Fig. 22.1
SPECT
22.3.2 Muscle Strain
Muscle strains are a common cause of back pain in the pediatric and adolescent athlete. They have been estimated to occur in 27 % of adolescent athletes presenting with lower back pain [16, 27]. Strains result from disruption in muscle fibers within the muscle belly or musculotendinous junction.
Numerous factors such as acute trauma, repetitive stress, poor technique, obesity, muscle imbalance, and poor footwear can contribute to muscle strain. Patients with a spinal muscle strain present with progressively worsening lower back pain and possible spasms. Symptoms peak 24–48 h after onset. Diagnostic testing such as plain radiography, bone scan, and MRI are usually negative and do not contribute to the diagnosis. However, if patients present with any “red flags,” imaging is necessary to rule out other etiologies [16].
Many children presenting with “mechanical back pain” are experiencing failure of their core muscles during exertional activities. After a growth spurt, the adolescent athlete often develops transient lower extremity muscle contractures, further altering the stresses acting upon the lumbosacral junction. Treatment should focus on lower extremity stretching and core strengthening exercises.
22.3.3 Lumbar Scheuermann’s Disease
Lumbar Scheuermann’s disease is another potential cause of back pain in the adolescent athlete. It is an overuse injury involving the lumbar spine that occurs in sports requiring repetitive flexion and extension. Male weight lifters and football players are most commonly affected. Patients present with localized back pain exacerbated by forward flexion. Pain may be associated with muscle spasm and loss of lumbar lordosis. Neurological deficit is a rare finding.
Radiographic evaluation of Scheuermann’s disease involves a plain lateral radiograph of the lumbar spine. Interestingly, lumbar Scheuermann’s disease may not present with the classic anterior wedging deformity (greater than 5° of anterior wedging across three consecutive vertebral bodies) as is associated with the thoracic variant. The original paper by Blumenthal, Roach, and Herring found that only 6/13 patients had classic anterior wedging. The remainder presented with anterior Schmorl’s nodes—and all of these atypical cases presented with pain [28–30].
Lumbar Scheuermann’s disease can be managed conservatively. Activity modification and lumbar bracing may facilitate pain control. Physical therapy should be directed at pelvic and lumbar stabilization exercises. The patient may return to play when pain subsides and after completion of physical therapy [29].
22.3.4 Back Pain Secondary to Stress Fractures
Spinal stress fractures are a common cause of back pain in the immature athlete (Fig. 22.2). It is particularly common in athletes participating in sports requiring repetitive hyperextension and flexion [31]. Stress fractures result from repetitive low-intensity load and microtrauma to the bone. Two theories have been postulated to explain the occurrence of stress fractures. In the overload theory, repetitive rhythmic contractures of muscles result in stress at their osseous insertions, consequently reducing the mechanical resistance of the bone. The muscle fatigue theory attributes stress fractures to diminished shock absorbing properties of a fatigued muscle subjected to repetitive stress. This leads to aberrant loading of bone and subsequent failure [22, 32].
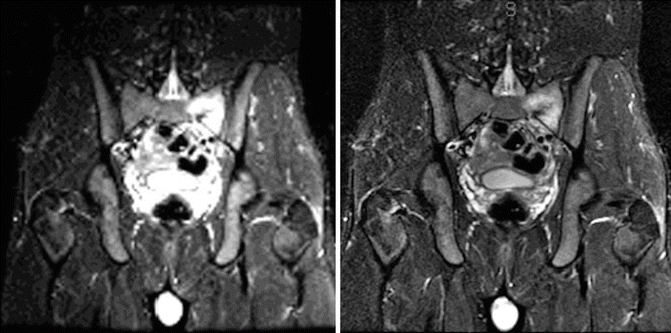

Fig. 22.2
A 17-year-old boy presented with 3 weeks of left lower back and sacral pain. While he had no specific injury, his symptoms began during a 13-mile cross-country run. He notes the pain was 6 out of 10 at its worse. Past medical history reveals no prior illness, injuries, surgeries, or hospitalization. On physical examination, his pain was localized with palpation along the left posterior superior iliac spine. Radiographs show no evidence of stress fractures or other osseous abnormalities. MRI of the pelvis reveals a left sacral stress fracture with soft tissue edema
The immature adolescent spine is particularly susceptible to stress fractures because of the absence of complete ossification. Areas of incomplete ossification within the vertebrae are weak points that become susceptible to failure when subjected to repetitive compressive, torsional, or distraction forces [31]. Adolescent athletes participating in sports such as gymnastics, weightlifting, or diving among others expose their spine to such forces thereby increasing the risk of stress injury. Of note, there is an additional risk seen in competitive female athletes suffering from the female athlete triad syndrome: disordered eating, amenorrhea, and osteoporosis. Both osteopenia and their propensity for overexertion increase the risk of stress fractures in this population. It is important to evaluate female adolescent athletes for this condition with both the history and physical examination, and begin a multidisciplinary approach to treatment if symptoms are present [22].
22.3.4.1 Spondylolysis/Spondylolisthesis
Spondylolysis is a common cause of back pain in the adolescent athlete (Fig. 22.3). Many studies have investigated the incidence of spondylolysis in the adolescent athlete. Notably, Micheli and Wood reported 47 % incidence of spondylolysis in adolescent athlete presenting with back pain [22]. However, Rossi reported a much lower incidence of 15 % in a review of radiographs of adolescent athletes [33]. Additionally, Drummond et al investigated nearly 3,000 adolescent patients presenting with low back pain, diagnosing only 7.8 % of them with spondylolysis [25].
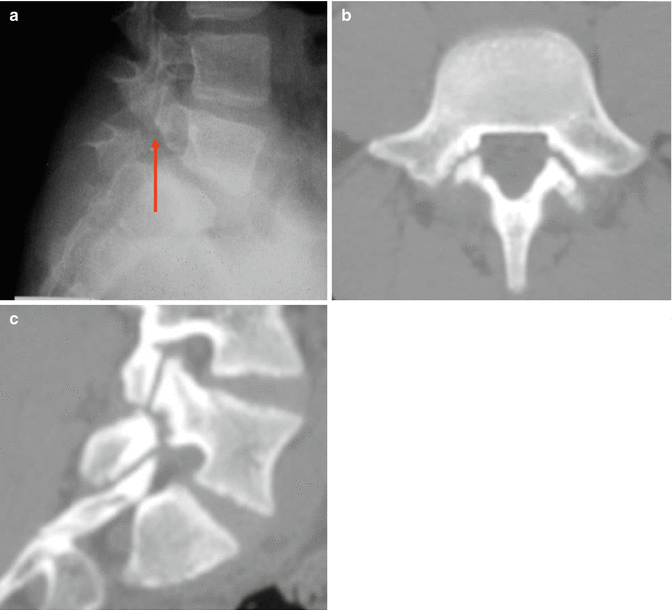

Fig. 22.3
Imaging of a 13-year-old elite level gymnast with 2 years of back pain who was diagnosed with spondylolysis. (a) Lesion visible on lateral radiograph with arrow demonstrating spondylolysis (b) and (c) CT images further define the stress fracture. Note the sclerotic margins on the transverse cut. This is a typical finding of a long-standing fracture with failure to heal
Spondylolysis is a defect in the vertebral pars interarticularis. It most commonly occurs at L5–S1 resulting from an L5 pars defect, though it may also occur at more cephalad levels. Subsequent translation of the cephalad vertebral body on the caudad vertebral body describes spondylolisthesis (Fig. 22.4) [34]. For more detail, please refer to Chap. 24 on Spondylolysis/Spondylolisthesis.
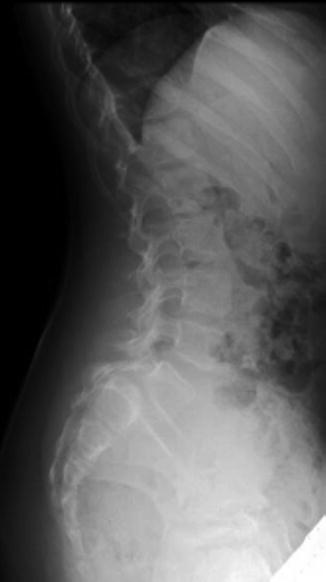

Fig. 22.4
Plain radiographic lateral view of an 8-year-old female with Grade III spondylolisthesis
Clinical Presentation
Spondylolysis is often asymptomatic and found incidentally. Athletes who do develop symptoms typically report focal back pain with occasional radiation to the buttocks or proximal thighs. The pain may either be insidious in onset or associated with an inciting traumatic event. Patients may also report an acute worsening of chronic mild pain after a new injury. Pain is often exacerbated by activities requiring repetitive flexion and extension of the lumbar spine [35]. Hamstring tightness is also a common complaint of patients with spondylolysis, especially in the presence of advanced spondylolisthesis. This may be manifested by a shortened gait stride with flexion at the hips and knees. Radicular symptoms are rare in spondylolysis and low-grade spondylolisthesis, but may be present with high-grade spondylolisthesis [34].
The one-legged hyperextension maneuver is considered by many to be pathognomonic for spondylolysis. In this maneuver, pain is elicited with a one-legged stance and lumbar extension. If the lesion is unilateral, pain is often localized to the ipsilateral side. Other findings include a hyperlordotic thoracolumbar posture, which compensates for a loss of lumbar lordosis. Neurological deficits are usually absent unless in the presence of significant spondylolisthesis.
22.3.4.2 Pedicle Fractures
A component of the neural arch, the pedicle is also vulnerable to fracture from the cyclic loads stressing the lumbosacral spine during sports. However, pedicle stress fractures are much less common than pars stress fractures [22]. This is partly secondary to the greater intrinsic strength of the pedicles and shorter moment arm from the vertebral body. The pedicles are therefore capable of resisting greater shear forces than the pars. In a biomechanical study evaluating the mechanical strength of 74 vertebral units subject to repetitive mechanical loads, Cyron and Hutton demonstrated five pedicular stress fractures compared to 55 pars fractures [36]. Contralateral pedicular fractures have been associated with isthmic pars fractures. This phenomenon has been attributed to increased and aberrant loading of the pedicles that result from an unstable neural arch following a pars fracture [37–39]. Ulmer et al. showed a 40 % incidence of reactive changes on MRI in pedicles with contralateral spondylolysis [40].
Radiographic evaluation of pedicular fractures involves plain radiographs and CT scan. CT scan has a higher accuracy in the evaluation of these patients. When visible, hypertrophy or sclerosis is seen on the involved pedicle. Pediculolysis is clearly demonstrated as a linear lucency at the base of the involved pedicle on CT. In addition, presence of a concomitant pars defect can also be identified [39, 41]. When evaluating patients with pediculolysis, one must consider osteoid osteoma and osteoblastoma in the differential diagnosis. These entities can be differentiated from a pediculolysis by the absence of a nidus, the presence of contralateral pars defect, or the presence of a linear defect in a pedicular stress fracture. Differentiating these lesions is important because pedicle excision—a management option for symptomatic tumor—may further destabilize an already unstable neural arch [39, 42].
Early diagnosis of a pedicular stress fracture and prompt treatment is necessary to facilitate rapid return to sports. Management of pedicular stress fractures is similar to that of a pars stress fracture. Initial management is conservative and involves rest and bracing. Surgery is indicated in the setting of failed conservative treatment, though surgical treatment is rarely necessary. Techniques described in the literature include compression fixation of the defect, excision of the hypertrophic defect with lateral fusion, and bone grafting of the pars and pedicular defects with subsequent pedicle screw fixation [37, 39, 43].
22.3.5 Radicular Pain in the Growing Athlete
22.3.5.1 Disc Herniation
Disc herniation is a rare cause of back pain in the adolescent athlete (Fig. 22.5). Only 1 % of disc herniations occur in the second decade [44]. As opposed to an incidence 48 % in the adult population, only 11 % of adolescent athletes present with symptomatic disc herniation. The most common location of herniation in the young athlete is the L4–L5 and L5–S1 level. In the skeletally immature patient, the disk may be herniated into the vertebral end plate with axial loading, demonstrating a Schmorl’s node on radiographs [29, 45].
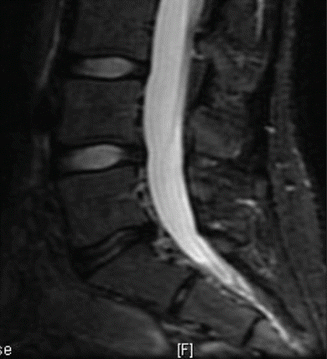

Fig. 22.5
Disc herniation
Young athletes with disc herniations typically present with localized back pain and paraspinal muscle spasm. Impingement of the nerve roots may result in radicular symptoms. Radicular symptoms warrant an MRI evaluation. In the absence of neurological compromise, conservative management is recommended, consisting of rest and activity modification. Prolonged bed rest is discouraged. NSAIDs, muscle relaxants, and oral corticosteroids may also be beneficial. The majority of adolescents can be treated nonoperatively. However, those with progressive neurological deficits or debilitating pain that has failed conservative management are candidates for a microdiscectomy. Patients are usually able to return to full participation in sports [45, 46]. While more applicable to adult patients as it examined an adult patient population, the SPORT trial examined the effects of operative versus nonoperative management for patients with a mean age of 42 who presented with symptomatic lumbar herniated discs. This multicenter randomized controlled trial concluded that at 2 years, patients treated surgically and nonoperatively both demonstrated substantial improvement and could not make conclusions about the superiority of one treatment over the other [47].
22.3.5.2 Vertebral Apophyseal Avulsion Fractures
An apophyseal ring fracture is a rare injury in the pediatric population, occurring primarily in the male adolescent athlete (Fig. 22.6) [48]. It most frequently affects L4 and L5. The incidence of apophyseal fractures may be underreported as it is frequently misdiagnosed as lumbar disc herniation [49].
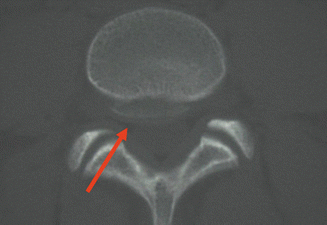

Fig. 22.6
Vertebral apophyseal ring avulsion fracture with arrow demonstrating fracture fragment
In the developing lumbar spine, the superior and inferior endplates are bordered by the vertebral ring apophysis. Ossification of the apophysis commences at approximately 5 years with fusion by age 18. During the rapid adolescent growth phase, the apophysis is separated from the underlying vertebral body by a physeal zone. This area of weakness is susceptible to avulsion injuries. It has been suggested that hyperextension of the lumbar spine or rapid flexion with axial load may be the causative mechanism [48].
Clinical presentation includes low back pain with potential radicular symptoms. Neurogenic claudication, paresis, and cauda equina syndrome has also been reported. The most common finding on examination is restricted lumbar range of motion. The straight leg raise test may be positive in these patients though frank neurological deficits are usually rare [49, 50].
Radiographic evaluation involves the use of both the plain radiograph and CT scan. Bony defects can be visualized on the lateral radiograph; however, the axial CT scan images have been proven to be more sensitive [51].
Takata et al. reported on a large series of apophyseal injures, classifying these injuries into three categories based on CT findings. Type 1 fracture is a separation of the posterior rim of the vertebra body with negligible defect in the vertebra body. This type was noted primarily in patients between the ages of 11 and 13. Type 2 describes an avulsion fracture of the posterior rim of vertebra body including the posterior segment of the overlying annulus fibrosis. It is more prevalent in older patients. Type 3 fracture is a small localized fracture posterior to an irregularity in the cartilaginous endplate [49].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








