50
Reduction of High-Grade Spondylolisthesis
Charles C. Edwards and Charles C. Edwards II
Description
Full correction of high-grade spondylolisthesis (Fig. 50.1) is achieved through an entirely posterior approach, with or without sacral dome osteotomy, by using graduated instrumented distraction, posterior translation of the proximal spine, and flexion of the sacrum.
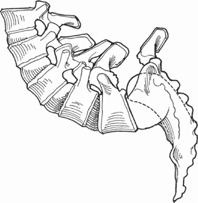
Fig. 50.1 A full-grade spondyloptosis.
Expectations
Careful preoperative planning, complete neural decompression, and the gradual application of corrective forces over time with effective instrumentation consistently yields anatomic reduction of the spine and a high rate of successful fusion without the need for anterior surgical approaches. For spondyloptosis, sacral dome osteotomy or a second stage of surgery may be necessary to limit lumbar root stretch.
Indications
High-grade spondylolisthesis and spondyloptosis.
Contraindications
Lack of Patience or Surgical Experience
This is a technically difficult and demanding undertaking even for the most experienced spinal surgeon. The surgeon cannot force reduction ahead of stress-relaxation and nerve accommodation. Hands-on training, experience with lesser slips, and a long learning curve are necessary to master the planning and reduction techniques for consistently excellent results.
Older or Frail Patients
This surgery is rarely indicated in patients over 40 or 50 years of age.
Special Considerations
Preoperative planning is essential. Standing lateral and supine flexion/extension radiographs are needed to determine the “root-lengthening limit” and for planning surgery. First, make two tracings of the flexion lateral film: sacrum and L1–L5. To simulate complete reduction, the sacrum is flexed with its long axis oriented 35 degrees from vertical. The L1–L5 tracing is then positioned with L5 reduced, L3 horizontal, and L1 vertically centered over the anterior body of S1 (Fig. 50.2). To determine how much L5 nerve root lengthening will occur with full reduction, measure the distance from the L4 pedicle (root origin) to the sciatic notch (root exit) on the pre-reduction standing lateral and postreduction lateral tracings. The difference represents expected root lengthening.
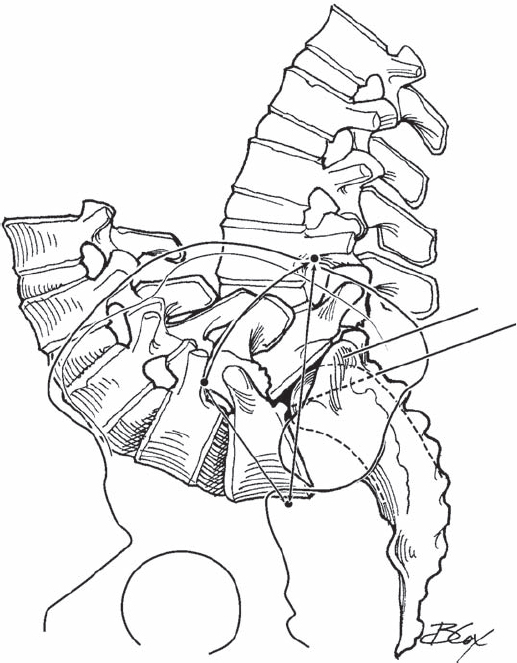
Fig. 50.2 Preoperative planning demonstrating the corrected position of the spine, the location of the sacral osteotomy, and measurement of the anticipated change in the L5 nerve length.
The root-lengthening limit without deficit for one stage of surgery varies between 2 and 5 cm depending on several factors. The lengthening limit is reduced (from 5 toward 2 cm) when (1) the patient is older than 20; (2) the duration of optosis exceeds 2 years; (3) the L5/S1 slip angle is greater than 50 degrees; (4) bending films demonstrate a rather fixed panlumbar lordosis; (5) there have been prior lumbosacral (LS) fusion attempts or; (6) preoperative lumbar radiculitis/radiculopathy is present. If all six predictors are negative, only about 2 cm of lengthening is safe in one day, whereas if there are no negative predictors, 5 cm of lengthening is generally possible without deficit. If reduction exceeds the root lengthening limit, there are two alternatives: (1) the reduction may be divided between two procedures a week apart, or (2) the spine is shortened by removing 0.5 to 1.5 cm from the proximal sacrum through the posterior approach.
Special Instructions, Position, and Anesthesia
Before surgery the patient practices ankle dorsiflexion for the wake-up test. An overhead traction frame is assembled over the head of the table. The patient is positioned prone with hips initially flexed 30 degrees to facilitate LS visualization and knees flexed 70–90 degrees to relax the sciatic nerve. Hips are extended later to facilitate reduction.
Tips, Pearls, and Lessons Learned
The Spondylo Construct of the Edwards Modular Spine System (EMSS) (Scientific Spinal, Baltimore, MD) is specifically designed to facilitate this operation. It allows the surgeon to move and stabilize the spine simultaneously with 6 degrees of freedom. Controlled incremental change in spine position is made possible with ratcheted rods and threaded connectors.
Difficulties Encountered
The relationship of L5 to the sacral ala and L5 transverse process changes during the reduction sequence. The L5 roots need to be checked often during reduction to ensure no compression. Reduction lengthens the L5 root, which must also be checked for excessive tightness in addition to somatosensory evoked potential (SSEP)/electromyogram (EMG) monitoring. Reduction must be stopped if there is depression of the SSEP or EMG response or excess nerve tightness to palpation. Additional sacral shortening, root decompression as it crosses the ala, or an additional stage may be needed to safely complete the reduction.
Key Procedural Steps
- Exposure: Expose the spine from L3 to S2. Identify and protect the L3-L4 and L4-L5 facet capsules. L5 may sit anterior to the sacrum and be difficult to see. Partial reduction is therefore needed to safely decompress the L5 roots. This is accomplished with concurrent alar rod distraction and posterior traction.
- Alar rods: Insert EMSS combination connectors (reduction screws) into the L4 pedicles without injuring the facet capsules. Combination connectors consist of a pedicle screw-swivel joint-threaded rod and adjustable ring body. Next, insert the shoe of high (10 mm) anatomic hooks into holes burred in the top of the sacral ala. A short ratcheted universal rod is inserted into the hook distally and into the ring body of the L4 combination connector proximally. The ring bodies are ratcheted up these “alar rods” in small gradation to gradually raise L5 out of the pelvis.
- Overhead traction: Initial reduction to achieve L5 visualization requires both distraction and posterior translation of the lumbar spine. The posterior vector is provided by 18-gauge wires attached to the ring bodies of the L4 connectors or proximal end of the alar rods. The two sterile wires are passed to the anesthesiologist who ties them to traction rope. The rope passes over a pulley attached to the trapeze erected over the head of the bed; 20 to 30 lb are added to the end of each rope to create the cephalodorsal vector. Sequential distraction of the alar rods combined with the constant pull of dorsal traction yields stressrelaxation of the contracted anterior tissues. The L5 vertebra gradually rises out of the pelvis and around the sacral dome.
- L5 root decompression: Remove the L5 arch as a single block using the Gill technique. The L5 roots are covered by the medial edge of the superior facet of L5 and pars nonunion fibrocartilage. Place a small angled Kerrison punch into the canal just proximal to the L4-L5 facet joint and resect redundant liga-mentum flavum, the osteophytic medial projection from the L5 superior facet, and various arrays of fibrocartilage all covering the L5 roots. Continue the decompression laterally with a 3- to 4-mm narrow-shoe Kerrison punch across the iliolumbar ligaments until the L5 roots pass anterior to the sacral ala. To prevent root injury, the L5 root must be continuously observed.
- Sacral osteotomy: If the preoperative planning radiographs indicate the need for proximal sacral osteotomy, the L5 and S1 roots and dural sac are fully mobilized to expose the sacral dome. The epidural venous plexus overlying the annulus is cauterized with a bipolar electrode. A 1/4-inch osteotome is tamped into the sacral dome and adjusted under C-arm visualization until it matches the position planned for the osteotomy on the preoperative radiograph. The osteotomy is completed with 1/2-inch osteotomes from one side and then the other side of the dura extending to the lateral ala. The posterior annulus is then resected from its origin on the posteriorly projecting osteophytes at the base of the L5 vertebral body using curved osteotomes and large pituitary rongeurs. The resected sacral dome is cut into sections and removed in pieces together with the lumbosacral disk. If more than 1 cm is removed from the sacral dome, it is necessary to fashion posteromedial to anterolateral channels (pseudo-foramen) into the superior ala for the L5 roots to exit between the L5 transverse processes and the ala.
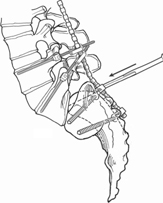
- The spondylo construct: Once alar rod distraction and posterior translation from overhead traction have raised L5 out of the pelvis, screws can be safely inserted into L5. With the L5 root and medial pedicle cortex under direct view, the L5 pedicle is cannulated with a blunt probe, oriented 20 degrees medially to spare the L4-L5 facet capsule dorsally and engage the vertebral body ventrally. After confirmation of appropriate trajectory with biplanar C-arm views, combination connector screws are inserted into L5. S1 screws may be directed either medially through the sacral pedicle or laterally across the ala. Bicortical alar screws are preferable after generous sacral osteotomy. A second point of distal fixation is needed to effectively control sacral rotation and to provide an adequate lever-arm for sacral flexion and mechanically sound fixation. When sacral bone is weak or the patient is obese, iliac screws can provide even stronger distal fixation. Mid-sacral alar screws, however, require less dissection and do not span the SI joints. In either case, rods are attached to the distal screws and to the S1 screws using a low or medium hook linkage. Before loading the rods, apply a cross-lock to the rods between the S1 and the distal fixation points. Then remove the alar rods one at a time and attach the L5 connectors to the rods (Fig. 50.3).
- Reduction: The first phase of reduction is to raise L5 out of the pelvis. This is accomplished by the overhead traction and alar rods. Further correction is achieved by incrementally ratcheting and shorting the L5 connectors. First, shorten the connectors until resistance is felt, and then distract the connectors to separate the L5 body from the sacrum. Sequentially shorten (tighten) and distract (ratchet) the connectors to two-finger tightness every 10 minutes. Re-image to determine the relative amount of distraction versus translation required. Periodically check the L5 roots with a probe to ensure that they do not become overly taut or compressed between the L5 transverse process and the ala. Allow 30 to 60 minutes per grade for stress relaxation of the contracted anterior tissues to permit reduction of the deformity (Fig. 50.4). Reduction is continued until (1) the nerve lengthening threshold is met, (2) nerves become taut, (3) SSEP (or triggered EMG) data begin to deteriorate, or (4) function is reduced on wakeup. In the event of (3) or (4), reduction is partially released until normal function is restored.
- Optional stage 2: If a subsequent stage is required to safely complete the reduction, the instrumentation is locked in place, and the wound closed. Patients are kept on bed rest for 1 week. We usually begin the second-stage reduction under local anesthesia. We have found that patients consistently experience sciatic pain from excess root stretch long before any change can be detected on EMG or SSEP. The surgeon is able to continuously monitor motor function by talking with the awake patient and observing ankle dorsiflexion. Once L5 is positioned on top of the sacrum within a few millimeters of anatomic alignment, the L5 connectors are compressed toward the sacrum to restore lordosis and further shortened until a normal alignment is achieved. Once reduction is nearly complete, the patient is given general anesthesia. The instrumentation is locked into its final position and any further needed root decompression is performed, followed by posterolateral decortication and iliac grafting (Fig. 50.5).
- Postoperative bracing: Following surgery, our patients are routinely mobilized in a custom-made, below-the-breast thoracolumbar spinal orthosis (TLSO) with a thigh cuff. The brace serves to (1) lessen stress on the bone-implant interface, (2) counteract the flexion moment caused by contracted anterior tissues such as the rectus abdominus and iliopsoas muscles until they relax over time, and (3) prevent adjacent-segment kyphosis due to this flexion moment coupled with extensor muscle and L4-L5 facet capsular impairment from surgery.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







