37 Posterior Cervical Foraminotomy
I. Key Points
– The posterior cervical foraminotomy approach (also referred to as laminoforaminotomy) allows nerve root decompression without the need to enter the disc space.
– In contrast to the anterior discectomy approach, posterior cervical foraminotomy is not destabilizing; therefore, there is no need for fusion/implants or harvesting autograft.
II. Indications and Contraindications
Indications
– Cervical neuroforaminal nerve root compression by a (lateral) soft disc herniation or spondylosis (osteophyte) with progressive or intractable cervical radiculopathy
– Cervical nerve root decompression if an anterior approach is not desirable (recurrent surgery, difficult anterior approach, cervicothoracic levels).
Contraindications
– Primary axial neck pain
– Cervical instability at the involved level
– Cervical myelopathy
– Severe kyphosis
– Large central disc herniation
– Central spinal canal stenosis
III. Technique
Patient Positioning
– After induction of general endotracheal anesthesia the patient is positioned in a prone position with the head clamped in a Mayfield head holder (Schaerer Mayfield, Randolph, MA) or in Gardner-Wells tongs with 5 to 10 pounds of traction. The advantages of traction are interspace distraction and stability.
– Alternatively, the patient can be positioned in a (semi)sitting position with the head clamped in a Mayfield head holder. The sitting position reduces venous pressure and reduces intraoperative blood loss. Additionally, the position of the head in relation to the cervical spine can be better adjusted than in a prone position.
– The (semi)sitting position carries the risk of air embolism and requires the placement of a precordial or intraesophageal Doppler probe and a central venous line for air aspiration in case of an embolism.
– The (semi)sitting position is contraindicated in patients with a patent foramen ovale and the possibility of paradoxical arterial embolism.
Preparation and Draping
– Confirmation and adequate visualization of the correct level with plain x-ray or fluoroscopy in a lateral position is mandatory.
Incision, Soft-Tissue Dissection, and Spine Exposure
Classical Procedure
– Posterior midline incision approximately 3 to 4 cm in length for an open microsurgical approach
– Exposure and incision of the nuchal fascia
– Unilateral, subperiosteal dissection of the muscle layers from the spinous process and lamina to the facet joint with a Bovie cautery (Bovie Medical Corp., Clearwater, FL) and a Cobb elevator. Supra- and interspinal ligaments should be preserved.
– Placement of a retractor and radiographic confirmation of the correct level
Minimally Invasive Procedure
– The proper incision site is marked with a spinal needle and lateral fluoroscopy. The incision is centered slightly rostral to the intended level of decompression.
– The skin incision is made approximately 2 cm lateral to the midline.
– If a retractor system is used (small-blade retractor, tubular retractor), only very small incisions are necessary (1.5 to 2 cm).
– Incise the fascia with a Bovie cautery.
– With the use of a bladed retractor, blunt dissection is performed with a finger down to the level of the lamina.
– If a tubular retractor system is used, a K-wire is positioned on the inferior articular facet of the upper vertebral body under fluoroscopic guidance. In this situation it is imperative that the K-wire engage bone at all times.
– Serial dilators are used to bluntly widen the approach through the muscles, and finally the tubular retractors are placed.
– A final radiographic check is recommended to confirm the correct level.
– The retractor should be placed on the interlaminar space (twothirds) and on the facet joint (one-third).
– Bring in the draped microscope.
Foraminotomy and Wound Closure
– Expose and mark the cranial and caudal lamina of the appropriate level and check again with fluoroscopy.
– Expose the medial parts of the capsule of the facet joint.
– Perform a laminotomy by removing bone from the lateral parts of the caudal and cranial lamina with a high-speed drill or with a small Kerrison rongeur.
– Open the ligamentum flavum with a nerve hook or a dissector, and resect it with a small Kerrison rongeur.
– Extend the laminotomy cranially and laterally, and expose the lateral edge of the dura and the nerve root. The nerve root is generally displaced dorsally.
– Try to remove free disc material under the nerve root with a nerve hook and a pituitary rongeur.
– If the disc sequestrum is still covered with layers of the posterior longitudinal ligament, it has to be opened with a small dissector or with bipolar forceps.
– Undercut the superior articular process with 1 and 2 mm Kerrison rongeurs until the entire foramen is patent (but preserve at least 50% of the facet) (Fig. 37.1).
– Epidural bleeding is controlled with Gelfoam (Pfizer, New York) and Cottonoids (Saramall, Buenos Aires, Argentina).
– Placement of a wound drain (Hemovac [Gohar Shafa, Tehran, Iran]) is usually not necessary.
– Close fascia with 0 or 2-0 absorbable sutures.
– Use inverted, interrupted 3-0 absorbable sutures for closure of the subcutaneous layer.
– Close the skin with a running, absorbable intracutaneous suture or with staples.
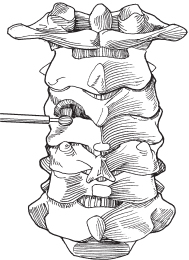
Fig. 37.1 Foraminotomy. The superior articular process can be removed by using a burr to thin it and a 1 mm Kerrison rongeur to remove remaining articular process, leaving the nerve root decompressed. (From Vaccaro AR, Albert TJ, Spine Surgery: Tricks of the Trade 2nd ed, Thieme; pg. 7, Fig. 2.3D.)
IV. Complications
– Wound dehiscence
– Wound infection and epidural abscess (1.2%)1
– Cerebrospinal fluid (CSF) leak (0.6 to 2.5%)1,2
– Neurologic deterioration due to injury or manipulation of the nerve root or spinal cord or postoperative epidural hematoma
– Air embolism (sitting position) (1.6 to 2.3%)2,3
– Persistent radiculopathy indicating residual nerve root compression, epidural scarring, early recurrent disk herniation, or neuropathic pain requiring additional surgery (5.1 to 8%)1,2
– Recurrent disk herniation (7.6%)2
– Intraoperative hemorrhage caused by epidural veins or as a result of an inadvertent injury to vertebral artery (very rare and usually due to a wrong approach)
– Secondary instability due to excessive resection of the facet joint (4.9%)1
– Loss of cervical lordosis (18.5%)1
V. Postoperative Care
– Mobilize patient immediately after surgery.
– There is no need for external bracing; patients typically have full range of neck motion.
– Pain control is usually achieved with orally administered opioids.
– Discharge patients when discharge criteria are met (usually on post-op day 1).
VI. Outcomes
– Large series have reported excellent or good outcomes for posterior cervical foraminotomy in 90 to 96% of patients with monoradiculopathy.1,2,4
VII. Surgical Pearls
– Removal of more than 50% of the facet significantly compromises torsional stiffness of the cervical spine.5
– The entire length of the foramen can be enlarged safely with the use of curettes or a high-speed drill with preservation of more than 50% of the facet by initially working parallel and just inferior to the nerve root and then, as more room is gained, removing the rim just dorsal to the nerve root.
– Minimal bone removal (keyhole exposure) is acceptable, but not at the expense of excessive nerve root retraction or insufficient exposure of the dura with an increased risk of dural laceration.
Common Clinical Questions
1. What are the most common indications for a posterior cervical foraminotomy?
2. What are the two options for performing a posterior cervical foraminotomy?
3. How much of the facet joint can safely be removed without creating instability, and how much of the facet joint is usually removed during a posterior cervical foraminotomy?
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







