54 Linda P. D’Andrea, JahanGir Asghar, James T. Guille, and Randal R. Betz Vertebral stapling is a method of regulating spinal curvature development in the young patient with a coronal plane deformity. This can be accomplished using traditional or minimal access approaches. Ideally, a surgeon with experience in anterior spine surgery, especially using minimally invasive techniques, should be able to perform this procedure. It may be helpful to enlist the assistance of a general or thoracic surgeon with experience in thoracoscopic and minimally invasive techniques. With the use of these techniques, scoliotic vertebrae from T2 to L4 can be stapled, while limiting the total scar length. Patients who have at least 1 year of growth remaining, have a scoliosis deformity that would be considered for brace treatment, or may have failed or refused bracing are ideal candidates for the stapling procedure. Lenke 1, 3, 5, and 6 scoliosis curves are ideal for treatment with vertebral stapling. Medical contraindications are the same as for any anterior spine or chest procedure and include systemic infection, active respiratory disease such as uncontrolled asthma, or conditions with increased anesthetic risk. Significantly compromised pulmonary function may be a relative contraindication. We do not perform vertebral stapling for curves over 45 degrees, or in those whose curves do not correct to less than 20 degrees on bending films, because prior experience has yielded poor results. In children <8 years old with larger curves, it still may be desirable to perform stapling because of the ability to avoid early fusion and the potential for correction with continued growth, especially if a posterior growth device is added. Kyphosis greater than 40 degrees is also a relative contraindication, because of the potential for the creation of hyperkyphosis with growth. When performing thoracoscopic vertebral body stapling in small children (weighing under 50 lb), it may be difficult for the anesthesiologist to obtain or maintain single-lung ventilation. The child’s airway size may not be compatible with the limited sizes of endotracheal tubes available. In these cases, the use of carbon dioxide (CO2) insufflations for the thoracoscopic portion or two minithoracotomies may be used. If using CO2, it is important to maintain the intrathoracic pressures at 7 to 10 mm Hg. Higher pressures can produce adverse hemodynamic effects (e.g., tachycardia, hypotension). An important principle of insertion is to have the tines of the staples parallel and adjacent to the vertebral body end plates. In order for there to be actual correction of the scoliosis by modulation of the vertebral body growth, the patient should have at least 1 year of growth remaining. Staple tine deployment usually occurs over 5 minutes. The staples should be placed in the inserter, with the tines straightened, and immersed in the sterile ice bath until the moment of insertion. Using flexible or rigid portal sleeves or a nasal speculum to maintain open portals allows for quick passage of the staples while protecting the skin and muscle. If tine deployment is occurring as the staple is being driven into the body, it is essential that the surgeon stop, as the tines may curl enough to penetrate the disk space. If this occurs, the staple should be removed, re-iced, and then reinserted. Although the patient is in the lateral decubitus position, often the flexible, main thoracic curve reduces. To further reduce the curve while placing the staples, lateral pressure to the apical ribs can be applied. The dull staple trial may also be used to push at the apex of the convexity, further reducing the curve prior to staple impaction. This may be important, because evaluation of data from patients who have already undergone the procedure suggests that patients who had the greatest correction at the time of surgery (curve <20 degrees on first erect radiograph) maintained that correction best. If the staples are being placed thoracoscopically, the addition of carbon dioxide (CO2) gas allows for collapse of the lung without single-lung ventilation. Specialized equipment and portals are needed for this technique. Low-pressure CO2 gas also promotes hemostasis in the bleeding bone. Gas pressures should be kept low to prevent a lateral shift of the mediastinum, which may cause a drop in blood pressure. If staple or pilot holes are made but not used, then bone wax may be used to stop bone bleeding. Previously, patients were told to wear a noncorrecting thoracolumbosacral orthosis (TLSO) for a brief time after surgery, but over the last 4 years we have found that this is usually not necessary. In a very active child with stapling of a lumbar curve, we will request that the child wear a lumbosacral corset for 6 to 8 weeks post-surgery. All patients are asked to restrict activities for 4 to 6 weeks to allow for skin and muscles incised during the surgery to heal. Only two staples of 1400 have partially moved with normal activities or vigorous participation in sports (including gymnastics) or dancing. The recommended guideline for choosing levels is to include all vertebrae that lie within the Cobb angle of the curve. The levels that may be safely stapled include T2 to L4. If the vertebrae are small, sometimes only a single two-prong staple can be placed in the upper thoracic spine. Under general anesthesia, patients are placed in the lateral decubitus position with the convex side of the scoliosis curve in the up position. The table is not flexed, and only a small axillary roll is placed. If video-assisted thoracoscopy is being utilized for insertion, then one-lung ventilation will be necessary, unless CO2 gas insufflation is available to displace the lung for visualization of the spine and surrounding structures. After positioning the patient, biplanar fluoroscopy is used to determine the exact location for the intercostal portals before the patient is prepped and draped (Fig. 54.1). The incisions for staple insertion are along the posterior axillary line (Fig. 54.2). The incisions used for staple insertion are slightly larger than the staples themselves. Through each skin incision it is possible to make two to three internal intercostal portals. This allows several levels to be stapled through each skin incision and accommodates the size of the instruments and implants. The insertion device, which holds the single two-prong staples, is 10 mm × 14 mm wide. The staples come in many sizes, with the 12-mm four-prong, double staple being the widest, longest object (at 14 × 12 mm) that has to pass between the ribs (Fig. 54.3). Rigid, autoclavable plastic portals (Medtronic Sofamor Danek, Memphis, TN) have been custom made for this specific use. They allow for the maintenance of the intercostal portal space, quick removal of the staple trial, and placement of the appropriate-sized staple while protecting the muscle and pleura from repeated trauma. Small pediatric Finochietto retractors or nasal speculum distractors can also be used to enlarge the intercostal portals and may be used in place of collapsible or rigid portals.
Intervertebral Stapling for Spinal Deformity
Description
Expectations
Indications
Contraindications
Special Considerations
Tips, Pearls, and Lessons Learned
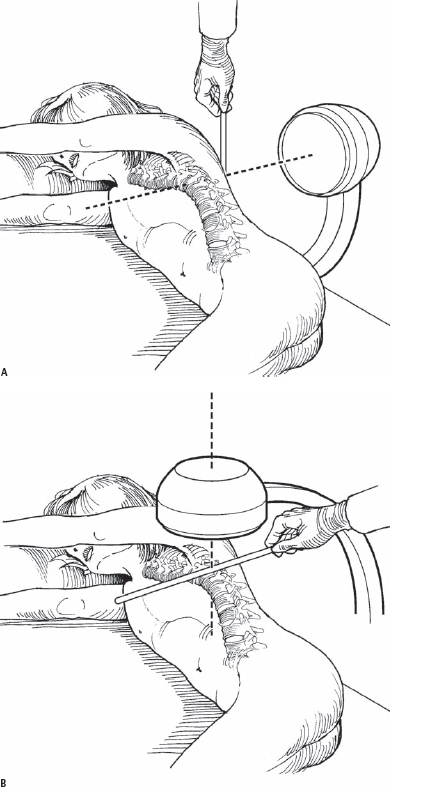
Key Procedural Steps
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







