Chapter 25 Proximal, Distal, and Generalized Weakness
Clinical Presentation by Affected Region
Neck, Diaphragm, and Axial Muscles
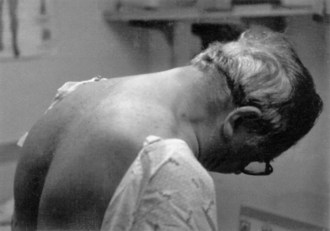
Neck muscle weakness becomes apparent when the patient must stabilize the head. Riding as a passenger in a car that brakes or accelerates, particularly in emergencies, may be disconcerting for the patient with neck weakness, because the head rocks forward or backward. Similarly, when the patient is stooping or bending forward, weakness of the posterior neck muscles may cause the chin to fall on the chest. A patient with neck-flexion weakness often notices difficulty lifting the head off the pillow in the morning. As neck weakness progresses, patients may develop the dropped head syndrome, in which they no longer can extend the neck, and the chin rests against the chest (Fig. 25.1). This posture leads to several secondary difficulties, especially with vision and swallowing.
Bedside Examination of the Weak Patient
Observation
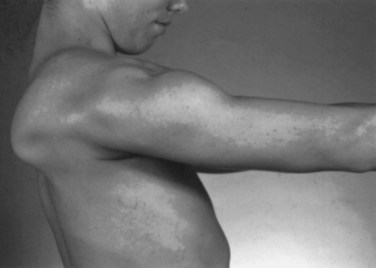
Weakness of the shoulder muscles causes a characteristic change in posture. Normally the shoulders brace back by means of the tone of the muscles, so the hands are positioned with the thumbs forward when the arms are by the side. As the shoulder muscles lose their tone, the point of the shoulder rotates forward. This forward rotation of the shoulder is associated with a rotation of the arm, so that the backs of the hands now are forward facing. Additionally, the loss of tone causes a rather loose swinging movement of the arms in normal walking. When shoulder weakness is severe, the patient may fling the arms by using a movement of the trunk, rather than lifting the arms in the normal fashion. In the most extreme example, the only way the patient can get the hand above the head on a wall is to use a truncal movement to throw the whole arm upward and forward so the hand rests on the wall, and then to creep the hand up the wall using finger movements. Atrophy of the pectoral muscles leads to the development of a horizontal or upward sloping of the anterior axillary fold. This is especially the case in facioscapulohumeral (FSH) muscular dystrophy. The examiner may observe winging of the scapula, a characteristic finding in weakness of muscles that normally fix the scapula to the thorax (i.e., the serratus anterior, rhomboid, or trapezius). As these muscles become weak, any attempted movement of the arm causes the scapula to rise off the back of the rib cage and protrude like a small wing. The arm and shoulder act as a crane—the boom of the crane is the arm, and the base is the scapula. Obviously, if the base is not fixed, any attempt to use the crane results in the whole structure’s falling over. This is the operative mechanism with attempts to elevate the arm; the scapula simply pops off the back of the chest wall in a characteristic fashion. In the most common type of winging, the entire medial border of the scapula protrudes backward. In some diseases, particularly FSH muscular dystrophy, the inferomedial angle juts out first, and the entire scapula rotates and rides up over the back. This often is associated with a trapezius hump, in which the middle part of the trapezius muscle in the web of the neck mounds over the upper border of the scapula (Fig. 25.2). Note that when examining a slender person or a child, in whom prominent shoulder blades are common, the shoulder configuration returns to normal with forcible use of the arm, as in a push-up.
Muscle Bulk and Deformities
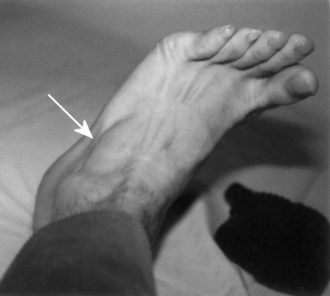
Assessment of muscle bulk looking for atrophy and hypertrophy is an important part of the neuromuscular examination. Prominent muscle wasting usually accompanies neurogenic disorders associated with axonal loss. However, severe wasting also occurs in chronic myopathic conditions. Wasting is best appreciated in the distal hand and foot muscles and around bony prominences. In the arm, wasting of the intrinsic hand muscles produces a characteristic hand posture in which the thumb rotates outward so that it lies in the same plane as that of the fingers (the simian hand), and the interphalangeal joints flex slightly with slight extension of metacarpophalangeal joints (the claw hand). Wasting of the small muscles leaves the bones easily visible through the skin, resulting in the characteristic guttered appearance of the back of the hand. In the foot, one of the easier muscles to inspect is the extensor digitorum brevis, a small muscle on the lateral dorsum of the foot that helps dorsiflex the toes (Fig. 25.3). It often wastes early in neuropathies and anterior horn cell disorders. In myopathic conditions in which proximal muscles are affected more than distal muscles, the extensor digitorum brevis may actually hypertrophy to try to compensate for weakness of the long toe dorsiflexors above it.
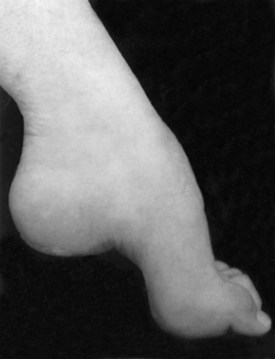
Several bony deformities often provide important clues to the presence of neuromuscular conditions. Proximal and axial muscle weakness often leads to scoliosis. Intrinsic foot muscle weakness present from childhood often leads to the characteristic foot deformity of pes cavus, in which the foot is foreshortened with high arches and hammer toes (Fig. 25.4). Pes cavus is a sign that weakness has been present at least since early childhood and implies a genetic disorder in most patients. Likewise, a high-arched palate often develops from chronic neuromuscular weakness present from childhood.
Strength
In an office situation and in many clinical drug trials, manual muscle testing gives perfectly adequate results and is preferable to fixed myometry in young children. The basis is the Medical Research Council grading system, with some modification (Table 25.1). This method is adequate for use in an office situation, particularly if supplemented by the functional evaluation. A scale of 0 to 5 is used, in which 5 indicates normal strength. A grade of 5 indicates that the examiner is certain a muscle is normal and never used to compensate for slightly weak muscles. Muscles that can move the joint against resistance may vary quite widely in strength; grades of 4+, 4, and 4− often are used to indicate differences, particularly between one side of the body and the other. Grade 4 represents a wide range of strength, from slight weakness to moderate weakness, which is a disadvantage. For this reason, the scale has been more useful in following the average strength of many muscles during the course of a disease, rather than the course of a single muscle. Averaging many muscle scores smoothes out the stepwise progression noted in a single muscle. This may demonstrate a steadily progressive decline. A grade of 3+ is assigned when the muscle can move the joint against gravity and can exert a tiny amount of resistance but then collapses under the pressure of the examiner’s hand. It does not denote the phenomenon of sudden give-way, which occurs in conversion disorders and in patients limited by pain. Grade 3 indicates that the muscle can move the joint throughout its full range against gravity, but not against any added resistance. Sometimes, particularly in muscles acting across large joints such as the knee, the muscle is capable of moving the limb partially against gravity but not through the full range of movement. A muscle that cannot extend the knee horizontally when the patient is in a sitting position but can extend the knee to within 30 to 40 degrees of horizontal is graded 3−. Grades 2, 1, and 0 are as defined in Table 25.1.
Table 25.1 The Medical Research Council Scale for Grading Muscle Strength
| Grade | Description |
|---|---|
| 0 | No contraction |
| 1 | Flicker or trace of contraction |
| 2 | Active movement with gravity eliminated |
| 3 | Active movement against gravity |
| 4 | Active movement against gravity and resistance |
| 5 | Normal power |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree