Fig. 62.1
Cavernous-carotid fistula. (a) Axial T2-weighted MR image. (b) Time-of-flight intracranial MR angiography image. Arterial flow void is observed in the right cavernous sinus (a, arrowhead). The right globe is mildly proptotic, with mild enlargement of the extraocular muscles. Flow-related enhancement is seen in the right cavernous sinus (b, arrow), indicating arterialization of the right cavernous sinus
MRI often shows an enlarged (congested) pituitary gland in patients with cavernous sinus dural AVMs [10].
Time-of-flight MR angiography is highly sensitive in detecting flow-related enhancement at the fistula connection extending to the cavernous sinuses immediately adjacent to the fistula (Fig. 62.1b).
Dynamic MRI has been shown to demonstrate asymmetric filling in patients with cavernous sinus AVMs. The side with the dural AVM typically shows reduced enhancement, and the pituitary gland on the whole enhances more slowly than in control subjects [10].
Angiography is the gold standard modality for visualization (and often treatment) of parasellar vascular malformations (Fig. 62.2).
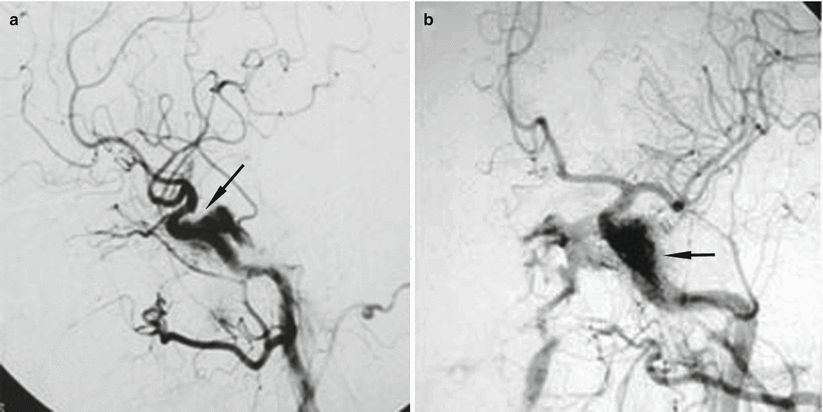

Fig. 62.2
Cavernous sinus dural arteriovenous fistula (DAVF) seen on lateral (a) and anteroposterior (b) digital subtraction angiography (DSA) (Adapted with permission from Kashiwazaki et al. [13])
62.3 Clinical and Surgical Management
Some patients with low-flow cavernous sinus dural AVMs will have spontaneous thrombosis and resolution of the fistula.
In patients with high-flow CCFs and dural AVMs that require intervention, management strategies vary. They typically involve endovascular techniques with embolization of the fistula. The available techniques include coil embolization, balloon embolization, and stent placement. The approach may be done transarterially or transvenously. Every attempt is made to obliterate the fistula while preserving ICA flow.
Successful superselective coil embolization of cavernous sinus dural AVMs has been reported. A majority of patients have excellent outcomes and can be treated in one setting [11, 12]. Cranial nerve paresis may occur in the setting of endovascular treatment for parasellar AVFs and CCFs [13].
Successful long-term embolization of direct (Type A) CCFs is possible in up to 95 % of patients [14].
Five years following treatment, over 80 % of patients with indirect fistulas (Types B–D) are typically cured [6, 14, 15].
Improvement in pituitary gland congestion size has been shown following embolization of cavernous sinus AVMs [7, 10].
Recanalization or recurrence occurs in about 9 % of patients after successful initial embolization [15].
Stereotactic surgery has been successfully used to treat patients with refractory low-flow fistulas. According to one study, 90 % of patients had resolution of the fistula at 7 months following the procedure [16].
References
1.
Gould TJ, Johnson LN, Colapinto EV, Spollen LE, Rodriguez FJ. Intrasellar vascular malformation mimicking a pituitary macroadenoma. J Neuroophthalmol. 1996;16:199–203.CrossRefPubMed
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








