Chapter 169 Posterior Lumbar Interbody Fusion
The introduction of novel fixation techniques and instrumentation has resulted in their ever increasing application for arthrodesis of the spine. The first successful report of a posterior lumbar interbody fusion (PLIF) dates to 1940, when Cloward performed this operation using a spinous process autograft.1 Since Cloward’s original report, many surgeons have modified this technique using various grafts.2–6 In recent years, two major improvements have resulted in greater application of PLIF or its variants: the application of pedicle screws to augment the rate of arthrodesis7,8 and the application of minimally invasive spine techniques to perform arthrodesis in a percutaneous fashion.9
The indications for performing a PLIF include recurrent disc herniation, failed back surgery syndrome, spondylolisthesis, bilateral midline disc herniation, segmental instability, and degenerative disc disease. Compared with classic posterolateral arthrodesis techniques, PLIF offers improved blood supply to the fusion/graft construct, balanced load sharing on the graft, complete decompression of the neural elements, a wide area of graft–intervertebral body contact, and restoration of the interbody and neural foraminal height.10–12 Herein, we describe our surgical technique for open and minimally invasive PLIF.
Open PLIF
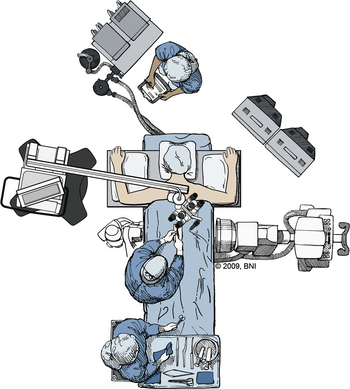
After the patient is placed in the prone position, pressure points are padded to minimize pressure sores (Fig. 169-1). A Jackson table can be used to avoid compression and venous congestion, which may cause excessive bleeding during posterior approaches. Fluoroscopy should be used to identify the spinal level of interest. As in any posterior approach, the landmarks are the spinous processes, iliac crest, and posterior superior iliac spine.
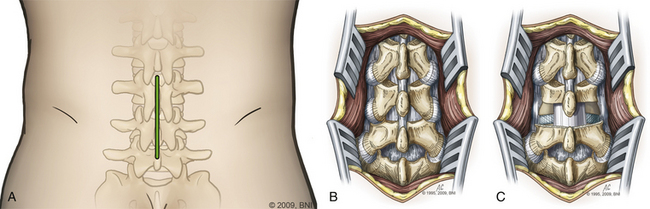
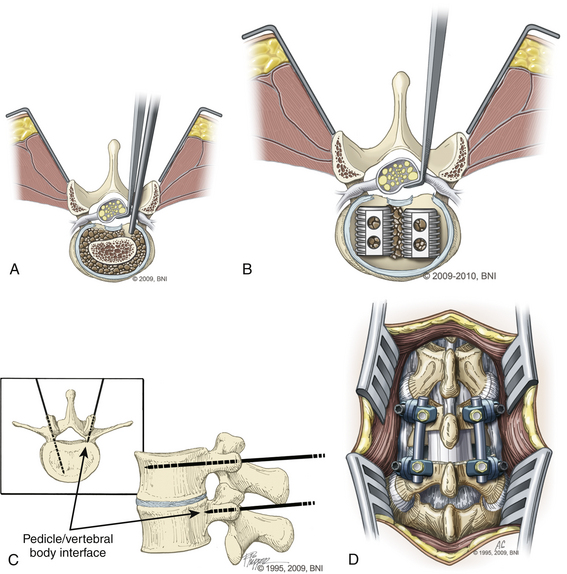
The skin is incised (Fig. 169-2A) in the midline above the spinous process, and the subcutaneous tissue is dissected. The thoracolumbar fascia is incised and dissection proceeds in a subperiosteal fashion, detaching the paraspinal muscles from the spinous process and lamina (Fig. 169-2B). For each level that is to be treated, the cranial lamina and ligamentum flavum are removed completely (Fig. 169-2C). The cranial aspect of the caudal lamina should also be removed to gain adequate access to the interbody space. To prevent traction on the spinal cord or nerve roots during placement of the interbody graft, a wide window is created by resecting the lower third of the inferior facet and the medial two thirds of the superior facet. Next, the nerve root and dural sac are retracted medially, creating maximal exposure of the interbody space for removal of any bony or disc material (Fig. 169-3A).
Following adequate decompression of the neural structures and removal of the disc material, the disc space is distracted using pedicle screws or disc space distractors. We prefer to use pedicle screws as distractors (Fig. 169-3B). Next, the end plates are prepared, using curettes to remove any remaining disc material while preserving the bony end plates to prevent graft subsidence. Adequate preparation of the graft site and preparation of the end plates are important steps for ensuring a proper fusion.
Next, a graft spacer or cage is placed into the interbody space under direct visualization of the cranial and caudal nerve roots (Fig. 169-3C). Bone graft packing is used to augment the fusion. The graft choice is highly surgeon dependent, with options such as threaded cages, titanium mesh cages, and auto- and allograft with or without the use of bone morphogenetic protein. The graft-filled interspace is stabilized with internal fixation using screws and rods or a plate construct to aid in fusion and immobilization (Fig. 169-3D).
PLIF is an effective procedure and results in excellent fusion (Fig. 169-4) with rates in the range of 80% to 98%.13,14 PLIF also has been shown to be effective for reducing pain and disability.13
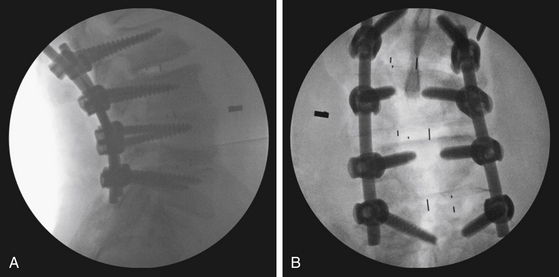
FIGURE 169-4 (A) Posterior and (B) anteroposterior computed tomography scan of the final construct after an open PLIF.
(Used with permission from Barrow Neurological Institute.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree