong’s Essentials of Pediatric Nursing, ed 6, St. Louis, 2001, Mosby, p 1301.)
Management
The Joint Commission on Accreditation of Healthcare Organizations (JCAHO) now requires hospital policies to address four standards of pain management in the accreditation process: management as a patient right, regular and comprehensive pain assessment, patient education, and performance monitoring [JCAHO, 2005]. The American Academy of Pediatrics, the American Pain Society, and the National Association of Neonatal Nurses all provide standards of pain management [AAP, 2000, 2001].
A four-step approach to painful conditions, initially intended as a model for cancer pain management but applicable to other diseases, has been advocated by the World Health Organization [Schug et al., 1990]. Pain, acute or chronic, should be assessed regularly and treated aggressively with nonpharmacologic methods and appropriate analgesic therapies. Effective pain management schemes should utilize the simplest effective pharmacologic regimen, dose around the clock for on-going painful conditions, and tailor the regimen to fit individual patient needs. A variety of nonpharmacologic techniques may be effective in managing mild to moderate pain. In neonates, non-nutritive sucking (with or without sucrose), distraction, breastfeeding, swaddling, kangaroo care, music therapy, and multisensorial stimulation have been utilized to mitigate the severity of procedural pain [Golianu et al., 2007]. Massage and acupuncture have also been suggested for the treatment of pain in neonates [Golianu et al., 2007]. For older infants and children, nonpharmacologic interventions should be age-appropriate for the patient’s developmental stage [Khan and Weisman, 2007].
Sucrose (given orally as a 24 or 30 percent solution) is effective in reducing mild procedural pain (such as circumcision and immunizations) in neonates and infants; however, an association between poor neurodevelopmental outcomes with repeated sucrose analgesia has been reported [Johnston et al., 2002].
Mild pain unresponsive to cognitive techniques, or sucrose in neonates, can be treated with weak (nonopiate) analgesics (e.g., non-steroidal anti-inflammatory drugs [NSAIDs] or acetaminophen). For moderate pain, oral “weaker” opioids, or combinations of opioids and NSAIDs or acetaminophen, can be used. Severe pain requires more aggressive parenteral opioids, such as morphine or fentanyl. Intractable pain or unacceptable toxicities of pain medications may require invasive interventions, such as nerve blocks or intraspinal anesthetic infusions. A multimodal approach to pain relief allows drug synergy or potentiation and can reduce single drug doses, minimizing side effects [Galloway and Yaster, 2000]. Common side effects of opiates, such as drowsiness, constipation, nausea, respiratory distress, and pruritus, can be anticipated and treated before or when they occur, without reducing analgesic dosing.
Types of Pain Medications
Aspirin, Acetaminophen, and NSAIDs
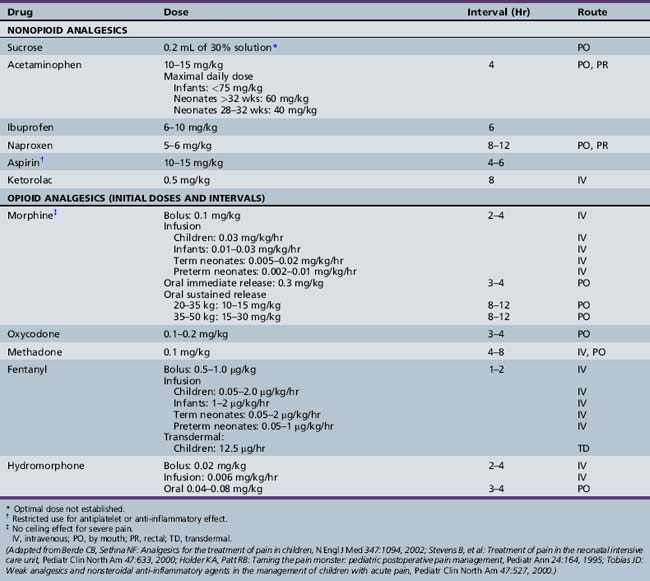
Except for specific indications in rheumatologic diseases and for inhibition of platelet adhesion, aspirin is used less commonly as an analgesic in pediatrics because of its association with Reye’s syndrome. NSAIDs are most effective as pre-emptive agents, or for treatment of mild to moderate pain of somatic origin. Acetaminophen is used widely for minor pain and discomfort. Dosage guidelines for aspirin and other analgesics are summarized in Table 106-1. As excess dosing can cause hepatic failure in infants and children, maximal daily doses are also listed. Other NSAIDs, most commonly ibuprofen and naproxen, have gained wide acceptance in pediatric use, and are equally effective. For children who cannot tolerate oral dosing, ketorolac is available. NSAIDs provide a weak analgesia effect that tends to be more effective for pain that has an inflammatory component, as with postoperative pain. The concurrent use of NSAIDs can reduce opioid dosing needed for effective pain management. The use of more than one NSAID concurrently offers little therapeutic advantage and increases risks for side effects, such as gastrointestinal ulceration and bleeding. NSAIDs used in conjunction with corticosteroids augment risks of serious gastrointestinal complications.
Opioids
Opioids are the mainstay of treatment of severe pain, operative procedures, postoperative pain relief, and management of chronic painful medical conditions in neonates and children [Davies et al., 2008b; Berde and Sethna, 2002; Golianu et al., 2000; Stevens et al., 2000]. Opioids bind to brain and spinal cord opiate receptors to block neurotransmitter production. Mu-receptor agonists, such as morphine, codeine, fentanyl, hydrocodone, and hydromorphone, are effective drugs for all pain intensities and are first-line choices for pain management. Agonist–antagonist drugs are not recommended, as they have an analgesic ceiling, may precipitate withdrawal if given concomitantly with full agonists, and have limited routes of administration. Suggested guidelines for opiate-naive patients are shown in Table 106-1. As opiate agonists have no therapeutic ceiling, dosages should be adjusted to meet the patient’s individual needs. The overall safety and efficacy of opioids are well established. In children, as in adults, the risks of addiction after receiving opioids for pain are low; thus, clinicians should not hesitate to treat pain aggressively. However, increased risks for respiratory depression in infants less than 6 months of age require close cardiorespiratory and saturation monitoring in settings in which emergent airway management is feasible. Respiratory depression is seen more commonly when sedatives are used. Methadone, a long-acting opioid agonist, has been utilized in combination therapy for children with cancer pain, as it adds to the opioid analgesia and prevents or reverses a portion of the opioid tolerance [ Davies et al., 2008b; Gold et al., 2006]. Fentanyl is the drug most often used for short procedures because of its rapid onset (1–2 minutes), peak effect (3–5 minutes), and short duration of action (2–4 hours). Morphine has a somewhat slower onset (5 minutes), with a peak response at 10–30 minutes, and longer duration of action (3–8 hours).
Intravenous bolus or continuous infusions allow more rapid and reliable onset of analgesia that can be titrated easily and reversed quickly by narcotic antagonists. Patient-controlled analgesia can be used in children (generally over age 7 years), but younger children should be under parent or nurse control. Opioids also may be administered subcutaneously, orally, rectally, transdermally, or intranasally. For some procedures, oral transmucosal fentanyl citrate provides an alternative for conscious sedation, although emesis is a frequent side effect. Transdermal fentanyl patches with a drug-release rate of 12.5 μg/hour match the lower dose requirements for pediatric cancer pain control [Zernikow et al., 2009]. Rectal administration can be utilized when oral dosing is contraindicated; intramuscular injection should be used only as a last resort. Adverse effects of opioids include respiratory depression, sedation, vasodilatation, hypotension, bradycardia (fentanyl), muscle rigidity, urinary retention, ileus, seizures, and rigid chest (fentanyl given rapidly). Tolerance may develop more rapidly with continuous infusions and with use of synthetic opioids. Characteristic withdrawal symptoms, including irritability, hypertonicity, diaphoresis, fever, and emesis, can occur when opioids are discontinued abruptly after several days’ exposure.
Procedural Sedation and Analgesia
Most minor procedures that are minimally invasive can be performed using a mild analgesic and sedation. Nonpharmacologic pain management strategies may also decrease the need for pharmacologic treatment. Among those demonstrated as effective are perioperative preparation, relaxation training, distraction, guided imagery, cognitive interventions, and hypnosis [Khan and Weisman, 2007]. More uncomfortable procedures require deeper sedation, more appropriately performed by anesthesiologists, intensivists, or emergency physicians trained in advanced life-support and experienced in deep sedation techniques and monitoring. The American Academy of Pediatrics has defined two levels of sedation less deep than general anesthesia [AAP, 2002]. Conscious sedation is a medically controlled state of depressed consciousness that:
Deep sedation is a medically controlled state of depressed consciousness or unconsciousness from which the patient is not easily aroused, loses protective airway reflexes, and cannot maintain an airway or respond purposefully to physical stimulation or verbal command. Guidelines for sedating children undergoing therapeutic or diagnostic procedures have been reviewed [Krauss and Green, 2000]. A recent review details procedural pain management in neonates [Lago et al., 2009].
Sedation
Benzodiazepines are the most commonly used drugs for sedating children, particularly in pediatric intensive care. Midazolam is the preferred drug for procedural sedation. It has a rapid onset of action (1–5 minutes) and a short half-life (1–12 hours). Available for intravenous, intramuscular, intrathecal, or enteral routes, it provides potent sedation, some muscle relaxation, memory loss, and anxiolysis. Oral or intravenous routes are preferable for children; nasal administration causes an intense irritant response. As it has shorter duration than diazepam or lorazepam, midazolam is a more appropriate choice for brief procedural sedation. Oral diazepam avoids the pain of intravenous injection and the variable absorption of intramuscular doses. For painful procedures, benzodiazepine sedation should be accompanied by opioid analgesia, and the patient should be monitored for hypoxia or respiratory depression. Midazolam can be reversed by flumazenil. Barbiturates are regarded as the sedatives of choice for diagnostic imaging in children under 3 years of age, but provide no analgesia. Barbiturates lower the pain threshold, especially when pain is already present. Intravenous pentobarbital, rectal methohexital, and thiopental are the drugs most extensively used for procedural sedation. Chloral hydrate, an acceptably safe alternate sedative without analgesic efficacy, can be used for nonpainful procedures; the oral or rectal dose is 25–100 mg/kg (maximum dose, 2 g). Its use is largely restricted to sedation for electroencephalograms and diagnostic imaging in young children under 3 years of age. Its extremely long half-life in neonates mitigates against repeated administration [Mayer et al., 1991], and other concerns have been raised about potential carcinogenicity and genotoxicity in mice, even when it is given as a single low dose [Salmon et al., 1995]. Given at subanesthetic doses, intravenous ultra-short-acting agents (etomidate, methohexital, propofol, remifentanil, and thiopental) can be used for procedural pain management, but should be used only by certified practitioners experienced in dealing with the potential for over-sedation or rapid swings in consciousness.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree