Fig. 14.1
(a–c) Artist’s depiction of a technique for minimally invasive sacroiliac screw placement. A small skin and muscle opening is placed medial to the PSIS to allow entry into the cancellous bone. Cannulation then occurs under fluoroscopic guidance. (d) Percutaneous cannulated iliac screws measuring 8 mm in diameter and 65 mm long
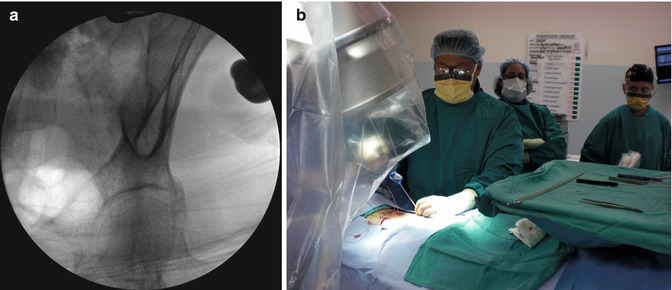
Fig. 14.2
(a) Obturator outlet view with fluoroscopy demonstrating the “teardrop” projection as the idealized endpoint for the screw tip. (b) Intraoperative view show the coronal and sagittal angulation needed to obtain the obturator outlet view to allow percutaneous screw placement over a guidewire, with screw extensions to allow for construct assembly
The screw entry site is located just ventral to the posterior superior iliac spine (PSIS). A drill or small osteotome is used to remove the cortical bone so that the screw head may be recessed to minimize hardware prominence. This entry site into the cancellous bone also minimizes the risk of inadvertent entry into the sacroiliac joint. A Jamshidi needle is then advanced to a depth of 80 mm under fluoroscopic guidance to keep the tip of the needle within the teardrop. This is followed by K-wire exchange and placement of a cannulated awl, tap, and instrumentation with Viper™ titanium alloy percutaneous iliac screws (Depuy Spine, Inc, Raynham, Massachusetts).
Hardware connections were made between screws and rods with the assistance of screw extensions. Subfascial rod passage was performed in a cranial to caudal direction by inserting the rod through the most cranial screw’s incision. This allowed for precise control of the length of rod passed beyond the iliac screw saddle distally in an effort to minimize hardware prominence. In several cases two-plane rod bending was necessary to place the distal rod laterally to meet the iliac screw head.
14.3 Clinical Applications
We have placed 61 sacropelvic screws using this technique [18]. All patients underwent CT scanning with three-dimensional reconstruction to assess screw placement and were found to have no bony breaches. This experience has increased our confidence that the targeting method innovated by Chapman and colleagues is reliable and safe. Furthermore, use of the obturator outlet view does not require special equipment, image guidance, or other advance technique.
We have applied percutaneous iliac screws in the settings of spinal infection, trauma, deformity, and neoplasia (Figs. 14.3, 14.4, and 14.5). In these settings, its use has been for the same indications and biomechanical purposes as traditional open sacroiliac fixation. It should also be noted that later explantation of screws may also be necessary given the relatively high rates of screw loosening with long-term follow-up after fusion has occurred.
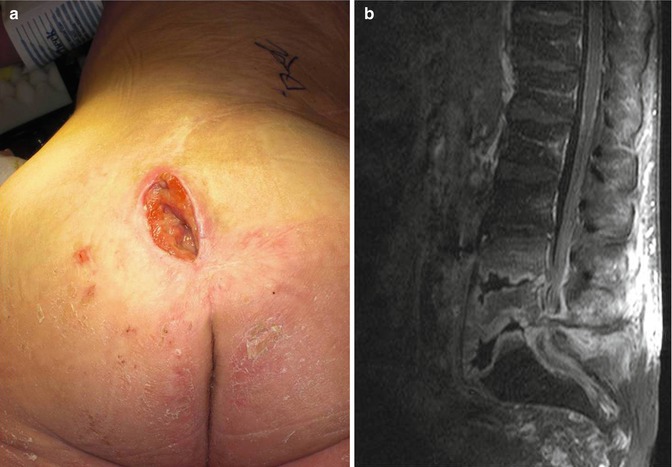
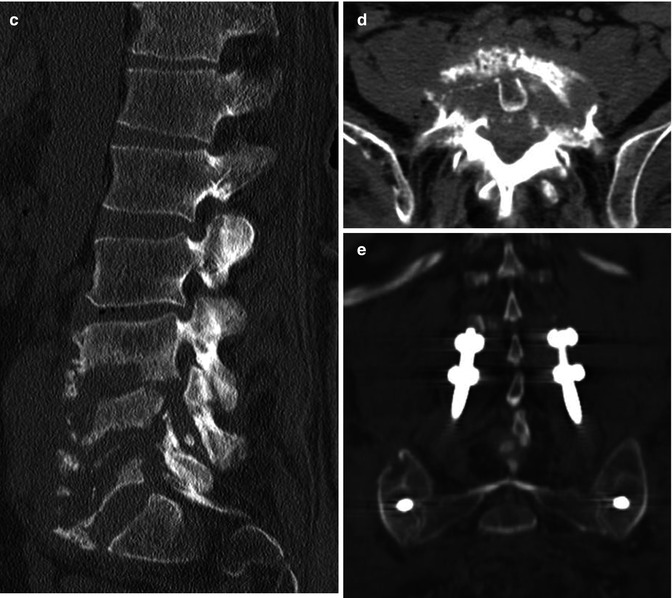
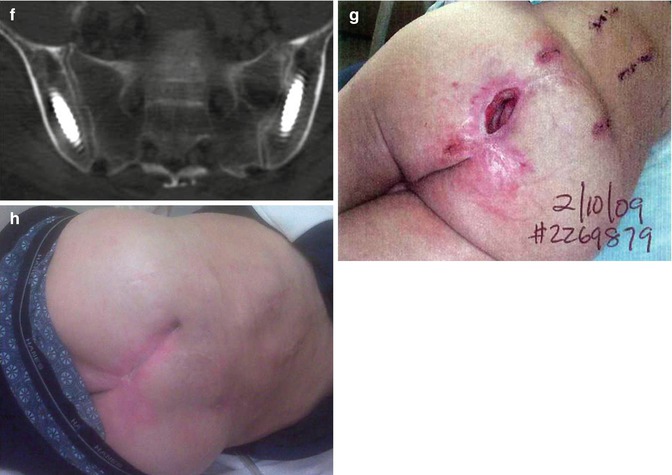
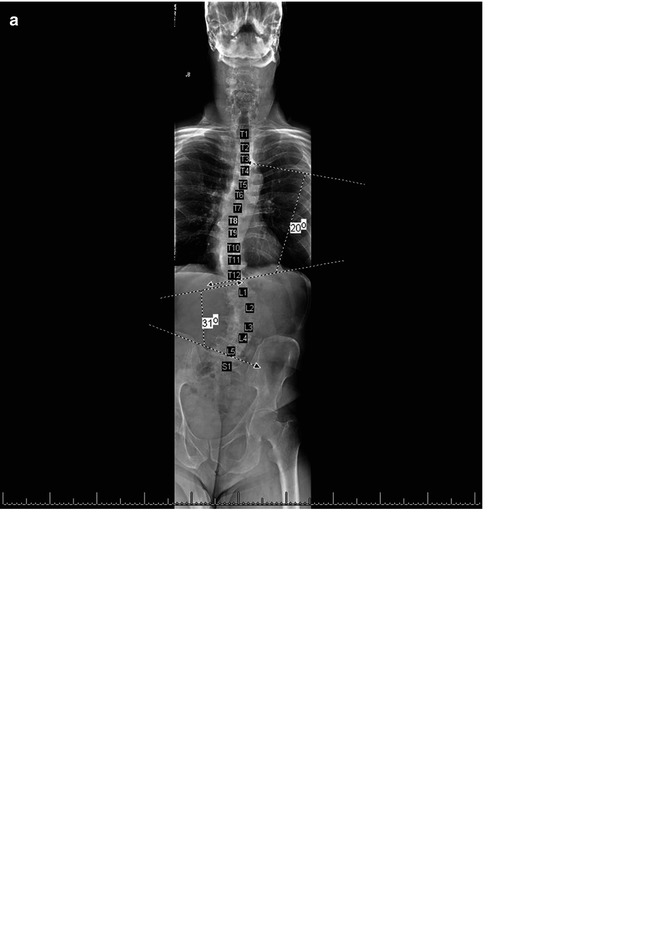
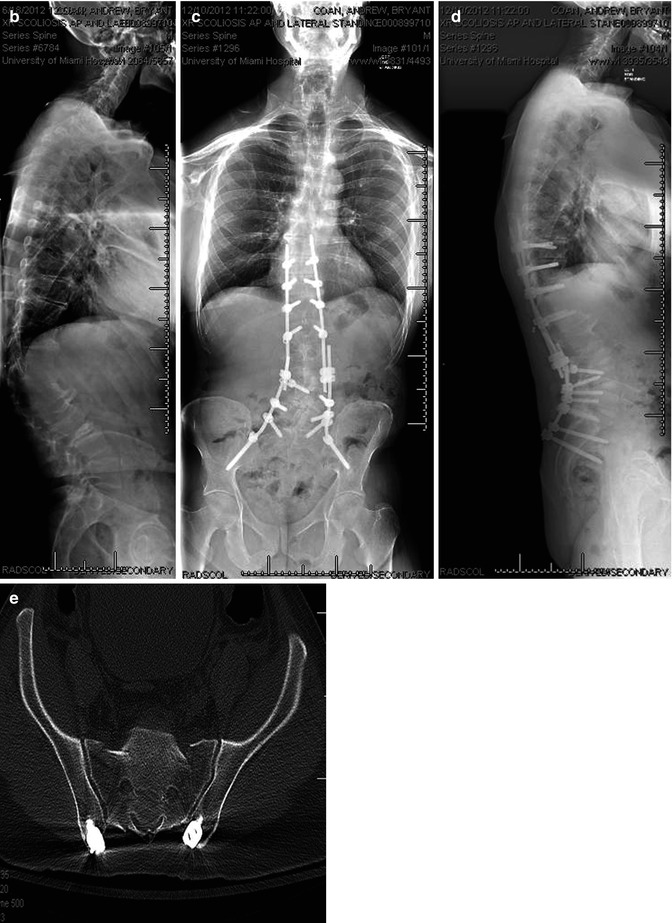
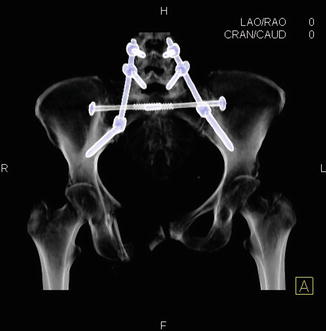



Fig. 14.3
(a) Case of a 46-year-old paraplegic who developed a sacral decubitus ulcer. This was treated with a local flap, which failed, and he subsequently developed osteomyelitis at the lumbosacral junction due to exposed bone. (b and c) The patient failed 6 months of intravenous antibiotic treatment with progression of osteomyelitis and back pain with deformity and bony destruction as demonstrated on MRI and CT imaging. (d) The patient was treated with an anterior debridement of L4–S1 with iliac crest autograft reconstruction and (e) percutaneous instrumentation from L4 to the ilium. (f) Proper iliac screw placement was confirmed with CT scanning. (g) The surgical incisions avoided the infected and affected soft tissues. (h) Fixation, debridement, and antibiotic treatment resulted in resolution of the open wound without need for another soft tissue flap to promote healing


Fig. 14.4
(a–d) AP and lateral imaging of a patient with lumbar degenerative scoliosis and positive sagittal balance which was treated with minimally invasive interbody fusion and percutaneous instrumentation demonstrating the use of percutaneous iliac screws in correction with S1 pedicle screws. (e) CT scanning demonstrates proper recession of screw saddles to minimize hardware prominence

Fig. 14.5




Postoperative imaging demonstrating application of iliac screws in concert with an iliosacral pin to treat a complex sacropelvic fracture
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








