10 Howard B. Levene and Jack I. Jallo Posterior cervical wiring is a relatively simple and inexpensive technique for achieving cervical stability by providing a posterior tension band that resists flexion. At one time the preferred procedure for posterior cervical stabilization, the technique has since fallen out of favor in light of the popularity of lateral mass screw fixation. However, the technique remains a valuable supplemental or salvage procedure. There are three general types of wiring: (1) spinous process wiring, (2) facet wiring, and (3) sublaminar wiring. Although sublaminar wiring continues to be useful for atlantoaxial fixation, it generally has been abandoned for subaxial cervical spine fixation due to the comparatively high risk of neurologic injury when compared with modern fixation systems. Spinous process wiring and facet wiring share the fundamental ability to fuse adjacent levels through the creation of a posterior tension band. Wires are passed through a bony element (spinous process or facet) and either looped over another bony element or passed through another bony element. Autograft/ allograft/artificial biomaterials can be used to supplement the fusion technique. There are multiple techniques for simple interspinous wiring: Rogers wiring, Whitehill modification of the Rogers Wiring, Benzel-Kesterson modification of Rogers wiring, Bohlman triple-wire technique, and the Murphy-Southwick modification of the Rogers technique. Facet wiring techniques include Cahill oblique facet wiring and Callahan non-oblique facet wiring. The Rogers method and its various modifications are expected to provide cervical stability to a single subaxial cervical motion segment. To stabilize additional levels, the procedure can be repeated. The Murphy-Southwick modification of the Rogers technique is designed to stabilize additional segments. Cervical wiring is indicated for subaxial instability resulting from trauma, neoplasm, degeneration, or infection (posttreatment). Cervical wiring is indicated when stability is restored with re-creation of a posterior tension band to prevent progression of deformity, to alleviate pain, or to promote bony fusion. These wiring techniques are contraindicated when there is an incomplete posterior bony ring, poor bone quality, or stability requirements (extension, rotation, lateral motion) beyond what can be delivered by posterior wiring. When choosing posterior wiring, it is important to remember that wiring provides almost no stability in extension, lateral bending, or axial rotation. Careful preoperative consultation with anesthesia colleagues is required. For intubation, the surgeon should arrange for fiberoptic laryngoscopic intubation. Prior to positioning, neuromonitoring (somato-sensory evoked potential [SSEP], motor evoked potential [MEP]) should be checked for baseline values. Changes in baseline signals during positioning are addressed with repositioning, steroid administration, or abandonment of the procedure. When positioning, the patient is prone with neutral cervical spine or slight extension to the cervical spine. Mayfield pins or cervical traction are options. Posterior wiring requires that the posterior elements are intact. Avoid this technique in cases of severe instability. Use it as a stand-alone device only when the anterior and middle load-bearing columns are intact and a posterior tension band needs to be restored. A rigid cervical collar or halo may be required for stability during fusion. Facet wiring can be used when the lamina or spinous process of the adjacent rostral segments are missing. When using autograft, ribs make good posterior strut grafts versus iliac crest due to their natural curvature. Stainless steel, titanium, and polyethylene cables are available; 16- to 20-gauge metallic wires are the preferred sizes. Stainless steel wires have the best tensile strength. Titanium is more susceptible to fatigue notching than stainless steel, but it has a better magnetic resonance imaging (MRI) profile. Polyethylene cables exhibit more creep than metal alloys, but have the best MRI profile. Methylmethacrylate may be used to reinforce the construct in cases of tumor. Braided (22-gauge) metallic cables possess a good combination of strength and handling properties. In all techniques, a midline incision is made. Using sharp, blunt, and electrocautery dissection, the incision is extended deep to the superficial fascia. The midline raphe is identified. Dissection is performed bilaterally down along the spinous processes. Lateral exposure identifies the medial aspect of the lateral masses. Fluoroscopy or a lateral plain x-ray is used to identify the correct surgical level. Trauma to the facet capsule and ligaments is avoided. For the Rogers interspinous wiring technique, a right-angle dental drill is used to make a hole at the base of the spinous process dorsal to the spinal laminar junction at each respective level. The drill hole for the cephalad vertebrae is in the superior third of the spinous process, and the drill hole for the caudal level is in the inferior third of the spinous process. A wire is passed through the hole and looped above the spinous process for the cephalad vertebrae. The loop is passed inferior to the spinous process for the inferior vertebral body. The wire ends are now tightened together. Remember to decorticate the spinous processes and the laminae for bone grafting (Fig. 10.1). In the Whitehill modification of the Rogers wiring technique, a hole is not drilled in the caudal vertebral spinous process as the wire is looped under the caudal spinous process prior to tightening (Fig. 10.2). This process may be repeated at several levels. The Benzel-Kesterson modification of the Whitehill technique calls for an additional wire to be passed through the drill holes to be used to attach to grafting material laid bilaterally along the posterior elements (Fig. 10.3). The Bohlman and McAfee triple-wire technique is similar to the Rogers technique at the superior and inferior vertebral levels. The first cable is passed through holes made within the spinous processes of the superior and inferior vertebral levels as with the Rogers technique. Two separate cables are then passed through these holes and are used to affix two strut grafts along the posterior elements on each side (Fig. 10.4). The Murphy-Southwick modification of the Rogers technique allows for fusion of two adjacent motion segments. Holes are drilled into each respective spinous process as above and wires are placed and tightened to bind all three spinous processes.
Posterior Cervical Wiring
Description
Expectations
Indications
Contraindications
Special Considerations
Special Instructions, Position, and Anesthesia
Tips, Pearls, and Lessons Learned
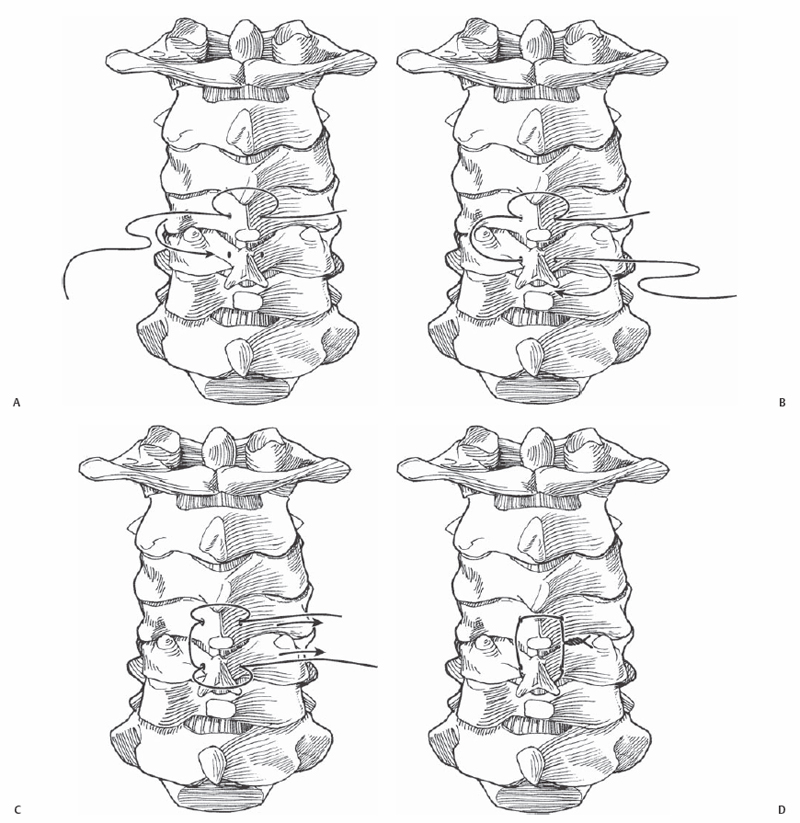
Key Procedural Steps
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







