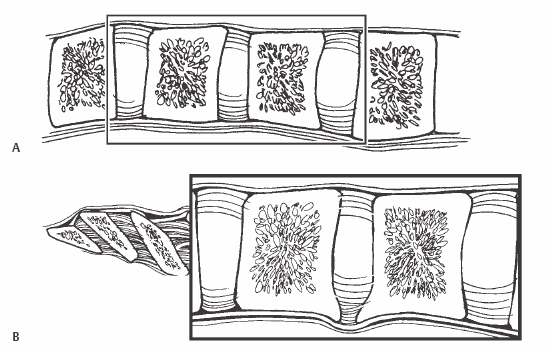
16 Iain H. Kalfas Resection of the posterior longitudinal ligament (PLL) following anterior cervical discectomy or corpectomy. Resection of the PLL provides optimal access to the epidural space. Following anterior cervical diskectomy or corpectomy, resection of the PLL allows for the removal of subligamentous or free disk fragments as well as providing for a more optimal removal of ventral epidural osteophytes. Access to the lateral neural foramina is also improved. Failure to remove the PLL may result in an incomplete decompression of the epidural space. Anterior cervical surgery for significant epidural compression (Fig. 16.1). Fig. 16.1 (A) Lateral view demonstrating the relationship of the PLL to the vertebrae and the underlying dura. (B) Lateral view demonstrating a ventral epidural osteophyte. The PLL is projected into the dura. Anterior cervical surgery without significant epidural compression. Ossification of the PLL may be a relative contraindication to removal of the PLL depending on its severity. Magnetic resonance imaging (MRI) or computed tomography (CT)/myelography is required preoperatively to demonstrate the spatial relationship of the disk herniation or osteophyte(s) to the epidural space as well as the degree of epidural compression. The patient is positioned supine with only a mild degree of cervical extension. Fiberoptic intubation is used if the patient’s symptoms are worsened during preoperative cervical extension. Intravenous steroids may be administered preoperatively for prophylaxis. Electrophysiologic monitoring is a consideration in procedures requiring removal of the PLL. The technique is more easily performed using the optimal illumination and visualization provided by a head light or a surgical microscope. The initial opening of the PLL can be made with a nerve hook inserted between the fibers of the PLL. The hook is then pulled upward, producing a small opening in the PLL. The opening can then be enlarged with a 1-mm Kerrison rongeur. Removal of the PLL rarely results in a durotomy. If this occurs, it is managed by placing a layer of Gelfoam over the defect. If the durotomy is large, a short period of lumbar subarachnoid drainage may be required. Removal of the PLL can also result in epidural bleeding. Except in the isolated cases of ossification of the posterior longitudinal ligament (OPLL), it is rarely significant. Epidural bleeding can usually be controlled with bipolar electrocautery and gentle epidural pressure with Gelfoam and cottonoid pledgets. Following the diskectomy or corpectomy, the PLL is opened with a nerve hook or No. 11 blade. The PLL is pulled upward to produce a small tear that will allow for insertion of a 1-mm Kerrison rongeur. As the opening is enlarged, the dura is visualized. It is differentiated from remaining thin leaflets of PLL by a glistening appearance and the lack of any longitudinal striations. Failure to easily pass the rongeur under the adjacent vertebrae is also an indication that the PLL has not been incised completely. As the decompression progresses, a 2- or 3-mm Kerrison rongeur can be used to undercut the adjacent vertebral end plates (Fig. 16.2). This allows for a more complete removal of intervertebral osteophytes as well as access to free disk material (Fig. 16.3). Removal of the PLL also provides access to the neural foramina. The proximal 2 to 3 mm of the root can be directly decompressed following PLL resection.
Posterior Longitudinal Ligament Takedown
Description
Key Principles
Expectations
Indications
Contraindications
Special Considerations
Special Instructions, Position, and Anesthesia
Tips, Pearls, and Lessons Learned
Difficulties Encountered
Key Procedural Steps

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







