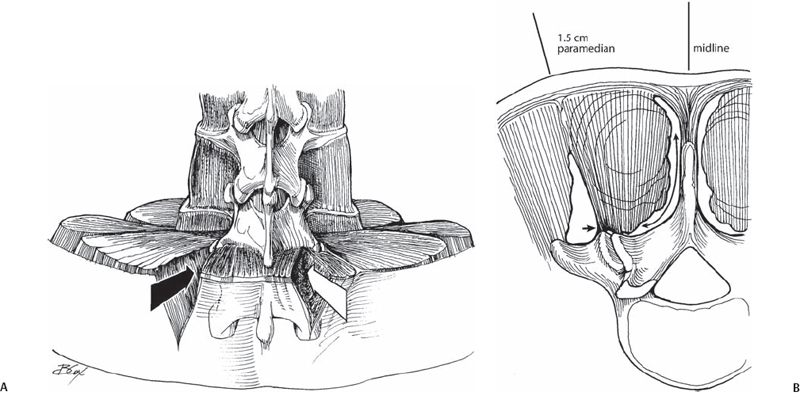
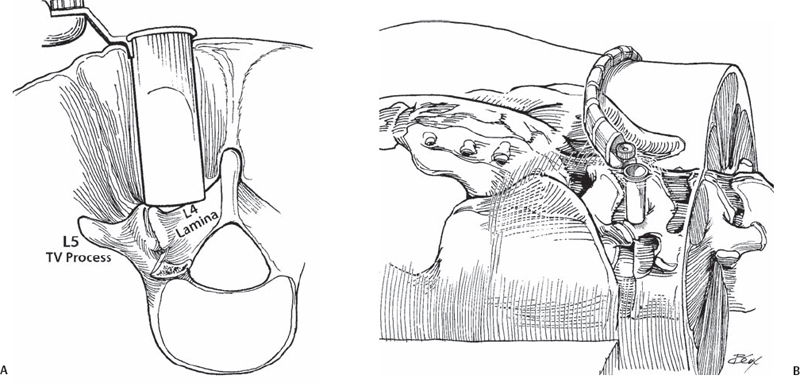
64 Y. Raja Rampersaud To provide access to the posterior spine by means of a paramedian muscle splitting approach that reduces the morbidity associated with conventional posterior spinal exposures. Technical and clinical outcomes associated with comparable procedures (see Indications and Contraindications, below) performed by conventional open exposures are achievable with this technique for one- and two-level pathology (and up to three levels for decompressions). Reduced blood loss, perioperative pain and length of hospital stay can be expected. For all medically fit patients, one- and two-level diskectomies or decompressive surgeries are performed on an outpatient basis. Surgical (primary or revision) management of symptomatic disk herniation, spinal stenosis (central or foraminal), spondylolisthesis (isthmic, degenerative, iatrogenic), as well as selective degenerative, traumatic, and oncologic cases. Cauda equina syndrome or myelopathy secondary to centrally located ventral pathology; otherwise, the contraindications are the same as for the comparable conventional procedures. Minimal access surgery does not provide additional indications for surgery, nor does it improve outcomes for patients with multifactorial sources (spinal or nonspinal) of pain, significant secondary gain issues, or unrealistic expectations of operative intervention. There are two basic approaches (Fig. 64.1): intramuscular (diskectomy, stenosis decompression, posterior lumbar interbody fusion [PLIF], facet fusions), and intermuscular (far lateral diskectomy, transforaminal lumbar interbody fusion [TLIF], facet fusion, pedicle screw instrumentation). Fig. 64.1 (A) Illustration at L5-S1 demonstrating the intramuscular (white arrow) and intermuscular (black arrow) access intervals. Using an intramuscular approach gains access deep to the multifidus where there is a free interval on the dorsal surface of the lamina. (B)From an intermuscular approach, this interval or the facet can be accessed by lateral-to-medial release of the tendinous attachments (arrowhead) from the facet joint. It is crucial to accurately localize the skin /fascial incision. In addition, moving the retractor to maintain the anatomy of interest in the center of the surgical field facilitates the most efficient trajectory for the instruments. A larger or expandable retractor is less confining and is necessary for larger procedures (e.g., fusion). However, the larger retractors (22 to 26 mm) do not sit flat on the lamina and thus do not completely retract the surrounding muscles. Consequently, a smaller retractor is more efficient for diskectomies and decompressions. There are a variety of techniques to gain access to the epidural space. For a diskectomy, the ligamentum is split longitudinally along its fibers or released from its caudal insertion point. For stenosis procedures, the ligamentum is released from the caudal insertion point and cephalad origin. Bleeding control can be difficult; thus, preemptive hemostasis and release of epidural veins are essential. Use of all microsurgical bleeding control techniques is possible through these retractors. The use of angle-tipped bipolar forceps can be invaluable. Most dural tears that occur are small and can be simply managed using a sealant. If necessary, dural suturing can be performed (although it is difficult with the 16- to 18-mm retractor). If a watertight seal is achieved, patients are mobilized and discharged the same day. For fusion procedures, the larger incision allows you to place your finger down the operative corridor to directly palpate and familiarize yourself with the anatomy. This is a powerful adjunct for surgeon assurance and patient safety. The patient is positioned prone on a radiolucent table and frame. The midline is identified and marked. Paramedian line(s) are then drawn 1.5 cm from the midline for diskectomy and decompression procedures and 3 to 5 cm from the midline (a more lateral starting point is utilized for larger patients) for fusion and instrumentation procedures. Localize the skin incision directly in line with the disk space of interest (typically with fluoroscopy, serial x-rays can also be used). The incision is made 2 mm larger than the diameter of the retractor. Unless there has been a previous decompression, the inferior lamina of the cephalad vertebrae overhangs the disk space and helps protect from inadvertent dural puncture. From the center of the incision, the guidewire is advanced just beyond the dorsal fascia. The initial cannulated dilator is advanced past the fascia, the guidewire is removed, and the dilator is docked onto the lamina. The initial dilator is then used to gently separate the soft tissues from the dorsal aspect of the lamina and to palpate the base of the spinous process medially, the facet joint laterally, and the inferior edge of the lamina. Palpation and subsequent visualization of the laminar edge is essential for orienting the operating surgeon to the remaining obscured anatomy. The remaining sequential dilators are then placed. A tubular retractor (Fig. 64.2) of the appropriate length is placed down to the lamina and secured in place (centered over the inferior laminar edge of the cephalad vertebrae). An operating microscope is used for illumination and visualization. Alternatively, a high-intensity head light or a fiber optic light source and loupes can be utilized. Often a small portion of the deep layer of the multifidus muscle may be required to be cauterized or resected to the boundaries of the retractor.
Tubular Access to the Posterior Spine: Fixed Diameter or Expandable Retractors
Description
Expectations
Indications
Contraindications
Special Considerations
Tips, Pearls, and Lessons Learned
Key Procedural Steps
Diskectomy and Decompression
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







