Fig. 9.1
MisLAT algorithm
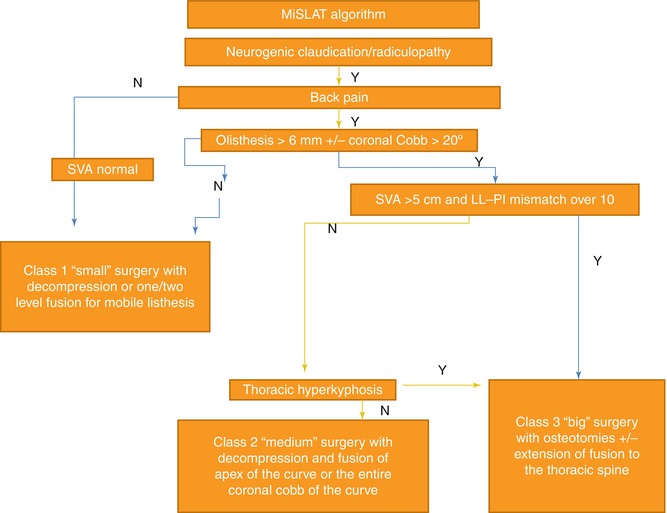
Fig. 9.2
Abbreviated MisLAT algorithm
9.5 The MiSLAT Algorithm
9.5.1 MiSLAT Treatment Level I
This patient population typically presents with symptoms consistent with neurogenic claudication due to central and/or lateral recess stenosis. These patients have no significant degree of back pain and/or any complaints consistent with their deformity. These patients do not have sagittal or coronal imbalance. The treatment goal is nerve root decompression and not deformity correction. Minimally invasive techniques are well suited for this treatment level. Typically, a tubular retractor is used to perform an ipsilateral hemilaminotomy and foraminotomy. Then, by angling the tubular retractor medially, an undercutting contralateral decompression is also possible (“ipsi-contra” decompression). This type of “ipsi-contra” minimally invasive tubular decompression may be performed at one or two contiguous levels through one small incision. However, the presence of radiographic instability precludes this approach/procedure. Patients in this treatment level cannot have subluxation of greater than 2 mm and no sagittal and/or coronal imbalance, and the curve should be less than 30°.
9.5.2 MiSLAT Treatment Level II
Typically in the MiSLAT level II cases, the decompression involves levels of the spine which are radiographically unstable and concomitant focal instrumentation at the area of decompression is recommended. This treatment level can be achieved via minimally invasive techniques as well. This level of treatment is well suited for patients who have neurogenic claudication, minimal to moderate low back pain, Cobb angles less than 30°, >2 mm subluxation, and lack of anterior bridging osteophytes at the decompression site. However, these patients should not have lumbar kyphosis or global imbalance. These patients benefit from focal decompression and minimally invasive fixation/fusion of the decompressed levels – typically using an expandable tubular retractor to perform a transforaminal interbody fusion with mini-open or percutaneous pedicle screw fixation at one or two contiguous levels.
MiSLAT treatment levels I and II are considered “small” surgery in the abbreviated MiSLAT algorithm (Fig. 9.2).
9.5.3 MiSLAT Treatment Level III
These patients suffer from back pain in addition to neurogenic claudication and radiculopathy. They have over 2 mm of subluxation, lack anterior bridging osteophytes, and Cobb angles greater than 30°. Besides extensive decompression and focal instrumentation at the decompressed levels of the lumbar spine, anterior or posterior interbody fusion of the apex of the lumbar curve is typically needed. Here again, minimally invasive techniques are well suited as they achieve the same goals as the open approaches. As with treatment level I, extensive decompression at multiple levels can be done through expandable tubular retractors; and, as with treatment level II, instrumentation can be performed via percutaneous or mini-open techniques, and interbody grafting achieved posteriorly via tubular retractors. Alternatively, minimally invasive lateral interbody procedures or anterior interbody fusions may be used with concomitant posterior percutaneous fixation. These anterior or lateral interbody procedures allow for indirect foraminal decompression by distracting the interbody space.
9.5.4 MiSLAT Treatment Level IV
These patients have claudication-radicular symptoms, back pain, and lumbar hypolordosis/kyphosis. The goal of the operative intervention includes decompression, instrumentation, interbody fusion, and correction of lumbar flat back or kyphosis. Radiographs of these patients demonstrate segmental instability and loss of lumbar lordosis, but no significant global imbalance (SVA < 5 cm) (Fig. 9.3a–d). As already delineated, decompression, instrumentation, and interbody graft placement and arthrodesis can all be undertaken via minimally invasive techniques. Lordotic interbody grafts are typically placed from a minimally invasive lateral approach prior to posterior segmental mini-open or percutaneous pedicle screw instrumentation. The minimally invasive laterally placed interbody cages not only serve in kyphoscoliosis correction and derotation but also place the pedicles in a more “physiologic” angle, making dorsal pedicle fixation easier. Particular attention is paid to restoring normal segmental lordosis in the lower levels of correction, particularly at L4–L5 and L5–S1 (typically via TLIF), as two-thirds of lumbar lordosis comes from these two segments. Also, it is important to match the lumbar lordosis to the patient’s individual pelvic incidence plus/minus ten degrees [12, 15, 16]. MiSLAT IV treatment typically involves fixation of the Cobb angles of the lumbar curve (beyond just the apex of the curve). If the curve extends to S1 or if the L5–S1 disc space is collapsed, then the instrumentation may need to extend to S1. In these cases, it may also be necessary to place iliac instrumentation in long fusions (L2 or above to sacrum) to help achieve a solid fusion at the lumbosacral junction and avoid sacral insufficiency fracture. Recent advances in minimally invasive techniques allow iliac screw fixation via percutaneous minimally invasive techniques [17]. MiSLAT III and IV levels are “medium” surgery in the simplified algorithm (Fig. 9.2).
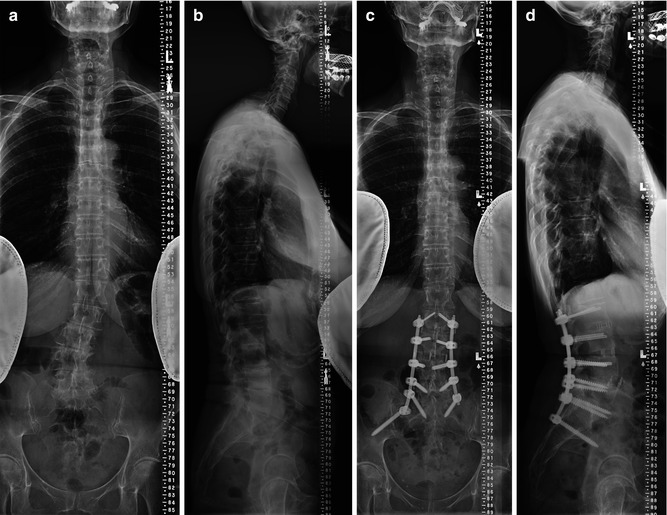

Fig. 9.3
Example of MisLAT IV patient
MiSLAT levels I–IV can now be performed using current minimally invasive techniques. Basic principles of proximal and distal fusion levels established for open surgery are also applicable to minimally invasive deformity treatment. As the soft tissue overlying the spine is preserved with minimally invasive approaches, typical cranial stopping points for multilevel lumbar instrumentation in MiSLAT IV treatments may vary from T10 to L2.
9.5.5 MiSLAT Treatment Levels V and VI
Schwab et al. recently updated the previous published SRS-Schwab classification to incorporate the spinopelvic parameters, which is highly correlated with HRQOL scores [18]. The classification is comprised of curve type, which is aimed at describing the relevant coronal aspects of the deformity and three modifiers to characterize sagittal components of the deformity. The inter- and intra-rater reliability and inter-rater agreement for the updated classification are excellent. When it comes to utilizing minimally invasive procedures to treat patients classified with SRS-Schwab classification, the patients with PI-LL modifier “B” or “C” (i.e., PI-LL value is greater than 20°) and/or global balance modifier “P” or “VP” (i.e., SVA is greater than 5 cm) are typically not suitable for a minimally invasive approach. These patients may need more extensive osteotomies to achieve sagittal vertical axis corrections [19]. These patients would fit into MiSLAT levels V or VI. This is “big” or open surgery in the simplified MiSLAT algorithm (Fig. 9.2).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








