68 John H. Peloza Lumbar percutaneous pedicle screw fixation has many advantages over other fixation techniques. Pedicle screw fixation provides the most rigid three-column stability to the lumbar spine without compromising the neurovascular or visceral structures. Pedicle screws can be applied in the absence of lamina or facet joints, and are utilized to reduce deformities, stabilize instabilities, and support interbody or anterior implants. In the past, the use of pedicle screws required large exposures causing significant damage to surrounding soft tissues. The retractors caused a relative “compartment syndrome” in the musculature whereas the exposure compromised the vascular and neurologic supply to the muscles. Collectively this caused micro-vascular damage and ischemia, metabolic changes, and eventual necrosis of the musculature. Additionally, older surgical techniques and implants could injure the facet joints and the adjacent segment, possibly contributing to adjacent level disease. Minimal access surgical technologies (MASTs) have several advantages over traditional open techniques. The incisions are small, with minimal muscle stripping or retraction. The majority of surgical procedures including instrumentation can be performed through a tube, avoiding the devascularization and denervation of the musculature and facet joints. With minimal access techniques, there is minimal iatrogenic muscle injury; therefore, the most important dynamic stabilizers of the spine, the muscles, are functional postoperatively. Early surgical results utilizing MAST techniques are encouraging with markedly improved and predictable clinical results. Compared with traditional open techniques, minimally invasive techniques have shown markedly decreased surgical time, blood loss, and postoperative pain. Indications for percutaneous pedicle screw fixation are similar to those of open techniques: Future indication may include revision of total disk arthroplasty (TDA) and posterior dynamic stabilization (supporting TDA or nucleoplasty and dynamic polymer or metal rods). The contraindications for percutaneous pedicle screw fixation are somewhat relative to the surgeon’s skill; however, some universal conditions preclude this technique. Morbidly obese patients may present a problem, as the retractor tubes may not be long enough to reach the spine. Generally, if the distance from the skin to the screw insertion point is greater than 9 cm, the open technique is recommended. Additionally, patients requiring multilevel constructs (greater than three levels) or those with multiplanar deformities requiring multiplanar correction are usually better suited to open techniques. Until minimally invasive systems are improved, most spinal tumors and three-column spinal injuries are also better suited to open techniques. The surgeon must take into account the following key points to safely implant percutaneous lumbar pedicle screws: Patient positioning and fluoroscopic alignment as previously described are critical to determine the starting holes and instrument orientation. The key step is passing the wire or awl lateral to the medial wall of the pedicle (on the anteroposterior [AP] view) at a depth at least equal to the pedicle/body junction (on the lateral view). However, fluoroscopy alone is only 68% accurate in pedicle screw placement. The addition of electrodiagnostic modalities (nerve root monitoring, not somatosensory evoked potential [SSEP] or motor evoked potential [MEP]) increases the sensitivity of identifying misplaced screws to 98%. This can be done dynamically by electrifying wires, awls, or taps, or statically by stimulating a screw after insertion. At this time, computer navigation systems are cumbersome, time-consuming, expensive, and often inaccurate. No system is 100% accurate. It is easier to pass or drop the rod into the screw heads if all the screws are in the same orientation in a single plane in relation to a vertical line perpendicular to the patient’s spine. An expandable retractor or a mini-open retractor (e.g., Quadrant, Medtronic Sofamor Danek, Memphis, TN) will make the procedure easier to perform. It is important for the surgeon and the operative team to be totally familiar with the implant system they are using. Each system has its own idiosyncrasies that can lead to problems (e.g., screws can disengage from drivers or holders; locking nuts can be prematurely advanced, preventing the passing of a rod; rods can disengage from holders). Placement of percutaneous pedicle screws requires several sequential steps. These steps can be divided into patient positioning, fluoroscopic identification, incision and approach, pedicle preparation, and hardware insertion. The first step in patient positioning is placing the patient prone on the operative frame. The surgeon must take care that the patient’s spine is rotated parallel to the floor and aligned perpendicular to the fluoros-copy beam, which is locked at 0 degrees. When patient positioning is accurate, proceed to fluoroscopic identification. Fluoroscopy is an important tool in percutaneous fixation, as the usual landmarks are not visible. The fluoroscope must be positioned at the precise angles of the anatomic structures; otherwise, the instruments may be placed inaccurately. On AP view, the superior end plate of the vertebrae of the pedicle of interest should be parallel to the fluoroscopy beam. Identify the transverse process of the pedicle on the AP fluoros-copy view and proceed to the incision and approach steps. The skin incision or stab wound is made between the midpoint of the transverse process (TP) and the lateral tip of the TP. This location is individualized by patient size: the larger the patient, the more lateral the incision is made (Fig. 68.1).
Percutaneous Lumbar Pedicle Screw Fixation
Description
Expectations
Indications
Contraindications
Special Considerations
Tips, Pearls, and Lessons Learned
Nerve Root Monitoring
Multiple-Level Percutaneous Instrumentation
Pedicle Screw with Decompression, Transforaminal Lumbar Interbody Fusion, Posterior Lumbar Interbody Fusion, or Posterolateral Fusion
Know Your Implant System
Key Procedural Steps
Patient Positioning
Fluoroscopic Identification
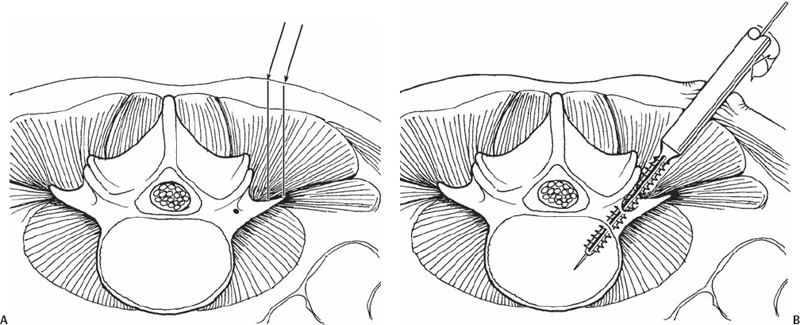
Incision and Approach
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







